Get your patient on Diclofenac Sodium - Diclofenac Sodium gel (Diclofenac Sodium)
Diclofenac Sodium - Diclofenac Sodium gel prescribing information
WARNING: RISK OF SERIOUS CARDIOVASCULAR AND GASTROINTESTINAL EVENTS
Cardiovascular Thrombotic Events
- Nonsteroidal anti-inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use [see Warnings and Precautions (5.4 )] .
- Diclofenac sodium is contraindicated in the setting of coronary artery bypass graft (CABG) surgery [see Contraindications (4 ) and Warnings and Precautions (5.4 )] .
Gastrointestinal Bleeding, Ulceration, and Perforation
- N SAIDs cause an increased risk of serious gastrointestinal (GI) adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients and patients with a prior history of peptic ulcer disease and/or GI bleeding are at a greater risk for serious GI events [see Warnings and Precautions (5.5 )] .
Warnings and Precautions
Serious Skin Reactions (5.3) (7/2024)
INDICATIONS AND USAGE
Diclofenac sodium topical gel is indicated for the topical treatment of actinic keratosis (AK).
DOSAGE AND ADMINISTRATION
Use the lowest effective dosage for the shortest duration consistent with individual patient treatment goals [see Warnings and Precautions (5 )] .
Apply diclofenac sodium topical gel gently to lesion areas twice daily to adequately cover each lesion. Use 0.5 g of gel (pea size) on each 5 cm x 5 cm lesion site. The recommended duration of therapy is from 60 days to 90 days. Complete healing of the lesion(s) or optimal therapeutic effect may not be evident for up to 30 days following cessation of therapy. Lesions that do not respond to therapy should be re-evaluated and management reconsidered.
Avoid contact of diclofenac sodium topical gel with eyes and mucous membranes.
DOSAGE FORMS AND STRENGTHS
Topical gel, 3%. Each gram of diclofenac sodium topical gel contains 30 mg of diclofenac sodium USP, in a clear, transparent, colorless to slightly yellow gel base. Diclofenac sodium topical gel is supplied in 100 g tubes.
USE IN SPECIFIC POPULATIONS
Pregnancy
Risk Summary Use of NSAIDs, including diclofenac sodium can cause premature closure of the fetal ductus arteriosus and fetal renal dysfunction leading to oligohydramnios and, in some cases, neonatal renal impairment. Because of these risks, limit dose and duration of diclofenac sodium use between about 20 and 30 weeks of gestation and avoid diclofenac sodium use at about 30 weeks of gestation and later in pregnancy.
Oligohydramnios/Neonatal Renal Impairment Use of NSAIDs at about 20 weeks gestation or later in pregnancy has been associated with cases of fetal renal dysfunction leading to oligohydramnios, and in some cases, neonatal renal impairment.
Premature Closure of Fetal Ductus Arteriosus Use of NSAIDs, including diclofenac sodium at about 30 weeks gestation or later in pregnancy increases the risk of premature closure of the fetal ductus arteriosus.
Data from observational studies regarding other potential embryofetal risks of NSAID use in women in the first or second trimesters of pregnancy are inconclusive.
In animal reproduction studies, no evidence of malformations was observed in mice, rats, or rabbits given diclofenac during the period of organogenesis at doses at least 15 times, the maximum recommended human dose (MRHD) of diclofenac sodium topical gel (see Data) . Based on published animal data, prostaglandins have been shown to have an important role in endometrial vascular permeability, blastocyst implantation, and decidualization, and administration of prostaglandin synthesis inhibitors such as diclofenac sodium, resulted in increased pre- and post-implantation loss. Prostaglandins also have been shown to have an important role in fetal kidney development. In published animal studies, prostaglandin synthesis inhibitors have been reported to impair kidney development when administered at clinically relevant doses.
The background risk of major birth defects and miscarriage for the indicated population(s) is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Clinical Considerations Fetal/Neonatal Adverse Reactions Premature Closure of Fetal Ductus Arteriosus Avoid use of NSAIDs in women at about 30 weeks gestation and later in pregnancy, because NSAIDs, including diclofenac sodium can cause premature closure of the fetal ductus arteriosus.
Oligohydramnios/Neonatal Renal Impairment If after careful consideration of alternative treatment options for actinic keratosis, an NSAID is necessary at about 20 weeks gestation or later in pregnancy, limit the use to the lowest effective dose and shortest duration possible. If diclofenac sodium treatment extends beyond 48 hours, consider monitoring with ultrasound for oligohydramnios. If oligohydramnios occurs, discontinue diclofenac sodium and follow up according to clinical practice .
Labor or Delivery There are no studies on the effects of diclofenac sodium during labor or delivery. In animal studies, NSAIDS, including diclofenac, inhibit prostaglandin synthesis, cause delayed parturition, and increase the incidence of stillbirth.
Data Human Data Premature Closure of Fetal Ductus Arteriosus Published literature reports that the use of NSAIDs at about 30 weeks of gestation and later in pregnancy may cause premature closure of the fetal ductus arteriosus.
Oligohydramnios/Neonatal Renal Impairment Published studies and postmarketing reports describe maternal NSAID use at about 20 weeks gestation or later in pregnancy associated with fetal renal dysfunction leading to oligohydramnios, and in some cases, neonatal renal impairment. These adverse outcomes are seen, on average, after days to weeks of treatment, although oligohydramnios has been infrequently reported as soon as 48 hours after NSAID initiation. In many cases, but not all, the decrease in amniotic fluid was transient and reversible with cessation of the drug. There have been a limited number of case reports of maternal NSAID use and neonatal renal dysfunction without oligohydramnios, some of which were irreversible. Some cases of neonatal renal dysfunction required treatment with invasive procedures, such as exchange transfusion or dialysis.
