Get your patient on Butorphanol Tartrate - Butorphanol Tartrate injection, Solution (Butorphanol Tartrate)
Butorphanol Tartrate - Butorphanol Tartrate injection, Solution prescribing information
WARNING: SERIOUS AND LIFE-THREATENING RISKS FROM USE OF BUTORPHANOL TARTRATE INJECTION
Addiction, Abuse, and Misuse
Because the use of Butorphanol Tartrate Injection exposes patients and other users to the risks of opioid addiction, abuse, and misuse, which can lead to overdose and death, assess each patient’s risk prior to prescribing and reassess all patients regularly for the development of these behaviors and conditions [see WARNINGS ] .
Life-Threatening Respiratory Depression
Serious, life-threatening, or fatal respiratory depression may occur with use of Butorphanol Tartrate Injection, especially during initiation or following a dosage increase. To reduce the risk of respiratory depression, proper dosing and titration of Butorphanol Tartrate Injection are essential [see WARNINGS ] .
Risks From Concomitant Use With Benzodiazepines Or Other CNS Depressants
Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Reserve concomitant prescribing of Butorphanol Tartrate Injection and benzodiazepines or other CNS depressants for use in patients for whom alternative treatment options are inadequate [see WARNINGS , PRECAUTIONS ; Drug Interactions ] .
Neonatal Opioid Withdrawal Syndrome (NOWS)
Advise pregnant women using opioids for an extended period of time of the risk of Neonatal Opioid Withdrawal Syndrome, which may be life-threatening if not recognized and treated. Ensure that management by neonatology experts will be available at delivery [see WARNINGS ] .
INDICATIONS AND USAGE
Butorphanol Tartrate Injection is indicated
- as a preoperative or pre-anesthetic medication
- as a supplement to balanced anesthesia
- for the relief of pain during labor, and
- for the management of pain severe enough to require an opioid analgesic and for which alternative treatments are inadequate.
Limitations of Use:
Because of the risks of addiction, abuse, misuse, overdose, and death, which can occur at any dosage or duration and persist over the course of therapy [see WARNINGS ], reserve opioid analgesics, including butorphanol tartrate, for use in patients for whom alternative treatment options are ineffective, not tolerated, or would be otherwise inadequate to provide sufficient management of pain.
DOSAGE AND ADMINISTRATION
Important Dosage and Administration Instructions
Butorphanol Tartrate Injection should be prescribed only by healthcare professionals who are knowledgeable about the use of opioids and how to mitigate the associated risks.
Use the lowest effective dosage for the shortest duration of time consistent with individual patient treatment goals [see WARNINGS ]. Because the risk of overdose increases as opioid doses increase, reserve titration to higher doses of Butorphanol Tartrate Injection for patients in whom lower doses are insufficiently effective and in whom the expected benefits of using a higher dose opioid clearly outweigh the substantial risks.
There is variability in the opioid analgesic dose and duration needed to adequately manage pain due both to the cause of pain and to individual patient factors. Initiate the dosing regimen for each patient individually, taking into account the patient’s underlying cause and severity of pain, prior analgesic treatment and response, and risk factors for addiction, abuse, and misuse [see WARNINGS ].
Respiratory depression can occur at any time during opioid therapy, especially when initiating and following dosage increases with Butorphanol Tartrate Injection. Consider this risk when selecting an initial dose and when making dose adjustments [see WARNINGS ].
Initial Dosage
Factors to be considered in determining the dose are age, body weight, physical status, underlying pathological condition, use of other drugs, type of anesthesia to be used, and surgical procedure involved. Use in the elderly, patients with hepatic or renal disease, or in labor requires extra caution [see PRECAUTIONS ; CLINICAL PHARMACOLOGY: Individualization of Dosage ]. The following doses are for patients who do not have impaired hepatic or renal function and who are not on CNS active agents.
Use for Pain
Intravenous
The usual recommended single-dose for IV administration is 1 mg repeated every three to four hours as necessary. The effective dosage range, depending on the severity of pain, is 0.5 to 2 mg repeated every three to four hours.
