Get your patient on Fluconazole - Fluconazole powder, For Suspension (Fluconazole)
Fluconazole - Fluconazole powder, For Suspension prescribing information
INDICATIONS AND USAGE
Fluconazole for oral suspension is indicated for the treatment of: 1. Oropharyngeal and esophageal candidiasis. In open noncomparative studies of relatively small numbers of patients, fluconazole for oral suspension was also effective for the treatment of Candida urinary tract infections, peritonitis, and systemic Candida infections including candidemia, disseminated candidiasis, and pneumonia. 2.000000000000000e+00 Cryptococcal meningitis . Before prescribing fluconazole for oral suspension for AIDS patients with cryptococcal meningitis , please see CLINICAL STUDIES section. Studies comparing fluconazole for oral suspension to amphotericin B in non-HIV infected patients have not been conducted. Prophylaxis: Fluconazole for oral suspension is also indicated to decrease the incidence of candidiasis in patients undergoing bone marrow transplantation who receive cytotoxic chemotherapy and/or radiation therapy. Specimens for fungal culture and other relevant laboratory studies (serology, histopathology) should be obtained prior to therapy to isolate and identify causative organisms. Therapy may be instituted before the results of the cultures and other laboratory studies are known; however, once these results become available, anti-infective therapy should be adjusted accordingly.
DOSAGE AND ADMINISTRATION
Dosage and Administration in Adults:
SINCE ORAL ABSORPTION IS RAPID AND ALMOST COMPLETE, THE DAILY DOSE OF FLUCONAZOLE IS THE SAME FOR ORAL (TABLETS AND SUSPENSION) AND INTRAVENOUS ADMINISTRATION. In general, a loading dose of twice the daily dose is recommended on the first day of therapy to result in plasma concentrations close to steady-state by the second day of therapy. The daily dose of fluconazole for oral suspension for the treatment of infections should be based on the infecting organism and the patient’s response to therapy. Treatment should be continued until clinical parameters or laboratory tests indicate that active fungal infection has subsided. An inadequate period of treatment may lead to recurrence of active infection. Patients with AIDS and cryptococcal meningitis or recurrent oropharyngeal candidiasis usually require maintenance therapy to prevent relapse. Oropharyngeal candidiasis : The recommended dosage of fluconazole for oral suspension for oropharyngeal candidiasis is 200 mg on the first day, followed by 100 mg once daily. Clinical evidence of oropharyngeal candidiasis generally resolves within several days, but treatment should be continued for at least 2 weeks to decrease the likelihood of relapse. Esophageal candidiasis : The recommended dosage of fluconazole for oral suspension for esophageal candidiasis is 200 mg on the first day, followed by 100 mg once daily. Doses up to 400 mg/day may be used, based on medical judgment of the patient’s response to therapy. Patients with esophageal candidiasis should be treated for a minimum of three weeks and for at least two weeks following resolution of symptoms. Systemic Candida infections : For systemic Candida infections including candidemia, disseminated candidiasis, and pneumonia, optimal therapeutic dosage and duration of therapy have not been established. In open, noncomparative studies of small numbers of patients, doses of up to 400 mg daily have been used. Urinary tract infections and peritonitis : For the treatment of Candida urinary tract infections and peritonitis, daily doses of 50 to 200 mg have been used in open, noncomparative studies of small numbers of patients. Cryptococcal meningitis : The recommended dosage for treatment of acute cryptococcal meningitis is 400 mg on the first day, followed by 200 mg once daily. A dosage of 400 mg once daily may be used, based on medical judgment of the patient’s response to therapy. The recommended duration of treatment for initial therapy of cryptococcal meningitis is 10 to 12 weeks after the cerebrospinal fluid becomes culture negative. The recommended dosage of fluconazole for oral suspension for suppression of relapse of cryptococcal meningitis in patients with AIDS is 200 mg once daily. Prophylaxis in patients undergoing bone marrow transplantation : The recommended fluconazole for oral suspension daily dosage for the prevention of candidiasis in patients undergoing bone marrow transplantation is 400 mg, once daily. Patients who are anticipated to have severe granulocytopenia (less than 500 neutrophils cells/mm 3 ) should start fluconazole for oral suspension prophylaxis several days before the anticipated onset of neutropenia, and continue for 7 days after the neutrophil count rises above 1000 cells/mm 3 .
Dosage and Administration in Children:
The following dose equivalency scheme should generally provide equivalent exposure in pediatric and adult patients:
| Pediatric Patients | Adults |
|---|---|
| 3 mg/kg | 100 mg |
| 6 mg/kg | 200 mg |
| 12 Some older children may have clearances similar to that of adults. Absolute doses exceeding 600 mg/day are not recommended. mg/kg | 400 mg |
Experience with fluconazole for oral suspension in neonates is limited to pharmacokinetic studies in premature newborns. (See CLINICAL PHARMACOLOGY .) Based on the prolonged half-life seen in premature newborns (gestational age 26 to 29 weeks), these children, in the first two weeks of life, should receive the same dosage (mg/kg) as in older children, but administered every 72 hours. After the first two weeks, these children should be dosed once daily. No information regarding fluconazole for oral suspension pharmacokinetics in full-term newborns is available. Oropharyngeal candidiasis : The recommended dosage of fluconazole for oral suspension for oropharyngeal candidiasis in children is 6 mg/kg on the first day, followed by 3 mg/kg once daily. Treatment should be administered for at least 2 weeks to decrease the likelihood of relapse. Esophageal candidiasis : For the treatment of esophageal candidiasis, the recommended dosage of fluconazole for oral suspension in children is 6 mg/kg on the first day, followed by 3 mg/kg once daily. Doses up to 12 mg/kg/day may be used, based on medical judgment of the patient’s response to therapy. Patients with esophageal candidiasis should be treated for a minimum of three weeks and for at least 2 weeks following the resolution of symptoms. Systemic Candida infections : For the treatment of candidemia and disseminated Candida infections, daily doses of 6 to 12 mg/kg/day have been used in an open, noncomparative study of a small number of children. Cryptococcal meningitis : For the treatment of acute cryptococcal meningitis , the recommended dosage is 12 mg/kg on the first day, followed by 6 mg/kg once daily. A dosage of 12 mg/kg once daily may be used, based on medical judgment of the patient’s response to therapy. The recommended duration of treatment for initial therapy of cryptococcal meningitis is 10 to 12 weeks after the cerebrospinal fluid becomes culture negative. For suppression of relapse of cryptococcal meningitis in children with AIDS, the recommended dose of fluconazole for oral suspension is 6 mg/kg once daily.
