Calcitriol - Calcitriol solution prescribing information
INDICATIONS AND USAGE
Predialysis Patients
Calcitriol Oral Solution is indicated in the management of secondary hyperparathyroidism and resultant metabolic bone disease in patients with moderate to severe chronic renal failure (Ccr 15 to 55 mL/min) not yet on dialysis. In children, the creatinine clearance value must be corrected for a surface area of 1.73 square meters. A serum iPTH level of ≥ 100 pg/mL is strongly suggestive of secondary hyperparathyroidism.
Dialysis Patients
Calcitriol Oral Solution is indicated in the management of hypocalcemia and the resultant metabolic bone disease in patients undergoing chronic renal dialysis. In these patients, Calcitriol Oral Solution administration enhances calcium absorption, reduces serum alkaline phosphatase levels, and may reduce elevated parathyroid hormone levels and the histological manifestations of osteitis fibrosa cystica and defective mineralization.
Hypoparathyroidism Patients
Calcitriol Oral Solution is also indicated in the management of hypocalcemia and its clinical manifestations in patients with postsurgical hypoparathyroidism, idiopathic hypoparathyroidism, and pseudohypoparathyroidism.
DOSAGE AND ADMINISTRATION
The optimal daily dose of Calcitriol Oral Solution must be carefully determined for each patient. Calcitriol Oral Solution can be administered as an oral solution (1 mcg/mL). Calcitriol Oral Solution therapy should always be started at the lowest possible dose and should not be increased without careful monitoring of serum calcium.
The effectiveness of Calcitriol Oral Solution therapy is predicated on the assumption that each patient is receiving an adequate but not excessive daily intake of calcium. Patients are advised to have a dietary intake of calcium at a minimum of 600 mg daily. The U.S. RDA for calcium in adults is 800 mg to 1200 mg. To ensure that each patient receives an adequate daily intake of calcium, the physician should either prescribe a calcium supplement or instruct the patient in proper dietary measures.
Because of improved calcium absorption from the gastrointestinal tract, some patients on Calcitriol Oral Solution may be maintained on a lower calcium intake. Patients who tend to develop hypercalcemia may require only low doses of calcium or no supplementation at all.
During the titration period of treatment with Calcitriol Oral Solution, serum calcium levels should be checked at least twice weekly. When the optimal dosage of Calcitriol Oral Solution has been determined, serum calcium levels should be checked every month (or as given below for individual indications). Samples for serum calcium estimation should be taken without a tourniquet.
Dialysis Patients
The recommended initial dose of Calcitriol Oral Solution is 0.25 mcg/day. If a satisfactory response in the biochemical parameters and clinical manifestations of the disease state is not observed, dosage may be increased by 0.25 mcg/day at 4- to 8-week intervals. During this titration period, serum calcium levels should be obtained at least twice weekly, and if hypercalcemia is noted, the drug should be immediately discontinued until normocalcemia ensues (see PRECAUTIONS: GENERAL ). Phosphorus, magnesium, and alkaline phosphatase should be determined periodically.
Patients with normal or only slightly reduced serum calcium levels may respond to Calcitriol Oral Solution doses of 0.25 mcg every other day. Most patients undergoing hemodialysis respond to doses between 0.5 and 1 mcg/day.
Calcitriol Oral Solution may normalize plasma-ionized calcium in some uremic patients, yet fail to suppress parathyroid hyperfunction. In these individuals with autonomous parathyroid hyper-function, Calcitriol Oral Solution may be useful to maintain normocalcemia, but has not been shown to be adequate treatment for hyperparathyroidism.
Hypoparathyroidism
The recommended initial dosage of Calcitriol Oral Solution is 0.25 mcg/day given in the morning. If a satisfactory response in the biochemical parameters and clinical manifestations of the disease is not observed, the dose may be increased at 2- to 4-week intervals. During the dosage titration period, serum calcium levels should be obtained at least twice weekly and, if hypercalcemia is noted, Calcitriol Oral Solution should be immediately discontinued until normocalcemia ensues (see PRECAUTIONS: GENERAL ). Careful consideration should also be given to lowering the dietary calcium intake. Serum calcium, phosphorus, and 24-hour urinary calcium should be determined periodically.
