Get your patient on Desmopressin Acetate - Desmopressin Acetate tablet (Desmopressin Acetate)
Desmopressin Acetate - Desmopressin Acetate tablet prescribing information
INDICATIONS AND USAGE
Central Diabetes Insipidus
Desmopressin acetate tablets are indicated as antidiuretic replacement therapy in the management of central diabetes insipidus and for the management of the temporary polyuria and polydipsia following head trauma or surgery in the pituitary region. Desmopressin acetate is ineffective for the treatment of nephrogenic diabetes insipidus.
Patients were selected for therapy based on the diagnosis by means of the water deprivation test, the hypertonic saline infusion test, and/or response to antidiuretic hormone. Continued response to desmopressin acetate can be monitored by measuring urine volume and osmolality.
Primary Nocturnal Enuresis
Desmopressin acetate tablets are indicated for the management of primary nocturnal enuresis. Desmopressin acetate may be used alone or as an adjunct to behavioral conditioning or other non-pharmacologic intervention.
DOSAGE AND ADMINISTRATION
The dosage of desmopressin acetate tablets must be determined for each individual patient and adjusted according to the diurnal pattern of response. Response should be estimated by two parameters: adequate duration of sleep and adequate, not excessive, water turnover. Patients previously on intranasal desmopressin acetate therapy should begin tablet therapy twelve hours after the last intranasal dose. During the initial dose titration period, patients should be observed closely and appropriate safety parameters measured to assure adequate response. Patients should be monitored at regular intervals during the course of desmopressin acetate tablet therapy to assure adequate antidiuretic response. Modifications in dosage regimen should be implemented as necessary to assure adequate water turnover. Fluid restriction should be observed (See WARNINGS , PRECAUTIONS, Pediatric Use and Geriatric Use ).
Adults and Children
It is recommended that patients be started on doses of 0.05 mg (1/2 of the 0.1 mg tablet) two times a day and individually adjusted to their optimum therapeutic dose. Most patients in clinical trials found that the optimal dosage range is 0.1 mg to 0.8 mg daily, administered in divided doses. Each dose should be separately adjusted for an adequate diurnal rhythm of water turnover. Total daily dosage should be increased or decreased in the range of 0.1 mg to 1.2 mg divided into two or three daily doses as needed to obtain adequate antidiuresis. See Pediatric Use subsection for special considerations when administering desmopressin acetate to pediatric diabetes insipidus patients.
Geriatric Use
This drug is known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function. (See CLINICAL PHARMACOLOGY, Human Pharmacokinetics , CONTRAINDICATIONS , and PRECAUTIONS, Geriatric Use ).
Primary Nocturnal Enuresis
The dosage of desmopressin acetate tablets must be determined for each individual patient and adjusted according to response. Patients previously on intranasal desmopressin acetate therapy can begin tablet therapy the night following (24 hours after) the last intranasal dose. The recommended initial dose for patients age 6 years and older is 0.2 mg at bedtime. The dose may be titrated up to 0.6 mg to achieve the desired response. Fluid restriction should be observed, and fluid intake should be limited to a minimum from 1 hour before desmopressin administration, until the next morning, or at least 8 hours after administration. (See WARNINGS , PRECAUTIONS, Pediatric Use and Geriatric Use ).
CONTRAINDICATIONS
Desmopressin acetate tablets are contraindicated in individuals with known hypersensitivity to desmopressin acetate or to any of the components of desmopressin acetate tablets.
Desmopressin acetate is contraindicated in patients with moderate to severe renal impairment (defined as a creatinine clearance below 50mL/min).
Desmopressin acetate is contraindicated in patients with hyponatremia or a history of hyponatremia.
ADVERSE REACTIONS
Infrequently, high doses of the intranasal formulations of desmopressin acetate and desmopressin acetate injection have produced transient headache, nausea, flushing and mild abdominal cramps. These symptoms have disappeared with reduction in dosage.
Central Diabetes Insipidus
In long-term clinical studies in which patients with diabetes insipidus were followed for periods up to 44 months of desmopressin acetate tablet therapy, transient increases in AST (SGOT) no higher than 1.5 times the upper limit of normal were occasionally observed. Elevated AST (SGOT) returned to the normal range despite continued use of desmopressin acetate tablets.
Primary Nocturnal Enuresis
The only adverse event occurring in ≥ 3% of patients in controlled clinical trials with desmopressin acetate tablets that was probably, possibly, or remotely related to study drug was headache (4% desmopressin acetate, 3% placebo).
Other
The following adverse events have been reported; however, their relationship to desmopressin acetate has not been established: abnormal thinking, diarrhea, and edema-weight gain.
See WARNINGS for the possibility of water intoxication and hyponatremia.
Post Marketing: There have been rare reports of hyponatremic convulsions associated with concomitant use with the following medications: oxybutinin and imipramine.