Dosage In Patients With Impaired Renal Function:
Fluconazole is cleared primarily by renal excretion as unchanged drug. In patients with impaired renal function who will receive multiple doses of fluconazole for oral suspension, an initial loading dose of 50 mg to 400 mg should be given. After the loading dose, the daily dose (according to indication) should be based on the following table:
| Creatinine Clearance (mL/min) | Recommended Dose (%) |
|---|---|
| >50 | 100 |
| ≤50 (no dialysis) | 50 |
| Hemodialysis | 100% after each hemodialysis |
Patients on hemodialysis should receive 100% of the recommended dose after each hemodialysis; on non-dialysis days, patients should receive a reduced dose according to their creatinine clearance.
These are suggested dose adjustments based on pharmacokinetics following administration of multiple doses. Further adjustment may be needed depending upon clinical condition. When serum creatinine is the only measure of renal function available, the following formula (based on sex, weight, and age of the patient) should be used to estimate the creatinine clearance in adults: Males: Weight (kg) x (140 – age) 72 x serum creatinine (mg/100 mL) Females: 0.85 × above value Although the pharmacokinetics of fluconazole has not been studied in children with renal insufficiency, dosage reduction in children with renal insufficiency should parallel that recommended for adults. The following formula may be used to estimate creatinine clearance in children: K x linear length or height (cm) serum creatinine (mg/100 mL) (Where K=0.55 for children older than 1 year and 0.45 for infants.)
Administration
Fluconazole for oral suspension is administered orally. Fluconazole for oral suspension can be taken with or without food.
Directions for Mixing the Oral Suspension
Prepare a suspension at time of dispensing as follows: tap bottle until all the powder flows freely. To reconstitute, add 24 mL of distilled water or Purified Water (USP) to fluconazole bottle and shake vigorously to suspend powder. Each bottle will deliver 35 mL of suspension. The concentrations of the reconstituted suspensions are as follows:
| Fluconazole Content per Bottle | Concentration of Reconstituted Suspension |
|---|---|
| 1400 mg | 40 mg/mL |
Note: Shake oral suspension well before using. Store reconstituted suspension between 30°C (86°F) and 5°C (41°F) and discard unused portion after 2 weeks. Protect from freezing.
CONTRAINDICATIONS
Fluconazole for oral suspension is contraindicated in patients who have shown hypersensitivity to fluconazole or to any of its excipients. There is no information regarding cross-hypersensitivity between fluconazole and other azole antifungal agents. Caution should be used in prescribing fluconazole for oral suspension to patients with hypersensitivity to other azoles. Coadministration of other drugs known to prolong the QT interval and which are metabolized via the enzyme CYP3A4 such as erythromycin, pimozide, and quinidine are contraindicated in patients receiving fluconazole for oral suspension. (See CLINICAL PHARMACOLOGY: Drug Interaction Studies and PRECAUTIONS .)
ADVERSE REACTIONS
Fluconazole is generally well tolerated. In some patients, particularly those with serious underlying diseases such as AIDS and cancer, changes in renal and hematological function test results and hepatic abnormalities have been observed during treatment with fluconazole and comparative agents, but the clinical significance and relationship to treatment is uncertain.
In Patients Receiving Multiple Doses:
Sixteen percent of over 4000 patients treated with fluconazole in clinical trials of 7 days or more experienced adverse events. Treatment was discontinued in 1.5% of patients due to adverse clinical events and in 1.3% of patients due to laboratory test abnormalities. Clinical adverse events were reported more frequently in HIV infected patients (21%) than in non-HIV infected patients (13%); however, the patterns in HIV infected and non-HIV infected patients were similar. The proportions of patients discontinuing therapy due to clinical adverse events were similar in the two groups (1.5%). The following treatment-related clinical adverse events occurred at an incidence of 1% or greater in 4048 patients receiving fluconazole for 7 or more days in clinical trials: nausea 3.7%, headache 1.9%, skin rash 1.8%, vomiting 1.7%, abdominal pain 1.7%, and diarrhea 1.5%. Hepato-biliary: In combined clinical trials and marketing experience, there have been rare cases of serious hepatic reactions during treatment with fluconazole. (See WARNINGS .) The spectrum of these hepatic reactions has ranged from mild transient elevations in transaminases to clinical hepatitis, cholestasis and fulminant hepatic failure, including fatalities. Instances of fatal hepatic reactions were noted to occur primarily in patients with serious underlying medical conditions (predominantly AIDS or malignancy) and often while taking multiple concomitant medications. Transient hepatic reactions, including hepatitis and jaundice, have occurred among patients with no other identifiable risk factors. In each of these cases, liver function returned to baseline on discontinuation of fluconazole. In two comparative trials evaluating the efficacy of fluconazole for the suppression of relapse of cryptococcal meningitis , a statistically significant increase was observed in median AST (SGOT) levels from a baseline value of 30 IU/L to 41 IU/L in one trial and 34 IU/L to 66 IU/L in the other. The overall rate of serum transaminase elevations of more than 8 times the upper limit of normal was approximately 1% in fluconazole-treated patients in clinical trials. These elevations occurred in patients with severe underlying disease, predominantly AIDS or malignancies, most of whom were receiving multiple concomitant medications, including many known to be hepatotoxic. The incidence of abnormally elevated serum transaminases was greater in patients taking fluconazole concomitantly with one or more of the following medications: rifampin, phenytoin, isoniazid, valproic acid, or oral sulfonylurea hypoglycemic agents.
Post-Marketing Experience
In addition, the following adverse events have occurred during post-marketing experience. Immunologic: In rare cases, anaphylaxis (including angioedema, face edema and pruritus) has been reported. Body as a Whole: Asthenia, fatigue, fever, malaise. Cardiovascular: QT prolongation, torsade de pointes. (See PRECAUTIONS .) Central Nervous System: Seizures, dizziness. Hematopoietic and Lymphatic: Leukopenia, including neutropenia and agranulocytosis, thrombocytopenia. Metabolic: Hypercholesterolemia, hypertriglyceridemia, hypokalemia. Gastrointestinal: Cholestasis, dry mouth, hepatocellular damage, dyspepsia, vomiting. Other Senses: Taste perversion. Musculoskeletal System: Myalgia. Nervous System: Insomnia, paresthesia, somnolence, tremor, vertigo. Skin and Appendages: Acute generalized exanthematous pustulosis, drug eruption including fixed drug eruption, increased sweating, exfoliative skin disorders including Stevens-Johnson syndrome and toxic epidermal necrolysis, drug reaction with eosinophilia and systemic symptoms (DRESS) (See WARNINGS ), alopecia.