Intramuscular
The usual recommended single-dose for IM administration is 2 mg in patients who will be able to remain recumbent, in the event drowsiness or dizziness occurs. This may be repeated every three to four hours, as necessary. The effective dosage range depending on the severity of pain is 1 to 4 mg repeated every three to four hours. There are insufficient clinical data to recommend single-doses above 4 mg.
Use as Preoperative/Preanesthetic Medication
The preoperative medication dosage of Butorphanol Tartrate Injection should be individualized [see CLINICAL PHARMACOLOGY: Individualization of Dosage ]. The usual adult dose is 2 mg IM, administered 60 to 90 minutes before surgery. This is approximately equivalent in sedative effect to 10 mg morphine or 80 mg meperidine.
Use in Balanced Anesthesia
The usual dose of Butorphanol Tartrate Injection is 2 mg IV shortly before induction and/or 0.5 to 1 mg IV in increments during anesthesia. The increment may be higher, up to 0.06 mg/kg (4 mg/70 kg), depending on previous sedative, analgesic, and hypnotic drugs administered. The total dose of butorphanol injection will vary; however, patients seldom require less than 4 mg or more than 12.5 mg (approximately 0.06 to 0.18 mg/kg).
Labor
In patients at full term in early labor a 1 to 2 mg dose of butorphanol tartrate IV or IM may be administered and repeated after 4 hours. Alternative analgesia should be used for pain associated with delivery or if delivery is expected to occur within 4 hours.
If concomitant use of butorphanol with drugs that may potentiate its effects is deemed necessary [see PRECAUTIONS: Drug Interactions ] the lowest effective dose should be employed.
Dosage Modifications in Elderly Patients and Patients with Renal or Hepatic Impairment
The initial dose sequence in elderly patients and patients with hepatic or renal impairment should be limited to 1 mg followed, if needed, by 1 mg in 90 to 120 minutes. The repeat dose sequence should be determined by the patient's response rather than at fixed times but will generally be no less than at 6 hours intervals [see CLINICAL PHARMACOLOGY: Individualization of Dosage , PRECAUTIONS ].
Titration and Maintenance of Therapy
Individually titrate Butorphanol Tartrate Injection to a dose that provides adequate analgesia and minimizes adverse reactions. Continually reevaluate patients receiving Butorphanol Tartrate Injection to assess the maintenance of pain control, signs and symptoms of opioid withdrawal, and other adverse reactions as well as reassessing for the development of addiction, abuse, or misuse [see WARNINGS ]. Frequent communication is important among the prescriber, other members of the healthcare team, the patient, and the caregiver/family during periods of changing analgesic requirements, including initial titration.
If the level of pain increases after dosage stabilization, attempt to identify the source of increased pain before increasing the Butorphanol Tartrate Injection dosage. If after increasing the dosage, unacceptable opioid-related adverse reactions are observed (including an increase in pain after dosage increase), consider reducing the dosage [see WARNINGS ]. Adjust the dosage to obtain an appropriate balance between management of pain and opioid-related adverse reactions.
Discontinuation of Butorphanol Tartrate Injection
When a patient who has been taking Butorphanol Tartrate Injection regularly and may be physically dependent no longer requires therapy with Butorphanol Tartrate Injection, taper the dose gradually, by 25% to 50% every 2 to 4 days, while monitoring carefully for signs and symptoms of withdrawal. If the patient develops these signs or symptoms, raise the dose to the previous level and taper more slowly, either by increasing the interval between decreases, decreasing the amount of change in dose, or both. Do not rapidly reduce or abruptly discontinue Butorphanol Tartrate Injection in patients who may be physically-dependent on opioids [see WARNINGS , DRUG ABUSE AND DEPENDENCE ].
Safety and Handling
Butorphanol Tartrate Injection is supplied in sealed delivery systems that have a low risk of accidental exposure to healthcare workers. Ordinary care should be taken to avoid aerosol generation while preparing a syringe for use. Following skin contact, rinsing with cool water is recommended.
