Get your patient on Cyclobenzaprine Hydrochloride - Cyclobenzaprine Hydrochloride tablet, Film Coated (Cyclobenzaprine Hydrochloride)
Cyclobenzaprine Hydrochloride - Cyclobenzaprine Hydrochloride tablet, Film Coated prescribing information
INDICATIONS AND USAGE
Cyclobenzaprine hydrochloride tablets, USP are indicated as an adjunct to rest and physical therapy for relief of muscle spasm associated with acute, painful musculoskeletal conditions.
Improvement is manifested by relief of muscle spasm and its associated signs and symptoms, namely, pain, tenderness, limitation of motion, and restriction in activities of daily living.
Cyclobenzaprine hydrochloride tablets should be used only for short periods (up to 2 or 3 weeks) because adequate evidence of effectiveness for more prolonged use is not available and because muscle spasm associated with acute, painful musculoskeletal conditions is generally of short duration and specific therapy for longer periods is seldom warranted.
Cyclobenzaprine hydrochloride tablets have not been found effective in the treatment of spasticity associated with cerebral or spinal cord disease, or in children with cerebral palsy.
DOSAGE AND ADMINISTRATION
For most patients, the recommended dose of cyclobenzaprine hydrochloride tablets is 5 mg three times a day. Based on individual patient response, the dose may be increased to 10 mg three times a day. Use of cyclobenzaprine hydrochloride tablets for periods longer than 2 or 3 weeks is not recommended (see INDICATIONS AND USAGE) .
Less frequent dosing should be considered for hepatically impaired or elderly patients (see PRECAUTIONS: Impaired Hepatic Function , and Use in the Elderly).
CONTRAINDICATIONS
Hypersensitivity to any component of this product.
Concomitant use of monoamine oxidase (MAO) inhibitors or within 14 days after their discontinuation. Hyperpyretic crisis seizures and deaths have occurred in patients receiving cyclobenzaprine (or structurally similar tricyclic antidepressants) concomitantly with MAO inhibitor drugs.
Acute recovery phase of myocardial infarction, and patients with arrhythmias, heart block or conduction disturbances, or congestive heart failure.
Hyperthyroidism.
ADVERSE REACTIONS
Incidence of most common adverse reactions in the two double-blind•, placebo-controlled 5 mg studies (incidence of > 3% on cyclobenzaprine hydrochloride 5 mg):
| Cyclobenzaprine Hydrochloride 5 mg | Cyclobenzaprine Hydrochloride 10 mg | Placebo | |
| N = 464 | N = 249 | N = 469 | |
| Drowsiness | 29% | 38% | 10% |
| Dry Mouth | 21% | 32% | 7% |
| Fatigue | 6% | 6% | 3% |
| Headache | 5% | 5% | 8% |
•Note: Cyclobenzaprine hydrochloride 10 mg data are from one clinical trial. Cyclobenzaprine hydrochloride 5 mg and placebo data are from two studies.
Adverse reactions which were reported in 1% to 3% of the patients were: abdominal pain, acid regurgitation, constipation, diarrhea, dizziness, nausea, irritability, mental acuity decreased, nervousness, upper respiratory infection, and pharyngitis.
The following list of adverse reactions is based on the experience in 473 patients treated with cyclobenzaprine hydrochloride 10 mg in additional controlled clinical studies, 7,607 patients in the postmarketing surveillance program, and reports received since the drug was marketed. The overall incidence of adverse reactions among patients in the surveillance program was less than the incidence in the controlled clinical studies.
The adverse reactions reported most frequently with cyclobenzaprine were drowsiness, dry mouth and dizziness. The incidence of these common adverse reactions was lower in the surveillance program than in the controlled clinical studies:
| Clinical Studies with Cyclobenzaprine hydrochloride 10 mg | Surveillance Program with Cyclobenzaprine hydrochloride 10 mg | |
| Drowsiness | 39% | 16% |
| Dry Mouth | 27% | 7% |
| Dizziness | 11% | 3% |
Among the less frequent adverse reactions, there was no appreciable difference in incidence in controlled clinical studies or in the surveillance program. Adverse reactions which were reported in 1% to 3% of the patients were: fatigue/tiredness, asthenia, nausea, constipation, dyspepsia, unpleasant taste, blurred vision, headache, nervousness, and confusion.