Adverse Reactions in Children:
The pattern and incidence of adverse events and laboratory abnormalities recorded during pediatric clinical trials are comparable to those seen in adults. In Phase II/III clinical trials conducted in the United States and in Europe, 577 pediatric patients, ages 1 day to 17 years were treated with fluconazole at doses up to 15 mg/kg/day for up to 1,616 days. Thirteen percent of children experienced treatment-related adverse events. The most commonly reported events were vomiting (5%), abdominal pain (3%), nausea (2%), and diarrhea (2%). Treatment was discontinued in 2.3% of patients due to adverse clinical events and in 1.4% of patients due to laboratory test abnormalities. The majority of treatment-related laboratory abnormalities were elevations of transaminases or alkaline phosphatase.
| Fluconazole (N=577) | Comparative Agents (N=451) | |
|---|---|---|
| With any side effect | 13.0 | 9.3 |
| Vomiting | 5.4 | 5.1 |
| Abdominal pain | 2.8 | 1.6 |
| Nausea | 2.3 | 1.6 |
| Diarrhea | 2.1 | 2.2 |
Drug Interaction Studies (See PRECAUTIONS, Drug Interactions)
Oral contraceptives: Oral contraceptives were administered as a single dose both before and after the oral administration of fluconazole 50 mg once daily for 10 days in 10 healthy women. There was no significant difference in ethinyl estradiol or levonorgestrel AUC after the administration of 50 mg of fluconazole. The mean increase in ethinyl estradiol AUC was 6% (range: –47 to 108%) and levonorgestrel AUC increased 17% (range: –33 to 141%).
In a second study, twenty-five normal females received daily doses of both 200 mg fluconazole tablets or placebo for two, ten-day periods. The treatment cycles were one month apart with all subjects receiving fluconazole during one cycle and placebo during the other. The order of study treatment was random. Single doses of an oral contraceptive tablet containing levonorgestrel and ethinyl estradiol were administered on the final treatment day (Day 10) of both cycles. Following administration of 200 mg of fluconazole, the mean percentage increase of AUC for levonorgestrel compared to placebo was 25% (range: –12 to 82%) and the mean percentage increase for ethinyl estradiol compared to placebo was 38% (range: –11 to 101%). Both of these increases were statistically significantly different from placebo. A third study evaluated the potential interaction of once-weekly dosing of fluconazole 300 mg to 21 normal females taking an oral contraceptive containing ethinyl estradiol and norethindrone. In this placebo-controlled, double-blind, randomized, two-way crossover study carried out over three cycles of oral contraceptive treatment, fluconazole dosing resulted in small increases in the mean AUCs of ethinyl estradiol and norethindrone compared to similar placebo dosing. The mean AUCs of ethinyl estradiol and norethindrone increased by 24% (95% C.I. range: 18 to 31%) and 13% (95% C.I. range: 8 to 18%), respectively, relative to placebo. Fluconazole treatment did not cause a decrease in the ethinyl estradiol AUC of any individual subject in this study compared to placebo dosing. The individual AUC values of norethindrone decreased very slightly (<5%) in 3 of the 21 subjects after fluconazole treatment. Cimetidine: Fluconazole 100 mg was administered as a single oral dose alone and two hours after a single dose of cimetidine 400 mg to six healthy male volunteers. After the administration of cimetidine, there was a significant decrease in fluconazole AUC and C max . There was a mean ± SD decrease in fluconazole AUC of 13% ± 11% (range: –3.4 to –31%) and C max decreased 19% ± 14% (range: –5 to –40%). However, the administration of cimetidine 600 mg to 900 mg intravenously over a four-hour period (from one hour before to 3 hours after a single oral dose of fluconazole 200 mg) did not affect the bioavailability or pharmacokinetics of fluconazole in 24 healthy male volunteers. Antacid: Administration of Maalox ® (20 mL) to 14 normal male volunteers immediately prior to a single dose of fluconazole 100 mg had no effect on the absorption or elimination of fluconazole. Hydrochlorothiazide: Concomitant oral administration of 100 mg fluconazole and 50 mg hydrochlorothiazide for 10 days in 13 normal volunteers resulted in a significant increase in fluconazole AUC and C max compared to fluconazole given alone. There was a mean ± SD increase in fluconazole AUC and C max of 45% ± 31% (range: 19 to 114%) and 43% ± 31% (range: 19 to 122%), respectively. These changes are attributed to a mean ± SD reduction in renal clearance of 30% ± 12% (range: –10 to –50%). Rifampin: Administration of a single oral 200 mg dose of fluconazole after 15 days of rifampin administered as 600 mg daily in eight healthy male volunteers resulted in a significant decrease in fluconazole AUC and a significant increase in apparent oral clearance of fluconazole. There was a mean ± SD reduction in fluconazole AUC of 23% ± 9% (range: –13 to –42%). Apparent oral clearance of fluconazole increased 32% ± 17% (range: 16 to 72%). Fluconazole half-life decreased from 33.4 ± 4.4 hours to 26.8 ± 3.9 hours. (See PRECAUTIONS .) Warfarin: There was a significant increase in prothrombin time response (area under the prothrombin time-time curve) following a single dose of warfarin (15 mg) administered to 13 normal male volunteers following oral fluconazole 200 mg administered daily for 14 days as compared to the administration of warfarin alone. There was a mean ± SD increase in the prothrombin time response (area under the prothrombin time-time curve) of 7% ± 4% (range: –2 to 13%). (See PRECAUTIONS .) Mean is based on data from 12 subjects as one of 13 subjects experienced a 2-fold increase in his prothrombin time response. Phenytoin: Phenytoin AUC was determined after 4 days of phenytoin dosing (200 mg daily, orally for 3 days followed by 250 mg intravenously for one dose) both with and without the administration of fluconazole (oral fluconazole 200 mg daily for 16 days) in 10 normal male volunteers. There was a significant increase in phenytoin AUC. The mean ± SD increase in phenytoin AUC was 88% ± 68% (range: 16 to 247%). The absolute magnitude of this interaction is unknown because of the intrinsically nonlinear disposition of phenytoin. (See PRECAUTIONS .) Cyclosporine: Cyclosporine AUC and C max were determined before and after the administration of fluconazole 200 mg daily for 14 days in eight renal transplant patients who had been on cyclosporine therapy for at least 6 months and on a stable cyclosporine dose for at least 6 weeks. There was a significant increase in cyclosporine AUC, C max , C min (24-hour concentration), and a significant reduction in apparent oral clearance following the administration of fluconazole. The mean ± SD increase in AUC was 92% ± 43% (range: 18 to 147%). The C max increased 60% ± 48% (range: –5 to 133%). The C min increased 157% ± 96% (range: 33 to 360%). The apparent oral clearance decreased 45% ± 15% (range: –15 to –60%). (See PRECAUTIONS .) Zidovudine: Plasma zidovudine concentrations were determined on two occasions (before and following fluconazole 200 mg daily for 15 days) in 13 volunteers with AIDS or ARC who were on a stable zidovudine dose for at least two weeks. There was a significant increase in zidovudine AUC following the administration of fluconazole. The mean ± SD increase in AUC was 20% ± 32% (range: –27 to 104%). The metabolite, GZDV, to parent drug ratio significantly