Get your patient on Desogestrel And Ethinyl Estradiol - Desogestrel And Ethinyl Estradiol (Desogestrel And Ethinyl Estradiol)
Desogestrel And Ethinyl Estradiol - Desogestrel And Ethinyl Estradiol prescribing information
WARNING: CARDIOVASCULAR RISK ASSOCIATED WITH SMOKING
Cigarette smoking increases the risk of serious cardiovascular events from combination oral contraceptive use. This risk increases with age, particularly in women over 35 years of age, and with the number of cigarettes smoked. For this reason, combination oral contraceptives, including desogestrel and ethinyl estradiol tablets 0.15 mg/0.03 mg, should not be used by women who are over 35 years of age and smoke.
INDICATIONS AND USAGE
Desogestrel and ethinyl estradiol tablets USP 0.15 mg/0.03 mg are indicated for the prevention of pregnancy in women who elect to use oral contraceptives as a method of contraception.
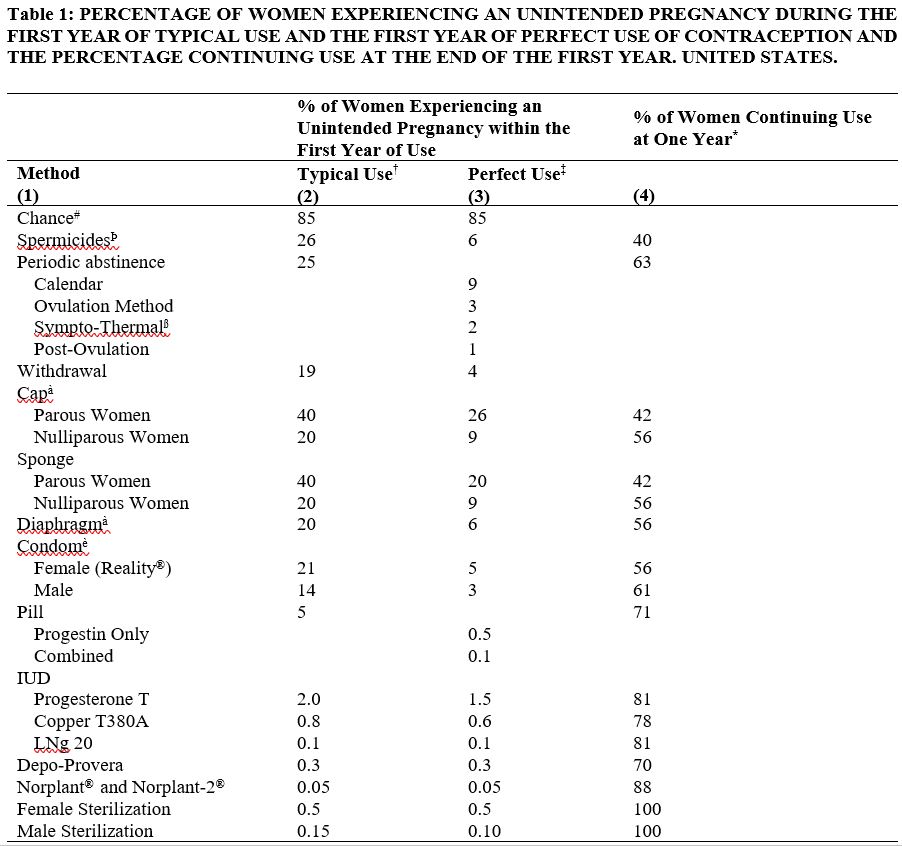
Oral contraceptives are highly effective. Table 1 lists the typical accidental pregnancy rates for users of combined oral contraceptives and other methods of contraception. The efficacy of these contraceptive methods, except sterilization, the IUD, and the Norplant System depends upon the reliability with which they are used. Correct and consistent use of these methods can result in lower failure rates.
In a clinical trial with desogestrel and ethinyl estradiol tablets, 1,195 subjects completed 11,656 cycles and a total of 10 pregnancies were reported. This represents an overall user-efficacy (typical user-efficacy) pregnancy rate of 1.12 per 100 women-years. This rate includes patients who did not take the drug correctly.

Desogestrel and ethinyl estradiol tablets 0.15 mg/0.03 mg has not been studied for and is not indicated for use in emergency contraception.
