Get your patient on Albuterol - Albuterol tablet (Albuterol)
Albuterol - Albuterol tablet prescribing information
INDICATIONS AND USAGE
Albuterol tablets, USP are indicated for the relief of bronchospasm in adults and children 6 years of age and older with reversible obstructive airway disease.
DOSAGE AND ADMINISTRATION
The following dosages of albuterol tablets are expressed in terms of albuterol base.
Albuterol tablets
Usual Dosage
Pediatric Patients 6 to 12 Years of Age:
For pediatric patients 6 to 12 years of age, the usual dosage is 2 mg three or four times a day.
Adults and Pediatric Patients Over 12 Years of Age:
For adults and pediatric patients over 12 years of age, the usual starting dosage is 2 or 4 mg three or four times a day.
Dosage Adjustment
Pediatric Patients 6 to 12 Years of Age Who Fail to Res pond to the Initial Starting
Dosage of 2 mg Four Times a Day:
For pediatric patients from 6 to 12 years of age who fail to respond to the initial starting dosage of 2 mg four times a day, the dosage may be cautiously increased stepwise, but not to exceed 24 mg/day (given in divided doses).
Adults and Pediatric Patients Over 12 Years of Age:
For adults and pediatric patients over 12 years of age, a dosage above 4 mg four times a day should be used only when the patient fails to respond to lower dose. The dosage should be cautiously increased stepwise up to a maximum of 8 mg four times a day as tolerated if a favorable response does not occur with the 4 mg initial dosage.
Elderly Patients and Those Sensitive to Beta-adrenergic Stimulators:
An initial dosage of 2 mg three or four times a day is recommended for elderly patients and for those with a history of unusual sensitivity to beta-adrenergic stimulators. If adequate bronchodilation is not obtained, dosage may be increased gradually as tolerated to as much as 8 mg three or four times a day.
The total daily dose should not exceed 24 mg per day in pediatric patients from 6 to 12 years of age and 32 mg in adults and pediatric patients over 12 years of age.
CONTRAINDICATIONS
Albuterol tablets are contraindicated in patients with a history of hypersensitivity to albuterol, or any of its components.
ADVERSE REACTIONS
The adverse reactions to albuterol are similar in nature to those of other sympathomimetic agents.
| Adverse Event | Percent Incidence |
| Central nervous system | |
| Nervousness | 20% |
| Tremor | 20% |
| Headache | 7% |
| Dizziness | 2% |
| Weakness | 2% |
| Sleeplessness | 2% |
| Irritability | <1% |
| Drowsiness | <1% |
| Restlessness | <1% |
| Cardiovascular | |
| Palpitations | 5% |
| Tachycardia | 5% |
| Flushing | <1% |
| Chest discomfort | <1% |
| Musculoskeletal | |
| Muscle cramps | 3% |
| Gastrointestinal | |
| Nausea | 2% |
| Genitourinary | |
| Difficulty in micturition | <1% |
Cases of urticaria, angioedema, rash, bronchospasm, oropharyngeal edema and antirhytmias (including atrial fibrillation, supraventricular tachycardia, and extrasystoles) have been reported after the use of albuterol tablets.
In addition to those adverse reactions reported above, albuterol, like other sympathomimetic agents, can cause adverse reactions such as angina, central nervous system stimulation, drying or irritation of the oropharynx, hypertension, unusual taste, and vertigo.
The reactions are generally transient in nature, and it is usually not necessary to discontinue treatment with albuterol tablets. In selected cases, however, dosage may be reduced temporarily; after the reaction has subsided, dosage should be increased in small increments to the optimal dosage.
Drug Interactions
The concomitant use of albuterol tablets and other oral sympathomimetic agents is not recommended since such combined use may lead to deleterious cardiovascular effects. This recommendation does not preclude the judicious use of an aerosol bronchodilator of the adrenergic stimulant type in patients receiving albuterol tablets. Such concomitant use, however, should be individualized and not given on a routine basis. If regular coadministration is required, then alternative therapy should be considered.
DESCRIPTION
Albuterol tablets, USP contain albuterol sulfate, USP, the racemic form of albuterol and a relatively selective beta 2 -adrenergic bronchodilator. Albuterol sulfate has the chemical name α 1 -[( tert -Butylamino)methyl]- 4-hydroxy- m -xylene-α,α'-diol sulfate (2:1) (salt) and the following structural formula:
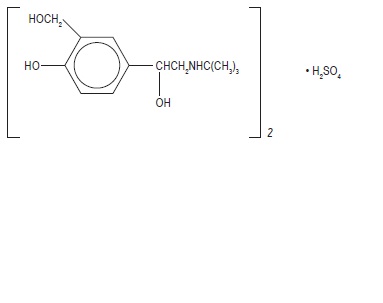
The molecular weight of albuterol sulfate is 576.71, and the molecular formula is (C 13 H 21 NO 3 ) 2 •H 2 SO 4 . Albuterol sulfate, USP is a white or practically white powder. It is freely soluble in water, slightly soluble in alcohol, in chloroform and in ether.
The World Health Organization recommended name for albuterol base is salbutamol.
Each albuterol tablet, USP for oral administration contains 2 mg or 4 mg of albuterol as 2.4 mg or 4.8 mg of albuterol sulfate, USP respectively and following inactive ingredients: colloidal silicon dioxide, lactose monohydrate, magnesium stearate, microcrystalline cellulose, povidone, pregelatinized starch (botanical source: maize) and sodium starch glycolate.
FDA approved dissolution specification differs from the USP dissolution specification.