decreased after the administration of fluconazole, from 7.6 ± 3.6 to 5.7 ± 2.2. Theophylline: The pharmacokinetics of theophylline were determined from a single intravenous dose of aminophylline (6 mg/kg) before and after the oral administration of fluconazole 200 mg daily for 14 days in 16 normal male volunteers. There were significant increases in theophylline AUC, C max , and half-life with a corresponding decrease in clearance. The mean ± SD theophylline AUC increased 21% ± 16% (range: –5 to 48%). The C max increased 13% ± 17% (range: –13 to 40%). Theophylline clearance decreased 16% ± 11% (range: –32 to 5%). The half-life of theophylline increased from 6.6 ± 1.7 hours to 7.9 ± 1.5 hours. (See PRECAUTIONS .) Quinidine: Although not studied in vitro or in vivo , concomitant administration of fluconazole with quinidine may result in inhibition of quinidine metabolism. Use of quinidine has been associated with QT prolongation and rare occurrences of torsade de pointes. Coadministration of fluconazole and quinidine is contraindicated. (See CONTRAINDICATIONS and PRECAUTIONS .) Oral hypoglycemics: The effects of fluconazole on the pharmacokinetics of the sulfonylurea oral hypoglycemic agents tolbutamide, glipizide, and glyburide were evaluated in three placebo-controlled studies in normal volunteers. All subjects received the sulfonylurea alone as a single dose and again as a single dose following the administration of fluconazole 100 mg daily for 7 days. In these three studies, 22/46 (47.8%) of fluconazole-treated patients and 9/22 (40.1%) of placebo-treated patients experienced symptoms consistent with hypoglycemia. (See PRECAUTIONS .) Tolbutamide: In 13 normal male volunteers, there was significant increase in tolbutamide (500 mg single dose) AUC and C max following the administration of fluconazole. There was a mean ± SD increase in tolbutamide AUC of 26% ± 9% (range: 12 to 39%). Tolbutamide C max increased 11% ± 9% (range: –6 to 27%). (See PRECAUTIONS .) Glipizide: The AUC and C max of glipizide (2.5 mg single dose) were significantly increased following the administration of fluconazole in 13 normal male volunteers. There was a mean ± SD increase in AUC of 49% ± 13% (range: 27 to 73%) and an increase in C max of 19% ± 23% (range: –11 to 79%). (See PRECAUTIONS .) Glyburide: The AUC and C max of glyburide (5 mg single dose) were significantly increased following the administration of fluconazole in 20 normal male volunteers. There was a mean ± SD increase in AUC of 44% ± 29% (range: –13 to 115%) and C max increased 19% ± 19% (range: –23 to 62%). Five subjects required oral glucose following the ingestion of glyburide after 7 days of fluconazole administration. (See PRECAUTIONS .) Rifabutin: There have been published reports that an interaction exists when fluconazole is administered concomitantly with rifabutin, leading to increased serum levels of rifabutin. (See PRECAUTIONS .) Tacrolimus: There have been published reports that an interaction exists when fluconazole is administered concomitantly with tacrolimus, leading to increased serum levels of tacrolimus. (See PRECAUTIONS .) Midazolam: The effect of fluconazole on the pharmacokinetics and pharmacodynamics of midazolam was examined in a randomized, cross-over study in 12 volunteers. In the study, subjects ingested placebo or 400 mg fluconazole on Day 1 followed by 200 mg daily from Day 2 to Day 6. In addition, a 7.5 mg dose of midazolam was orally ingested on the first day, 0.05 mg/kg was administered intravenously on the fourth day, and 7.5 mg orally on the sixth day. Fluconazole reduced the clearance of IV midazolam by 51%. On the first day of dosing, fluconazole increased the midazolam AUC and C max by 259% and 150%, respectively. On the sixth day of dosing, fluconazole increased the midazolam AUC and C max by 259% and 74%, respectively. The psychomotor effects of midazolam were significantly increased after oral administration of midazolam but not significantly affected following intravenous midazolam. A second randomized, double-dummy, placebo-controlled, cross over study in three phases was performed to determine the effect of route of administration of fluconazole on the interaction between fluconazole and midazolam. In each phase the subjects were given oral fluconazole 400 mg and intravenous saline; oral placebo and intravenous fluconazole 400 mg; and oral placebo and IV saline. An oral dose of 7.5 mg of midazolam was ingested after fluconazole/placebo. The AUC and C max of midazolam were significantly higher after oral than IV administration of fluconazole. Oral fluconazole increased the midazolam AUC and C max by 272% and 129%, respectively. IV fluconazole increased the midazolam AUC and C max by 244% and 79%, respectively. Both oral and IV fluconazole increased the pharmacodynamic effects of midazolam. (See PRECAUTIONS .) Azithromycin: An open-label, randomized, three-way crossover study in 18 healthy subjects assessed the effect of a single 800 mg oral dose of fluconazole on the pharmacokinetics of a single 1200 mg oral dose of azithromycin as well as the effects of azithromycin on the pharmacokinetics of fluconazole. There was no significant pharmacokinetic interaction between fluconazole and azithromycin. Voriconazole: Voriconazole is a substrate for both CYP2C9 and CYP3A4 isoenzymes. Concurrent administration of oral Voriconazole (400 mg Q12h for 1 day, then 200 mg Q12h for 2.5 days) and oral fluconazole (400 mg on Day 1, then 200 mg Q24h for 4 days) to 6 healthy male subjects resulted in an increase in C max and AUCτ of voriconazole by an average of 57% (90% CI: 20% to 107%) and 79% (90% CI: 40% to 128%), respectively. In a follow-on clinical study involving 8 healthy male subjects, reduced dosing and/or frequency of voriconazole and fluconazole did not eliminate or diminish this effect. (See PRECAUTIONS . ) Tofacitinib: Coadministration of fluconazole (400 mg on Day 1 and 200 mg once daily for 6 days [Days 2 to 7]) and tofacitinib (30 mg single dose on Day 5) in healthy subjects resulted in increased mean tofacitinib AUC and C max values of approximately 79% (90% CI: 64% to 96%) and 27% (90% CI: 12% to 44%), respectively, compared to administration of tofacitinib alone. (See PRECAUTIONS . ) Abrocitinib: When coadministered with fluconazole (inhibitor of CYP2C9, 2C19, and 3A4), the systemic exposure (AUC) of abrocitinib was approximately 4.8-fold higher and the combined exposure (AUC) of abrocitinib and its active metabolites was approximately 2.5-fold higher compared to when abrocitinib was administered alone. (See PRECAUTIONS . )
DESCRIPTION
Fluconazole, the first of a new subclass of synthetic triazole antifungal agents, is available as a powder for oral suspension. Fluconazole is designated chemically as 2,4-difluoro-α,α 1 -bis(1H-1,2,4-triazol-1-ylmethyl) benzyl alcohol with a molecular formula of C 13 H 12 F 2 N 6 O and molecular weight of 306.3. The structural formula is:
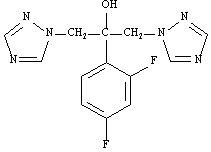
Fluconazole USP is a white or almost white, crystalline powder which is slightly soluble in water and saline. Fluconazole for oral suspension USP contains 1400 mg of fluconazole and the following inactive ingredients: sodium benzoate, citric acid anhydrous, sodium citrate dihydrate, xanthan gum, titanium dioxide, colloidal silicon dioxide, and sucrose. After reconstitution with 24 mL of distilled water or Purified Water (USP), each mL of reconstituted suspension contains 40 mg of fluconazole.