Methodological limitations of these postmarketing studies and reports include lack of a control group; limited information regarding dose, duration, and timing of drug exposure; and concomitant use of other medications. These limitations preclude establishing a reliable estimate of the risk of adverse fetal and neonatal outcomes with maternal NSAID use.
Because the published safety data on neonatal outcomes involved mostly preterm infants, the generalizability of certain reported risks to the full-term infant exposed to NSAIDs through maternal use is uncertain.
Animal Data The multiples provided in this labeling are based on an MRHD that assumes 10% bioavailability following topical application of 2 g diclofenac sodium topical gel per day (1 mg/kg diclofenac sodium).
Reproductive studies performed with diclofenac sodium alone at oral doses up to 20 mg/kg/day (15 times the MRHD based on body surface area (BSA) comparisons) in mice, 10 mg/kg/day (15 times the MRHD based on BSA comparisons) in rats, and 10 mg/kg/day (30 times the MRHD based on BSA comparisons) in rabbits have revealed no evidence of malformations despite the induction of maternal toxicity. In rats, maternally toxic doses were associated with dystocia, prolonged gestation, reduced fetal weights and growth, and reduced fetal survival. Diclofenac has been shown to cross the placental barrier in mice and rats.
Lactation
Risk Summary Data from published literature cases with oral preparations of diclofenac indicate the presence of small amounts of diclofenac in human milk . There are no data on the effects on the breastfed infant, or the effects on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for diclofenac sodium topical gel and any potential adverse effects on the breastfed infant from the diclofenac sodium topical gel or from the underlying maternal condition.
Data One woman treated orally with a diclofenac salt, 150 mg/day, had a milk diclofenac level of 100 mcg/L, equivalent to an infant dose of about 0.03 mg/kg/day. Diclofenac was not detectable in breast milk in 12 women using diclofenac (after either 100 mg/day orally for 7 days or a single 50 mg intramuscular dose administered in the immediate postpartum period). The systemic bioavailability after topical application of diclofenac sodium topical gel is lower than after oral dosing [see Clinical Pharmacology (12.3 )].
Females and Males of Reproductive Potential
Female Infertility Based on the mechanism of action, the use of prostaglandin mediated NSAIDs, including diclofenac sodium may delay or prevent rupture of ovarian follicles, which has been associated with reversible infertility in some women [see Clinical Pharmacology (12.1 )] .
Published animal studies have shown that administration of prostaglandin synthesis inhibitors has the potential to disrupt prostaglandin-mediated follicular rupture required for ovulation. Small studies in women treated with NSAIDs have also shown a reversible delay in ovulation. Consider withdrawal of NSAIDs, including diclofenac sodium in women who have difficulties conceiving or who are undergoing investigation of infertility.
Pediatric Use
Actinic keratoses is not a condition seen within the pediatric population. Diclofenac sodium should not be used by children.
Geriatric Use
Elderly patients, compared to younger patients, are at greater risk for NSAID-associated serious cardiovascular, gastrointestinal, and/or renal adverse reactions. If the anticipated benefit for the elderly patient outweighs these potential risks, start dosing at the low end of the dosing range, and monitor patients for adverse effects [see Warnings and Precautions (5.4 , 5.5 , 5.6 , 5.9 , 5.14 )].
Of the 211 subjects treated with diclofenac sodium in controlled clinical trials, 143 subjects were 65 years of age and over. Of those 143 subjects, 55 subjects were 75 years of age and over. No overall differences in safety or effectiveness were observed between these subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
CONTRAINDICATIONS
Diclofenac sodium topical gel is contraindicated in the following patients:
- With known hypersensitivity (e.g., anaphylactic reactions and serious skin reactions) to diclofenac or any components of the drug product [see Warnings and Precautions (5.1 , 5.3 , 5.10 ) and Description (11 )]
- With the history of asthma, urticaria, or other allergic type reactions after taking aspirin or other NSAIDs. Severe, sometimes fatal, anaphylactic reactions to NSAIDs have been reported in such patients [see Warnings and Precautions (5.1 , 5.2 )]
- Application on damaged skin resulting from any etiology, including exudative dermatitis, eczema, infected lesions, burns or wounds [see Warnings and Precautions (5.3 )]
- In the setting of coronary bypass graft (CABG) surgery [see Warnings and Precautions (5.4 )]
WARNINGS AND PRECAUTIONS
Anaphylactic Reactions
Exacerbation of Asthma Related to Aspirin Sensitivity
A subpopulation of patients with asthma may have aspirin-sensitive asthma which may include chronic rhinosinusitis complicated by nasal polyps; severe, potentially fatal bronchospasm; and/or intolerance to aspirin and other NSAIDs. Because cross-reactivity between aspirin and other NSAIDs has been reported in such aspirin-sensitive patients, diclofenac sodium is contraindicated in patients with this form of aspirin sensitivity. When diclofenac sodium is used in patients with preexisting asthma (without known aspirin sensitivity), monitor patients for changes in the signs and symptoms of asthma.
Serious Skin Reactions
NSAIDs, including diclofenac, can cause serious skin adverse reactions such as exfoliative dermatitis, Stevens-Johnson Syndrome (SJS), and toxic epidermal necrolysis (TEN), which can be fatal. NSAIDs can also cause fixed drug eruption (FDE). FDE may present as a more severe variant known as generalized bullous fixed drug eruption (GBFDE), which can be life-threatening. These serious events may occur without warning. Inform patients about the signs and symptoms of serious skin reactions, and to discontinue the use of diclofenac sodium topical gel at the first appearance of skin rash or any other sign of hypersensitivity. Diclofenac sodium topical gel is contraindicated in patients with previous serious skin reactions to NSAIDs. Do not apply diclofenac sodium topical gel to open skin wounds, infections, or exfoliative dermatitis, as it may affect absorption and tolerability of the drug [see Contraindications (4 ) ] .