The disposal of Schedule IV controlled substances must be consistent with State and Federal Regulations.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
CONTRAINDICATIONS
Butorphanol Tartrate Injection is contraindicated in:
- Patients with significant respiratory depression [see WARNINGS ]
- Patients with acute of severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment [see WARNINGS ]
- Patients with known or suspected gastrointestinal obstruction, including paralytic ileus [see WARNINGS ]
- Patients with hypersensitivity to butorphanol tartrate or any of the formulation excipients (e.g., anaphylaxis) [see WARNINGS ]
ADVERSE REACTIONS
Clinical Trial Experience
A total of 1658 patients were studied in premarketing clinical trials of Butorphanol Tartrate Injection. In nearly all cases the type and incidence of side effects with butorphanol were those commonly observed with opioid analgesics.
The adverse experiences described below are based on data from short- and long-term clinical trials in patients receiving Butorphanol Tartrate Injection.
The most frequently reported adverse experiences across all clinical trials with Butorphanol Tartrate Injection and Nasal Spray were somnolence (43%), dizziness (19%), nausea and/or vomiting (13%). The following adverse experiences were reported at a frequency of 1% or greater in clinical trials and were considered to be probably related to the use of butorphanol:
Body as a Whole: Asthenia/Lethargy, Headache, Sensation of Heat
Cardiovascular: Vasodilation, Palpitations
Digestive: Anorexia, Constipation, Dry Mouth, Nausea and/or Vomiting, Stomach Pain
Nervous: Anxiety, Confusion, Dizziness, Euphoria, Floating Feeling, Insomnia, Nervousness, Paresthesia, Somnolence, Tremor
Respiratory: Cough, Dyspnea
Skin and Appendages: Sweating, Pruritus
Special Senses: Blurred Vision, Ear Pain, Tinnitus, Unpleasant Taste
The following adverse experiences were reported with a frequency of less than 1% in clinical trials and were considered to be probably related to the use of butorphanol:
Cardiovascular: Hypotension, Syncope
Nervous: Abnormal Dreams, Agitation, Dysphoria, Hallucinations, Hostility, Withdrawal Symptoms
Skin and Appendages: Rash/Hives
Urogenital: Impaired Urination
The following infrequent additional adverse experiences were reported in a frequency of less than 1% of the patients studied in short-term butorphanol tartrate nasal sprays trials and under circumstances where the association between these events and butorphanol administration is unknown. They are being listed as alerting information for the physician due to their clinical significance:
Body as a Whole: Edema
Cardiovascular: Chest Pain, Hypertension, Tachycardia
Nervous: Depression
Respiratory: Shallow Breathing
Postmarketing Experience
The following adverse reactions have been identified during post approval use of Butorphanol Tartrate Injection. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Serotonin syndrome: Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of opioids with serotonergic drugs.
- Adrenal insufficiency: Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use.
- Anaphylaxis: Anaphylaxis has been reported with ingredients contained in Butorphanol Tartrate Injection.
- Androgen deficiency: Cases of androgen deficiency have occurred with use of opioids for an extended period of time [see CLINICAL PHARMACOLOGY ].
- Hyperalgesia and Allodynia: Cases of hyperalgesia and allodynia have been reported with opioid therapy of any duration [see WARNINGS ].
- Hypoglycemia: Cases of hypoglycemia have been reported in patients taking opioids. Most reports were in patients with at least one predisposing risk factor (e.g., diabetes).
- Opioid-induced esophageal dysfunction (OIED): Cases of OIED have been reported in patients taking opioids and may occur more frequently in patients taking higher doses of opioids, and/or in patients taking opioids longer term [see WARNINGS ].
Adverse Reactions from Observational Studies
A prospective, observational cohort study estimated the risks of addiction, abuse, and misuse in patients initiating long-term use of Schedule II opioid analgesics between 2017 and 2021. Study participants included in one or more analyses had been enrolled in selected insurance plans or health systems for at least one year, were free of at least one outcome at baseline, completed a minimum number of follow-up assessments, and either: 1) filled multiple extended-release/long-acting opioid analgesic prescriptions during a 90-day period (n=978); or 2) filled any Schedule II opioid analgesic prescriptions covering at least 70 of 90 days (n=1,244). Those included also had no dispensing of the qualifying opioids in the previous 6 months.