The following adverse reactions have been reported in postmarketing experience or with an incidence of less than 1% of patients in clinical trials with the 10 mg tablet:
Body as a Whole: Syncope; malaise.
Cardiovascular: Tachycardia; arrhythmia; vasodilatation; palpitation; hypotension.
Digestive: Vomiting; anorexia; diarrhea; gastrointestinal pain; gastritis; thirst; flatulence; edema of the tongue; abnormal liver function and rare reports of hepatitis, jaundice and cholestasis.
Hypersensitivity: Anaphylaxis; angioedema; pruritus; facial edema; urticaria; rash.
Musculoskeletal: Local weakness.
Nervous System and Psychiatric: Seizures; ataxia; vertigo; dysarthria; tremors; hypertonia; convulsions; muscle twitching; disorientation; insomnia; depressed mood; abnormal sensations; anxiety; agitation; psychosis; abnormal thinking and dreaming; hallucinations; excitement; paresthesia; diplopia, serotonin syndrome.
Skin: Sweating.
Special Senses: Ageusia; tinnitus.
Urogenital: Urinary frequency and/or retention.
Causal Relationship Unknown
Other reactions, reported rarely for cyclobenzaprine under circumstances where a causal relationship could not be established or reported for other tricyclic drugs, are listed to serve as alerting information to physicians:
Body as a Whole: Chest pain; edema.
Cardiovascular: Hypertension; myocardial infarction; heart block; stroke.
Digestive: Paralytic ileus; tongue discoloration; stomatitis; parotid swelling.
Endocrine: Inappropriate ADH syndrome.
Hematic and Lymphatic: Purpura; bone marrow depression; leukopenia; eosinophilia; thrombocytopenia.
Metabolic, Nutritional and Immune: Elevation and lowering of blood sugar levels; weight gain or loss.
Musculoskeletal: Myalgia.
Nervous System and Psychiatric: Decreased or increased libido; abnormal gait; delusions; aggressive behavior; paranoia; peripheral neuropathy; Bell's palsy; alteration in EEG patterns; extrapyramidal symptoms.
Respiratory: Dyspnea.
Skin: Photosensitization; alopecia.
Urogenital: Impaired urination; dilatation of urinary tract; impotence; testicular swelling; gynecomastia; breast enlargement; galactorrhea.
DESCRIPTION
Cyclobenzaprine hydrochloride, USP is a tricyclic amine salt which is white to off white, odourless, crystalline powder with the molecular formula C 20 H 21 N • HCl and a molecular weight of 311.9. It has a melting point of 217°C, and a pKa of 8.47 at 25°C. It is freely soluble in water, in alcohol and in methanol, sparingly soluble in isopropanol, slightly soluble in chloroform and in methylene chloride, insoluble in n-hexane. If aqueous solutions are made alkaline, the free base separates. Cyclobenzaprine hydrochloride is designated chemically as 3-(5H -dibenzo[a,d] cyclohepten-5-ylidene)- N,N -dimethyl-1-propanamine hydrochloride, and has the following structural formula:
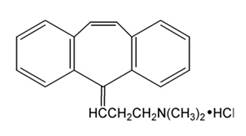
Cyclobenzaprine hydrochloride tablets, USP are available as 5 mg, 7.5 mg and 10 mg tablets for oral administration. Each 5 mg, 7.5 mg and 10 mg tablet contains cyclobenzaprine hydrochloride and the following inactive ingredients: crospovidone, hypromellose, lactose anhydrous, macrogol, magnesium stearate, polysorbate 80, pregelatinized starch, silicified microcrystalline cellulose, titanium dioxide. The tablets of 5 mg and 10 mg also contain D&C Yellow #10 Aluminum Lake and FD&C Yellow #6 Sunset Yellow FCF Aluminum Lake. In addition, the 5 mg tablets contain FD&C Blue #2/INDIGO Carmine Aluminum Lake.
