Get your patient on Lopressor Hct - Metoprolol Tartrate And Hydrochlorothiazide tablet (Metoprolol Tartrate And Hydrochlorothiazide)
Lopressor Hct - Metoprolol Tartrate And Hydrochlorothiazide tablet prescribing information
1 INDICATIONS AND USAGE
LOPRESSOR HCT is indicated for the treatment of hypertension, to lower blood pressure. Lowering blood pressure lowers the risk of fatal and non-fatal cardiovascular events, primarily strokes and myocardial infarctions. These benefits have been seen in controlled trials of antihypertensive drugs from a wide variety of pharmacologic classes including metoprolol.
Control of high blood pressure should be part of comprehensive cardiovascular risk management, including, as appropriate, lipid control, diabetes management, antithrombotic therapy, smoking cessation, exercise, and limited sodium intake. Many patients will require more than 1 drug to achieve blood pressure goals. For specific advice on goals and management, see published guidelines, such as those of the National High Blood Pressure Education Program’s Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC).
Numerous antihypertensive drugs, from a variety of pharmacologic classes and with different mechanisms of action, have been shown in randomized controlled trials to reduce cardiovascular morbidity and mortality, and it can be concluded that it is blood pressure reduction, and not some other pharmacologic property of the drugs, that is largely responsible for those benefits. The largest and most consistent cardiovascular outcome benefit has been a reduction in the risk of stroke, but reductions in myocardial infarction and cardiovascular mortality also have been seen regularly.
Elevated systolic or diastolic pressure causes increased cardiovascular risk, and the absolute risk increase per mmHg is greater at higher blood pressures, so that even modest reductions of severe hypertension can provide substantial benefit. Relative risk reduction from blood pressure reduction is similar across populations with varying absolute risk, so the absolute benefit is greater in patients who are at higher risk independent of their hypertension (for example, patients with diabetes or hyperlipidemia), and such patients would be expected to benefit from more aggressive treatment to a lower blood pressure goal.
Some antihypertensive drugs have smaller blood pressure effects (as monotherapy) in black patients, and many antihypertensive drugs have additional approved indications and effects (e.g., on angina, heart failure, or diabetic kidney disease). These considerations may guide selection of therapy.
LOPRESSOR HCT may be administered with other antihypertensive agents.
Limitation of Use
LOPRESSOR HCT is not indicated for initial therapy of hypertension. If the fixed combination represents the dose titrated to the individual patient’s needs, therapy with the fixed combination may be more convenient than with the separate components.
2 DOSAGE AND ADMINISTRATION
- Usual dose range: Hydrochlorothiazide 12.5 to 25 mg and metoprolol tartrate 100 mg dosed once daily. (2.1 )
2.1 Recommended Dosage
Titrate doses of individual components before switching to LOPRESSOR HCT.
Administer LOPRESSOR HCT with or immediately following meals.
Hydrochlorothiazide is usually given at a dosage of 12.5 mg to 50 mg per day. The usual initial dosage of metoprolol is 100 mg daily in single or divided doses. Dosage may be increased gradually until optimum blood pressure control is achieved.
Once daily dosing may not maintain the full effect for the entire dosing period, particularly at lower doses. In such patients, consider administration in divided doses.
Dosing regimens that exceed 50 mg of hydrochlorothiazide per day are not recommended.
3 DOSAGE FORMS AND STRENGTHS
LOPRESSOR HCT (metoprolol tartrate and hydrochlorothiazide) is supplied as capsule-shaped tablets in the following strengths:
50 mg / 25 mg: white and mottled-blue, scored (imprinted LOPHCT on one side and 463 twice on the scored side)
100 mg / 25 mg: white and mottled-pink, scored (imprinted LOPHCT on one side and 461 twice on the scored side)
100 mg / 50 mg: white and mottled-yellow, scored (imprinted LOPHCT on one side and 462 twice on the scored side)
4 CONTRAINDICATIONS
LOPRESSOR HCT is contraindicated in patients with:
- Cardiogenic shock or decompensated heart failure .
- Sinus bradycardia, sick sinus syndrome, and greater than first-degree block unless a permanent pacemaker is in place .
- Anuria
- Hypersensitivity to metoprolol tartrate or hydrochlorothiazide or to other sulfonamide-derived drugs.