DOSAGE AND ADMINISTRATION
To achieve maximum contraceptive effectiveness, desogestrel and ethinyl estradiol tablets must be taken exactly as directed and at intervals not exceeding 24 hours. Desogestrel and ethinyl estradiol tablets are available in a blister pack.
Day 1 Start
The dosage of desogestrel and ethinyl estradiol tablets for the initial cycle of therapy is one light orange "active" tablet administered daily from the 1st day through the 21st day of the menstrual cycle, counting the first day of menstrual flow as "Day 1". Tablets are taken without interruption as follows: One light orange "active" tablet daily for 21 days, then one green "reminder" tablet daily for 7 days. After 28 tablets have been taken, a new course is started and a light orange "active" tablet is taken the next day.
The use of desogestrel and ethinyl estradiol tablets for contraception may be initiated 4 weeks postpartum in women who elect not to breastfeed. When the tablets are administered during the postpartum period, the increased risk of thromboembolic disease associated with the postpartum period must be considered. (See CONTRAINDICATIONS and WARNINGS concerning thromboembolic disease. See also PRECAUTIONS: Nursing Mothers .) If the patient starts on desogestrel and ethinyl estradiol tablets postpartum, and has not yet had a period, she should be instructed to use another method of contraception until a light orange "active" tablet has been taken daily for 7 days. The possibility of ovulation and conception prior to initiation of medication should be considered. If the patient misses one (1) light orange "active" tablet in Weeks 1, 2, or 3, the light orange "active" tablet should be taken as soon as she remembers. If the patient misses two (2) light orange "active" tablets in Week 1 or Week 2, the patient should take two (2) light orange "active" tablets the day she remembers and two (2) light orange "active" tablets the next day; and then continue taking one (1) light orange "active" tablet a day until she finishes the pack. The patient should be instructed to use a back-up method of birth control such as a condom or spermicide if she has sex in the seven (7) days after missing pills. If the patient misses two (2) light orange "active" tablets in the third week or misses three (3) or more light orange "active" tablets in a row, the patient should throw out the rest of the pack and start a new pack that same day. The patient should be instructed to use a back-up method of birth control if she has sex in the seven (7) days after missing pills.
Sunday Start
When taking desogestrel and ethinyl estradiol tablets, the first light orange "active" tablet should be taken on the first Sunday after menstruation begins. If the period begins on Sunday, the first light orange "active" tablet is taken on that day. If switching directly from another oral contraceptive, the first light orange "active" tablet should be taken on the first Sunday after the last ACTIVE tablet of the previous product. Tablets are taken without interruption as follows: One light orange "active" tablet daily for 21 days, then one green "reminder" tablet daily for 7 days. After 28 tablets have been taken, a new course is started and a light orange "active" tablet is taken the next day (Sunday). When initiating a Sunday start regimen, another method of contraception should be used until after the first 7 consecutive days of administration.
The use of desogestrel and ethinyl estradiol tablets for contraception may be initiated 4 weeks postpartum. When the tablets are administered during the postpartum period, the increased risk of thromboembolic disease associated with the postpartum period must be considered. (See CONTRAINDICATIONS and WARNINGS concerning thromboembolic disease. See also PRECAUTIONS: Nursing Mothers .) If the patient starts on desogestrel and ethinyl estradiol tablets postpartum, and has not yet had a period, she should be instructed to use another method of contraception until a light orange "active" tablet has been taken daily for 7 days. The possibility of ovulation and conception prior to initiation of medication should be considered. If the patient misses one (1) light orange active tablet in Weeks 1, 2, or 3, the light orange "active" tablet should be taken as soon as she remembers. If the patient misses two (2) light orange "active" tablets in Week 1 or Week 2, the patient should take two (2) light orange "active" tablets the day she remembers and two (2) light orange "active" tablets the next day; and then continue taking one (1) light orange "active" tablet a day until she finishes the pack. The patient should be instructed to use a back-up method of birth control such as a condom or spermicide if she has sex in the seven (7) days after missing pills. If the patient misses two (2) light orange "active" tablets in the third week or misses three (3) or more light orange "active" tablets in a row, the patient should continue taking one light orange "active" tablet every day until Sunday. On Sunday the patient should throw out the rest of the pack and start a new pack that same day. The patient should be instructed to use a back-up method of birth control if she has sex in the seven (7) days after missing pills.