Over 12 months:
- approximately 1% to 6% of participants across the two cohorts newly met criteria for addiction, as assessed with two validated interview-based measures of moderate-to-severe opioid use disorder based on Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) criteria, and
- approximately 9% and 22% of participants across the two cohorts newly met criteria for prescription opioid abuse and misuse [defined in DRUG ABUSE AND DEPENDENCE ], respectively, as measured with a validated self-reported instrument.
A retrospective, observational cohort study estimated the risk of opioid-involved overdose or opioid overdose-related death in patients with new long-term use of Schedule II opioid analgesics from 2006 through 2016 (n=220,249). Included patients had been enrolled in either one of two commercial insurance programs, one managed care program, or one Medicaid program for at least 9 months. New long-term use was defined as having Schedule II opioid analgesic prescriptions covering at least 70 days’ supply over the 3 months prior to study entry and none during the preceding 6 months. Patients were excluded if they had an opioid-involved overdose in the 9 months prior to study entry. Overdose was measured using a validated medical code-based algorithm with linkage to the National Death Index database. The 5-year cumulative incidence estimates for opioid-involved overdose or opioid overdose-related death ranged from approximately 1.5% to 4% across study sites, counting only the first event during follow-up. Approximately 17% of first opioid overdoses observed over the entire study period (5-11 years, depending on the study site) were fatal. Higher baseline opioid dose was the strongest and most consistent predictor of opioid-involved overdose or opioid overdose-related death. Study exclusion criteria may have selected patients at lower risk of overdose, and substantial loss to follow-up (approximately 80%) also may have biased estimates.
The risk estimates from the studies described above may not be generalizable to all patients receiving opioid analgesics, such as those with exposures shorter or longer than the duration evaluated in the studies.
Drug Interactions
Benzodiazepines and Other Central Nervous System (CNS) Depressants
Due to additive pharmacologic effect, the concomitant use of benzodiazepines or other CNS depressants such as alcohol, sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, gabapentinoids (gabapentin or pregabalin), and other opioids, can increase the risk of respiratory depression, profound sedation, coma, and death.
Reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate. Limit dosages and durations to the minimum required. Monitor patients closely for signs of respiratory depression and sedation [see WARNINGS ]. If concomitant use is warranted, consider prescribing naloxone for the emergency treatment of opioid overdose.
Serotonergic Drugs
The concomitant use of opioids with other drugs that affect the serotonergic neurotransmitter system, such as selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that affect the serotonin neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (eg., cyclobenzaprine, metaxalone), and monoamine oxidase (MAO) inhibitors (those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue), has resulted in serotonin syndrome [see PRECAUTIONS; INFORMATION FOR PATIENTS ].
If concomitant use is warranted, regularly monitor the patient, particularly during treatment initiation and dose adjustment. Discontinue Butorphanol Tartrate Injection if serotonin syndrome is suspected.
Cytochrome P450 (CYP 450) Interactions
It is not known if the effects of Butorphanol Tartrate Injection are altered by concomitant medications that affect hepatic metabolism of drugs (CYP 450 inhibitors or inducers) (e.g., erythromycin, theophylline, etc.), but physicians should be alert to the possibility that a smaller initial dose and longer intervals between doses may be needed.
Monoamine Oxidase inhibitors (MAOIs)
No information is available about the use of butorphanol concurrently with MAO inhibitors.
Advise patient to avoid concomitant use of these drugs.
DESCRIPTION
Butorphanol tartrate is a synthetically derived opioid agonist-antagonist analgesic of the phenanthrene series. The chemical name is (-)-17-(cyclobutylmethyl) morphinan-3, 14-diol D-(-)- tartrate (1:1) (salt). The molecular formula is C 21 H 29 NO 2 ∙ C 4 H 6 O 6 , which corresponds to a molecular weight of 477.56 and the following structural formula:
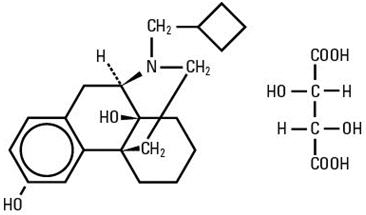
Butorphanol tartrate is a white crystalline substance. The dose is expressed as the tartrate salt. One milligram of the salt is equivalent to 0.68 mg of the free base. The n-octanol/aqueous buffer partition coefficient of butorphanol is 180:1 at pH 7.5.