Cardiovascular Thrombotic Events
Clinical trials of several COX-2 selective and nonselective NSAIDs of up to three years duration have shown an increased risk of serious cardiovascular (CV) thrombotic events, including myocardial infarction (MI) and stroke, which can be fatal. Based on available data, it is unclear that the risk for CV thrombotic events is similar for all NSAIDs. The relative increase in serious CV thrombotic events over baseline conferred by NSAID use appears to be similar in those with and without known CV disease or risk factors for CV disease. However, patients with known CV disease or risk factors had a higher absolute incidence of excess serious CV thrombotic events, due to their increased baseline rate. Some observational studies found that this increased risk of serious CV thrombotic events began as early as the first weeks of treatment. The increase in CV thrombotic risk has been observed most consistently at higher doses.
To minimize the potential risk for an adverse CV event in NSAID-treated patients, use the lowest effective dose for the shortest duration possible. Physicians and patients should remain alert for the development of such events, throughout the entire treatment course, even in the absence of previous CV symptoms. Patients should be informed about the symptoms of serious CV events and the steps to take if they occur.
There is no consistent evidence that concurrent use of aspirin mitigates the increased risk of serious CV thrombotic events associated with NSAID use. The concurrent use of aspirin and an NSAID, such as diclofenac, increases the risk of serious gastrointestinal (GI) events.
Status Post Coronary Artery Bypass Graft (CABG) Surgery Two controlled clinical trials of a COX-2 selective NSAID for the treatment of pain in the first 10–14 days following CABG surgery found an increased incidence of myocardial infarction and stroke. NSAIDs are contraindicated in the setting of CABG.
Post-MI Patients Observational studies conducted in the Danish National Registry have demonstrated that patients treated with NSAIDs in the post-MI period were at increased risk of reinfarction, CV-related death, and all-cause mortality beginning in the first week of treatment. In this same cohort, the incidence of death in the first-year post MI was 20 per 100 person years in NSAID-treated patients compared to 12 per 100 person years in non-NSAID exposed patients. Although the absolute rate of death declined somewhat after the first year post-MI, the increased relative risk of death in NSAID users persisted over at least the next four years of follow-up.
Avoid the use of diclofenac sodium topical gel in patients with a recent MI unless the benefits are expected to outweigh the risk of recurrent CV thrombotic events. If diclofenac sodium topical gel is used in patients with a recent MI, monitor patients for signs of cardiac ischemia.
Gastrointestinal Bleeding, Ulceration, and Perforation
NSAIDs, including diclofenac, cause serious GI adverse events including inflammation, bleeding, ulceration, and perforation of the esophagus, stomach, small intestine, or large intestine, which can be fatal. These serious adverse events can occur at any time, with or without warning symptoms, in patients treated with NSAIDs.
Only one in five patients who develop a serious upper GI adverse event on NSAID therapy is symptomatic. Upper GI ulcers, gross bleeding, or perforation caused by NSAIDs occurred in approximately 1% of patients treated for 3 to 6 months, and in about 2% to 4% of patients treated for one year. However, even short-term NSAID therapy is not without risk.
Risk Factors for GI Bleeding, Ulceration, and Perforation Patients with a prior history of peptic ulcer disease and/or GI bleeding who used NSAIDs had a greater than 10-fold increased risk for developing a GI bleed compared to patients without these risk factors. Other factors that increase the risk of GI bleeding in patients treated with NSAIDs include longer duration of NSAID therapy; concomitant use of oral corticosteroids, aspirin, anticoagulants, or selective serotonin reuptake inhibitors (SSRIs); smoking; use of alcohol; older age; and poor general health status. Most postmarketing reports of fatal GI events occurred in elderly or debilitated patients. Additionally, patients with advanced liver disease and/or coagulopathy are at increased risk for GI bleeding.
Strategies to Minimize the GI Risks in NSAID-Treated Patients:
- Use the lowest effective dosage for the shortest possible duration.
- Avoid administration of more than one NSAID at a time.
- Avoid use in patients at higher risk unless benefits are expected to outweigh the increased risk of bleeding. For such patients, as well as those with active GI bleeding, consider alternate therapies other than NSAIDs.
- Remain alert for signs and symptoms of GI ulceration and bleeding during NSAID therapy.
- If a serious GI adverse event is suspected, promptly initiate evaluation and treatment, and discontinue diclofenac sodium topical gel until a serious GI adverse event is ruled out.
- In the setting of concomitant use of low-dose aspirin for cardiac prophylaxis, monitor patients more closely for evidence of GI bleeding [see Drug Interactions (7 )] .
Hepatotoxicity
In clinical trials with diclofenac sodium topical gel, 2% to 3% of subjects had elevations of liver function tests (LFTs) [see Clinical Trials Experience (6.1 )]. To minimize the potential risk for an adverse liver-related event in patients treated with diclofenac sodium topical gel use the lowest effective dose for the shortest duration possible. Exercise caution when prescribing diclofenac sodium topical gel with concomitant drugs that are known to be potentially hepatotoxic (e.g., acetaminophen, antibiotics, anti-epileptics).
