Get your patient on Carbamazepine - Carbamazepine tablet (Carbamazepine)
Carbamazepine - Carbamazepine tablet prescribing information
WARNINGS
SERIOUS DERMATOLOGIC REACTIONS AND HLA-B•1502 ALLELE
SERIOUS AND SOMETIMES FATAL DERMATOLOGIC REACTIONS, INCLUDING TOXIC EPIDERMAL NECROLYSIS (TEN) AND STEVENS-JOHNSON SYNDROME (SJS), HAVE BEEN REPORTED DURING TREATMENT WITH CARBAMAZEPINE. THESE REACTIONS ARE ESTIMATED TO OCCUR IN 1 TO 6 PER 10,000 NEW USERS IN COUNTRIES WITH MAINLY CAUCASIAN POPULATIONS, BUT THE RISK IN SOME ASIAN COUNTRIES IS ESTIMATED TO BE ABOUT 10 TIMES HIGHER. STUDIES IN PATIENTS OF CHINESE ANCESTRY HAVE FOUND A STRONG ASSOCIATION BETWEEN THE RISK OF DEVELOPING SJS/TEN AND THE PRESENCE OF HLA-B•1502, AN INHERITED ALLELIC VARIANT OF THE HLA-B GENE. HLA-B•1502 IS FOUND ALMOST EXCLUSIVELY IN PATIENTS WITH ANCESTRY ACROSS BROAD AREAS OF ASIA. PATIENTS WITH ANCESTRY IN GENETICALLY AT-RISK POPULATIONS SHOULD BE SCREENED FOR THE PRESENCE OF HLA-B•1502 PRIOR TO INITIATING TREATMENT WITH CARBAMAZEPINE. PATIENTS TESTING POSITIVE FOR THE ALLELE SHOULD NOT BE TREATED WITH CARBAMAZEPINE UNLESS THE BENEFIT CLEARLY OUTWEIGHS THE RISK (SEE WARNINGS AND PRECAUTIONS, LABORATORY TESTS).
APLASTIC ANEMIA AND AGRANULOCYTOSIS
APLASTIC ANEMIA AND AGRANULOCYTOSIS HAVE BEEN REPORTED IN ASSOCIATION WITH THE USE OF CARBAMAZEPINE. DATA FROM A POPULATION-BASED CASE CONTROL STUDY DEMONSTRATE THAT THE RISK OF DEVELOPING THESE REACTIONS IS 5 TO 8 TIMES GREATER THAN IN THE GENERAL POPULATION. HOWEVER, THE OVERALL RISK OF THESE REACTIONS IN THE UNTREATED GENERAL POPULATION IS LOW, APPROXIMATELY SIX PATIENTS PER ONE MILLION POPULATION PER YEAR FOR AGRANULOCYTOSIS AND TWO PATIENTS PER ONE MILLION POPULATION PER YEAR FOR APLASTIC ANEMIA.
ALTHOUGH REPORTS OF TRANSIENT OR PERSISTENT DECREASED PLATELET OR WHITE BLOOD CELL COUNTS ARE NOT UNCOMMON IN ASSOCIATION WITH THE USE OF CARBAMAZEPINE, DATA ARE NOT AVAILABLE TO ESTIMATE ACCURATELY THEIR INCIDENCE OR OUTCOME. HOWEVER, THE VAST MAJORITY OF THE CASES OF LEUKOPENIA HAVE NOT PROGRESSED TO THE MORE SERIOUS CONDITIONS OF APLASTIC ANEMIA OR AGRANULOCYTOSIS.
BECAUSE OF THE VERY LOW INCIDENCE OF AGRANULOCYTOSIS AND APLASTIC ANEMIA, THE VAST MAJORITY OF MINOR HEMATOLOGIC CHANGES OBSERVED IN MONITORING OF PATIENTS ON CARBAMAZEPINE ARE UNLIKELY TO SIGNAL THE OCCURRENCE OF EITHER ABNORMALITY. NONETHELESS, COMPLETE PRETREATMENT HEMATOLOGICAL TESTING SHOULD BE OBTAINED AS A BASELINE. IF A PATIENT IN THE COURSE OF TREATMENT EXHIBITS LOW OR DECREASED WHITE BLOOD CELL OR PLATELET COUNTS, THE PATIENT SHOULD BE MONITORED CLOSELY. DISCONTINUATION OF THE DRUG SHOULD BE CONSIDERED IF ANY EVIDENCE OF SIGNIFICANT BONE MARROW DEPRESSION DEVELOPS.