Butorphanol Tartrate Injection is a sterile, nonpyrogenic parenteral aqueous solution of butorphanol tartrate for intravenous or intramuscular administration.
Each milliliter (mL) contains butorphanol tartrate 1 or 2 mg; sodium citrate, dihydrate, 6.4 mg; citric acid hydrous 3.3 mg; sodium chloride 6.4 mg. The pH is 4.5 (3.0 to 5.5).
CLINICAL PHARMACOLOGY
Mechanism of Action
Butorphanol is a partial opioid agonist at the mu opioid receptor and a full agonist at the kappa opioid receptor. The principal therapeutic action of butorphanol is analgesia. Clinically, dosage is titrated to provide adequate analgesia and may be limited by adverse reactions, including respiratory and CNS depression.
The precise mechanism of the analgesic action is unknown. However, specific CNS opioid receptors for endogenous compounds with opioid-like activity have been identified throughout the brain and spinal cord and are thought to play a role in the analgesic effects of this drug.
Pharmacodynamics
The analgesic effect of butorphanol is influenced by the route of administration. Onset of analgesia is within a few minutes for intravenous administration and within 15 minutes for intramuscular injection.
Peak analgesic activity occurs within 30 to 60 minutes following intravenous and intramuscular administration.
The duration of analgesia varies depending on the pain model as well as the route of administration, but is generally 3 to 4 hours with IM and IV doses as defined by the time 50% of patients required remedication. In postoperative studies, the duration of analgesia with IV or IM butorphanol was similar to morphine, meperidine and pentazocine when administered in the same fashion at equipotent doses [see Clinical Trials ].
Effects on the Central Nervous System
Butorphanol produces respiratory depression by direct action on brain stem respiratory centers. The respiratory depression involves a reduction in the responsiveness of the brain stem respiratory centers to both increases in carbon dioxide tension and electrical stimulation.
In human studies involving individuals without significant respiratory dysfunction, 2 mg of butorphanol IV and 10 mg of morphine sulfate IV depressed respiration to a comparable degree. At higher doses, the magnitude of respiratory depression with butorphanol is not appreciably increased; however, the duration of respiratory depression is longer. Respiratory depression noted after administration of butorphanol to humans by any route is reversed by treatment with naloxone, a specific opioid antagonist [see OVERDOSAGE ].
Butorphanol, like other mixed agonist-antagonists with a high affinity for the kappa receptor, may produce unpleasant psychotomimetic effects in some individuals.
Nausea and/or vomiting may be produced by doses of 1 mg or more administered by any route.
In human studies of butorphanol [see CLINICAL PHARMACOLOGY; Clinical Trials ], sedation is commonly noted at doses of 0.5 mg or more. Narcosis is produced by 10 to 12 mg doses of butorphanol administered over 10 to 15 minutes intravenously.
Butorphanol causes miosis, even in total darkness. Pinpoint pupils are a sign of opioid overdose but are not pathognomonic (e.g., pontine lesions of hemorrhagic or ischemic origins may produce similar findings). Marked mydriasis rather than miosis may be seen due to hypoxia in overdose situations.
Effects on the Gastrointestinal Tract and Other Smooth Muscle
Butorphanol causes a reduction in motility associated with an increase in smooth muscle tone in the antrum of the stomach and duodenum. Digestion of food in the small intestine is delayed and propulsive contractions are decreased. Propulsive peristaltic waves in the colon are decreased, while tone may be increased to the point of spasm, resulting in constipation. Other opioid-induced effects may include a reduction in biliary and pancreatic secretions, spasm of sphincter of Oddi, transient elevations in serum amylase, and opioid-induced esophageal dysfunction (OIED).