Physicians should measure transaminases at baseline and periodically in patients receiving long-term therapy with diclofenac, because severe hepatotoxicity may develop without a prodrome of distinguishing symptoms. The optimum times for making the first and subsequent transaminase measurements are not known. Based on clinical trial data and postmarketing experiences, transaminases should be monitored within 4 to 8 weeks after initiating treatment with diclofenac. However, severe hepatic reactions can occur at any time during treatment with diclofenac.
If abnormal liver tests persist or worsen, if clinical signs and/or symptoms consistent with liver disease develop, or if systemic manifestations occur (e.g., eosinophilia, rash, abdominal pain, diarrhea, dark urine, etc.), diclofenac sodium topical gel should be discontinued immediately.
Inform patients of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, diarrhea, pruritus, jaundice, right upper quadrant tenderness, and "flu-like" symptoms). If clinical signs and symptoms consistent with liver disease develop, or if systemic manifestations occur (e.g., eosinophilia, rash, etc.), discontinue diclofenac sodium topical gel immediately, and perform a clinical evaluation of the patient.
Hypertension
NSAIDs, including diclofenac sodium, can lead to new onset of hypertension or worsening of pre-existing hypertension, either of which may contribute to the increased incidence of CV events. Patients taking angiotensin converting enzyme (ACE) inhibitors, thiazide diuretics, or loop diuretics may have impaired response to these therapies when taking NSAIDs [see Drug Interactions (7 )] .
Monitor blood pressure (BP) during the initiation of NSAID treatment and throughout the course of therapy.
Heart Failure and Edema
The Coxib and traditional NSAID Trialists’ Collaboration meta-analysis of randomized controlled trials demonstrated an approximately two-fold increase in hospitalizations for heart failure in COX-2 selective-treated patients and nonselective NSAID-treated patients compared to placebo-treated patients. In a Danish National Registry study of patients with heart failure, NSAID use increased the risk of MI, hospitalization for heart failure, and death.
Additionally, fluid retention and edema have been observed in some patients treated with NSAIDs. Use of diclofenac may blunt the CV effects of several therapeutic agents used to treat these medical conditions [e.g., diuretics, ACE inhibitors, or angiotensin receptor blockers (ARBs)].
Avoid the use of diclofenac sodium topical gel in patients with severe heart failure unless the benefits are expected to outweigh the risk of worsening heart failure. If diclofenac sodium topical gel is used in patients with severe heart failure, monitor patients for signs of worsening heart failure.
Renal Toxicity and Hyperkalemia
Renal Toxicity Long-term administration of NSAIDs has resulted in renal papillary necrosis and other renal injury.
Patients at greatest risk of this reaction are those with impaired renal function, dehydration, hypovolemia, heart failure, liver dysfunction, those taking diuretics and ACE inhibitors or ARBs, and the elderly. Discontinuation of NSAID therapy is usually followed by recovery to the pretreatment state.
No information is available from controlled clinical trials regarding the use of diclofenac sodium in patients with advanced renal disease. The renal effects of diclofenac sodium may hasten the progression of renal dysfunction in patients with pre-existing renal disease.
Correct volume status in dehydrated or hypovolemic patients prior to initiating diclofenac sodium topical gel. Monitor renal function in patients with renal or hepatic impairment, heart failure, dehydration, or hypovolemia during use of diclofenac sodium topical gel [see Drug Interactions (7 )]. Avoid the use of diclofenac sodium topical gel in patients with advanced renal disease unless the benefits are expected to outweigh the risk of worsening renal function. If diclofenac sodium topical gel is used in patients with advanced renal disease, monitor patients for signs of worsening renal function.
Hyperkalemia Increases in serum potassium concentration, including hyperkalemia, have been reported with use of NSAIDs, even in some patients without renal impairment. In patients with normal renal function, these effects have been attributed to a hyporeninemic-hypoaldosteronism state.
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) has been reported in patients taking NSAIDs such as diclofenac sodium topical gel. Some of these events have been fatal or life-threatening. DRESS typically, although not exclusively, presents with fever, rash, lymphadenopathy, and/or facial swelling. Other clinical manifestations may include hepatitis, nephritis, hematological abnormalities, myocarditis, or myositis. Sometimes symptoms of DRESS may resemble an acute viral infection. Eosinophilia is often present. Because this disorder is variable in its presentation, other organ systems not noted here may be involved. It is important to note that early manifestations of hypersensitivity, such as fever or lymphadenopathy, may be present even though rash is not evident. If such signs or symptoms are present, discontinue diclofenac sodium topical gel and evaluate the patient immediately.
Fetal Toxicity
Premature Closure of Fetal Ductus Arteriosus Avoid use of NSAIDs, including diclofenac sodium, in pregnant women at about 30 weeks gestation and later. NSAIDs, including diclofenac sodium, increase the risk of premature closure of the fetal ductus arteriosus at approximately this gestational age.
Oligohydramnios/Neonatal Renal Impairment Use of NSAIDs, including diclofenac, at about 20 weeks gestation or later in pregnancy may cause fetal renal dysfunction leading to oligohydramnios and, in some cases, neonatal renal impairment. These adverse outcomes are seen, on average, after days to weeks of treatment, although oligohydramnios has been infrequently reported as soon as 48 hours after NSAID initiation. Oligohydramnios is often, but not always, reversible with treatment discontinuation. Complications of prolonged oligohydramnios may, for example, include limb contractures and delayed lung maturation. In some postmarketing cases of impaired neonatal renal function, invasive procedures such as exchange transfusion or dialysis were required.
If, after careful consideration of alternative treatment options for actinic keratoses, NSAID treatment is necessary between about 20 weeks and 30 weeks gestation, limit diclofenac sodium topical gel use to the lowest effective dose and shortest duration possible.
