Get your patient on Vincristine Sulfate - Vincristine Sulfate injection, Solution (Vincristine Sulfate)
Vincristine Sulfate - Vincristine Sulfate injection, Solution prescribing information
WARNINGS
Caution–This preparation should be administered by individuals experienced in the administration of Vincristine Sulfate Injection. It is extremely important that the intravenous needle or catheter be properly positioned before any vincristine is injected. Leakage into surrounding tissue during intravenous administration of Vincristine Sulfate Injection may cause considerable irritation. If extravasation occurs, the injection should be discontinued immediately, and any remaining portion of the dose should then be introduced into another vein. Local injection of hyaluronidase and the application of moderate heat to the area of leakage help disperse the drug and are thought to minimize discomfort and the possibility of cellulitis.
FOR INTRAVENOUS USE ONLY – FATAL IF GIVEN BY OTHER ROUTES.
See OVERDOSAGE section for the treatment of patients given intrathecal Vincristine Sulfate Injection.
INDICATIONS AND USAGE
Vincristine Sulfate Injection is indicated in acute leukemia.
Vincristine Sulfate Injection has also been shown to be useful in combination with other oncolytic agents in Hodgkin's disease, non–Hodgkin's malignant lymphomas, rhabdomyosarcoma, neuroblastoma, and Wilms' tumor.
DOSAGE AND ADMINISTRATION
This preparation is for intravenous use only (see WARNINGS ).
Neurotoxicity appears to be dose related. Extreme care must be used in calculating and administering the dose of Vincristine Sulfate Injection since overdosage may have a very serious or fatal outcome.
The usual dose of Vincristine Sulfate Injection for pediatric patients is 1.5–2 mg/m 2 . For pediatric patients weighing 10 kg or less, the starting dose should be 0.05 mg/kg, administered once a week. The usual dose of Vincristine Sulfate Injection for adults is 1.4 mg/m 2 . A 50% reduction in the dose of Vincristine Sulfate Injection is recommended for patients having a direct serum bilirubin value above 3 mg/100 mL.
The drug is administered intravenously at weekly intervals.
TO REDUCE THE POTENTIAL FOR FATAL MEDICATION ERRORS DUE TO INCORRECT ROUTE OF ADMINISTRATION, VINCRISTINE SULFATE INJECTION SHOULD BE DILUTED IN A FLEXIBLE PLASTIC CONTAINER AND PROMINENTLY LABELED AS INDICATED FOR INTRAVENOUS USE ONLY – FATAL IF GIVEN BY OTHER ROUTES (See WARNINGS ).
The concentration of Vincristine Sulfate Injection is 1 mg/mL. Do not add extra fluid to the vial prior to removal of the dose. Withdraw the solution of Vincristine Sulfate Injection into an accurate dry syringe, measuring the dose carefully. Do not add extra fluid to the vial in an attempt to empty it completely.
Preparation for flexible plastic container
Vincristine Sulfate Injection when diluted with 0.9% Sodium Chloride Injection in concentrations from 0.0015 mg/mL to 0.08 mg/mL is stable for up to 24 hours when protected from light or 8 hours under normal light at 25°C.
Caution: It is extremely important that the intravenous needle or catheter be properly positioned before any vincristine is injected. Leakage into surrounding tissue during intravenous administration of Vincristine Sulfate Injection may cause considerable irritation. If extravasation occurs, the injection should be discontinued immediately and any remaining portion of the dose should then be introduced into another vein. Local injection of hyaluronidase and the application of moderate heat to the area of leakage will help disperse the drug and may minimize discomfort and the possibility of cellulitis.
Vincristine Sulfate Injection must be administered via an intact, free–flowing intravenous needle or catheter. Care should be taken that there is no leakage or swelling occurring during administration (see boxed WARNINGS ).
The diluted Vincristine Sulfate Injection may be infused via a flexible plastic container directly into an intravenous catheter/needle or into a running intravenous infusion (see Drug Interactions below).
