Get your patient on Dobutamine - Dobutamine injection (Dobutamine)
Dobutamine - Dobutamine injection prescribing information
INDICATIONS AND USAGE
Dobutamine Injection, USP is indicated when parenteral therapy is necessary for inotropic support in the short-term treatment of patients with cardiac decompensation due to depressed contractility resulting either from organic heart disease or from cardiac surgical procedures. Experience with intravenous dobutamine in controlled trials does not extend beyond 48 hours of repeated boluses and/or continuous infusions.
Whether given orally, continuously intravenously, or intermittently intravenously, neither dobutamine nor any other cyclic-AMP-dependent inotrope has been shown in controlled trials to be safe or effective in the long-term treatment of congestive heart failure. In controlled trials of chronic oral therapy with various such agents, symptoms were not consistently alleviated, and the cyclic-AMP-dependent inotropes were consistently associated with increased risk of hospitalization and death. Patients with NYHA Class IV symptoms appeared to be at particular risk.
DOSAGE AND ADMINISTRATION
Note −Do not add dobutamine injection to 5% Sodium Bicarbonate Injection or to any other strongly alkaline solution. Because of potential physical incompatibilities, it is recommended that dobutamine injection not be mixed with other drugs in the same solution. Dobutamine injection should not be used in conjunction with other agents or diluents containing both sodium bisulfite and ethanol.
Preparation and Stability − At the time of administration, dobutamine injection must be further diluted in an IV container to at least a 50-mL solution using one of the following intravenous solutions as a diluent: 5% Dextrose Injection, 5% Dextrose and 0.45% Sodium Chloride Injection, 5% Dextrose and 0.9% Sodium Chloride Injection, 10% Dextrose Injection, Isolyte® M with 5% Dextrose Injection, Lactated Ringer’s Injection, 5% Dextrose in Lactated Ringer’s Injection, Normosol®-M in D5-W, 20% Osmitrol® in Water for Injection, 0.9% Sodium Chloride Injection, or Sodium Lactate Injection. Intravenous solution should be used within 24 hours.
Recommended Dosage −Infusion of dobutamine should be started at a low rate (0.5-1.0 μg/kg/min) and titrated at intervals of a few minutes, guided by the patient’s response, including systemic blood pressure, urine flow, frequency of ectopic activity, heart rate, and (whenever possible) measurements of cardiac output, central venous pressure, and/or pulmonary capillary wedge pressure. In reported trials, the optimal infusion rates have varied from patient to patient, usually 2-20 μg/kg/min but sometimes slightly outside of this range. On rare occasions, infusion rates up to 40 μg/kg/min have been required to obtain the desired effect. Rates of infusion (mL/h) for dobutamine injection concentrations of 500 μg/mL, 1,000 μg/mL, and 2,000 μg/mL necessary to attain various delivery rates of dobutamine (μg/kg/min) for patients of different weights are given in Table 1.
Table 1 Dobutamine Injection Infusion Rate (mL/h) for 500 μg/mL concentration
Drug Delivery Rate (μg/kg/min) | Patient Body Weight (kg) | |||||||||||
5 | 10 | 20 | 30 | 40 | 50 | 60 | 70 | 80 | 90 | 100 | 110 | |
0.5 | 0.3 | 0.6 | 1.2 | 1.8 | 2.4 | 3 | 3.6 | 4.2 | 4.8 | 5.4 | 6 | 6.5 |
1 | 0.6 | 1.2 | 2.4 | 3.6 | 4.8 | 6 | 7.2 | 8.4 | 9.6 | 10.8 | 12 | 13.2 |
2.5 | 1.5 | 3 | 6 | 9 | 12 | 15 | 18 | 21 | 24 | 27 | 30 | 33 |
5 | 3 | 6 | 12 | 18 | 24 | 30 | 36 | 42 | 48 | 54 | 60 | 66 |
7.5 | 4.5 | 9 | 18 | 27 | 36 | 45 | 54 | 63 | 72 | 81 | 90 | 99 |
10 | 6 | 12 | 24 | 36 | 48 | 60 | 72 | 84 | 96 | 108 | 120 | 132 |
12.5 | 7.5 | 15 | 30 | 45 | 60 | 75 | 90 | 105 | 120 | 135 | 150 | 165 |