Consider ultrasound monitoring of amniotic fluid if diclofenac treatment extends beyond 48 hours. Discontinue diclofenac sodium topical gel if oligohydramnios occurs and follow up according to clinical practice [see Use in Specific Populations (8.1 )].
Hematologic Toxicity
Anemia has occurred in NSAID-treated patients. This may be due to occult or gross blood loss, fluid retention, or an incompletely described effect on erythropoiesis. If a patient treated with diclofenac sodium topical gel has any signs or symptoms of anemia, monitor hemoglobin or hematocrit.
NSAIDs, including diclofenac sodium, may increase the risk of bleeding events. Co-morbid conditions such as coagulation disorders, concomitant use of warfarin, other anticoagulants, antiplatelet agents (e.g., aspirin), serotonin reuptake inhibitors (SSRIs) and serotonin norepinephrine reuptake inhibitors (SNRIs) may increase this risk. Monitor these patients for signs of bleeding [see Drug Interactions (7 )].
Masking of Inflammation and Fever
The pharmacological activity of diclofenac sodium in reducing inflammation, and possibly fever, may diminish the utility of diagnostic signs in detecting infections.
Laboratory Monitoring
Photosensitivity
Patients should minimize or avoid exposure to natural or artificial sunlight (tanning beds or UVA/B treatment) while using diclofenac sodium topical gel. If patients need to be outdoors while using diclofenac sodium topical gel they should wear loose-fitting clothes that protect skin from sun exposure and discuss other sun protection measures with their physician. Advise patients to discontinue treatment with diclofenac sodium topical gel at the first evidence of sunburn.
Exposure to Eyes and Mucosal Membranes
Avoid contact of diclofenac sodium with eyes and mucosa. Advise patients that if contact in the eye, or mucosal membranes occurs, immediately wash out the eye or mucosal membranes with water or saline and consult a physician if irritation persists for more than an hour.
Oral Nonsteroidal Anti-inflammatory Drugs
Concomitant use of oral and topical NSAIDs may result in a higher rate of hemorrhage, more frequent abnormal creatinine, urea and hemoglobin. Do not use diclofenac sodium topical gel in combination with an oral NSAID unless the benefit outweighs the risk and periodic laboratory evaluations are conducted.
ADVERSE REACTIONS
The following adverse reactions are discussed in greater detail in other sections of the labeling:
- Anaphylactic Reactions [see Warnings and Precautions (5.1 )]
- Exacerbation of Asthma Related to Aspirin Sensitivity [see Warnings and Precautions (5.2 )]
- Serious Skin Reactions [see Warnings and Precautions (5.3 )]
- Cardiovascular Thrombotic Events [see Warnings and Precautions (5.4 )]
- GI Bleeding, Ulceration and Perforation [see Warnings and Precautions (5.5 )]
- Hepatotoxicity [see Warnings and Precautions (5.6 )]
- Hypertension [see Warnings and Precautions (5.7 )]
- Heart Failure and Edema [see Warnings and Precautions (5.8 )]
- Renal Toxicity and Hyperkalemia [see Warnings and Precautions (5.9 )]
- DRESS [see Warnings and Precautions (5.10 )]
- Hematologic Toxicity [see Warnings and Precautions (5.12 )]
- Photosensitivity [see Warnings and Precautions (5.15 )]
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Of the 423 subjects evaluable for safety in adequate and well-controlled trials, 211 were treated with diclofenac sodium drug product and 212 were treated with a vehicle gel. Eighty-seven percent (87%) of the diclofenac sodium-treated subjects (183 subjects) and 84% of the vehicle-treated subjects (178 subjects) experienced one or more adverse events (AEs) during the trials. The majority of these reactions were mild to moderate in severity and resolved upon discontinuation of therapy.
Of the 211 subjects treated with diclofenac sodium, 172 (82%) experienced AEs involving skin and the application site compared to 160 (75%) vehicle-treated subjects. Application site reactions (ASRs) were the most frequent AEs in both diclofenac sodium-and vehicle-treated groups. Of note, four reactions, contact dermatitis, rash, dry skin and exfoliation (scaling) were significantly more prevalent in the diclofenac sodium group than in the vehicle-treated subjects.
Eighteen percent of diclofenac sodium-treated subjects and 4% of vehicle-treated subjects discontinued from the clinical trials due to adverse events (whether considered related to treatment or not). These discontinuations were mainly due to skin irritation or related cutaneous adverse reactions.
Table 1 below presents the AEs reported at an incidence of >1% for subjects treated with either diclofenac sodium or vehicle (60-and 90-day treatment groups) during the phase 3 trials.