To report SUSPECTED ADVERSE REACTIONS, contact KVK-Tech, Inc. at 1-215-579-1842 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
DESCRIPTION
Desmopressin acetate is a synthetic analogue of the natural pituitary hormone 8- arginine vasopressin (ADH), an antidiuretic hormone affecting renal water conservation. It is chemically defined as follows:
Mol. Wt. 1183.34
Empirical Formula:
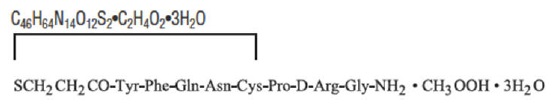
1-(3-mercaptopropionic acid)-8-D-arginine vasopressin monoacetate (salt) trihydrate.
Desmopressin acetate tablets contain either 0.1 or 0.2 mg desmopressin acetate. Inactive ingredients include: corn starch, lactose monohydrate, magnesium stearate and povidone.
CLINICAL PHARMACOLOGY
Desmopressin acetate tablets contain as active substance, desmopressin acetate, a synthetic analogue of the natural hormone arginine vasopressin.
Central Diabetes Insipidus
Dose response studies in patients with diabetes insipidus have demonstrated that oral doses of 0.025 mg to 0.4 mg produced clinically significant antidiuretic effects. In most patients, doses of 0.1 mg to 0.2 mg produced optimal antidiuretic effects lasting up to eight hours. With doses of 0.4 mg, antidiuretic effects were observed for up to 12 hours; measurements beyond 12 hours were not recorded. Increasing oral doses produced dose dependent increases in the plasma levels of desmopressin acetate.
The plasma half-life of desmopressin acetate followed a monoexponential time course with t 1/2 values of 1.5 to 2.5 hours which was independent of dose.
The bioavailability of desmopressin acetate oral tablets is about 5% compared to intranasal desmopressin acetate, and about 0.16% compared to intravenous desmopressin acetate. The time to reach maximum plasma desmopressin acetate levels ranged from 0.9 to 1.5 hours following oral or intranasal administration, respectively. Following administration of desmopressin acetate tablets, the onset of antidiuretic effect occurs at around 1 hour, and it reaches a maximum at about 4 to 7 hours based on the measurement of increased urine osmolality.
The use of desmopressin acetate tablets in patients with an established diagnosis will result in a reduction in urinary output with an accompanying increase in urine osmolality. These effects usually will allow resumption of a more normal life style, with a decrease in urinary frequency and nocturia.
There are reports of an occasional change in response to the intranasal formulations of desmopressin acetate (desmopressin acetate Nasal Spray and desmopressin acetate Rhinal Tube). Usually, the change occurred over a period of time greater than six months. This change may be due to decreased responsiveness, or to shortened duration of effect. There is no evidence that this effect is due to the development of binding antibodies, but may be due to a local inactivation of the peptide. No lessening of effect was observed in the 46 patients who were treated with desmopressin acetate tablets for 12 to 44 months and no serum antibodies to desmopressin were detected.
The change in structure of arginine vasopressin to desmopressin acetate resulted in less vasopressor activity and decreased action on visceral smooth muscle relative to enhanced antidiuretic activity. Consequently, clinically effective antidiuretic doses are usually below the threshold for effects on vascular or visceral smooth muscle. In the four long-term studies of desmopressin acetate tablets, no increases in blood pressure in 46 patients receiving desmopressin acetate tablets for periods of 12 to 44 months were reported.
In one study, the pharmacodynamic characteristics of desmopressin acetate tablets and intranasal formulation were compared during an 8-hour dosing interval at steady state. The doses administered to 36 hydrated (water loaded) healthy male adult volunteers every 8 hours were 0.1, 0.2, 0.4 mg orally and 0.01 mg intranasally by rhinal tube. The results are shown in the following table:
| Treatment | Total Urine Volume in mL | Maximum Urine Osmolality in mOsm/kg |
| 0.1 mg PO q8h | -3689.3 (149.6) | 514.8 (21.9) |
| 0.2 mg PO q8h | -4429.9 (149.6) | 686.3 (21.9) |
| 0.4 mg PO q8h | -4998.8 (149.6) | 769.3 (21.9) |
| 0.01 mg IN q8h | -4844.9 (149.6) | 754.1 (21.9) |
(SE) = Standard error of the mean
With respect to the mean values of total urine volume decrease and maximum urine osmolality increase from baseline, the 90% confidence limits estimated that the 0.4 mg and 0.2 mg oral dose produced between 95% and 110% and 84% to 99% of pharmacodynamic activity, respectively, when compared to the 0.01 mg intranasal dose.
While both the 0.2 mg and 0.4 mg oral doses are considered pharmacodynamically similar to the 0.01 mg intranasal dose, the pharmacodynamic data on an inter-subject basis was highly variable and, therefore, individual dosing is recommended.