Effects on the Cardiovascular System
Hemodynamic changes noted during cardiac catheterization in patients receiving single 0.025 mg/kg intravenous doses of butorphanol have included increases in pulmonary artery pressure, wedge pressure and vascular resistance, increases in left ventricular end diastolic pressure and in systemic arterial pressure.
Effects on the Endocrine System
Opioids inhibit the secretion of adrenocorticotropic hormone (ACTH), cortisol, and luteinizing hormone (LH) in humans [see ADVERSE REACTIONS ]. They also stimulate prolactin, growth hormone (GH) secretion, and pancreatic secretion of insulin and glucagon.
Use of opioids for an extended period of time may influence the hypothalamic-pituitary-gonadal axis, leading to androgen deficiency that may manifest as low libido, impotence, erectile dysfunction, amenorrhea, or infertility. The causal role of opioids in the clinical syndrome of hypogonadism is unknown because the various medical, physical, lifestyle, and psychological stressors that may influence gonadal hormone levels have not been adequately controlled for in studies conducted to date [see ADVERSE REACTIONS ].
Effects on the Immune System
Opioids have been shown to have a variety of effects on components of the immune system. The clinical significance of these findings is unknown. Overall, the effects of opioids appear to be modestly immunosuppressive.
Concentration–Efficacy Relationships
The minimum effective analgesic concentration will vary widely among patients, especially among patients who have been previously treated with opioid agonists. The minimum effective analgesic concentration of butorphanol for any individual patient may increase over time due to an increase in pain, the development of a new pain syndrome, and/or the development of analgesic tolerance [see DOSAGE AND ADMINISTRATION ].
Concentration–Adverse Reaction Relationships
There is a relationship between increasing butorphanol plasma concentration and increasing frequency of dose-related opioid adverse reactions such as nausea, vomiting, CNS effects, and respiratory depression. In opioid-tolerant patients, the situation may be altered by the development of tolerance to opioid-related adverse reactions [see DOSAGE AND ADMINISTRATION ].
Pharmacokinetics
Butorphanol Tartrate Injection is rapidly absorbed after IM injection and peak plasma levels are reached in 20 to 40 minutes.
Following its initial absorption/distribution phase, the single-dose pharmacokinetics of butorphanol by the intravenous and intramuscular routes of administration are similar (see Figure 1).
| Figure 1—Butorphanol Plasma Levels After IV and IM Administration of 2 mg Dose |
|---|
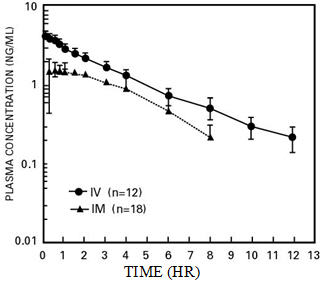 |
Serum protein binding is independent of concentration over the range achieved in clinical practice (up to 7 ng/mL) with a bound fraction of approximately 80%.
The volume of distribution of butorphanol varies from 305 to 901 liters and total body clearance from 52 to 154 liters/hr (see Table 1 ).
| Parameters | Young | Elderly |
|---|---|---|
AUC (inf) Area under plasma concentration-time curve after a 1 mg dose. | 7.24 (1.57) Mean (1S.D.). | 8.71 (2.02) |
(hr ∙ ng/mL) | (4.40–9.77) (range of observed values). | (4.76–13.03) |
Half-life (hr) | 4.56 (1.67) | 5.61 (1.36) |
(2.06–8.70) | (3.25–8.79) | |
Volume of Distribution Derived from IV data. (L) | 487 (155) (305–901) | 552 (124) (305–737) |
Total body | 99 (23) | 82 (21) |
Clearance (L/hr) | (70–154) | (52–143) |
The drug is transported across the blood-brain and placental barriers and into human milk [see PRECAUTIONS: Labor or Delivery and Nursing Mothers ].
Butorphanol is extensively metabolized in the liver. Metabolism is qualitatively and quantitatively similar following intravenous or intramuscular administration. Oral bioavailability is only 5 to 17% because of extensive first pass metabolism of butorphanol.