INDICATIONS AND USAGE
Epilepsy Carbamazepine tablets are indicated for use as an anticonvulsant drug. Evidence supporting efficacy of carbamazepine as an anticonvulsant was derived from active drug-controlled studies that enrolled patients with the following seizure types: 1. Partial seizures with complex symptomatology (psychomotor, temporal lobe). Patients with these seizures appear to show greater improvement than those with other types. 2. Generalized tonic-clonic seizures (grand mal). 3. Mixed seizure patterns which include the above, or other partial or generalized seizures. Absence seizures (petit mal) do not appear to be controlled by carbamazepine (see PRECAUTIONS, General).
Trigeminal Neuralgia Carbamazepine tablets are indicated in the treatment of the pain associated with true trigeminal neuralgia.
Beneficial results have also been reported in glossopharyngeal neuralgia.
This drug is not a simple analgesic and should not be used for the relief of trivial aches or pains.
DOSAGE AND ADMINISTRATION (SEE TABLE BELOW)
Tegretol suspension in combination with liquid chlorpromazine or thioridazine results in precipitate formation, and, in the case of chlorpromazine, there has been a report of a patient passing an orange rubbery precipitate in the stool following co administration of the two drugs (see PRECAUTIONS, Drug Interactions). Because the extent to which this occurs with other liquid medications is not known, Tegretol suspension should not be administered simultaneously with other liquid medications or diluents.
Monitoring of blood levels has increased the efficacy and safety of anticonvulsants (see PRECAUTIONS, Laboratory Tests). Dosage should be adjusted to the needs of the individual patient. A low initial daily dosage with a gradual increase is advised. As soon as adequate control is achieved, the dosage may be reduced very gradually to the minimum effective level. Medication should be taken with meals.
Since a given dose of Tegretol suspension will produce higher peak levels than the same dose given as the tablet, it is recommended to start with low doses (children 6 to 12 years: ½ teaspoon four times a day and to increase slowly to avoid unwanted side effects.
Conversion of patients from oral carbamazepine tablets to Tegretol suspension: Patients should be converted by administering the same number of mg per day in smaller, more frequent doses (i.e., twice a day tablets to three times a day suspension).
Tegretol-XR is an extended-release formulation for twice a day administration. When converting patients from carbamazepine conventional tablets to Tegretol-XR, the same total daily mg dose of Tegretol-XR should be administered. Tegretol-XR tablets must be swallowed whole and never crushed or chewed. Tegretol-XR tablets should be inspected for chips or cracks. Damaged tablets, or tablets without a release portal, should not be consumed. Tegretol-XR tablet coating is not absorbed and is excreted in the feces; these coatings may be noticeable in the stool.
Epilepsy (SEE INDICATIONS AND USAGE )
Adults and children over 12 years of age-Initial: Either 200 mg twice a day for tablets and XR tablets, or 1 teaspoon four times a day for suspension (400 mg/day). Increase at weekly intervals by adding up to 200 mg/day using a twice a day regimen of Tegretol-XR or a three times a day or four times a day regimen of the other formulations until the optimal response is obtained. Dosage generally should not exceed 1000 mg daily in children 12 to 15 years of age, and 1200 mg daily in patients above 15 years of age. Doses up to 1600 mg daily have been used in adults in rare instances. Maintenance: Adjust dosage to the minimum effective level, usually 800 to 1200 mg daily.
Children 6 to 12 years of age-Initial: Either 100 mg twice a day for tablets or XR tablets, or ½ teaspoon four times a day for suspension (200 mg/day). Increase at weekly intervals by adding up to 100 mg/day using a twice a day regimen of Tegretol-XR or a three times a day or four times a day regimen of the other formulations until the optimal response is obtained. Dosage generally should not exceed 1000 mg daily. Maintenance: Adjust dosage to the minimum effective level, usually 400 to 800 mg daily.
Children under 6 years of age-Initial: 10 to 20 mg/kg/day twice a day or three times a day as tablets, or four times a day as suspension. Increase weekly to achieve optimal clinical response administered three times a day or four times a day. Maintenance: Ordinarily, optimal clinical response is achieved at daily doses below 35 mg/kg. If satisfactory clinical response has not been achieved, plasma levels should be measured to determine whether or not they are in the therapeutic range. No recommendation regarding the safety of carbamazepine for use at doses above 35 mg/kg/24 hours can be made.