Patients Receiving Radiation Therapy
Vincristine Sulfate Injection should not be given to patients while they are receiving radiation therapy through ports that include the liver. When Vincristine Sulfate Injection is used in combination with L–asparaginase, Vincristine Sulfate Injection should be given 12 to 24 hours before administration of the enzyme in order to minimize toxicity; administering L–asparaginase before Vincristine Sulfate Injection may reduce hepatic clearance of vincristine.
Drug Interactions
Vincristine Sulfate Injection should not be diluted in solutions that raise or lower the pH outside the range of 3.5 to 5.5. It should not be mixed with anything other than 0.9% Sodium Chloride Injection USP.
Whenever solution and container permit, parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration.
Handling and Disposal
Procedures for proper handling and disposal of anticancer drugs should be considered. Several guidelines on this subject have been published. 1 There is no general agreement that all of the procedures recommended in the guidelines are necessary or appropriate.
CONTRAINDICATIONS
Patients with the demyelinating form of Charcot–Marie–Tooth syndrome should not be given Vincristine Sulfate Injection. Careful attention should be given to those conditions listed under WARNINGS and PRECAUTIONS .
ADVERSE REACTIONS
Prior to the use of this drug, patients and/or their parents/guardian should be advised of the possibility of untoward symptoms.
In general, adverse reactions are reversible and are related to dosage. The most common adverse reaction is hair loss; the most troublesome adverse reactions are neuromuscular in origin.
When single, weekly doses of the drug are employed, the adverse reactions of leukopenia, neuritic pain, and constipation occur but are usually of short duration (ie., less than 7 days). When the dosage is reduced, these reactions may lessen or disappear. The severity of such reactions seems to increase when the calculated amount of drug is given in divided doses. Other adverse reactions, such as hair loss, sensory loss, paresthesia, difficulty in walking, slapping gait, loss of deep–tendon reflexes, and muscle wasting, may persist for at least as long as therapy is continued. Generalized sensorimotor dysfunction may become progressively more severe with continued treatment. Although most such symptoms usually disappear by about the sixth week after discontinuance of treatment, some neuromuscular difficulties may persist for prolonged periods in some patients. Regrowth of hair may occur while maintenance therapy continues.
The following adverse reactions have been reported:
Hepatic veno-occlusive disease has been reported in patients receiving vincristine, particularly in pediatric patients, as part of standard combination chemotherapy regimens. Some of the patients had fatal outcomes; some who survived had undergone liver transplantation.
Hypersensitivity
Rare cases of allergic–type reactions, such as anaphylaxis, rash and edema, that are temporally related to vincristine therapy have been reported in patients receiving vincristine as a part of multidrug chemotherapy regimens.
Gastrointestinal
Constipation, abdominal cramps, weight loss, nausea, vomiting, oral ulceration, diarrhea, paralytic ileus, intestinal necrosis and/or perforation, and anorexia have occurred. Constipation may take the form of upper–colon impaction, and, on physical examination, the rectum may be empty. Colicky abdominal pain coupled with an empty rectum may mislead the physician. A flat film of the abdomen is useful in demonstrating this condition. All cases have responded to high enemas and laxatives. A routine prophylactic regimen against constipation is recommended for all patients receiving Vincristine Sulfate Injection.
Paralytic ileus (which mimics the "surgical abdomen") may occur, particularly in young pediatric patients. The ileus will reverse itself with temporary discontinuance of Vincristine Sulfate Injection and with symptomatic care.
Genitourinary
Polyuria, dysuria, and urinary retention due to bladder atony have occurred. Other drugs known to cause urinary retention (particularly in the elderly) should, if possible, be discontinued for the first few days following administration of Vincristine Sulfate Injection.
Cardiovascular
Hypertension and hypotension have occurred. Chemotherapy combinations that have included vincristine sulfate, when given to patients previously treated with mediastinal radiation, have been associated with coronary artery disease and myocardial infarction. Causality has not been established.
Neurologic
Frequently, there is a sequence to the development of neuromuscular side effects. Initially, only sensory impairment and paresthesia may be encountered. With continued treatment, neuritic pain and, later, motor difficulties may occur. There have been no reports of any agent that can reverse the neuromuscular manifestations that may accompany therapy with vincristine sulfate.