The major metabolite of butorphanol is hydroxybutorphanol, while norbutorphanol is produced in small amounts. Both have been detected in plasma following administration of butorphanol, with norbutorphanol present at trace levels at most time points. The elimination half-life of hydroxybutorphanol is about 18 hours and, as a consequence, considerable accumulation (~5-fold) occurs when butorphanol is dosed to steady state.
Elimination occurs by urine and fecal excretion. When 3 H labeled butorphanol is administered to normal subjects, most (70 to 80%) of the dose is recovered in the urine, while approximately 15% is recovered in the feces.
About 5% of the dose is recovered in the urine as butorphanol. Forty-nine percent is eliminated in the urine as hydroxybutorphanol. Less than 5% is excreted in the urine as norbutorphanol.
Butorphanol pharmacokinetics in the elderly differ from younger patients (see Table 1 ).
In renally impaired patients with creatinine clearances <30 mL/min, the elimination half-life was approximately doubled and the total body clearance was approximately one half (10.5 hours [clearance 150 L/h] compared to 5.8 hours [clearance 260 L/h] in healthy subjects). No effect on C max or T max was observed after a single-dose.
After intravenous administration to patients with hepatic impairment, the elimination half-life of butorphanol was approximately tripled and total body clearance was approximately one half (half-life 16.8 hours, clearance 92 L/h) compared to healthy subjects (half-life 4.8 hours, clearance 175 L/h). The exposure of hepatically impaired patients to butorphanol was significantly greater (about 2-fold) than that in healthy subjects [see PRECAUTIONS: Hepatic and Renal Disease , Drug Interactions and Geriatric Use and CLINICAL PHARMACOLOGY: Individualization of Dosage ].
Clinical Trials
The effectiveness of opioid analgesics varies in different pain syndromes. Studies with Butorphanol Tartrate Injection have been performed in postoperative (primarily abdominal and orthopedic) pain and pain during labor and delivery, as preoperative and preanesthetic medication, and as a supplement to balanced anesthesia (see below).
Use in the Management of Pain-Postoperative Pain
The analgesic efficacy of Butorphanol Tartrate Injection in postoperative pain was investigated in several double-blind active-controlled studies involving 958 butorphanol-treated patients. The following doses were found to have approximately equivalent analgesic effect: 2 mg butorphanol, 10 mg morphine, 40 mg pentazocine and 80 mg meperidine.
After intravenous administration of butorphanol tartrate, onset and peak analgesic effect occurred by the time of first observation (30 minutes). After intramuscular administration, pain relief onset occurred at 30 minutes or less, and peak effect occurred between 30 minutes and one hour. The duration of action of Butorphanol Tartrate Injection was 3 to 4 hours when defined as the time necessary for pain intensity to return to pretreatment level or the time to retreatment.
Preanesthetic Medication
Butorphanol Tartrate Injection, (2 mg and 4 mg) and meperidine (80 mg) were studied for use as preanesthetic medication in hospitalized surgical patients. Patients received a single intramuscular dose of either butorphanol or meperidine approximately 90 minutes prior to anesthesia. The anesthesia regimen included barbiturate induction, followed by nitrous oxide and oxygen with halothane or enflurane, with or without a muscle relaxant.
Anesthetic preparation was rated as satisfactory in all 42 butorphanol injection patients regardless of the type of surgery.
Balanced Anesthesia
Butorphanol tartrate administered intravenously (mean dose 2 mg) was compared to intravenous morphine sulfate (mean dose 10 mg) as premedication shortly before thiopental induction, followed by balanced anesthesia in 50 ASA Class 1 and 2 patients. Anesthesia was then maintained by repeated intravenous doses, averaging 4.6 mg butorphanol and 22.8 mg morphine per patient.
Anesthetic induction and maintenance were generally rated as satisfactory with both butorphanol injection (25 patients) and morphine (25 patients) regardless of the type of surgery performed. Emergence from anesthesia was comparable with both agents.
Labor
[see PRECAUTIONS ]
The analgesic efficacy of intravenous Butorphanol Tartrate Injection was studied in pain during labor. In a total of 145 patients butorphanol (1 mg and 2 mg) was as effective as 40 mg and 80 mg of meperidine (144 patients) in the relief of pain in labor with no effect on the duration or progress of labor. Both drugs readily crossed the placenta and entered fetal circulation. The condition of the infants in these studies, determined by Apgar scores at 1 and 5 minutes (8 or above) and time to sustained respiration, showed that butorphanol had the same effects on the infants as meperidine.