Combination Therapy: Carbamazepine may be used alone or with other anticonvulsants. When added to existing anticonvulsant therapy, the drug should be added gradually while the other anticonvulsants are maintained or gradually decreased, except phenytoin, which may have to be increased (see PRECAUTIONS, Drug Interactions, and Pregnancy).
Trigeminal Neuralgia (SEE INDICATIONS AND USAGE)
Initial: On the first day, either 100 mg twice a day for tablets or XR tablets, or ½ teaspoon four times a day for suspension, for a total daily dose of 200 mg. This daily dose may be increased by up to 200 mg/day using increments of 100 mg every 12 hours for tablets or XR tablets, or 50 mg (½ teaspoon) four times a day for suspension, only as needed to achieve freedom from pain. Do not exceed 1200 mg daily. Maintenance: Control of pain can be maintained in most patients with 400 to 800 mg daily. However, some patients may be maintained on as little as 200 mg daily, while others may require as much as 1200 mg daily. At least once every 3 months throughout the treatment period, attempts should be made to reduce the dose to the minimum effective level or even to discontinue the drug.
Dosage Information
| Initial Dose | Subsequent Dose | Maximum Daily Dose | |||||||
| Indication | Tablet • | XR † | Suspension | Tablet • | XR † | Suspension | Tablet • | XR † | Suspension |
| Epilepsy Under 6 yr | 10 to 20 mg/kg/day twice a day or 3 times a day | 10 to 20 mg/kg/day 4 times a day | Increase weekly to achieve optimal clinical response, 3 times a day or 4 times a day | Increase weekly to achieve optimal clinical response, 3 times a day or 4 times a day | 35 mg/kg/24 hr (see Dosage and Administration section above) | 35 mg/kg/24 hr (see Dosage and Administration section above) | |||
| 6 to 12 yr | 100 mg twice a day (200 mg/day) | 100 mg twice a day (200 mg/day) | ½ tsp 4 times a day (200 mg/day) | Add up to 100 mg/day at weekly intervals, 3 times a day or 4 times a day | Add 100 mg/day at weekly intervals, twice a day | Add up to 1 tsp (100 mg)/day at weekly intervals, 3 times a day or 4 times a day | 1000 mg/24 hr | ||
| Over 12 yr | 200 mg twice a day (400 mg/day) | 200 mg twice a day (400 mg/day) | 1 tsp 4 times a day (400 mg/day) | Add up to 200 mg/day at weekly intervals, 3 times a day or 4 times a day | Add up to 200 mg/day at weekly intervals, twice a day | Add up to 2 tsp (200 mg)/day at weekly intervals, 3 times a day or 4 times a day | 1000 mg/24 hr (12 to 15 yr) 1200 mg/24 hr (> 15 yr) 1600 mg/24 hr (adults, in rare instances) | ||
| Trigeminal Neuralgia | 100 mg twice a day (200 mg/day) | 100 mg twice a day (200 mg/day) | ½ tsp 4 times a day (200 mg/day) | Add up to 200 mg/day in increments of 100 mg every 12 hr | Add up to 200 mg/day in increments of 100 mg every 12 hr | Add up to 2 tsp (200 mg)/day in increments of 50 mg (½ tsp) 4 times a day | 1200 mg/24 hr | ||
• Tablet = Chewable or conventional tablets † XR = Tegretol -XR extended-release tablets
CONTRAINDICATIONS
Carbamazepine should not be used in patients with a history of previous bone marrow depression, hypersensitivity to the drug, or known sensitivity to any of the tricyclic compounds, such as amitriptyline, desipramine, imipramine, protriptyline, nortriptyline, etc. Likewise, on theoretical grounds its use with monoamine oxidase (MAO) inhibitors is not recommended. Before administration of carbamazepine, MAO inhibitors should be discontinued for a minimum of 14 days, or longer if the clinical situation permits.
Coadministration of carbamazepine and nefazodone may result in insufficient plasma concentrations of nefazodone and its active metabolite to achieve a therapeutic effect. Coadministration of carbamazepine with nefazodone is contraindicated.