ADDITIONAL INSTRUCTIONS FOR ALL DOSING REGIMENS
Breakthrough bleeding, spotting, and amenorrhea are frequent reasons for patients discontinuing oral contraceptives. In breakthrough bleeding, as in all cases of irregular bleeding from the vagina, nonfunctional causes should be borne in mind. In undiagnosed persistent or recurrent abnormal bleeding from the vagina, adequate diagnostic measures are indicated to rule out pregnancy or malignancy. If pathology has been excluded, time or a change to another formulation may solve the problem. Changing to an oral contraceptive with a higher estrogen content, while potentially useful in minimizing menstrual irregularity, should be done only if necessary since this may increase the risk of thromboembolic disease.
Use of oral contraceptives in the event of a missed menstrual period:
- If the patient has not adhered to the prescribed schedule, the possibility of pregnancy should be considered at the time of the first missed period and oral contraceptive use should be discontinued if pregnancy is confirmed.
- If the patient has adhered to the prescribed regimen and misses two consecutive periods, pregnancy should be ruled out.
CONTRAINDICATIONS
Desogestrel and ethinyl estradiol tablets are contraindicated in females who are known to have or develop the following conditions:
- Thrombophlebitis or thromboembolic disorders
- A past history of deep vein thrombophlebitis or thromboembolic disorders
- Known thrombophilic conditions
- Cerebral vascular or coronary artery disease (current or history)
- Valvular heart disease with complications
- Persistent blood pressure values of ≥ 160 mm Hg systolic or ≥ 100 mg Hg diastolic 102
- Diabetes with vascular involvement
- Headaches with focal neurological symptoms
- Major surgery with prolonged immobilization
- Current diagnosis of, or history of, breast cancer, which may be hormone-sensitive
- Carcinoma of the endometrium or other known or suspected estrogen-dependent neoplasia
- Undiagnosed abnormal genital bleeding
- Cholestatic jaundice of pregnancy or jaundice with prior pill use
- Acute or chronic hepatocellular disease with abnormal liver function
- Hepatic adenomas or carcinomas
- Known or suspected pregnancy
- Hypersensitivity to any component of this product
- Are receiving Hepatitis C drug combinations containing ombitasivir/paritaprevir/ritonavir, with or without dasabuvir, due to the potential for ALT elevations (see section 5 in WARNINGS ), Risk of Liver Enzyme Elevations with Concomitant Hepatitis C Treatment).
ADVERSE REACTIONS
Post Marketing Experience Five studies that compared breast cancer risk between ever-users (current or past use) of COCs and never-users of COCs reported no association between ever use of COCs and breast cancer risk, with effect estimates ranging from 0.90 - 1.12 (Figure 2).
Three studies compared breast cancer risk between current or recent COC users (<6 months since last use) and never users of COCs (Figure 2). One of these studies reported no association between breast cancer risk and COC use. The other two studies found an increased relative risk of 1.19 - 1.33 with current or recent use. Both of these studies found an increased risk of breast cancer with current use of longer duration, with relative risks ranging from 1.03 with less than one year of COC use to approximately 1.4 with more than 8-10 years of COC use.
Figure 2. Risk of Breast Cancer with Combined Oral Contraceptive Use
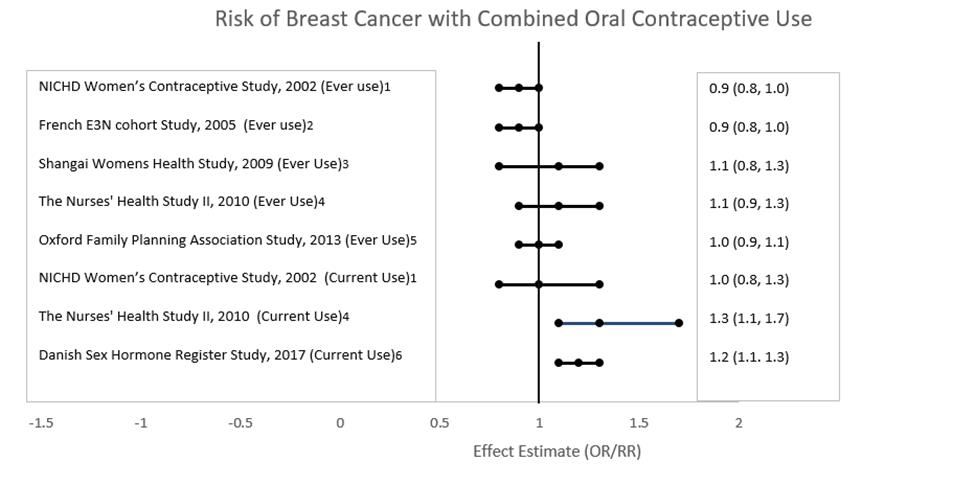
RR = relative risk; OR = odds ratio; HR = hazard ratio. “ever COC” are females with current or past COC use; “never COC use” are females that never used COCs
An increased risk of the following serious adverse reactions has been associated with the use of oral contraceptives (see WARNINGS ).