In these studies neurobehavioral testing in infants exposed to butorphanol injection at a mean of 18.6 hours after delivery, showed no significant differences between treatment groups.
Individualization of Dosage
Use of butorphanol in geriatric patients, patients with renal impairment, patients with hepatic impairment and during labor requires extra caution [see below and the appropriate sections in PRECAUTIONS ].
For pain relief the recommended initial dosage regimen of Butorphanol Tartrate Injection is 1 mg IV or 2 mg IM with repeated doses every three to four hours as necessary. This dosage regimen is likely to be effective for the majority of patients. Dosage adjustments of butorphanol injection should be based on observations of its beneficial and adverse effects. The initial dose in the elderly and in patients with renal or hepatic impairment should generally be half the recommended adult dose (0.5 mg IV and 1 mg IM). Repeat doses in these patients should be determined by the patient's response rather than at fixed intervals but will generally be no less than 6 hours [see PRECAUTIONS ].
The usual preoperative dose is 2 mg IM given 60 to 90 minutes before surgery or 2 mg IV shortly before induction. This is approximately equivalent in sedative effect to 10 mg morphine or 80 mg of meperidine. This single preoperative dose should be individualized based on age, body weight, physical status, underlying pathological condition, use of other drugs, type of anesthesia to be used and the surgical procedure involved.
During maintenance in balanced anesthesia the usual incremental dose of butorphanol tartrate is 0.5 to 1 mg IV. The incremental dose may be higher, up to 0.06 mg/kg (4 mg/70 kg), depending on previous sedative, analgesic, and hypnotic drugs administered. The total dose of butorphanol injection will vary; however, patients seldom require less than 4 mg or more than 12.5 mg (approximately 0.06 to 0.18 mg/kg).
As with other opioids of this class, butorphanol injection may not provide adequate intraoperative analgesia in every patient or under all conditions. A failure to achieve successful analgesia during balanced anesthesia is commonly reflected by increases in general sympathetic tone. Consequently, if blood pressure or heart rate continue to rise, consideration should be given to adding a potent volatile liquid inhalation anesthetic or another intravenous medication.
In labor, the recommended initial dose of butorphanol tartrate is 1 or 2 mg IM or IV in mothers with fetuses of 37 weeks gestation or beyond and without signs of fetal distress. Dosage adjustments of butorphanol in labor should be based on initial response with consideration given to concomitant analgesic or sedative drugs and the expected time of delivery. A dose should not be repeated in less than four hours nor administered less than four hours prior to the anticipated delivery [see PRECAUTIONS ].
HOW SUPPLIED
Butorphanol Tartrate Injection, USP is supplied as single-dose glass fliptop vials, and available as follows:
| Unit of Sale | Concentration (Total Butorphanol Concentration Per Container) |
|---|---|
NDC 0409-1623-01 Carton of 10 – 1 mL Single-Dose Glass Fliptop Vials | 1 mg/mL |
NDC 0409-1626-01 Carton of 10 – 1 mL Single-Dose Glass Fliptop Vials | 2 mg/mL |
NDC 0409-1626-02 Carton of 10 – 2 mL Single-Dose Glass Fliptop Vials | 4 mg/2 mL (2 mg/mL) |
Store at 20°C to 25°C (68°F to 77°F). [See USP Controlled Room Temperature.]
Protect from light.
Mechanism of Action
Butorphanol is a partial opioid agonist at the mu opioid receptor and a full agonist at the kappa opioid receptor. The principal therapeutic action of butorphanol is analgesia. Clinically, dosage is titrated to provide adequate analgesia and may be limited by adverse reactions, including respiratory and CNS depression.
The precise mechanism of the analgesic action is unknown. However, specific CNS opioid receptors for endogenous compounds with opioid-like activity have been identified throughout the brain and spinal cord and are thought to play a role in the analgesic effects of this drug.