ADVERSE REACTIONS
If adverse reactions are of such severity that the drug must be discontinued, the physician must be aware that abrupt discontinuation of any anticonvulsant drug in a responsive epileptic patient may lead to seizures or even status epilepticus with its life-threatening hazards.
The most severe adverse reactions have been observed in the hemopoietic system and skin (see BOXED WARNING), the liver, and the cardiovascular system.
The most frequently observed adverse reactions, particularly during the initial phases of therapy, are dizziness, drowsiness, unsteadiness, nausea, and vomiting. To minimize the possibility of such reactions, therapy should be initiated at the lowest dosage recommended.
The following additional adverse reactions have been reported:
Hemopoietic System: Aplastic anemia, agranulocytosis, pancytopenia, bone marrow depression, thrombocytopenia, leukopenia, leukocytosis, eosinophilia, acute intermittent porphyria, variegate porphyria, porphyria cutanea tarda.
Skin: Toxic epidermal necrolysis (TEN) and Stevens-Johnson syndrome (SJS) (see BOXED WARNING), Acute Generalized Exanthematous Pustulosis (AGEP), pruritic and erythematous rashes, urticaria, photosensitivity reactions, alterations in skin pigmentation, exfoliative dermatitis, erythema multiforme and nodosum, purpura, aggravation of disseminated lupus erythematosus, alopecia, diaphoresis, onychomadesis and hirsutism. In certain cases, discontinuation of therapy may be necessary.
Cardiovascular System: Congestive heart failure, edema, aggravation of hypertension, hypotension, syncope and collapse, aggravation of coronary artery disease, arrhythmias and AV block, thrombophlebitis, thromboembolism (e.g., pulmonary embolism), and adenopathy or lymphadenopathy.
Some of these cardiovascular complications have resulted in fatalities. Myocardial infarction has been associated with other tricyclic compounds.
Liver: Abnormalities in liver function tests, cholestatic and hepatocellular jaundice, hepatitis, very rare cases of hepatic failure.
Pancreatic: Pancreatitis.
Respiratory System: Pulmonary hypersensitivity characterized by fever, dyspnea, pneumonitis, or pneumonia.
Genitourinary System: Urinary frequency, acute urinary retention, oliguria with elevated blood pressure, azotemia, renal failure, and impotence. Albuminuria, glycosuria, elevated BUN, and microscopic deposits in the urine have also been reported. There have been rare reports of impaired male fertility and/or abnormal spermatogenesis.
Testicular atrophy occurred in rats receiving carbamazepine orally from 4 to 52 weeks at dosage levels of 50 to 400 mg/kg/day. Additionally, rats receiving carbamazepine in the diet for 2 years at dosage levels of 25, 75, and 250 mg/kg/day had a dose-related incidence of testicular atrophy and aspermatogenesis. In dogs, it produced a brownish discoloration, presumably a metabolite, in the urinary bladder at dosage levels of 50 mg/kg and higher. Relevance of these findings to humans is unknown.
Nervous System: Dizziness, drowsiness, disturbances of coordination, confusion, headache, fatigue, blurred vision, visual hallucinations, transient diplopia, oculomotor disturbances, nystagmus, speech disturbances, abnormal involuntary movements, peripheral neuritis and paresthesias, depression with agitation, talkativeness, tinnitus, hyperacusis, neuroleptic malignant syndrome.
There have been reports of associated paralysis and other symptoms of cerebral arterial insufficiency, but the exact relationship of these reactions to the drug has not been established.
Isolated cases of neuroleptic malignant syndrome have been reported both with and without concomitant use of psychotropic drugs.
Digestive System: Nausea, vomiting, gastric distress and abdominal pain, diarrhea, constipation, anorexia, and dryness of the mouth and pharynx, including glossitis and stomatitis.
Eyes: Scattered punctate cortical lens opacities, increased intraocular pressure (see WARNINGS, General) as well as conjunctivitis, have been reported. Although a direct causal relationship has not been established, many phenothiazines and related drugs have been shown to cause eye changes.
Musculoskeletal System: Aching joints and muscles, and leg cramps.
Metabolism: Fever and chills. Hyponatremia (see WARNINGS, General). Decreased levels of plasma calcium have been reported. Osteoporosis has been reported.
Isolated cases of a lupus erythematosus-like syndrome have been reported. There have been occasional reports of elevated levels of cholesterol, HDL cholesterol, and triglycerides in patients taking anticonvulsants.