60-day Treatment | 90-day Treatment | |||
Diclofenac Sodium Topical Gel (%) N=48 | Gel vehicle (%) N=49 | Diclofenac Sodium Topical Gel (%) N=114 | Gel vehicle (%) N=114 | |
BODY AS A WHOLE | 21 | 20 | 20 | 18 |
Abdominal Pain | 2 | 0 | 1 | 0 |
Accidental Injury | 0 | 0 | 4 | 2 |
Allergic Reaction | 0 | 0 | 1 | 3 |
Asthenia | 0 | 0 | 2 | 0 |
Back Pain | 4 | 0 | 2 | 2 |
Chest Pain | 2 | 0 | 1 | 0 |
Chills | 0 | 2 | 0 | 0 |
Flu Syndrome | 10 | 6 | 1 | 4 |
Headache | 0 | 6 | 7 | 6 |
Infection | 4 | 6 | 4 | 5 |
Neck Pain | 0 | 0 | 2 | 0 |
Pain | 2 | 0 | 2 | 2 |
CARDIOVASCULAR SYSTEM | 2 | 4 | 3 | 1 |
Hypertension | 2 | 0 | 1 | 0 |
Migraine | 0 | 2 | 1 | 0 |
Phlebitis | 0 | 2 | 0 | 0 |
DIGESTIVE SYSTEM | 4 | 0 | 6 | 8 |
Constipation | 0 | 0 | 0 | 2 |
Diarrhea | 2 | 0 | 2 | 3 |
Dyspepsia | 2 | 0 | 3 | 4 |
METABOLIC AND NUTRITIONAL DISORDERS | 2 | 8 | 7 | 2 |
Creatine Phosphokinase Increased | 0 | 0 | 4 | 1 |
Creatinine Increased | 2 | 2 | 0 | 1 |
Edema | 0 | 2 | 0 | 0 |
Hypercholesteremia | 0 | 2 | 1 | 0 |
Hyperglycemia | 0 | 2 | 1 | 0 |
SGOT Increased | 0 | 0 | 3 | 0 |
SGPT Increased | 0 | 0 | 2 | 0 |
MUSCULOSKELETAL SYSTEM | 4 | 0 | 3 | 4 |
Arthralgia | 2 | 0 | 0 | 2 |
Arthrosis | 2 | 0 | 0 | 0 |
Myalgia | 2 | 0 | 3 | 1 |
NERVOUS SYSTEM | 2 | 2 | 2 | 5 |
Anxiety | 0 | 2 | 0 | 1 |
Dizziness | 0 | 0 | 0 | 4 |
Hypokinesia | 2 | 0 | 0 | 0 |
RESPIRATORY SYSTEM | 8 | 8 | 7 | 6 |
Asthma | 2 | 0 | 0 | 0 |
Dyspnea | 2 | 0 | 2 | 0 |
Pharyngitis | 2 | 8 | 2 | 4 |
Pneumonia | 2 | 0 | 0 | 1 |
Rhinitis | 2 | 2 | 2 | 2 |
Sinusitis | 0 | 0 | 2 | 0 |
SKIN AND APPENDAGES | 75 | 86 | 86 | 71 |
Acne | 0 | 2 | 0 | 1 |
Application Site Reaction | 75 | 71 | 84 | 70 |
Acne | 0 | 4 | 1 | 0 |
Alopecia | 2 | 0 | 1 | 1 |
Contact Dermatitis | 19 | 4 | 33 | 4 |
Dry Skin | 27 | 12 | 25 | 17 |
Edema | 4 | 0 | 3 | 0 |
Exfoliation | 6 | 4 | 24 | 13 |
Hyperesthesia | 0 | 0 | 3 | 1 |
Pain | 15 | 22 | 26 | 30 |
Paresthesia | 8 | 4 | 20 | 20 |
Photosensitivity Reaction | 0 | 2 | 3 | 0 |
Pruritus | 31 | 59 | 52 | 45 |
Rash | 35 | 20 | 46 | 17 |
Vesiculobullous Rash | 0 | 0 | 4 | 1 |
Contact Dermatitis | 2 | 0 | 0 | 0 |
Dry Skin | 0 | 4 | 3 | 0 |
Herpes Simplex | 0 | 2 | 0 | 0 |
Maculopapular Rash | 0 | 2 | 0 | 0 |
Pain | 2 | 2 | 1 | 0 |
Pruritus | 4 | 6 | 4 | 1 |
Rash | 2 | 10 | 4 | 0 |
Skin Carcinoma | 0 | 6 | 2 | 2 |
Skin Nodule | 0 | 2 | 0 | 0 |
Skin Ulcer | 2 | 0 | 1 | 0 |
SPECIAL SENSES | 2 | 0 | 4 | 2 |
Conjunctivitis | 2 | 0 | 4 | 1 |
Eye Pain | 0 | 2 | 2 | 0 |
UROGENITAL SYSTEM | 0 | 0 | 4 | 5 |
Hematuria | 0 | 0 | 2 | 1 |
OTHER | 0 | 0 | 0 | 3 |
Procedure | 0 | 0 | 0 | 3 |
Skin and Appendages Adverse Events Reported for Diclofenac Sodium Topical Gel at Less Than 1% Incidence in the Phase 3 Studies: skin hypertrophy, paresthesia, seborrhea, urticaria, application site reactions (skin carcinoma, hypertonia, skin hypertrophy lacrimation disorder, maculopapular rash, purpuric rash, vasodilation).
Adverse Reactions Reported for Oral Diclofenac Dosage Form (not Diclofenac Sodium Topical Gel): •Incidence Greater than 1% marked with asterisk.
Body as a Whole: abdominal pain or cramps•, headache•, fluid retention•, abdominal distention•, malaise, swelling of lips and tongue, photosensitivity, anaphylaxis, anaphylactoid reactions, chest pain.
Cardiovascular: hypertension, congestive heart failure, palpitations, flushing, tachycardia, premature ventricular contractions, myocardial infarction, hypotension.
Digestive: diarrhea•, indigestion•, nausea•, constipation•, flatulence•, liver test abnormalities•, PUB•, i.e., peptic ulcer, with or without bleeding and/or perforation, or bleeding without ulcer, vomiting, jaundice, melena, esophageal lesions, aphthous stomatitis, dry mouth and mucous membranes, bloody diarrhea, hepatitis, hepatic necrosis, cirrhosis, hepatorenal syndrome, appetite change, pancreatitis with or without concomitant hepatitis, colitis, intestinal perforation.
Hemic and Lymphatic: hemoglobin decrease, leukopenia, thrombocytopenia, eosinophilia, hemolytic anemia, aplastic anemia, agranulocytosis, purpura, allergic purpura, bruising.