- Thrombophlebitis and venous thrombosis with or without embolism
- Arterial thromboembolism
- Pulmonary embolism
- Myocardial infarction
- Cerebral hemorrhage
- Cerebral thrombosis
- Hypertension
- Gallbladder disease
- Hepatic adenomas or benign liver tumors
There is evidence of an association between the following conditions and the use of oral contraceptives:
- Mesenteric thrombosis
- Retinal thrombosis
The following adverse reactions have been reported in patients receiving oral contraceptives and are believed to be drug-related:
- Nausea
- Vomiting
- Gastrointestinal symptoms (such as abdominal cramps and bloating)
- Breakthrough bleeding
- Spotting
- Change in menstrual flow
- Amenorrhea
- Temporary infertility after discontinuation of treatment
- Edema
- Melasma which may persist
- Breast changes: tenderness, enlargement, secretion
- Change in weight (increase or decrease)
- Change in cervical erosion and secretion
- Diminution in lactation when given immediately postpartum
- Cholestatic jaundice
- Migraine
- Allergic reaction, including rash, urticaria, and angioedema
- Mental depression
- Reduced tolerance to carbohydrates
- Vaginal candidiasis
- Change in corneal curvature (steepening)
- Intolerance to contact lenses
The following adverse reactions have been reported in users of oral contraceptives and a causal association has been neither confirmed nor refuted:
- Pre-menstrual syndrome
- Cataracts
- Changes in appetite
- Cystitis-like syndrome
- Headache
- Nervousness
- Dizziness
- Hirsutism
- Loss of scalp hair
- Erythema multiforme
- Erythema nodosum
- Hemorrhagic eruption
- Vaginitis
- Porphyria
- Impaired renal function
- Hemolytic uremic syndrome
- Acne
- Changes in libido
- Colitis
- Budd-Chiari Syndrome
Drug Interactions
Consult the labeling of concurrently-used drugs to obtain further information about interactions with hormonal contraceptives or the potential for enzyme alterations.
Effects of Other Drugs on Combined Hormonal Contraceptives
Substances decreasing the plasma concentrations of COCs and potentially diminishing the efficacy of COCs:
Drugs or herbal products that induce certain enzymes, including cytochrome P450 3A4 (CYP3A4), may decrease the plasma concentrations of COCs and potentially diminish the effectiveness of CHCs or increase breakthrough bleeding. Some drugs or herbal products that may decrease the effectiveness of hormonal contraceptives include phenytoin, barbiturates, carbamazepine, bosentan, felbamate, griseofulvin, oxcarbazepine, rifampicin, topiramate, rifabutin, rufinamide, aprepitant, and products containing St. John's wort. Interactions between hormonal contraceptives and other drugs may lead to breakthrough bleeding and/or contraceptive failure. Counsel women to use an alternative method of contraception or a back-up method when enzyme inducers are used with CHCs, and to continue back-up contraception for 28 days after discontinuing the enzyme inducer to ensure contraceptive reliability.
Substances increasing the plasma concentrations of COCs:
Co-administration of atorvastatin or rosuvastatin and certain COCs containing EE increase AUC values for EE by approximately 20 to 25%. Ascorbic acid and acetaminophen may increase plasma EE concentrations, possibly by inhibition of conjugation. CYP3A4 inhibitors such as itraconazole, voriconazole, fluconazole, grapefruit juice, or ketoconazole may increase plasma hormone concentrations.