CLINICAL PHARMACOLOGY
Cyclobenzaprine hydrochloride relieves skeletal muscle spasm of local origin without interfering with muscle function. It is ineffective in muscle spasm due to central nervous system disease.
Cyclobenzaprine reduced or abolished skeletal muscle hyperactivity in several animal models. Animal studies indicate that cyclobenzaprine does not act at the neuromuscular junction or directly on skeletal muscle. Such studies show that cyclobenzaprine acts primarily within the central nervous system at brain stem as opposed to spinal cord levels, although its action on the latter may contribute to its overall skeletal muscle relaxant activity. Evidence suggests that the net effect of cyclobenzaprine is a reduction of tonic somatic motor activity, influencing both gamma (γ) and alpha (α) motor systems.
Pharmacological studies in animals showed a similarity between the effects of cyclobenzaprine and the structurally related tricyclic antidepressants, including reserpine antagonism, norepinephrine potentiation, potent peripheral and central anticholinergic effects, and sedation. Cyclobenzaprine caused slight to moderate increase in heart rate in animals.
Pharmacokinetics
Estimates of mean oral bioavailability of cyclobenzaprine range from 33% to 55%. Cyclobenzaprine exhibits linear pharmacokinetics over the dose range 2.5 mg to 10 mg, and is subject to enterohepatic circulation. It is highly bound to plasma proteins. Drug accumulates when dosed 3 times a day, reaching steady-state within 3 to 4 days at plasma concentrations about 4-fold higher than after a single dose. At steady-state in healthy subjects receiving 10 mg t.i.d. (n = 18), peak plasma concentration was 25.9 ng/mL (range, 12.8 to 46.1 ng/mL), and area under the concentration-time (AUC) curve over an 8-hour dosing interval was 177 ng·hr/mL (range, 80 to 319 ng·hr/mL).
Cyclobenzaprine is extensively metabolized, and is excreted primarily as glucuronides via the kidney. Cytochromes P450 3A4, 1A2, and, to a lesser extent, 2D6, mediate N-demethylation, one of the oxidative pathways for cyclobenzaprine. Cyclobenzaprine is eliminated quite slowly, with an effective half-life of 18 hours (range 8 to 37 hours; n = 18); plasma clearance is 0.7 L/min.
The plasma concentration of cyclobenzaprine is generally higher in the elderly and in patients with hepatic impairment (see PRECAUTIONS: Use in the Elderly and PRECAUTIONS: Impaired Hepatic Function ).
Elderly
In a pharmacokinetic study in elderly individuals (≥ 65 yrs old), mean (n = 10) steady-state cyclobenzaprine AUC values were approximately 1.7-fold (171 ng·hr/mL, range 96.1 to 255.3) higher than those seen in a group of 18 younger adults (101.4 ng·hr/mL, range 36.1 to 182.9) from another study. Elderly male subjects had the highest observed mean increase, approximately 2.4-fold (198.3 ng·hr/mL, range 155.6 to 255.3 vs. 83.2 ng·hr/mL, range 41.1 to 142.5 for younger males) while levels in elderly females were increased to a much lesser extent, approximately 1.2-fold (143.8 ng·hr/mL, range 96.1 to 196.3 vs. 115.9 ng·hr/mL, range 36.1 to 182.9 for younger females).
In light of these findings, therapy with cyclobenzaprine in the elderly should be initiated with a 5 mg dose and titrated slowly upward.
Hepatic Impairment
In a pharmacokinetic study of 16 subjects with hepatic impairment (15 mild, 1 moderate per Child-Pugh score), both AUC and C max were approximately double the values seen in the healthy control group. Based on the findings, cyclobenzaprine should be used with caution in subjects with mild hepatic impairment starting with the 5 mg dose and titrating slowly upward. Due to the lack of data in subjects with more severe hepatic insufficiency, the use of cyclobenzaprine in subjects with moderate to severe impairment is not recommended.