Most adult patients and pediatric patients age 6 years and older have responded to dosages in the range of 0.5 mcg to 2 mcg daily. Pediatric patients in the 1- to 5-year age group with hypoparathyroidism have usually been given 0.25 mcg to 0.75 mcg daily. The number of treated patients with pseudohypoparathyroidism less than 6 years of age is too small to make dosage recommendations.
Malabsorption is occasionally noted in patients with hypoparathyroidism; hence, larger doses of Calcitriol Oral Solution may be needed.
Predialysis Patients
The recommended initial dosage of Calcitriol Oral Solution is 0.25 mcg/day in adults and pediatric patients 3 years of age and older. This dosage may be increased if necessary to 0.5 mcg/day.
For pediatric patients less than 3 years of age, the recommended initial dosage of Calcitriol Oral Solution is 10 to 15 ng/kg/day.
CONTRAINDICATIONS
Calcitriol Oral Solution should not be given to patients with hypercalcemia or evidence of vitamin D toxicity. Use of Calcitriol Oral Solution in patients with known hypersensitivity to Calcitriol Oral Solution (or drugs of the same class) or any of the inactive ingredients is contraindicated.
ADVERSE REACTIONS
Since Calcitriol Oral Solution is believed to be the active hormone which exerts vitamin D activity in the body, adverse effects are, in general, similar to those encountered with excessive vitamin D intake, ie, hypercalcemia syndrome or calcium intoxication (depending on the severity and duration of hypercalcemia) (see WARNINGS ). Because of the short biological half-life of calcitriol, pharmacokinetic investigations have shown normalization of elevated serum calcium within a few days of treatment withdrawal, ie, much faster than in treatment with vitamin D 3 preparations.
The early and late signs and symptoms of vitamin D intoxication associated with hypercalcemia include:
Early : weakness, headache, somnolence, nausea, vomiting, dry mouth, constipation, muscle pain, bone pain, metallic taste, and anorexia, abdominal pain or stomach ache.
Late : polyuria, polydipsia, anorexia, weight loss, nocturia, conjunctivitis (calcific), pancreatitis, photophobia, rhinorrhea, pruritus, hyperthermia, decreased libido, elevated BUN, albuminuria, hypercholesterolemia, elevated SGOT (AST) and SGPT (ALT), ectopic calcification, nephrocalcinosis, hypertension, cardiac arrhythmias, dystrophy, sensory disturbances, dehydration, apathy, arrested growth, urinary tract infections, and, rarely, overt psychosis.
In clinical studies on hypoparathyroidism and pseudohypoparathyroidism, hypercalcemia was noted on at least one occasion in about 1 in 3 patients and hypercalciuria in about 1 in 7 patients. Elevated serum creatinine levels were observed in about 1 in 6 patients (approximately one half of whom had normal levels at baseline).
In concurrent hypercalcemia and hyperphosphatemia, soft-tissue calcification may occur; this can be seen radiographically (see WARNINGS ).
In patients with normal renal function, chronic hypercalcemia may be associated with an increase in serum creatinine (see PRECAUTIONS: GENERAL ).
Hypersensitivity reactions (pruritus, rash, urticaria, and very rarely severe erythematous skin disorders) may occur in susceptible individuals. One case of erythema multiforme and one case of allergic reaction (swelling of lips and hives all over the body) were confirmed by rechallenge.
To report SUSPECTED ADVERSE REACTIONS, contact Rising Pharma Holdings, Inc. at 1-844-874-7464 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
DESCRIPTION
Calcitriol Oral Solution is a synthetic vitamin D analog which is active in the regulation of the absorption of calcium from the gastrointestinal tract and its utilization in the body. Calcitriol oral solution contains 1 mcg/mL of calcitriol. Calcitriol Oral Solution contains butylated hydroxyanisole (BHA) and butylated hydroxytoluene (BHT) as antioxidants. Calcitriol oral solution contains caprylic triglycerides. The oral solution contains no additional adjuvants or coloring principles.