A case of aseptic meningitis, accompanied by myoclonus and peripheral eosinophilia, has been reported in a patient taking carbamazepine in combination with other medications. The patient was successfully dechallenged, and the meningitis reappeared upon rechallenge with carbamazepine.
Drug Interactions
There has been a report of a patient who passed an orange rubbery precipitate in his stool the day after ingesting Tegretol suspension immediately followed by Thorazine ® • solution. Subsequent testing has shown that mixing Tegretol suspension and chlorpromazine solution (both generic and brand name) as well as Tegretol suspension and liquid Mellaril ® , resulted in the occurrence of this precipitate. Because the extent to which this occurs with other liquid medications is not known, Tegretol suspension should not be administered simultaneously with other liquid medicinal agents or diluents (see DOSAGE AND ADMINISTRATION).
Clinically meaningful drug interactions have occurred with concomitant medications and include (but are not limited to) the following:
Agents That May Affect Carbamazepine Plasma Levels
When carbamazepine is given with drugs that can increase or decrease carbamazepine levels, close monitoring of carbamazepine levels is indicated and dosage adjustment may be required.
Agents That Increase Carbamazepine Levels
CYP3A4 inhibitors inhibit carbamazepine metabolism and can thus increase plasma carbamazepine levels. Drugs that have been shown, or would be expected, to increase plasma carbamazepine levels include aprepitant, cimetidine, ciprofloxacin, danazol, diltiazem, macrolides (e.g., erythromycin, clarithromycin), fluoxetine, fluvoxamine, trazodone, omeprazole, oxybutynin, isoniazid, niacinamide (nicotinamide), azoles (e.g., ketaconazole, itraconazole, fluconazole, voriconazole), acetazolamide, verapamil, ticlopidine, grapefruit juice, and protease inhibitors.
Human microsomal epoxide hydrolase has been identified as the enzyme responsible for the formation of the 10, 11-transdiol derivative from carbamazepine-10, 11 epoxide. Coadministration of inhibitors of human microsomal epoxide hydrolase may result in increased carbamazepine-10, 11 epoxide plasma concentrations. Accordingly, the dosage of carbamazepine should be adjusted and/or the plasma levels monitored when used concomitantly with loxapine, quetiapine, or valproic acid, or brivaracetam.
Agents That Decrease Carbamazepine Levels
CYP3A4 inducers can increase the rate of carbamazepine metabolism. Drugs that have been shown, or that would be expected, to decrease plasma carbamazepine levels include cisplatin, doxorubicin HCl, felbamate, fosphenytoin, rifampin, phenobarbital, phenytoin, primidone, methsuximide, theophylline, aminophylline.
Effect of Carbamazepine on Plasma Levels of Concomitant Agents
Decreased Levels of Concomitant Medications
Carbamazepine is a potent inducer of hepatic 3A4 and is also known to be an inducer of CYP1A2, 2B6, 2C8/9/19 and may therefore reduce plasma concentrations of co-medications mainly metabolized by CYP 1A2, 2B6, 2C8/9/19 and 3A4, through induction of their metabolism. When used concomitantly with carbamazepine, monitoring of concentrations or dosage adjustment of these agents may be necessary:
- When carbamazepine is added to aripiprazole, the aripiprazole dose should be doubled. Additional dose increases should be based on clinical evaluation. If carbamazepine is later withdrawn, the aripiprazole dose should be reduced.
- When carbamazepine is used with tacrolimus, monitoring of tacrolimus blood concentrations and appropriate dosage adjustments are recommended.
- The use of concomitant strong CYP3A4 inducers, such as carbamazepine should be avoided with temsirolimus. If patients must be coadministered carbamazepine with temsirolimus, an adjustment of temsirolimus dosage should be considered.
- The use of carbamazepine with lapatinib should generally be avoided. If carbamazepine is started in a patient already taking lapatinib, the dose of lapatinib should be gradually titrated up. If carbamazepine is discontinued, the lapatinib dose should be reduced.
- Concomitant use of carbamazepine with nefazodone results in plasma concentrations of nefazodone and its active metabolite insufficient to achieve a therapeutic effect. Coadministration of carbamazepine with nefazodone is contraindicated (see CONTRAINDICATIONS).
- Monitor concentrations of valproate when carbamazepine is introduced or withdrawn in patients using valproic acid.