Loss of deep–tendon reflexes, foot drop, ataxia, and paralysis have been reported with continued administration. Cranial nerve manifestations, such as isolated paresis and/or paralysis of muscles controlled by cranial motor nerves including potentially life–threatening bilateral vocal cord paralysis, may occur in the absence of motor impairment elsewhere; extraocular and laryngeal muscles are those most commonly involved. Jaw pain, pharyngeal pain, parotid gland pain, bone pain, back pain, limb pain, and myalgias have been reported; pain in these areas may be severe. Convulsions, frequently with hypertension, have been reported in a few patients receiving vincristine sulfate. Several instances of convulsions followed by coma have been reported in pediatric patients. Transient cortical blindness and optic atrophy with blindness have been reported. Treatment with vinca alkaloids has resulted in both vestibular and auditory damage to the eighth cranial nerve. Manifestations include partial or total deafness which may be temporary or permanent, and difficulties with balance including dizziness, nystagmus, and vertigo. Particular caution is warranted when vincristine is used in combination with other agents known to be ototoxic such as the platinum–containing oncolytics.
Pulmonary
See PRECAUTIONS section. Acute respiratory distress syndrome has been reported.
Endocrine
Rare occurrences of a syndrome attributable to inappropriate antidiuretic hormone secretion have been observed in patients treated with vincristine sulfate. This syndrome is characterized by high urinary sodium excretion in the presence of hyponatremia; renal or adrenal disease, hypotension, dehydration, azotemia, and clinical edema are absent. With fluid deprivation, improvement occurs in the hyponatremia and in the renal loss of sodium.
Hematologic
Vincristine Sulfate Injection does not appear to have any constant or significant effect on platelets or red blood cells. Serious bone–marrow depression is usually not a major dose–limiting event. However, anemia, leukopenia, and thrombocytopenia have been reported. Thrombocytopenia, if present when therapy with Vincristine Sulfate Injection is begun, may actually improve before the appearance of bone marrow remission. Granulocytopenia has been reported.
Skin
Alopecia and rash have been reported.
Other
Fever, headache, dehydration, and hyperuricemia have occurred.
Drug Interactions
The simultaneous oral or intravenous administration of phenytoin and antineoplastic chemotherapy combinations that included vincristine sulfate has been reported to reduce blood levels of the anticonvulsant and to increase seizure activity. Dosage adjustment should be based on serial blood level monitoring. The contribution of vincristine sulfate to this interaction is not certain. The interaction may result from reduced absorption of phenytoin and an increase in the rate of its metabolism and elimination.
Vincristine sulfate is a substrate for cytochrome P450 3A isozymes (CYP3A). Concurrent administration of vincristine sulfate with itraconazole or fluconazole (known inhibitors of the CYP3A metabolic pathway) has been reported to cause an earlier onset and/or an increased severity of neuromuscular side effects (see ADVERSE REACTIONS ). This interaction is presumed to be related to inhibition of the metabolism of vincristine. Therefore, the concomitant use of strong CYP3A inhibitors with vincristine sulfate should be avoided. Patients should be frequently monitored for adverse reactions with concomitant use of moderate CYP3A inhibitors (e.g., fluconazole) with vincristine sulfate.
Concurrent use of strong CYP3A inducers (e.g., St. John's Wort) with vincristine sulfate should be avoided.
Vincristine sulfate is also a substrate for P-glycoprotein (P-gp). Therefore, the concomitant use of P-gp inhibitors or inducers should be avoided.
DESCRIPTION
Vincristine Sulfate Injection, USP is the salt of an alkaloid obtained from a common flowering herb, the periwinkle plant ( Vinca rosea Linn). Originally known as leurocristine, it has also been referred to as LCR and VCR.
The molecular formula for Vincristine Sulfate, USP is C 46 H 56 N 4 O 10 ∙H 2 SO 4 . It has a molecular weight of 923.04.
The structural formula is as follows:
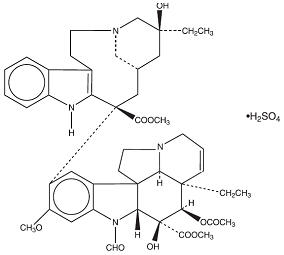
Vincristine Sulfate, USP is a white to off–white powder. It is soluble in methanol, freely soluble in water, but only slightly soluble in 95% ethanol. In 98% ethanol, Vincristine Sulfate, USP has an ultraviolet spectrum with maxima at 221 nm (ϵ+47,100).