Calcitriol is a white, crystalline compound which occurs naturally in humans. It has a calculated molecular weight of 416.65 and is soluble in organic solvents but relatively insoluble in water. Chemically, calcitriol is 9,10-seco(5Z,7E)-5,7,10(19)-cholestatriene-1α, 3β, 25-triol and has the following structural formula:
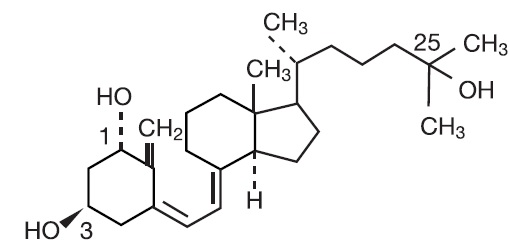
The other names frequently used for calcitriol are 1α,25-dihydroxycholecalciferol, 1,25-dihydroxyvitamin D 3 , 1,25-DHCC, 1,25(OH) 2 D 3 and 1,25-diOHC.
CLINICAL PHARMACOLOGY
Man's natural supply of vitamin D depends mainly on exposure to the ultraviolet rays of the sun for conversion of 7-dehydrocholesterol in the skin to vitamin D 3 (cholecalciferol). Vitamin D 3 must be metabolically activated in the liver and the kidney before it is fully active as a regulator of calcium and phosphorus metabolism at target tissues. The initial transformation of vitamin D 3 is catalyzed by a vitamin D 3 -25-hydroxylase enzyme (25-OHase) present in the liver, and the product of this reaction is 25-hydroxyvitamin D 3 [25-(OH)D 3 ]. Hydroxylation of 25-(OH)D 3 occurs in the mitochondria of kidney tissue, activated by the renal 25-hydroxyvitamin D 3 -1 alpha-hydroxylase (alpha-OHase), to produce 1,25-(OH) 2 D 3 (calcitriol), the active form of vitamin D 3 . Endogenous synthesis and catabolism of calcitriol, as well as physiological control mechanisms affecting these processes, play a critical role regulating the serum level of calcitriol. Physiological daily production is normally 0.5 to 1.0 mcg and is somewhat higher during periods of increased bone synthesis (eg, growth or pregnancy).
Pharmacodynamics
The two known sites of action of calcitriol are intestine and bone. A calcitriol receptor-binding protein appears to exist in the mucosa of human intestine. Additional evidence suggests that calcitriol may also act on the kidney and the parathyroid glands. Calcitriol is the most active known form of vitamin D 3 in stimulating intestinal calcium transport. In acutely uremic rats calcitriol has been shown to stimulate intestinal calcium absorption. The kidneys of uremic patients cannot adequately synthesize calcitriol, the active hormone formed from precursor vitamin D. Resultant hypocalcemia and secondary hyperparathyroidism are a major cause of the metabolic bone disease of renal failure. However, other bone-toxic substances which accumulate in uremia (eg, aluminum) may also contribute.
The beneficial effect of Calcitriol Oral Solution in renal osteodystrophy appears to result from correction of hypocalcemia and secondary hyperparathyroidism. It is uncertain whether Calcitriol Oral Solution produces other independent beneficial effects. Calcitriol Oral Solution treatment is not associated with an accelerated rate of renal function deterioration. No radiographic evidence of extraskeletal calcification has been found in predialysis patients following treatment. The duration of pharmacologic activity of a single dose of calcitriol is about 3 to 5 days.
Pharmacokinetics
Absorption
Calcitriol is rapidly absorbed from the intestine. Peak serum concentrations (above basal values) were reached within 3 to 6 hours following oral administration of single doses of 0.25 to 1.0 mcg of Calcitriol Oral Solution. Following a single oral dose of 0.5 mcg, mean serum concentrations of calcitriol rose from a baseline value of 40.0±4.4 (SD) pg/mL to 60.0±4.4 pg/mL at 2 hours, and declined to 53.0±6.9 at 4 hours, 50±7.0 at 8 hours, 44±4.6 at 12 hours, and 41.5±5.1 at 24 hours.
Following multiple-dose administration, serum calcitriol levels reached steady-state within 7 days.