CLINICAL PHARMACOLOGY
The primary action of beta-adrenergic agonist drugs, including albuterol, is to stimulate adenyl cyclase, the enzyme which catalyzes the formation of cyclic-3',5'- adenosine monophosphate (cyclic AMP) from adenosine triphosphate (ATP) in beta-adrenergic cells. The cyclic AMP thus formed mediates the cellular responses. Increased cyclic AMP levels are associated with relaxation of bronchial smooth muscle and inhibition of release of mediators of immediate hypersensitivity from cells, especially from mast cells.
In vitro studies and in vivo pharmacologic studies have demonstrated that albuterol has a preferential effect on beta 2 -adrenergic receptors compared with isoproterenol. While it is recognized that beta 2 -adrenergic receptors are the predominant receptors in bronchial smooth muscle, data indicate that there is a population of beta 2 -receptors in the human heart existing in a concentration between 10% and 50%. The precise function of these receptors has not been established (see WARNINGS ).
In controlled clinical trials, albuterol has been shown to have more effect on the respiratory tract, in the form of bronchial smooth muscle relaxation, than isoproterenol at comparable doses while producing fewer cardiovascular effects. Controlled clinical studies and other clinical experience have shown that inhaled albuterol, like other beta-adrenergic agonist drugs, can produce a significant cardiovascular effect in some patients, as measured by pulse rate, blood pressure, symptoms, and/or ECG changes.
Albuterol is longer acting than isoproterenol in most patients by any route of administration because it is not a substrate for the cellular uptake processes for catecholamines nor for catechol- O -methyl transferase.
Preclinical
Intravenous studies in rats with albuterol sulfate have demonstrated that albuterol crosses the blood-brain barrier and reaches brain concentrations amounting to approximately 5% of the plasma concentrations. In structures outside the blood-brain barrier (pineal and pituitary glands), albuterol concentrations were found to be 100 times those in the whole brain.
Studies in laboratory animals (minipigs, rodents, and dogs) have demonstrated the occurrence of cardiac arrhythmias and sudden death (with histologic evidence of myocardial necrosis) when beta-agonists and methylxanthines are administered concurrently. The clinical significance of these findings is unknown.
Pharmacokinetics
Albuterol is rapidly and well absorbed following oral administration.
In studies involving normal volunteers, the mean steady-state peak and trough plasma levels of albuterol were 6.7 and 3.8 ng/mL, respectively, following dosing with a 2 mg albuterol tablet every 6 hours and 14.8 and 8.6 ng/mL, respectively following dosing with a 4 mg albuterol tablet every 6 hours. Maximum albuterol plasma levels are usually obtained between 2 and 3 hours after dosing, and the elimination half-life is 5 to 6 hours. These data indicate that albuterol administered orally is dose proportional and exhibits dose independent pharmacokinetics.
It has been shown that administration of a 4 mg albuterol extended-release tablets every 12 hours and 2 mg albuterol tablets every 6 hours for 5 days gave comparable peak albuterol levels and similar extent of absorption at steady state.
In other studies, the analysis of urine samples of patients given tritiated albuterol (4 to 10 mg) orally showed that 65% to 90% of the dose was excreted over 3 days, with the majority of the dose being excreted within the first 24 hours. Sixty percent of this radioactivity was shown to be the metabolite. Feces collected over this period contained 4% of the administered dose.
Clinical Trials
In controlled clinical trials in patients with asthma, the onset of improvement in pulmonary function, as measured by maximum midexpiratory flow rate (MMEF), was noted within 30 minutes after a dose of albuterol tablets, with peak improvement occurring between 2 and 3 hours. In controlled clinical trials in which measurements were conducted for 6 hours, significant clinical improvement in pulmonary function (defined as maintaining a 15% or more increase in FEV 1 and a 20% or more increase in MMEF over baseline values) was observed in 60% of patients at 4 hours and in 40% at 6 hours. In other single-dose, controlled clinical trials, clinically significant improvement was observed in at least 40% of the patients at 8 hours with the 4 mg albuterol tablet. No decrease in the effectiveness of albuterol tablets has been reported in patients who received long-term treatment with the drug in uncontrolled studies for periods up to 6 months.
In another controlled clinical study in asthmatic patients, it has been demonstrated that the initiation of therapy with either the 4 mg albuterol extended-release tablets dosed every 12 hours or the 2 mg albuterol tablet dosed every 6 hours, achieve therapeutically comparable effects.
HOW SUPPLIED
Each albuterol tablet, USP for oral administration contains 2 mg or 4 mg of albuterol as 2.4 mg or 4.8 mg of albuterol sulfate, USP respectively.
Albuterol tablets USP, 2 mg are white to off white colored, round shaped, flat faced, beveled edge uncoated tablets debossed with '10' on upper half of score line and '61' on lower half of score line on one side and plain on other side and are supplied as follows:
NDC 70710-1061-1 in bottle of 100 tablets with child-resistant closure
Albuterol tablets USP, 4 mg are white to off white colored, round shaped, flat faced, beveled edge uncoated tablets debossed with '10' on upper half of score line and '62' on lower half of score line on one side and plain on other side and are supplied as follows:
NDC 70710-1062-1 in bottle of 100 tablets with child-resistant closure
NDC 70710-1062-5 in bottle of 500 tablets
Store at 20° to 25°C (68° to 77°F) [See USP Controlled Room Temperature]. Protect from light.
Dispense in a tight, light-resistant container as defined in the USP using a child-resistant closure.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
Please address medical inquiries to, MedicalAffairs@zydususa.com or Tel.: 1-877-993-8779.