5 WARNINGS AND PRECAUTIONS
- Abrupt cessation may exacerbate myocardial ischemia. (5.1 )
- May worsen congestive heart failure. (5.2 )
- Bronchospasm: Avoid beta-blockers. (5.3 )
- Bradycardia. (5.4 )
- Avoid discontinuing therapy prior to major surgery. (5.5 )
- Diabetes: May mask symptoms of hypoglycemia and alter glucose levels; monitor. (5.6 )
- Monitor serum electrolytes and creatinine periodically. (5.7 )
- Peripheral vascular disease: Can aggravate symptoms of arterial insufficiency. (5.9 )
- Pheochromocytoma: First initiate therapy with an alpha blocker. (5.10 )
- Abrupt withdrawal in thyrotoxicosis might precipitate a thyroid storm. (5.11 )
- Patients may be unresponsive to the usual doses of epinephrine used to treat allergic reaction. (5.12 )
5.1 Abrupt Cessation of Therapy
Following abrupt cessation of therapy with beta adrenergic blockers, exacerbations of angina pectoris and myocardial infarction may occur. When discontinuing chronically administered LOPRESSOR HCT, particularly in patients with ischemic heart disease, gradually reduce the dosage over a period of 1 to 2 weeks and monitor the patient. If angina markedly worsens or acute coronary ischemia develops, promptly resume therapy and take measures appropriate for the management of unstable angina. Warn patients not to interrupt therapy without their physician’s advice. Because coronary artery disease is common and may be unrecognized, avoid abruptly discontinuing metoprolol tartrate in patients treated only for hypertension.
5.2 Heart Failure
Worsening cardiac failure may occur during up-titration of beta-blockers. If such symptoms occur, increase diuretics and restore clinical stability before advancing the dose of metoprolol. It may be necessary to lower the dose of metoprolol tartrate or temporarily discontinue it. Such episodes do not preclude subsequent successful titration of metoprolol tartrate.
5.3 Bronchospastic Disease
Beta adrenergic blockers can cause bronchospasm. Patients with bronchospastic diseases should, in general, not receive beta-blockers. Because of its relative beta 1 cardio-selectivity, however, metoprolol tartrate may be used in patients with bronchospastic disease who do not respond to, or cannot tolerate, other antihypertensive treatment. Because beta 1 -selectivity is not absolute, use the lowest possible dose of metoprolol tartrate and have bronchodilators (e.g., beta 2 -agonists) readily available or administered concomitantly .
5.000000000000000e+00 4 Bradycardia
Bradycardia, including sinus pause, heart block, and cardiac arrest have occurred with the use of LOPRESSOR HCT. Patients with first-degree atrioventricular block, sinus node dysfunction, conduction disorders (including Wolff-Parkinson-White) or on concomitant drugs [see Drug Interactions (7 )] that cause bradycardia may be at increased risk. Monitor heart rate in patients receiving LOPRESSOR HCT. If severe bradycardia develops, reduce or stop LOPRESSOR HCT.
5.5 Major Surgery
Avoid initiation of high-dose regimen of LOPRESSOR HCT in patients with cardiovascular risk factors undergoing non-cardiac surgery, since use in such patients has been associated with bradycardia, hypotension, stroke and death.
Chronically administered beta-adrenergic blockers should not be routinely withdrawn prior to major surgery; however, the impaired ability of the heart to respond to reflex adrenergic stimuli may augment the risks of general anesthesia and surgical procedures [see Warnings and Precautions (5.1 )].
5.000000000000000e+00 6 Masked Symptoms of Hypoglycemia
Beta-blockers may prevent early warning signs of hypoglycemia, such as tachycardia, and increase the risk for severe or prolonged hypoglycemia at anytime during treatment, especially in patients with diabetes mellitus or children and patients who are fasting (i.e., surgery, not eating regularly, or are vomiting). If severe hypoglycemia occurs, patients should be instructed to seek emergency treatment.
5.7 Electrolyte and Metabolic Effects
LOPRESSOR HCT contains hydrochlorothiazide which can cause hypokalemia and hyponatremia. Hypomagnesemia can result in hypokalemia which may be difficult to treat despite potassium repletion. Monitor serum electrolytes periodically.
Hydrochlorothiazide may alter glucose tolerance and raise serum levels of cholesterol and triglycerides.
Hydrochlorothiazide reduces clearance of uric acid and may cause or exacerbate hyperuricemia and precipitate gout in susceptible patients.
Hydrochlorothiazide decreases urinary calcium excretion and may cause elevations of serum calcium. Monitor calcium levels.
5.000000000000000e+00 8 Renal Impairment
Patients with chronic kidney disease, severe heart failure, or volume depletion may be at increased risk for developing acute renal failure on drugs containing hydrochlorothiazide, including LOPRESSOR HCT.
5.000000000000000e+00 9 Peripheral Vascular Disease
Beta-blockers can precipitate or aggravate symptoms of arterial insufficiency in patients with peripheral vascular disease.