In addition, carbamazepine causes, or would be expected to cause, decreased levels of the following drugs, for which monitoring of concentrations or dosage adjustment may be necessary: acetaminophen, albendazole, alprazolam, aprepitant, buprenorphone, bupropion, citalopram, clonazepam, clozapine, corticosteroids (e.g., prednisolone, dexamethasone), cyclosporine, dicumarol, dihydropyridine calcium channel blockers (e.g., felodipine), doxycycline, eslicarbazepine, ethosuximide, everolimus, haloperidol, imatinib, itraconazole, lamotrigine, levothyroxine, methadone, methsuximide, mianserin, midazolam, olanzapine, oral and other hormonal contraceptives, oxcarbazepine, paliperidone, phensuximide, phenytoin, praziquantel, protease inhibitors, risperidone, sertraline, sirolimus, tadalafil, theophylline, tiagabine, topiramate, tramadol, trazodone, tricyclic antidepressants (e.g., imipramine, amitriptyline, nortriptyline),valproate, warfarin, ziprasidone, zonisamide.
Other Drug Interactions
- Cyclophosphamide is an inactive prodrug and is converted to its active metabolite in part by CYP3A. The rate of metabolism and the leukopenic activity of cyclophosphamide are reportedly increased by chronic coadministration of CYP3A4 inducers. There is a potential for increased cyclophosphamide toxicity when coadministered with carbamazepine.
- Concomitant administration of carbamazepine and lithium may increase the risk of neurotoxic side effects.
- Concomitant use of carbamazepine with olanzapine, dantrolene, or ibuprofen may increase plasma carbamazepine levels.
- Concomitant use of carbamazepine and isoniazid has been reported to increase isoniazid-induced hepatotoxicity.
- Alterations of thyroid function have been reported in combination therapy with other anticonvulsant medications.
- Concomitant use of carbamazepine with hormonal contraceptive products (e.g., oral, and levonorgestrel subdermal implant contraceptives) may render the contraceptives less effective because the plasma concentrations of the hormones may be decreased. Breakthrough bleeding and unintended pregnancies have been reported. Alternative or back-up methods of contraception should be considered.
- Resistance to the neuromuscular blocking action of the nondepolarizing neuromuscular blocking agents pancuronium, vecuronium, rocuronium and cisatracurium has occurred in patients chronically administered carbamazepine. Whether or not carbamazepine has the same effect on other non-depolarizing agents is unknown. Patients should be monitored closely for more rapid recovery from neuromuscular blockade than expected, and infusion rate requirements may be higher.
- Concomitant use of carbamazepine with rivaroxaban, apixaban, dabigatran, and edoxaban (direct acting oral anticoagulants) is expected to result in decreased plasma concentrations of these anticoagulants that may be insufficient to achieve the intended therapeutic effect. In general, coadministration of carbamazepine with rivaroxaban, apixaban, dabigatran, and edoxaban should be avoided.
DESCRIPTION
Carbamazepine USP, is an anticonvulsant and specific analgesic for trigeminal neuralgia, available for oral administration as tablets of 200 mg. Its chemical name is 5 H -dibenz[ b,f ]azepine-5-carboxamide, and its structural formula is:
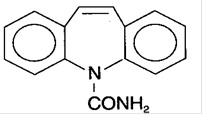
Carbamazepine USP is a white to off-white powder, soluble in alcohol, sparingly soluble in acetone and practically insoluble in water. Its molecular weight is 236.27.
Inactive Ingredients : Microcrystalline cellulose, crospovidone, sodium lauryl sulfate, FD&C Red No. 40 Aluminium Lake, talc and magnesium stearate.
FDA approved dissolution test specifications differ from the USP.
CLINICAL PHARMACOLOGY
In controlled clinical trials, carbamazepine has been shown to be effective in the treatment of psychomotor and grand mal seizures, as well as trigeminal neuralgia.
Mechanism of Action
Carbamazepine has demonstrated anticonvulsant properties in rats and mice with electrically and chemically induced seizures. It appears to act by reducing polysynaptic responses and blocking the post-tetanic potentiation. Carbamazepine greatly reduces or abolishes pain induced by stimulation of the infraorbital nerve in cats and rats. It depresses thalamic potential and bulbar and polysynaptic reflexes, including the linguomandibular reflex in cats. Carbamazepine is chemically unrelated to other anticonvulsants or other drugs used to control the pain of trigeminal neuralgia. The mechanism of action remains unknown.