Distribution
Calcitriol is approximately 99.9% bound in blood. Calcitriol and other vitamin D metabolites are transported in blood, by an alpha-globulin vitamin D binding protein. There is evidence that maternal calcitriol may enter the fetal circulation. Calcitriol is transferred into human breast milk at low levels (ie, 2.2±0.1 pg/mL).
Metabolism
In vivo and in vitro studies indicate the presence of two pathways of metabolism for calcitriol. The first pathway involves the 24-hydroxylase as the first step in catabolism of calcitriol. There is definite evidence of 24-hydroxylase activity in the kidney; this enzyme is also present in many target tissues which possess the vitamin D receptor such as the intestine. The end product of this pathway is a side chain shortened metabolite, calcitroic acid. The second pathway involves the conversion of calcitriol via the stepwise hydroxylation of carbon-26 and carbon-23, and cyclization to yield ultimately 1α, 25R(OH) 2 -26, 23S-lactone D 3 . The lactone appears to be the major metabolite circulating in humans, with mean serum concentrations of 131±17 pg/mL. In addition, several other metabolites of calcitriol have been identified: 1α, 25(OH) 2 -24-oxo-D 3 ; 1α, 23,25(OH) 3 -24-oxo-D 3 ; 1α, 24R,25(OH) 3 D 3 ; 1α, 25S,26(OH) 3 D 3 ; 1α, 25(OH) 2 -23-oxo-D 3 ; 1α, 25R,26(OH) 3 -23-oxo-D 3 ; 1α, (OH)24,25,26,27-tetranor-COOH-D 3 .
Excretion
Enterohepatic recycling and biliary excretion of calcitriol occur. The metabolites of calcitriol are excreted primarily in feces. Following intravenous administration of radiolabeled calcitriol in normal subjects, approximately 27% and 7% of the radioactivity appeared in the feces and urine, respectively, within 24 hours. When a 1-mcg oral dose of radiolabeled calcitriol was administered to normal subjects, approximately 10% of the total radioactivity appeared in urine within 24 hours. Cumulative excretion of radioactivity on the sixth day following intravenous administration of radiolabeled calcitriol averaged 16% in urine and 49% in feces. The elimination half-life of calcitriol in serum after single oral doses is about 5 to 8 hours in normal subjects.
Special Populations
Pediatric Pharmacokinetics
The steady-state pharmacokinetics of Calcitriol Oral Solution were determined in a small group of pediatric patients (age range: 1.8 to 16 years) undergoing peritoneal dialysis. Calcitriol Oral Solution was administered for 2 months at an average dose of 10.2 ng/kg (SD 5.5 ng/kg). In this pediatric population, mean C max was 116 pmol/L, mean serum half-life was 27.4 hours, and mean clearance was 15.3 mL/hr/kg.1
Geriatric
No studies have examined the pharmacokinetics of calcitriol in geriatric patients.
Gender
Controlled studies examining the influence of gender on calcitriol have not been conducted.
Hepatic Insufficiency
Controlled studies examining the influence of hepatic disease on calcitriol have not been conducted.
Renal Insufficiency
Lower predose and peak calcitriol levels in serum were observed in patients with nephrotic syndrome and in patients undergoing hemodialysis compared with healthy subjects. The elimination half-life of calcitriol increased by at least twofold in chronic renal failure and hemodialysis patients compared with healthy subjects. Peak serum levels in patients with nephrotic syndrome were reached in 4 hours. For patients requiring hemodialysis peak serum levels were reached in 8 to 12 hours; half-lives were estimated to be 16.2 and 21.9 hours, respectively.
HOW SUPPLIED
Oral Solution: a clear, colorless oral solution containing 1 mcg/mL of calcitriol; each amber glass bottle of 15 mL of oral solution supplied with 20 single-use, graduated oral dispensers NDC: 64980-447-15
Calcitriol Oral Solution should be protected from light. Store at 59° to 86°F (15° to 30°C).
REFERENCE
1. Jones CL, et al. Comparisons between oral and intraperitoneal 1,25-dihydroxyvitamin D 3 therapy in children treated with peritoneal dialysis. Clin Nephrol. 1994; 42:44-49.
Manufactured for: Rising Pharma Holdings, Inc. East Brunswick, NJ 08816
Revised: 02/2025
PIR44715-00