5.000000000000000e+00 10 Pheochromocytoma
If LOPRESSOR HCT is used in the setting of pheochromocytoma, it should be given in combination with an alpha blocker, and only after the alpha blocker has been initiated. Administration of beta-blockers alone in the setting of pheochromocytoma has been associated with a paradoxical increase in blood pressure due to the attenuation of beta-mediated vasodilatation in skeletal muscle.
5.000000000000000e+00 11 Thyrotoxicosis
Beta-adrenergic blockade may mask certain clinical signs of hyperthyroidism, such as tachycardia. Abrupt withdrawal of beta-blockade may precipitate a thyroid storm.
5.12 Anaphylactic Reaction
While taking beta-blockers, patients with a history of severe anaphylactic reactions to a variety of allergens may be more reactive to repeated challenge and may be unresponsive to the usual doses of epinephrine used to treat an allergic reaction.
5.1 3 Acute Myopia and Second Angle-Closure Glaucoma
Hydrochlorothiazide, a sulfonamide, can cause acute transient myopia and acute angle-closure glaucoma (idiosyncratic reactions). Symptoms include acute onset of decreased visual acuity or ocular pain and typically occur within hours to weeks of hydrochlorothiazide initiation. Risk factors for developing acute angle-closure glaucoma may include a history of sulfonamide or penicillin allergy.
Untreated acute angle-closure glaucoma can lead to permanent vision loss. Given that LOPRESSOR HCT contains hydrochlorothiazide, if these symptoms occur, discontinue LOPRESSOR HCT. Consider prompt medical or surgical treatment if the intraocular pressure remains uncontrolled.
5.1 4 Exacerbation of Systemic Lupus Erythematosus
Hydrochlorothiazide can exacerbate or activate systemic lupus erythematosus.
6 ADVERSE REACTIONS
The following adverse reactions are described in more detail elsewhere in the label;
6.2 Post-Marketing Experience
The following adverse reactions have been reported in postmarketing experience: adverse reactions have been identified during post approval use of LOPRESSOR HCT. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Metoprolol
Confusional state, an increase in blood triglycerides and a decrease in High Density Lipoprotein (HDL). Very rare reports of hepatitis, jaundice and non-specific hepatic dysfunction. Isolated cases of transaminase, alkaline phosphatase, and lactic dehydrogenase elevations have also been reported.
Hydrochlorothiazide
Digestive: Pancreatitis, jaundice (intrahepatic cholestatic), sialadenitis, vomiting, diarrhea, cramping, nausea, gastric irritation, constipation, anorexia.
Cardiovascular: Orthostatic hypotension (may be potentiated by alcohol, barbiturates, or narcotics).
Neurologic: Vertigo, dizziness, transient blurred vision, headache, paresthesia, xanthopsia, weakness, restlessness.
Musculoskeletal: Muscle spasm.
Hematologic: Aplastic anemia, agranulocytosis, leukopenia, thrombocytopenia.
Metabolic: Hyperglycemia, glycosuria, hyperuricemia.
Hypersensitive Reactions: Necrotizing angiitis, Stevens-Johnson syndrome, respiratory distress including pneumonitis and pulmonary edema, purpura, urticaria, rash, photosensitivity.
Other beta-adrenergic agent reactions
A variety of adverse reactions have been reported with other beta-adrenergic blocking agents and should be considered potential adverse reactions to Lopressor.
Central Nervous System: Reversible mental depression progressing to catatonia; visual disturbances; hallucinations; an acute reversible syndrome characterized by disorientation for time and place, emotional lability, clouded sensorium, and decreased performance on neuropsychometrics.
Hematologic: Agranulocytosis, nonthrombocytopenic purpura, thrombocytopenic purpura.
Hypersensitive Reactions: Laryngospasm and respiratory distress.
7 DRUG INTERACTIONS
- Catecholamine-depleting drugs (e.g., MAO inhibitors): Hypotension, bradycardia. (7.1 )
- CYP2D6 inhibitors: Increased metoprolol concentration. (12.3 )
- Digitalis glycosides, clonidine, diltiazem and verapamil: Bradycardia. (5.4 , 7.1 )
- Clonidine: Rebound hypertension following clonidine withdrawal. (7.1 )
- Antidiabetic drugs: Dosage adjustment may be required. (7.2 )
- Cholestyramine and colestipol: Reduced absorption of thiazides. (7.2 )
- Lithium: Risk of lithium toxicity. (7.2 )
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): Reduced diuretic, natriuretic, and antihypertensive effects of diuretics. (7.2 )
7.1 Drug Interactions with Metoprolol
Catecholamine Depleting Drugs:
The concomitant use of catecholamine-depleting drugs (e.g., reserpine, monoamine oxidase (MAO) inhibitors) with beta adrenergic blockers may have an additive affect and increase the risk of hypotension or bradycardia.