Human immunodeficiency virus (HIV)/ Hepatitis C virus (HCV) protease inhibitors and non-nucleoside reverse transcriptase inhibitors:
Significant changes (increase or decrease) in the plasma concentrations of estrogen and/or progestin have been noted in some cases of co-administration with HIV protease inhibitors (decrease [e.g., nelfinavir, ritonavir, darunavir/ritonavir, (fos)amprenavir/ritonavir, lopinavir/ritonavir, and tipranavir/ritonavir] or increase [e.g., indinavir and atazanavir/ritonavir]) /HCV protease inhibitors (decrease [e.g., boceprevir and telaprevir]) or with non-nucleoside reverse transcriptase inhibitors (decrease [e.g., nevirapine] or increase [e.g., etravirine]).
Concomitant Use with HCV Combination Therapy – Liver Enzyme Elevation:
Do not co-administer desogestrel and ethinyl estradiol tablets with HCV drug combinations containing ombitasvir/ paritaprevir/ritonavir, with or without dasabuvir, due to potential for ALT elevations (see section 5 in WARNINGS ), Risk of Liver Enzyme Elevations with Concomitant Hepatitis C Treatment).
Colesevelam: Colesevelam, a bile acid sequestrant, given together with a combination oral hormonal contraceptive, has been shown to significantly decrease the AUC of EE. A drug interaction between the contraceptive and colesevelam was decreased when the two drug products were given 4 hours apart.
Effects of Combined Hormonal Contraceptives on Other Drugs
COCs containing EE may inhibit the metabolism of other compounds (e.g., cyclosporine, prednisolone, theophylline, tizanidine, and voriconazole) and increase their plasma concentrations. COCs have been shown to decrease plasma concentrations of acetaminophen, clofibric acid, morphine, salicylic acid, temazepam and lamotrigine. Significant decrease in plasma concentration of lamotrigine has been shown, likely due to induction of lamotrigine glucuronidation. This may reduce seizure control; therefore, dosage adjustments of lamotrigine may be necessary.
Women on thyroid hormone replacement therapy may need increased doses of thyroid hormone because serum concentrations of thyroid-binding globulin increases with use of COCs.
DESCRIPTION
Desogestrel and ethinyl estradiol tablets USP 0.15 mg/0.03 mg provide an oral contraceptive regimen of 21 light orange round tablets each containing 0.15 mg desogestrel (13-ethyl-11-methylene-18,19-dinor-17 alpha-pregn-4-en-20-yn-17-ol) and 0.03 mg ethinyl estradiol (19-nor-17 alpha-pregna-1,3,5 (10)-trien-20-yne-3,17,diol). Inactive ingredients include colloidal anhydrous silica, corn starch, ferric oxide red, ferric oxide yellow, hypromellose, lactose monohydrate, magnesium stearate, polyethylene glycol, povidone, stearic acid, talc, titanium dioxide, and vitamin E. Each green tablet contains the following inactive ingredients: colloidal anhydrous silica, FD&C Blue No.2 Aluminum Lake, ferric oxide yellow, hypromellose, lactose monohydrate, magnesium stearate, polyethylene glycol, pregelatinized starch (maize), talc and titanium dioxide.
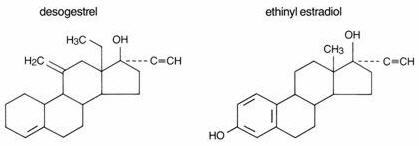
Desogestrel and Ethinyl Estradiol Tablets USP 0.15 mg/0.03 mg meet USP Dissolution Test 2.
CLINICAL PHARMACOLOGY
Pharmacodynamics
Combined oral contraceptives act by suppression of gonadotropins. Although the primary mechanism of this action is inhibition of ovulation, other alterations include changes in the cervical mucus, which increase the difficulty of sperm entry into the uterus, and changes in the endometrium which reduce the likelihood of implantation.
Receptor binding studies, as well as studies in animals, have shown that 3-keto-desogestrel, the biologically active metabolite of desogestrel, combines high progestational activity with 91,92 minimal intrinsic androgenicity. The relevance of this latter finding in humans is unknown.
Pharmacokinetics
Desogestrel is rapidly and almost completely absorbed and converted into 3-keto-desogestrel, its biologically active metabolite. Following oral administration, the relative bioavailability of desogestrel, as measured by serum levels of 3-keto-desogestrel, is approximately 84%.