15 | 9 | 18 | 36 | 54 | 72 | 90 | 108 | 126 | 144 | 162 | 180 | 198 |
17.5 | 10.5 | 21 | 42 | 63 | 84 | 105 | 126 | 147 | 168 | 189 | 210 | 231 |
20 | 12 | 24 | 48 | 72 | 96 | 120 | 144 | 168 | 192 | 216 | 240 | 264 |
Dobutamine Injection Infusion Rate (mL/h) for 1,000 μg/mL concentration
Drug Delivery Rate (μg/kg/min) | Patient Body Weight (kg) | |||||||||||
5 | 10 | 20 | 30 | 40 | 50 | 60 | 70 | 80 | 90 | 100 | 110 | |
0.5 | 0.1 | 0.3 | 0.6 | 0.9 | 1.2 | 1.5 | 1.8 | 2.1 | 2.4 | 2.7 | 3 | 3.3 |
1 | 0.3 | 0.6 | 1.2 | 1.8 | 2.4 | 3 | 3.6 | 4.2 | 4.8 | 5.4 | 6 | 6.6 |
2.5 | 0.7 | 1.5 | 3 | 4.5 | 6 | 7.5 | 9 | 10.5 | 12 | 13.5 | 15 | 16.5 |
5 | 1.5 | 3 | 6 | 9 | 12 | 15 | 18 | 21 | 24 | 27 | 30 | 33 |
7.5 | 2.2 | 4.5 | 9 | 13.5 | 18 | 22.5 | 27 | 31.5 | 36 | 40.5 | 45 | 49.5 |
10 | 3 | 6 | 12 | 18 | 24 | 30 | 36 | 42 | 48 | 54 | 60 | 66 |
12.5 | 3.7 | 7.5 | 15 | 22.5 | 30 | 37.5 | 45 | 52.5 | 60 | 67.5 | 75 | 82.5 |
15 | 4.5 | 9 | 18 | 27 | 36 | 45 | 54 | 63 | 72 | 81 | 90 | 99 |
17.5 | 5.2 | 10.5 | 21 | 31.5 | 42 | 52.5 | 63 | 73.5 | 84 | 94.5 | 105 | 115.5 |
20 | 6 | 12 | 24 | 36 | 48 | 60 | 72 | 84 | 96 | 108 | 120 | 132 |
Dobutamine Injection Infusion Rate (mL/h) for 2,000 μg/mL concentration
Drug Delivery Rate (μg/kg/min) | Patient Body Weight (kg) | |||||||||||
5 | 10 | 20 | 30 | 40 | 50 | 60 | 70 | 80 | 90 | 100 | 110 | |
0.5 | 0.07 | 0.1 | 0.3 | 0.4 | 0.6 | 0.7 | 0.9 | 1 | 1.2 | 1.3 | 1.5 | 1.6 |
1 | 0.1 | 0.3 | 0.6 | 0.9 | 1.2 | 1.5 | 1.8 | 2.1 | 2.4 | 2.7 | 3 | 3.3 |
2.5 | 0.4 | 0.7 | 1.5 | 2 | 3 | 4 | 4.5 | 5 | 6 | 7 | 7.5 | 8 |
5 | 0.7 | 1.5 | 3 | 4.5 | 6 | 7.5 | 9 | 10.5 | 12 | 13.5 | 15 | 16.5 |
7.5 | 1.1 | 2.2 | 4.5 | 7 | 9 | 11 | 13.5 | 16 | 18 | 20 | 22.5 | 25 |
10 | 1.5 | 3 | 6 | 9 | 12 | 15 | 18 | 21 | 24 | 27 | 30 | 33 |
12.5 | 1.9 | 3.7 | 7 | 11 | 15 | 19 | 22.5 | 26 | 30 | 34 | 37.5 | 41 |
15 | 2.2 | 4.5 | 9 | 13.5 | 18 | 22.5 | 27 | 31.5 | 36 | 40.5 | 45 | 49.5 |
Concentrations of up to 5,000 mcg/mL have been administered to humans (250 mg/50 mL). The final volume administered should be determined by the fluid requirements of the patient.
Intravenous drug products should be inspected visually and should not be used if particulate matter or discoloration is present.
CONTRAINDICATIONS
Dobutamine hydrochloride is contraindicated in patients with idiopathic hypertrophic subaortic stenosis and in patients who have shown previous manifestations of hypersensitivity to Dobutamine Injection solution.
ADVERSE REACTIONS
Increased Heart Rate, Blood Pressure, and Ventricular Ectopic Activity − A 10 to 20 mm increase in systolic blood pressure and an increase in heart rate of 5 to 15 beats/minute have been noted in most patients (see WARNINGS regarding exaggerated chronotropic and pressor effects). Approximately 5% of patients have had increased premature ventricular beats during infusions. These effects are dose related.
Hypotension − Precipitous decreases in blood pressure have occasionally been described in association with dobutamine therapy. Decreasing the dose or discontinuing the infusion typically results in rapid return of blood pressure to baseline values. In rare cases, however, intervention may be required and reversibility may not be immediate.
Reactions at Sites of Intravenous Infusion − Phlebitis has occasionally been reported. Local inflammatory changes have been described following inadvertent infiltration. Isolated cases of cutaneous necrosis (destruction of skin tissue) have been reported.
Miscellaneous Uncommon Effects − The following adverse effects have been reported in 1% to 3% of patients: nausea, headache, anginal pain, nonspecific chest pain, palpitations and shortness of breath. Isolated cases of thrombocytopenia have been reported.