Vincristine Sulfate Injection, USP is a sterile, preservative–free, single-dose only solution available for intravenous use in 1 mg/mL and 2 mg/2 mL (1 mg/mL) vials. Each mL contains 1 mg Vincristine Sulfate, USP, 100 mg mannitol and Water for Injection, USP. Q.S. Sulfuric acid or sodium hydroxide have been added for pH control. The pH of Vincristine Sulfate Injection, USP ranges from 4.0 to 5.0. At the time of manufacture, the air in the containers is replaced by nitrogen.
CLINICAL PHARMACOLOGY
The mechanisms of action of vincristine sulfate remain under investigation. The mechanism of action of vincristine sulfate has been related to the inhibition of microtubule formation in mitotic spindle, resulting in an arrest of dividing cells at the metaphase stage.
Central nervous system leukemia has been reported in patients undergoing otherwise successful therapy with vincristine sulfate. This suggests that vincristine does not penetrate well into the cerebrospinal fluid.
Pharmacokinetic studies in patients with cancer have shown a triphasic serum decay pattern following rapid intravenous injection. The initial, middle and terminal half–lives are 5 minutes, 2.3 hours, and 85 hours respectively; however, the range of the terminal half–life in humans is from 19 to 155 hours. The liver is the major excretory organ in humans and animals. The metabolism of vinca alkaloids has been shown to be mediated by hepatic cytochrome P450 isoenzymes in the CYP 3A subfamily. This metabolic pathway may be impaired in patients with hepatic dysfunction or who are taking concomitant potent inhibitors of these isoenzymes (see PRECAUTIONS ). About 80% of an injected dose of vincristine sulfate appears in the feces and 10% to 20% can be found in the urine. Within 15 to 30 minutes after injection, over 90% of the drug is distributed from the blood into tissue, where it remains tightly, but not irreversibly, bound.
Current principles of cancer chemotherapy involve the simultaneous use of several agents. Generally, each agent used has a unique toxicity and mechanism of action so that therapeutic enhancement occurs without additive toxicity. It is rarely possible to achieve equally good results with single–agent methods of treatment. Thus, vincristine sulfate is often chosen as part of polychemotherapy because of lack of significant bone–marrow suppression (at recommended doses) and of unique clinical toxicity (neuropathy). See DOSAGE AND ADMINISTRATION section for possible increased toxicity when used in combination therapy.
HOW SUPPLIED
Vincristine Sulfate Injection, USP, is available as follows:
Unit of Sale | Total Strength/Total Volume (Concentration) |
NDC 61703–309–26 Carton of 1 single-dose flip-top vial (blue cap) | 1 mg/mL |
NDC 61703–309–25 Carton of 1 single-dose flip-top vial (blue cap) | 2 mg/2 mL (1 mg/mL) |
This product should be refrigerated between 2°C–8°C (36°F–46°F). Discard unused solution. Protect from light. Store Upright.
Vincristine Sulfate - Vincristine Sulfate injection, Solution PubMed™ news
- Journal Article • 2026 MayPrimary Langerhans Cell Histiocytosis of the Maxilla: Case Report.
- Journal Article • 2026 MayConcurrent cytomegalovirus iridocyclitis and vitreoretinal lymphoma in the same eye during long-term infliximab therapy: a case report.
- Journal Article • 2026 MayCytomorphologic changes in blood erythrocytes, leukocytes, and platelets in dogs progressing through CHOP therapy to treat multicentric lymphoma.
- Journal Article • 2026 MayChanges in mast cell density, fibrosis, and immunohistochemical expression of tryptase, chymase, SCF, and PAR2 during regression of canine transmissible venereal tumors.
- Journal Article • 2026 MayThe long-term efficacy and safety of high-dose chemotherapy with autologous stem cell transplantation in the treatment of primary central nervous system lymphoma: A real-world report from the Polish Lymphoma Research Group.