No significant effect on plasma levels or bioavailability of cyclobenzaprine or aspirin was noted when single or multiple doses of the two drugs were administered concomitantly. Concomitant administration of cyclobenzaprine and naproxen or diflunisal was well tolerated with no reported unexpected adverse effects. However combination therapy of cyclobenzaprine with naproxen was associated with more side effects than therapy with naproxen alone, primarily in the form of drowsiness. No well controlled studies have been performed to indicate that cyclobenzaprine enhances the clinical effect of aspirin or other analgesics, or whether analgesics enhance the clinical effect of cyclobenzaprine in acute musculoskeletal conditions.
Clinical Studies
Eight double-blind controlled clinical studies were performed in 642 patients comparing cyclobenzaprine hydrochloride 10 mg, diazepam, and placebo. Muscle spasm, local pain and tenderness, limitation of motion, and restriction in activities of daily living were evaluated. In three of these studies there was a significantly greater improvement with cyclobenzaprine than with diazepam, while in the other studies the improvement following both treatments was comparable.
Although the frequency and severity of adverse reactions observed in patients treated with cyclobenzaprine were comparable to those observed in patients treated with diazepam, dry mouth was observed more frequently in patients treated with cyclobenzaprine and dizziness more frequently in those treated with diazepam. The incidence of drowsiness, the most frequent adverse reaction, was similar with both drugs.
The efficacy of cyclobenzaprine hydrochloride 5 mg was demonstrated in two 7-day, double-blind, controlled clinical trials enrolling 1,405 patients. One study compared cyclobenzaprine hydrochloride 5 mg and 10 mg t.i.d. to placebo; and a second study compared cyclobenzaprine hydrochloride 5 mg and 2.5 mg t.i.d. to placebo. Primary endpoints for both trials were determined by patient-generated data and included global impression of change, medication helpfulness, and relief from starting backache. Each endpoint consisted of a score on a 5-point rating scale (from 0 or worst outcome to 4 or best outcome). Secondary endpoints included a physician's evaluation of the presence and extent of palpable muscle spasm.
Comparisons of cyclobenzaprine hydrochloride 5 mg and placebo groups in both trials established the statistically significant superiority of the 5 mg dose for all three primary endpoints at day 8 and, in the study comparing 5 mg and 10 mg, at day 3 or 4 as well. A similar effect was observed with cyclobenzaprine hydrochloride 10 mg (all endpoints). Physician-assessed secondary endpoints also showed that cyclobenzaprine hydrochloride 5 mg was associated with a greater reduction in palpable muscle spasm than placebo.
Analysis of the data from controlled studies shows that cyclobenzaprine produces clinical improvement whether or not sedation occurs.
Surveillance Program
A post-marketing surveillance program was carried out in 7,607 patients with acute musculoskeletal disorders, and included 297 patients treated with cyclobenzaprine hydrochloride 10 mg for 30 days or longer. The overall effectiveness of cyclobenzaprine was similar to that observed in the double-blind controlled studies; the overall incidence of adverse effects was less (see ADVERSE REACTIONS ).
HOW SUPPLIED
Cyclobenzaprine Hydrochloride Tablets, USP are available containing 5 mg, 7.5 mg or 10 mg of cyclobenzaprine hydrochloride, USP.
The 5 mg tablets are butter scotch yellow film-coated, round tablets debossed with 020 on one side and plain on other side. They are available as follows:
NDC 52817-330-10
bottles of 100 tablets
NDC 52817-330-50
bottles of 500 tablets
The 7.5 mg tablets are white to off-white film-coated, round tablets debossed with 021 on one side and plain on other side. They are available as follows:
NDC 52817-331-10
bottles of 100 tablets
The 10 mg tablets are orange-yellow film-coated, round tablets debossed with 022 on one side and plain on other side. They are available as follows:
NDC 52817-332-10
bottles of 100 tablets
NDC 52817-332-00
bottles of 1000 tablets
NDC 52817-332-50
bottles of 500 tablets
Store at 20°C to 25°C (68°F to 77°F). [See USP Controlled Room Temperature.]
Dispense in a tight, light-resistant container as defined in the USP using a child-resistant closure.
Distributed By:
TruPharma, LLC
Tampa,FL 33609
Manufactured by:
Rubicon Research Private Limited,
Ambernath,Dist. Thane,421506 India
Rev. 02, June 2018