CLINICAL PHARMACOLOGY
Pharmacokinetics and Metabolism
The pharmacokinetic properties of fluconazole are similar following administration by the intravenous or oral routes. In normal volunteers, the bioavailability of orally administered fluconazole is over 90% compared with intravenous administration. Bioequivalence was established between the 100 mg tablet and both suspension strengths when administered as a single 200 mg dose. Peak plasma concentrations (C max ) in fasted normal volunteers occur between 1 and 2 hours with a terminal plasma elimination half-life of approximately 30 hours (range: 20 to 50 hours) after oral administration.
In fasted normal volunteers, administration of a single oral 400 mg dose of fluconazole leads to a mean C max of 6.72 mcg/mL (range: 4.12 to 8.08 mcg/mL) and after single oral doses of 50 to 400 mg, fluconazole plasma concentrations and area under the plasma concentration-time curve (AUC) are dose proportional.
The C max and AUC data from a food-effect study involving administration of fluconazole tablets to healthy volunteers under fasting conditions and with a high-fat meal indicated that exposure to the drug is not affected by food. Therefore, fluconazole may be taken without regard to meals. (See DOSAGE AND ADMINISTRATION .) Steady-state concentrations are reached within 5 to 10 days following oral doses of 50 to 400 mg given once daily. Administration of a loading dose (on Day 1) of twice the usual daily dose results in plasma concentrations close to steady-state by the second day. The apparent volume of distribution of fluconazole approximates that of total body water. Plasma protein binding is low (11 to 12%). Following either single- or multiple oral doses for up to 14 days, fluconazole penetrates into all body fluids studied (see table below). In normal volunteers, saliva concentrations of fluconazole were equal to or slightly greater than plasma concentrations regardless of dose, route, or duration of dosing. In patients with bronchiectasis, sputum concentrations of fluconazole following a single 150 mg oral dose were equal to plasma concentrations at both 4 and 24 hours post dose. In patients with fungal meningitis, fluconazole concentrations in the cerebrospinal fluid (CSF) are approximately 80% of the corresponding plasma concentrations. A single oral 150 mg dose of fluconazole administered to 27 patients penetrated into vaginal tissue, resulting in tissue: plasma ratios ranging from 0.94 to 1.14 over the first 48 hours following dosing. A single oral 150 mg dose of fluconazole administered to 14 patients penetrated into vaginal fluid, resulting in fluid: plasma ratios ranging from 0.36 to 0.71 over the first 72 hours following dosing.
| Tissue or Fluid | Ratio of Fluconazole Tissue (Fluid)/Plasma Concentration Relative to concurrent concentrations in plasma in subjects with normal renal function. |
|---|---|
| Cerebrospinal fluid Independent of degree of meningeal inflammation. | 0.5–0.9 |
| Saliva | 1 |
| Sputum | 1 |
| Blister fluid | 1 |
| Urine | 10 |
| Normal skin | 10 |
| Nails | 1 |
| Blister skin | 2 |
| Vaginal tissue | 1 |
| Vaginal fluid | 0.4–0.7 |
In normal volunteers, fluconazole is cleared primarily by renal excretion, with approximately 80% of the administered dose appearing in the urine as unchanged drug. About 11% of the dose is excreted in the urine as metabolites. The pharmacokinetics of fluconazole are markedly affected by reduction in renal function. There is an inverse relationship between the elimination half-life and creatinine clearance. The dose of fluconazole may need to be reduced in patients with impaired renal function. (See DOSAGE AND ADMINISTRATION .) A 3-hour hemodialysis session decreases plasma concentrations by approximately 50%.
In normal volunteers, fluconazole administration (doses ranging from 200 mg to 400 mg once daily for up to 14 days) was associated with small and inconsistent effects on testosterone concentrations, endogenous corticosteroid concentrations, and the adrenocorticotropic hormone (ACTH)-stimulated cortisol response.
Pharmacokinetics in Children
In children, the following pharmacokinetic data {Mean (%cv)} have been reported:
| Age Studied | Dose (mg/kg) | Clearance (mL/min/kg) | Half-life (Hours) | Cmax (mcg/mL) | Vdss (L/kg) |
|---|---|---|---|---|---|
| 9 months–13 years | Single-Oral 2 mg/kg | 0.40 (38%) N=14 | 25.0 | 2.9 (22%) N=16 | ___ |
| 9 months–13 years | Single-Oral 8 mg/kg | 0.51 (60%) N=15 | 19.5 | 9.8 (20%) N=15 | ___ |
| 5–15 years | Multiple IV 2 mg/kg | 0.49 (40%) N=4 | 17.4 | 5.5 (25%) N=5 | 0.722 (36%) N=4 |
| 5–15 years | Multiple IV 4 mg/kg | 0.59 (64%) N=5 | 15.2 | 11.4 (44%) N=6 | 0.729 (33%) N=5 |
| 5–15 years | Multiple IV 8 mg/kg | 0.66 (31%) N=7 | 17.6 | 14.1 (22%) N=8 | 1.069 (37%) N=7 |
Clearance corrected for body weight was not affected by age in these studies. Mean body clearance in adults is reported to be 0.23 (17%) mL/min/kg. In premature newborns (gestational age 26 to 29 weeks), the mean (%cv) clearance within 36 hours of birth was 0.18 (35%, N=7) mL/min/kg, which increased with time to a mean of 0.218 (31%, N=9) mL/min/kg six days later and 0.333 (56%, N=4) mL/min/kg 12 days later. Similarly, the half-life was 73.6 hours, which decreased with time to a mean of 53.2 hours six days later and 46.6 hours 12 days later.