Administration of dobutamine hydrochloride, like other catecholamines, can produce a mild reduction in serum potassium concentration, rarely to hypokalemic levels (see PRECAUTIONS ).
Drug Interactions
Animal studies indicate that dobutamine may be ineffective if the patient has recently received a β-blocking drug. In such a case, the peripheral vascular resistance may increase.
Preliminary studies indicate that the concomitant use of dobutamine and nitroprusside results in a higher cardiac output and, usually, a lower pulmonary wedge pressure than when either drug is used alone.
There was no evidence of drug interactions in clinical studies in which dobutamine was administered concurrently with other drugs, including digitalis preparations, furosemide, spironolactone, lidocaine, nitroglycerin, isosorbide dinitrate, morphine, atropine, heparin, protamine, potassium chloride, folic acid, and acetaminophen.
DESCRIPTION
Dobutamine Injection, USP is a clear, practically colorless, sterile, nonpyrogenic solution of dobutamine hydrochloride for intravenous use only. Each milliliter contains 12.5 mg (41.5 µmol) dobutamine, as the hydrochloride and sodium metabisulfite, 0.2 mg added as antioxidant. May contain hydrochloric acid and/or sodium hydroxide for pH adjustment. pH is 3.3 (2.5 to 5.0).
Dobutamine Hydrochloride, USP is chemically designated (±)-4-[2-[[3-(ρ-hydroxyphenyl)-1- methylpropyl] amino]ethyl]-pyrocatechol hydrochloride.
It is a synthetic catecholamine.
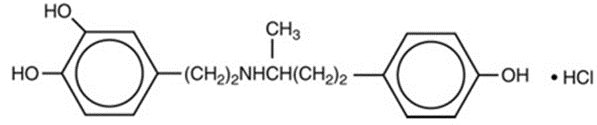
Molecular Weight: 337.85
Molecular Formula: C 18 H 23 NO 3 • HCl
CLINICAL PHARMACOLOGY
Dobutamine is a direct-acting inotropic agent whose primary activity results from stimulation of the β receptors of the heart while producing comparatively mild chronotropic, hypertensive, arrhythmogenic, and vasodilative effects. It does not cause the release of endogenous norepinephrine, as does dopamine. In animal studies, dobutamine produces less increase in heart rate and less decrease in peripheral vascular resistance for a given inotropic effect than does isoproterenol.
In patients with depressed cardiac function, both dobutamine and isoproterenol increase the cardiac output to a similar degree. In the case of dobutamine, this increase is usually not accompanied by marked increases in heart rate (although tachycardia is occasionally observed), and the cardiac stroke volume is usually increased. In contrast, isoproterenol increases the cardiac index primarily by increasing the heart rate while stroke volume changes little or declines.
Facilitation of atrioventricular conduction has been observed in human electrophysiologic studies and in patients with atrial fibrillation.
Systemic vascular resistance is usually decreased with administration of dobutamine. Occasionally, minimum vasoconstriction has been observed.
Most clinical experience with dobutamine is short-term − not more than several hours in duration. In the limited number of patients who were studied for 24, 48, and 72 hours, a persistent increase in cardiac output occurred in some, whereas output returned toward baseline values in others.
The onset of action of dobutamine is within 1 to 2 minutes; however, as much as 10 minutes may be required to obtain the peak effect of a particular infusion rate.
The plasma half-life of dobutamine in humans is 2 minutes. The principal routes of metabolism are methylation of the catechol and conjugation. In human urine, the major excretion products are the conjugates of dobutamine and 3-O-methyl dobutamine. The 3-O-methyl derivative of dobutamine is inactive.
Alteration of synaptic concentrations of catecholamines with either reserpine or tricyclic antidepressants does not alter the actions of dobutamine in animals, which indicates that the actions of dobutamine are not dependent on presynaptic mechanisms.
The effective infusion rate of dobutamine varies widely from patient to patient, and titration is always necessary (see Dosage and Administration ). At least in pediatric patients, dobutamine-induced increases in cardiac output and systemic pressure are generally seen, in any given patients, at lower infusion rates than those that cause substantial tachycardia (see Pediatric Use under Precautions ).
HOW SUPPLIED
Dobutamine Injection, USP is supplied in 20 mL single-dose glass vials containing 250 mg dobutamine, respectively, as the hydrochloride as follows:
Unit of Sale | Concentration |
NDC 70436-203-80 Carton containing 1 Vial | 250 mg/20 mL (12.5 mg/mL) |
NDC 70436-203-82 Carton containing 10 Vials | 250 mg/20 mL (12.5 mg/mL) |
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature.]
Discard unused portion.
Manufactured by:
Hainan Poly Pharm. Co., Ltd.,
Guilinyang Economic Development Zone,
Haikou, Hainan, 571127, China
Distributed by:
Slate Run Pharmaceuticals, LLC.,
Columbus, Ohio 43215
10000396/01
Revised: 02/2023