Metabolic and Nutritional Disorders: azotemia, hypoglycemia, weight loss.
Nervous System: dizziness•, insomnia, drowsiness, depression, diplopia, anxiety, irritability, aseptic meningitis, convulsions, paresthesia, memory disturbance, nightmares, tremor, tic, abnormal coordination, disorientation, psychotic reaction.
Respiratory: epistaxis, asthma, laryngeal edema, dyspnea, hyperventilation, edema of pharynx.
Skin and Appendages: rash•, pruritus•, alopecia, urticaria, eczema, dermatitis, bullous eruption, erythema multiforme major, angioedema, Stevens-Johnson syndrome, excess perspiration, exfoliative dermatitis.
Special Senses: tinnitus•, blurred vision, taste disorder, reversible and irreversible hearing loss, scotoma, vitreous floaters, night blindness, amblyopia.
Urogenital: nephrotic syndrome, proteinuria, oliguria, interstitial nephritis, papillary necrosis, acute renal failure, urinary frequency, nocturia, hematuria, impotence, vaginal bleeding.
Postmarketing Experience
The following adverse reactions have been identified during post-approval use of diclofenac sodium gel and other topical diclofenac products. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Adverse reactions from diclofenac sodium gel: burning sensation, hypersensitivity.
Adverse reactions from other topical diclofenac products: hypoesthesia, gait disturbance, musculoskeletal stiffness.
Skin and Appendages: Exfoliative dermatitis, Stevens-Johnson Syndrome (SJS), toxic epidermal necrolysis (TEN), and fixed drug eruption (FDE).
DRUG INTERACTIONS
See Table 2 for clinically significant drug interactions with diclofenac.
Drugs That Interfere with Hemostasis | |
Clinical Impact: |
|
Intervention: |
|
Aspirin | |
Clinical Impact: |
|
Intervention: |
|
ACE Inhibitors, Angiotensin Receptor Blockers, and Beta-Blockers | |
Clinical Impact: |
|
Intervention: |
|
Diuretics | |
Clinical Impact: |
|
Intervention: |
|
Digoxin | |
Clinical Impact: |
|
Intervention: |
|
Lithium | |
Clinical Impact: |
|
Intervention: |
|
Methotrexate | |
Clinical Impact: |
|
Intervention: |
|
Cyclosporine | |
Clinical Impact: |
|
Intervention: |
|
NSAIDs and Salicylates | |
Clinical Impact: |
|
Intervention: |
|
Pemetrexed | |
Clinical Impact: |
|
Intervention: |
|
DESCRIPTION
Diclofenac sodium topical gel, 3%, intended for dermatologic use, contains the active ingredient, diclofenac sodium USP, in a clear, transparent, colorless to slightly yellow gel base. Diclofenac sodium, USP is a white to slightly yellow crystalline powder. It is freely soluble in methanol, soluble in ethanol, sparingly soluble in water, slightly soluble in acetone, and partially insoluble in ether. The chemical name for diclofenac sodium is:
Sodium [ o -(2,6-dichloranilino) phenyl] acetate Diclofenac sodium, USP has a molecular weight of 318.13.
The CAS number is CAS-15307-79-6. The structural formula is represented below:
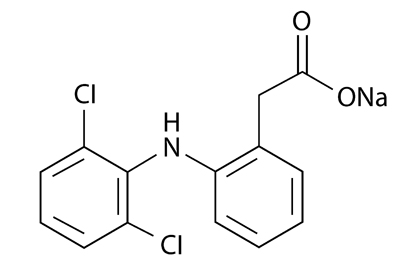
Diclofenac sodium topical gel also contains benzyl alcohol, hyaluronate sodium, polyethylene glycol monomethyl ether, and purified water. 1 g of Diclofenac sodium topical gel contains 30 mg of the active substance, diclofenac sodium, USP.
CLINICAL PHARMACOLOGY
Mechanism of Action
The mechanism of action of diclofenac sodium in the treatment of actinic keratoses (AK) is unknown.
Pharmacodynamics
The pharmacodynamics of diclofenac sodium in the treatment of actinic keratosis has not been assessed.
Pharmacokinetics
Absorption Diclofenac levels were measured at the end of treatment from 60 patients with AK lesions treated with diclofenac sodium topical gel in three adequate and well-controlled clinical trials. Each patient was administered 0.5 g of diclofenac sodium topical gel twice a day for up to 105 days. There were up to three 5 cm x 5 cm treatment sites per patient on the face, forehead, hands, forearm, and scalp. Serum concentrations of diclofenac were, on average, at or below 20 ng/mL.
Distribution Diclofenac binds tightly to serum albumin.
Metabolism Biotransformation of diclofenac following oral administration involves conjugation at the carboxyl group of the side chain or single or multiple hydroxylations resulting in several phenolic metabolites, most of which are converted to glucuronide conjugates. Two of these phenolic metabolites are biologically active, however to a much smaller extent than diclofenac. Metabolism of diclofenac following topical administration is thought to be similar to that after oral administration. The small amounts of diclofenac and its metabolites appearing in the plasma following topical administration makes the quantification of specific metabolites imprecise.
Elimination Diclofenac and its metabolites are excreted mainly in the urine after oral dosing.
NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, Impairment of Fertility
There did not appear to be any increase in drug-related neoplasms following daily topical applications of diclofenac sodium gel for 2 years at concentrations up to 0.035% diclofenac sodium and 2.5% hyaluronate sodium in albino mice.