In the third cycle of use after a single dose of desogestrel and ethinyl estradiol tablets 0.15 mg/0.03 mg, maximum concentrations of 3-keto-desogestrel of 2,805 ± 1,203 pg/mL (mean ± SD) are reached at 1.4 ± 0.8 hours. The area under the curve (AUC 0–∞ ) is 33,858 ± 11,043 pg/mL∙hr after a single dose. At steady state, attained from at least day 19 onwards, maximum concentrations of 5,840 ± 1,667 pg/mL are reached at 1.4 ± 0.9 hours. The minimum plasma levels of 3-keto-desogestrel at steady state are 1,400 ± 560 pg/mL. The AUC 0–24 at steady state is 52,299 ± 17,878 pg/mL∙hr. The mean AUC 0–∞ for 3-keto-desogestrel at single dose is significantly lower than the mean AUC 0–24 at steady state. This indicates that the kinetics of 3-keto-desogestrel are non-linear due to an increase in binding of 3-keto-desogestrel to sex hormone-binding globulin in the cycle, attributed to increased sex hormone-binding globulin levels which are induced by the daily administration of ethinyl estradiol. Sex hormone-binding globulin levels increased significantly in the third treatment cycle from day 1 (150 ± 64 nmol/L) to day 21 (230 ± 59 nmol/L).
The elimination half-life for 3-keto-desogestrel is approximately 38 ± 20 hours at steady state. In addition to 3-keto-desogestrel, other phase I metabolites are 3α-OH-desogestrel, 3β-OH-desogestrel, and 3α-OH-5α-H-desogestrel. These other metabolites are not known to have any pharmacologic effects, and are further converted in part by conjugation (phase II metabolism) into polar metabolites, mainly sulfates and glucuronides.
Ethinyl estradiol is rapidly and almost completely absorbed. In the third cycle of use after a single dose of desogestrel and ethinyl estradiol tablets, the relative bioavailability is approximately 83%.
In the third cycle of use after a single dose of desogestrel and ethinyl estradiol tablets, maximum concentrations of ethinyl estradiol of 95 ± 34 pg/mL are reached at 1.5 ± 0.8 hours. The AUC 0–∞ is 1,471 ± 268 pg/mL∙hr after a single dose. At steady state, attained from at least day 19 onwards, maximum ethinyl estradiol concentrations of 141 ± 48 pg/mL are reached at about 1.4 ± 0.7 hours. The minimum serum levels of ethinyl estradiol at steady state are 24 ± 8.3 pg/mL. The AUC 0–24 at steady state is 1,117 ± 302 pg/mL∙hr. The mean AUC 0–∞ for ethinyl estradiol following a single dose during treatment cycle 3 does not significantly differ from the mean AUC 0–24 at steady state. This finding indicates linear kinetics for ethinyl estradiol.
The elimination half-life is 26 ± 6.8 hours at steady state. Ethinyl estradiol is subject to a significant degree of presystemic conjugation (phase II metabolism). Ethinyl estradiol escaping gut wall conjugation undergoes phase I metabolism and hepatic conjugation (phase II metabolism). Major phase I metabolites are 2-OH-ethinyl estradiol and 2-methoxy-ethinyl estradiol. Sulfate and glucuronide conjugates of both ethinyl estradiol and phase I metabolites, which are excreted in bile, can undergo enterohepatic circulation.
HOW SUPPLIED
Desogestrel and ethinyl estradiol tablets, USP 0.15 mg/0.03 mg are available in a blister pack (NDC 79929-006-05). The blister pack contains 28 tablets, as follows: 21 light orange, round, biconvex, beveled edged, film coated tablets, debossed with “EY” on one side and “1” on other side containing 0.15 mg desogestrel together with 0.03 mg ethinyl estradiol, and 7 green, round, biconvex, beveled edged, film coated tablets, debossed with “EY” on one side and “2” on other side containing inert ingredients. Desogestrel and ethinyl estradiol tablets USP 0.15 mg/0.03 mg are packaged in a carton containing 3 blister pack.
STORAGE
Store at 25°C (77°F); excursions permitted to 15°C to 30°C (59°F to 86°F).
® The brands listed are trademarks of their respective owners.