Pharmacokinetics in Elderly
A pharmacokinetic study was conducted in 22 subjects, 65 years of age or older receiving a single 50 mg oral dose of fluconazole. Ten of these patients were concomitantly receiving diuretics. The C max was 1.54 mcg/mL and occurred at 1.3 hours post dose. The mean AUC was 76.4 ± 20.3 mcg⋅h/mL, and the mean terminal half-life was 46.2 hours. These pharmacokinetic parameter values are higher than analogous values reported for normal young male volunteers. Coadministration of diuretics did not significantly alter the AUC or C max . In addition, creatinine clearance (74 mL/min), the percent of drug recovered unchanged in urine (0 to 24 hours, 22%), and the fluconazole renal clearance estimates (0.124 mL/min/kg) for the elderly were generally lower than those of younger volunteers. Thus, the alteration of fluconazole disposition in the elderly appears to be related to reduced renal function characteristic of this group. A plot of each subject’s terminal elimination half-life versus creatinine clearance compared to the predicted half-life – creatinine clearance curve derived from normal subjects and subjects with varying degrees of renal insufficiency indicated that 21 of 22 subjects fell within the 95% confidence limit of the predicted half-life-creatinine clearance curves. These results are consistent with the hypothesis that higher values for the pharmacokinetic parameters observed in the elderly subjects compared to normal young male volunteers are due to the decreased kidney function that is expected in the elderly.
Drug Interaction Studies (See PRECAUTIONS, Drug Interactions)
Oral contraceptives: Oral contraceptives were administered as a single dose both before and after the oral administration of fluconazole 50 mg once daily for 10 days in 10 healthy women. There was no significant difference in ethinyl estradiol or levonorgestrel AUC after the administration of 50 mg of fluconazole. The mean increase in ethinyl estradiol AUC was 6% (range: –47 to 108%) and levonorgestrel AUC increased 17% (range: –33 to 141%).
In a second study, twenty-five normal females received daily doses of both 200 mg fluconazole tablets or placebo for two, ten-day periods. The treatment cycles were one month apart with all subjects receiving fluconazole during one cycle and placebo during the other. The order of study treatment was random. Single doses of an oral contraceptive tablet containing levonorgestrel and ethinyl estradiol were administered on the final treatment day (Day 10) of both cycles. Following administration of 200 mg of fluconazole, the mean percentage increase of AUC for levonorgestrel compared to placebo was 25% (range: –12 to 82%) and the mean percentage increase for ethinyl estradiol compared to placebo was 38% (range: –11 to 101%). Both of these increases were statistically significantly different from placebo. A third study evaluated the potential interaction of once-weekly dosing of fluconazole 300 mg to 21 normal females taking an oral contraceptive containing ethinyl estradiol and norethindrone. In this placebo-controlled, double-blind, randomized, two-way crossover study carried out over three cycles of oral contraceptive treatment, fluconazole dosing resulted in small increases in the mean AUCs of ethinyl estradiol and norethindrone compared to similar placebo dosing. The mean AUCs of ethinyl estradiol and norethindrone increased by 24% (95% C.I. range: 18 to 31%) and 13% (95% C.I. range: 8 to 18%), respectively, relative to placebo. Fluconazole treatment did not cause a decrease in the ethinyl estradiol AUC of any individual subject in this study compared to placebo dosing. The individual AUC values of norethindrone decreased very slightly (<5%) in 3 of the 21 subjects after fluconazole treatment. Cimetidine: Fluconazole 100 mg was administered as a single oral dose alone and two hours after a single dose of cimetidine 400 mg to six healthy male volunteers. After the administration of cimetidine, there was a significant decrease in fluconazole AUC and C max . There was a mean ± SD decrease in fluconazole AUC of 13% ± 11% (range: –3.4 to –31%) and C max decreased 19% ± 14% (range: –5 to –40%). However, the administration of cimetidine 600 mg to 900 mg intravenously over a four-hour period (from one hour before to 3 hours after a single oral dose of fluconazole 200 mg) did not affect the bioavailability or pharmacokinetics of fluconazole in 24 healthy male volunteers. Antacid: Administration of Maalox ® (20 mL) to 14 normal male volunteers immediately prior to a single dose of fluconazole 100 mg had no effect on the absorption or elimination of fluconazole. Hydrochlorothiazide: Concomitant oral administration of 100 mg fluconazole and 50 mg hydrochlorothiazide for 10 days in 13 normal volunteers resulted in a significant increase in fluconazole AUC and C max compared to fluconazole given alone. There was a mean ± SD increase in fluconazole AUC and C max of 45% ± 31% (range: 19 to 114%) and 43% ± 31% (range: 19 to 122%), respectively. These changes are attributed to a mean ± SD reduction in renal clearance of 30% ± 12% (range: –10 to –50%). Rifampin: Administration of a single oral 200 mg dose of fluconazole after 15 days of rifampin administered as 600 mg daily in eight healthy male volunteers resulted in a significant decrease in fluconazole AUC and a significant increase in apparent oral clearance of fluconazole. There was a mean ± SD reduction in fluconazole AUC of 23% ± 9% (range: –13 to –42%). Apparent oral clearance of fluconazole increased 32% ± 17% (range: 16 to 72%). Fluconazole half-life decreased from 33.4 ± 4.4 hours to 26.8 ± 3.9 hours. (See PRECAUTIONS .) Warfarin: There was a significant increase in prothrombin time response (area under the prothrombin time-time curve) following a single dose of warfarin (15 mg) administered to 13 normal male volunteers following oral fluconazole 200 mg administered daily for 14 days as compared to the administration of warfarin alone. There was a mean ± SD increase in the prothrombin time response (area under the prothrombin time-time curve) of 7% ± 4% (range: –2 to 13%). (See PRECAUTIONS .) Mean is based on data from 12 subjects as one of 13 subjects experienced a 2-fold increase in his prothrombin time response. Phenytoin: Phenytoin AUC was determined after 4 days of phenytoin dosing (200 mg daily, orally for 3 days followed by 250 mg intravenously for one dose) both with and without the administration of fluconazole (oral fluconazole 200 mg daily for 16 days) in 10 normal male volunteers. There was a significant increase in phenytoin AUC. The mean ± SD increase in phenytoin AUC was 88% ± 68% (range: 16 to 247%). The absolute magnitude of this interaction is unknown because of the intrinsically nonlinear disposition of phenytoin. (See PRECAUTIONS .) Cyclosporine: Cyclosporine AUC and C max were determined before and after the administration of fluconazole 200 mg daily for 14 days in eight renal transplant patients who had been on cyclosporine therapy for at least 6 months and on a stable cyclosporine dose for at least 6 weeks. There was a significant increase in cyclosporine AUC, C max , C min (24-hour concentration), and a significant reduction in apparent oral clearance following the administration of fluconazole. The mean ± SD increase in AUC was 92% ± 43% (range: 18 to 147%). The C max increased 60% ± 48% (range: –5 to 133%). The C min increased 157% ± 96% (range: 33 to 360%). The apparent oral clearance decreased 45% ± 15% (range: –15 to –60%). (See PRECAUTIONS .) Zidovudine: Plasma zidovudine concentrations were determined on two occasions (before and following fluconazole 200 mg daily for 15 days) in 13 volunteers with AIDS or ARC who were on a stable zidovudine dose for at least two weeks. There was a significant increase in zidovudine AUC following the administration of fluconazole. The mean ± SD increase in AUC was 20% ± 32% (range: –27 to 104%). The metabolite, GZDV, to parent drug ratio significantly decreased after the administration of fluconazole, from 7.6 ± 3.6 to 5.7 ± 2.2. Theophylline: The pharmacokinetics of theophylline were determined from a single intravenous dose of aminophylline (6 mg/kg) before and after the oral administration of fluconazole 200 mg daily for 14 days in 16 normal male volunteers. There were significant increases in theophylline AUC, C max , and half-life with a corresponding decrease in clearance. The mean ± SD theophylline AUC increased 21% ± 16% (range: –5 to 48%). The C max increased 13% ± 17% (range: –13 to 40%). Theophylline clearance decreased 16% ± 11% (range: –32 to 5%). The half-life of theophylline increased from 6.6 ± 1.7 hours to 7.9 ± 1.5 hours. (See PRECAUTIONS .) Quinidine: Although not studied in vitro or in vivo , concomitant administration of fluconazole with quinidine may result in inhibition of quinidine metabolism. Use of quinidine has been associated with QT prolongation and rare occurrences of torsade de pointes. Coadministration of fluconazole and quinidine is contraindicated. (See CONTRAINDICATIONS and PRECAUTIONS .) Oral hypoglycemics: The effects of fluconazole on the pharmacokinetics of the sulfonylurea oral hypoglycemic agents tolbutamide, glipizide, and glyburide were evaluated in three placebo-controlled studies in normal volunteers. All subjects received the sulfonylurea alone as a single dose and again as a single dose following the administration of fluconazole 100 mg daily for 7 days. In these three studies, 22/46 (47.8%) of fluconazole-treated patients and 9/22 (40.1%) of placebo-treated patients experienced symptoms consistent with hypoglycemia. (See PRECAUTIONS .) Tolbutamide: In 13 normal male volunteers, there was significant increase in tolbutamide (500 mg single dose) AUC and C max following the administration of fluconazole. There was a mean ± SD increase in tolbutamide AUC of 26% ± 9% (range: 12 to 39%). Tolbutamide C max increased 11% ± 9% (range: –6 to 27%). (See PRECAUTIONS .) Glipizide: The AUC and C max of glipizide (2.5 mg single dose) were significantly increased following the administration of fluconazole in 13 normal male volunteers. There was a mean ± SD increase in AUC of 49% ± 13% (range: 27 to 73%) and an increase in C max of 19% ± 23% (range: –11 to 79%). (See PRECAUTIONS .) Glyburide: The AUC and C max of glyburide (5 mg single dose) were significantly increased following the administration of fluconazole in 20 normal male volunteers. There was a mean ± SD increase in AUC of 44% ± 29% (range: –13 to 115%) and C max increased 19% ± 19% (range: –23 to 62%). Five subjects required oral glucose following the ingestion of glyburide after 7 days of fluconazole administration. (See PRECAUTIONS .) Rifabutin: There have been published reports that an interaction exists when fluconazole is administered concomitantly with rifabutin, leading to increased serum levels of rifabutin. (See PRECAUTIONS .) Tacrolimus: There have been published reports that an interaction exists when fluconazole is administered concomitantly with tacrolimus, leading to increased serum levels of tacrolimus. (See PRECAUTIONS .) Midazolam: The effect of fluconazole on the pharmacokinetics and pharmacodynamics of midazolam was examined in a randomized, cross-over study in 12 volunteers. In the study, subjects ingested placebo or 400 mg fluconazole on Day 1 followed by 200 mg daily from Day 2 to Day 6. In addition, a 7.5 mg dose of midazolam was orally ingested on the first day, 0.05 mg/kg was administered intravenously on the fourth day, and 7.5 mg orally on the sixth day. Fluconazole reduced the clearance of IV midazolam by 51%. On the first day of dosing, fluconazole increased the midazolam AUC and C max by 259% and 150%, respectively. On the sixth day of dosing, fluconazole increased the midazolam AUC and C max by 259% and 74%, respectively. The psychomotor effects of midazolam were significantly increased after oral administration of midazolam but not significantly affected following intravenous midazolam. A second randomized, double-dummy, placebo-controlled, cross over study in three phases was performed to determine the effect of route of administration of fluconazole on the interaction between fluconazole and midazolam. In each phase the subjects were given oral fluconazole 400 mg and intravenous saline; oral placebo and intravenous fluconazole 400 mg; and oral placebo and IV saline. An oral dose of 7.5 mg of midazolam was ingested after fluconazole/placebo. The AUC and C max of midazolam were significantly higher after oral than IV administration of fluconazole. Oral fluconazole increased the midazolam AUC and C max by 272% and 129%, respectively. IV fluconazole increased the midazolam AUC and C max by 244% and 79%, respectively. Both oral and IV fluconazole increased the pharmacodynamic effects of midazolam. (See PRECAUTIONS .) Azithromycin: An open-label, randomized, three-way crossover study in 18 healthy subjects assessed the effect of a single 800 mg oral dose of fluconazole on the pharmacokinetics of a single 1200 mg oral dose of azithromycin as well as the effects of azithromycin on the pharmacokinetics of fluconazole. There was no significant pharmacokinetic interaction between fluconazole and azithromycin. Voriconazole: Voriconazole is a substrate for both CYP2C9 and CYP3A4 isoenzymes. Concurrent administration of oral Voriconazole (400 mg Q12h for 1 day, then 200 mg Q12h for 2.5 days) and oral fluconazole (400 mg on Day 1, then 200 mg Q24h for 4 days) to 6 healthy male subjects resulted in an increase in C max and AUCτ of voriconazole by an average of 57% (90% CI: 20% to 107%) and 79% (90% CI: 40% to 128%), respectively. In a follow-on clinical study involving 8 healthy male subjects, reduced dosing and/or frequency of voriconazole and fluconazole did not eliminate or diminish this effect. (See PRECAUTIONS . ) Tofacitinib: Coadministration of fluconazole (400 mg on Day 1 and 200 mg once daily for 6 days [Days 2 to 7]) and tofacitinib (30 mg single dose on Day 5) in healthy subjects resulted in increased mean tofacitinib AUC and C max values of approximately 79% (90% CI: 64% to 96%) and 27% (90% CI: 12% to 44%), respectively, compared to administration of tofacitinib alone. (See PRECAUTIONS . ) Abrocitinib: When coadministered with fluconazole (inhibitor of CYP2C9, 2C19, and 3A4), the systemic exposure (AUC) of abrocitinib was approximately 4.8-fold higher and the combined exposure (AUC) of abrocitinib and its active metabolites was approximately 2.5-fold higher compared to when abrocitinib was administered alone. (See PRECAUTIONS . )
Microbiology
Mechanism of Action
Fluconazole is a highly selective inhibitor of fungal cytochrome P450 dependent enzyme lanosterol 14-α-demethylase. This enzyme functions to convert lanosterol to ergosterol. The subsequent loss of normal sterols correlates with the accumulation of 14-α-methyl sterols in fungi and may be responsible for the fungistatic activity of fluconazole. Mammalian cell demethylation is much less sensitive to fluconazole inhibition.