In another study in diabetes insipidus patients, the pharmacodynamic characteristics of desmopressin acetate tablets and intranasal formulations were compared over a 12-hour period. Ten fluid-controlled patients under age 18 were administered tablet doses of 0.2 mg and 0.4 mg, and intranasal doses of 0.01 mg and 0.02 mg.
| Treatment | Urine Volume in mL/min | Maximum Urine Osmolality in mOsm/kg |
| 0.01 mg IN | 0.3 (0.15) | 717.0 (224.63) |
| 0.02 mg IN | 0.3 (0.25) | 761.8 (298.82) |
| 0.2 mg PO | 0.3 (0.12) | 678.3 (147.91) |
| 0.4 mg PO | 0.2 (0.15) | 787.2 (73.34) |
(SD) = Standard Deviation
All four dose formulations (0.01 mg IN, 0.02 mg IN, 0.2 mg PO and 0.4 mg PO) have a similar, pronounced pharmacodynamic effect on urine volume and urine osmolality. At two hours after study drug administration, mean urine volume was 4 mL/min and urine osmolality was >500 mOsm/kg. Mean plasma osmolality remained relatively constant over the time course recorded (0 to 12 hours). A statistical separation from baseline did not occur at any dose or time point. In these patients, the 0.2 mg tablets and the 0.01 mg intranasal spray exhibited similar pharmacodynamic profiles as did the 0.4 mg tablets and the 0.02 mg intranasal spray formulation. In another study of adult diabetes insipidus patients previously controlled on desmopressin acetate intranasal spray, after one week of self-titration from spray to tablets, patients' diuresis was controlled with 0.1 mg desmopressin acetate tablets three times a day.
Primary Nocturnal Enuresis in Pediatrics
Two double-blind, randomized, placebo-controlled studies were conducted in 340 patients with primary nocturnal enuresis. Patients were 5-17 years old, and 72% were males. A total of 329 patients were evaluated for efficacy. Patients were evaluated over a two-week baseline period in which the average number of wet nights was 10 (range 4-14). Patients were then randomized to receive 0.2, 0.4, or 0.6 mg of desmopressin acetate or placebo. The pooled results after two weeks are shown in the following table:
| Placebo (n = 85) | 0.2 mg/day (n = 79) | 0.4 mg/day (n = 82) | 0.6 mg/day (n = 83) | |
| Baseline | 10(0.3) | 11 (0.3) | 10 (0.3) | 10 (0.3) |
| Reduction from Baseline | 1 (0.3) | 3 (0.4) | 3 (0.4) | 4 (0.4) |
| Percent Reduction from Baseline | 10% | 27% | 30% | 40% |
| p-value vs placebo | ----- | <0.05 | <0.05 | <0.05 |
Patients treated with desmopressin acetate tablets showed a statistically significant reduction in the number of wet nights compared to placebo-treated patients. A greater response was observed with increasing doses up to 0.6 mg.
In a six month, open-label extension study, patients completing the placebo-controlled studies were started on 0.2 mg/day desmopressin acetate, and the dose was progressively increased until the optimal response was achieved (maximum dose 0.6 mg/day). A total of 230 patients were evaluated for efficacy; the average number of wet nights/2 weeks during the untreated baseline period was 10 (range 4-14), and the average duration (SD) of treatment was 4.2 (1.8) months. Twenty-five (25) patients (11%) achieved a complete or near complete response (≤2 wet nights/2 weeks) and did not require titration to the 0.6 mg/day dose. The majority of patients (198 of 230, 86%) were titrated to the highest dose. When all dose groups were combined, 128 (56%) showed at least a 50% reduction from baseline in the number of wet nights/2 weeks, while 87 (38%) patients achieved a complete or near complete response.
Human Pharmacokinetics
Desmopressin acetate is mainly excreted in the urine. A pharmacokinetic study conducted in healthy volunteers and patients with mild, moderate, and severe renal impairment (n=24, 6 subjects in each group) receiving single dose desmopressin acetate (2 mcg) injection demonstrated a difference in desmopressin acetate terminal half- life. Terminal half-life significantly increased from 3 hours in normal healthy patients to 9 hours in patients with severe renal impairment (See CONTRAINDICATIONS ).
HOW SUPPLIED
Desmopressin Acetate Tablets, 0.1 mg, are white to off-white, modified oval shape, biconvex tablets debossed “A” above deep break line and “18” below deep break line on one side and plain on the other side. The tablets are supplied as follows:
Bottles of 100: NDC 10702-169-01
Desmopressin Acetate Tablets, 0.2 mg, are white to off-white, round shape, biconvex tablets debossed “A” above deep break line and “19” below deep break line on one side and plain on the other side. The tablets are supplied as follows:
Bottles of 100: NDC 10702-170-01
Store at 20°C to 25°C (68°F to 77°F); excursions permitted within 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
Avoid exposure to excessive heat or light.
Dispense in a tight, light-resistant container, as defined in USP, with a child-resistant closure.
Keep out of the reach of children.
Manufactured by: KVK-Tech, Inc. 110 Terry Drive Newtown, PA 18940
Manufacturer’s code: 10702 Item ID #: 6299/01 Rev.: 02/2019