The principal metabolite of carbamazepine, carbamazepine-10, 11-epoxide, has anticonvulsant activity as demonstrated in several in vivo animal models of seizures. Though clinical activity for the epoxide has been postulated, the significance of its activity with respect to the safety and efficacy of carbamazepine has not been established.
Pharmacokinetics
In clinical studies, Tegretol suspension, conventional tablets, and XR tablets delivered equivalent amounts of drug to the systemic circulation. However, the suspension was absorbed somewhat faster, and the XR tablet slightly slower, than the conventional tablet. The bioavailability of the XR tablet was 89% compared to suspension. Following a twice a day dosage regimen, the suspension provides higher peak levels and lower trough levels than those obtained from the conventional tablet for the same dosage regimen. On the other hand, following a three times a day dosage regimen, Tegretol suspension affords steady-state plasma levels comparable to carbamazepine tablets given twice a day when administered at the same total mg daily dose. Following a twice a day dosage regimen, Tegretol-XR tablets afford steady-state plasma levels comparable to conventional carbamazepine tablets given four times a day, when administered at the same total mg daily dose. Carbamazepine in blood is 76% bound to plasma proteins. Plasma levels of carbamazepine are variable and may range from 0.5 to 25 mcg/mL, with no apparent relationship to the daily intake of the drug. Usual adult therapeutic levels are between 4 and 12 mcg/mL. In polytherapy, the concentration of carbamazepine and concomitant drugs may be increased or decreased during therapy, and drug effects may be altered (see PRECAUTIONS, Drug Interactions). Following chronic oral administration of suspension, plasma levels peak at approximately 1.5 hours compared to 4 to 5 hours after administration of conventional carbamazepine tablets, and 3 to 12 hours after administration of Tegretol-XR tablets. The CSF/serum ratio is 0.22, similar to the 24% unbound carbamazepine in serum. Because carbamazepine induces its own metabolism, the half-life is also variable. Auto induction is completed after 3 to 5 weeks of a fixed dosing regimen. Initial half-life values range from 25 to 65 hours, decreasing to 12 to 17 hours on repeated doses. Carbamazepine is metabolized in the liver. Cytochrome P450 3A4 was identified as the major isoform responsible for the formation of carbamazepine-10, 11-epoxide from carbamazepine. Human microsomal epoxide hydrolase has been identified as the enzyme responsible for the formation of the 10, 11-transdiol derivative from carbamazepine-10, 11epoxide. After oral administration of 14 C-carbamazepine, 72% of the administered radioactivity was found in the urine and 28% in the feces. This urinary radioactivity was composed largely of hydroxylated and conjugated metabolites, with only 3% of unchanged carbamazepine.
The pharmacokinetic parameters of carbamazepine disposition are similar in children and in adults. However, there is a poor correlation between plasma concentrations of carbamazepine and carbamazepine dose in children. Carbamazepine is more rapidly metabolized to carbamazepine-10, 11-epoxide (a metabolite shown to be equipotent to carbamazepine as an anticonvulsant in animal screens) in the younger age groups than in adults. In children below the age of 15, there is an inverse relationship between CBZ-E/CBZ ratio and increasing age (in one report from 0.44 in children below the age of 1 year to 0.18 in children between 10 to 15 years of age).
The effects of race and gender on carbamazepine pharmacokinetics have not been systematically evaluated.
HOW SUPPLIED
Carbamazepine tablets USP, 200 mg having functional scoring are supplied as capsule-shaped, pink, single-scored tablets, debossed with “L802” on one side and scored on the other side.
Bottle of 60 tablets with child resistant closure, NDC 46708-731-60
Bottle of 100 tablets with child resistant closure, NDC 46708-731-31
Bottle of 1000 tablets, NDC 46708-731-91
Carton of 100 (10 x 10) unit-dose tablets, NDC 46708-731-10
Store at 25°C (77°F); excursions permitted to 15° to 30°C (59° to 86°F) [see USP Controlled Room Temperature]. Protect from moisture. Dispense in tight container (USP).
All brands mentioned are trademarks of their respective owners and are not trademarks of Alembic Pharmaceuticals Limited.
Manufactured by: Alembic Pharmaceuticals Limited (Formulation Division), Village Panelav, P. O. Tajpura, Near Baska, Taluka-Halol, Panchmahal, Gujarat, India.
Revised: 05/2024