Resistance
A potential for development of resistance to fluconazole is well known. Fungal isolates exhibiting reduced susceptibility to other azoles may also show reduced susceptibility to fluconazole. The frequency of drug resistance development for the various fungi for which this drug is indicated is not known.
Fluconazole resistance may arise from a modification in the quality or quantity of the target enzyme (lanosterol 14-α-demethylase), reduced access to the drug target, or some combination of these mechanisms.
Point mutations in the gene ( ERG11 ) encoding for the target enzyme lead to an altered target with decreased affinity for azoles. Overexpression of ERG11 results in the production of high concentrations of the target enzyme, creating the need for higher intracellular drug concentrations to inhibit all of the enzyme molecules in the cell.
The second major mechanism of drug resistance involves active efflux of fluconazole out of the cell through the activation of two types of multidrug efflux transporters; the major facilitators (encoded by MDR genes) and those of the ATP-binding cassette superfamily (encoded by CDR genes). Upregulation of the MDR gene leads to fluconazole resistance, whereas, upregulation of CDR genes may lead to resistance to multiple azoles.
Resistance in Candida glabrata usually includes upregulation of CDR genes resulting in resistance to multiple azoles. For an isolate where the minimum inhibitory concentration (MIC) is categorized as Intermediate (16 to 32 mcg/mL), the highest fluconazole dose is recommended.
Candida krusei should be considered to be resistant to fluconazole. Resistance in C. krusei appears to be mediated by reduced sensitivity of the target enzyme to inhibition by the agent.
There have been reports of cases of superinfection with Candida species other than C. albicans , which are often inherently not susceptible to fluconazole (e.g., Candida krusei ). Such cases may require alternative antifungal therapy.
Antimicrobial Activity
Fluconazole has been shown to be active against most isolates of the following microorganisms both in vitro and in clinical infections.
Candida albicans
Candida glabrata (Many isolates are intermediately susceptible)
Candida parapsilosis
Candida tropicalis
Cryptococcus neoformans The following in vitro data are available, but their clinical significance is unknown. At least 90% of the following fungi exhibit an in vitro MIC less than or equal to the susceptible breakpoint for fluconazole (https://www.fda.gov/STIC) against isolates of similar genus or organism group. However, the effectiveness of fluconazole in treating clinical infections due to these fungi has not been established in adequate and well-controlled clinical trials.
Candida dubliniensis
Candida guilliermondii
Candida kefyr
Candida lusitaniae
Candida krusei should be considered to be resistant to fluconazole. Resistance in C. krusei appears to be mediated by reduced sensitivity of the target enzyme to inhibition by the agent.
There have been reports of cases of superinfection with Candida species other than C. albicans, which are often inherently not susceptible to fluconazole (e.g., Candida krusei ). Such cases may require alternative antifungal therapy.
Susceptibility Testing
For specific information regarding susceptibility test interpretive criteria and associated test methods and quality control standards recognized by FDA for this drug, please see: https://www.fda.gov/STIC.
CLINICAL STUDIES
Cryptococcal meningitis: In a multicenter study comparing fluconazole (200 mg/day) to amphotericin B (0.3 mg/kg/day) for treatment of cryptococcal meningitis in patients with AIDS, a multivariate analysis revealed three pretreatment factors that predicted death during the course of therapy: abnormal mental status, cerebrospinal fluid cryptococcal antigen titer greater than 1:1024, and cerebrospinal fluid white blood cell count of less than 20 cells/mm 3 . Mortality among high risk patients was 33% and 40% for amphotericin B and fluconazole patients, respectively (p=0.58), with overall deaths 14% (9 of 63 subjects) and 18% (24 of 131 subjects) for the 2 arms of the study (p=0.48). Optimal doses and regimens for patients with acute cryptococcal meningitis and at high risk for treatment failure remain to be determined. (Saag, et al . N Engl J Med 1992; 326:83-9.) Pediatric Studies Oropharyngeal candidiasis: An open-label, comparative study of the efficacy and safety of fluconazole (2 to 3 mg/kg/day) and oral nystatin (400,000 I.U. 4 times daily) in immunocompromised children with oropharyngeal candidiasis was conducted. Clinical and mycological response rates were higher in the children treated with fluconazole. Clinical cure at the end of treatment was reported for 86% of fluconazole-treated patients compared to 46% of nystatin treated patients. Mycologically, 76% of fluconazole treated patients had the infecting organism eradicated compared to 11% for nystatin treated patients.
| Fluconazole | Nystatin | |
|---|---|---|
| Enrolled | 96 | 90 |
| Clinical Cure | 76/88 (86%) | 36/78 (46%) |
| Mycological eradication Subjects without follow-up cultures for any reason were considered nonevaluable for mycological response. | 55/72 (76%) | 6/54 (11%) |
The proportion of patients with clinical relapse 2 weeks after the end of treatment was 14% for subjects receiving fluconazole and 16% for subjects receiving nystatin. At 4 weeks after the end of treatment, the percentages of patients with clinical relapse were 22% for fluconazole and 23% for nystatin.
HOW SUPPLIED
Fluconazole for Oral Suspension USP is supplied as white to off-white odorless powder to provide 35 mL per bottle as follows: NDC 72673-091-14 Fluconazole 1400 mg per bottle with child-resistant closure.
Storage
Before reconstitured: Store dry powder at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature]. After reconstitured: Store suspension between 30°C (86°F) and 5°C (41°F) and discard unused portion after 2 weeks. Protect from freezing. Maalox ® is a registered trademark of Novartis Consumer Health, Inc. XELJANZ ® is a registered trademark of Pfizer Inc. LYNPARZA ® is a registered trademark of AstraZeneca group of companies. Manufactured for: Zhejiang Poly Pharm Co., Ltd.