When administered orally for 2 years, diclofenac showed no evidence of carcinogenic potential in rats given diclofenac sodium at up to 2 mg/kg/day (3 times the MRHD based on BSA comparison), or in mice given diclofenac sodium at up to 0.3 mg/kg/day in males and 1 mg/kg/day in females (25% and 83%, respectively, of the MRHD based on BSA comparison).
Diclofenac was not genotoxic in in vitro point mutation assays in mammalian mouse lymphoma cells and Ames microbial test systems, or when tested in mammalian in vivo assays including dominant lethal and male germinal epithelial chromosomal studies in mice, and nucleus anomaly and chromosomal aberration studies in Chinese hamsters. It was also negative in the transformation assay utilizing BALB/3T3 mouse embryo cells.
Fertility studies have not been conducted with diclofenac sodium showed no evidence of impairment of fertility after oral treatment with 4 mg/kg/day (7 times the MRHD based on BSA comparison) in male or female rats.
CLINICAL STUDIES
Clinical trials were conducted involving a total of 427 patients (213 treated with diclofenac sodium topical gel and 214 with a gel vehicle). Each patient had no fewer than five AK lesions in a major body area, which was defined as one of five 5 cm x 5 cm regions: scalp, forehead, face, forearm and hand. Up to three major body areas were studied in any patient. All patients were 18 years of age or older (male and female) with no clinically significant medical problems outside of the AK lesions and had undergone a 60-day washout period from disallowed medications (masoprocol, 5-fluorouracil, cyclosporine, retinoids, trichloroacetic acid/lactic acid/peel, 50% glycolic acid peel) and hyaluronan-containing cosmetics. Patients were excluded from participation for reasons of known or suspected hypersensitivity to any diclofenac sodium topical gel ingredient, pregnancy, allergies to aspirin or other nonsteroidal anti-inflammatory drugs (NSAIDs), or other dermatological conditions which might affect the absorption of the study medication. Application of dermatologic products such as sunscreens, cosmetics, and other drug products was not permitted. Patients were instructed to apply a small amount of diclofenac sodium topical gel (approximately 0.5 g) onto the affected skin, using their fingers, and gently smoothing the gel over the lesion. In addition, all patients were instructed to avoid sun exposure. Complete clearing of the AK lesions 30 days after completion of treatment was the primary efficacy variable. No long-term patient follow-ups, after the 30-day assessments, were performed for the detection of recurrence.
Diclofenac Sodium Topical Gel | Vehicle | p-value | |
Study 1 90 days treatment | 27/58 (47%) | 11/59 (19%) | <0.001 |
Study 2 90 days treatment | 18/53 (34%) | 10/55 (18%) | 0.061 |
Study 3 60 days treatment | 15/48 (31%) | 5/49 (10%) | 0.021 |
30 days treatment | 7/49 (14%) | 2/49 (4%) | 0.221 |
| Scalp | Forehead | Face | Arm/Forearm | Back of Hand | |
Study 1 | |||||
| 90 days treatment | |||||
| Diclofenac Sodium Topical Gel | 1/4 (25%) | 17/30 (57%) | 9/17 (53%) | 4/12 (33%) | 6/16 (38%) |
| Vehicle | 3/9 (33%) | 8/24 (33%) | 5/17 (29%) | 4/12 (33%) | 0/14 (0) |
| p-value | 0.7646 | 0.0908 | 0.1682 | 1.000 | 0.0650 |
Study 2 | |||||
90 days treatment | |||||
Diclofenac Sodium Topical Gel | 2/6 (33%) | 9/19 (47%) | 4/5 (80%) | 5/8 (63%) | 1/17 (6%) |
| Vehicle | 0/4 (0) | 6/22 (27%) | 2/8 (25%) | 0/5 (0) | 3/16 (19%) |
| p-value | 0.4235 | 0.1870 | 0.0727 | 0.0888 | 0.2818 |
Study 3 | |||||
| 60 days treatment | |||||
Diclofenac Sodium Topical Gel | 3/7 (43%) | 13/31 (42%) | 10/19 (53%) | 0/1 (0) | 2/8 (25%) |
Vehicle | 0/6 (0) | 5/36 (14%) | 2/13 (15%) | 0/2 (0) | 1/9 (11%) |
| p-value | 0.2271 | 0.0153 | 0.0433 | - | 0.4637 |
| 30 days treatment | |||||
Diclofenac Sodium Topical Gel | 2/5 (40%) | 4/29 (14%) | 3/14 (21%) | 0/0 (0) | 0/9 (0) |
| Vehicle | 0/5 (0) | 2/29 (7%) | 2/18 (11%) | 0/1 (0) | 1/9 (11%) |
| p-value | 0.2299 | 0.3748 | 0.4322 | - | 0.6521 |
| All data combined | |||||
| Diclofenac Sodium Topical Gel | 8/22 (36%) | 43/109 (39%) | 26/55 (47%) | 9/21 (43%) | 9/50 (18%) |
| Vehicle | 3/24 (13%) | 21/111 (19%) | 11/56 (20%) | 4/20 (20%) | 5/48 (10%) |
| p-value | 0.0903 | 0.0013 | 0.0016 | 0.2043 | 0.3662 |
HOW SUPPLIED/STORAGE AND HANDLING
Diclofenac sodium topical gel 3% contains the active ingredient, diclofenac sodium USP, in a clear, transparent, colorless to slightly yellow gel base. Each gram of gel contains 30 mg of diclofenac sodium, USP and is available in tubes of 100 g (NDC 0472-1783-10).
Storage: Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° to 30°C (59° to 86°F) [see USP Controlled Room Temperature]. Protect from heat. Avoid freezing.
Mechanism of Action
The mechanism of action of diclofenac sodium in the treatment of actinic keratoses (AK) is unknown.