CYP2D6 Inhibitors:
Drugs that are strong inhibitors of CYP2D6 such as quinidine, fluoxetine, paroxetine, and propafenone were shown to double metoprolol concentrations. While there is no information about moderate or weak inhibitors, these too are likely to increase metoprolol concentration. Increases in plasma concentration decrease the cardioselectivity of metoprolol [see Clinical Pharmacology (12.3)] . Monitor patients closely when the combination cannot be avoided.
Digitalis, Clonidine, and Calcium Channel Blockers:
Digitalis glycosides, clonidine, diltiazem and verapamil slow atrioventricular conduction and decrease heart rate. Concomitant use with beta blockers can increase the risk of bradycardia.
If clonidine and a beta blocker, such as metoprolol are coadministered, withdraw the beta-blocker several days before the gradual withdrawal of clonidine because beta-blockers may exacerbate the rebound hypertension that can follow the withdrawal of clonidine. If replacing clonidine by beta-blocker therapy, delay the introduction of beta-blockers for several days after clonidine administration has stopped.
7.2 Drug Interactions with Hydrochlorothiazide
Antidiabetic drugs (oral agents and insulin) : Dosage adjustment of the antidiabetic drug may be required.
Ion exchange resins: Absorption of hydrochlorothiazide is impaired in the presence of anionic exchange resins. Single doses of either cholestyramine or colestipol resins bind the hydrochlorothiazide and reduce its absorption from the gastrointestinal tract by up to 85% and 43%, respectively. Stagger the dosage of hydrochlorothiazide and ion exchange resins (e.g., cholestyramine and colestipol resins) such that hydrochlorothiazide is administered at least 4 hours before or 4-6 hours after the administration of resins to minimize the interaction.
Lithium : Diuretics reduce the renal clearance of lithium and increase the risk of lithium toxicity. Monitor serum lithium concentrations during concurrent use.
Non-Steroidal Anti-Inflammatory Drugs : NSAIDs can reduce the diuretic, natriuretic, and antihypertensive effects of thiazide diuretics.
11 DESCRIPTION
Lopressor HCT has the antihypertensive effect of Lopressor ® , metoprolol tartrate, a beta adrenoreceptor blocker, and hydrochlorothiazide, a thiazide diruetic. It is available as tablets for oral administration. The 50/25 tablets contain 50 mg of metoprolol tartrate USP and 25 mg of hydrochlorothiazide USP; the 100/25 tablets contain 100 mg of metoprolol tartrate USP and 25 mg of hydrochlorothiazide USP; and the 100/50 tablets contain 100 mg of metoprolol tartrate USP and 50 mg of hydrochlorothiazide USP. Metoprolol tartrate USP is (±)-1-(Isopropylamino)-3-[ p -(2-methoxyethyl)phenoxy]-2-propanol L-(+)-tartrate (2:1) salt, and its structural formula is
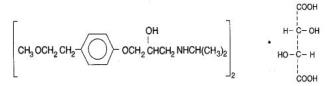
Metoprolol tartrate USP is a white, crystalline powder. It is very soluble in water; freely soluble in methylene chloride, in chloroform, and in alcohol; slightly soluble in acetone; and insoluble in ether. Its molecular weight is 684.82.
Hydrochlorothiazide is 6-chloro-3, 4-dihydro-2 H -1,2,4-benzothiadiazine-7- sulfonamide 1,1-dioxide, and its structural formula is
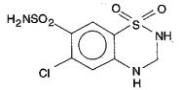
Hydrochlorothiazide USP is a white, or practically white, practically odorless, crystalline powder. It is freely soluble in sodium hydroxide solution, in n -butylamine, and in dimethylformamide; sparingly soluble in methanol; slightly soluble in water; and insoluble in ether, in chloroform, and in dilute mineral acids. Its molecular weight is 297.73.
Inactive Ingredients: microcrystalline cellulose , colloidal silicon dioxide, D&C Yellow No. 10 (100/50 mg tablets), FD&C Blue No. 1 (50/25 mg tablets), FD&C Red No. 80 and FD&C Yellow No. 6 and FD&C Yellow No. 5 (100/25 mg tablets), lactose monohydrate, magnesium stearate, povidone, sodium starch glycolate, sodium starch glycolate, stearic acid, and Confectioner's Sugar.
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Metoprolol is a beta 1 -selective (cardioselective) adrenergic receptor blocker. This preferential effect is not absolute however, and at higher plasma concentrations, metoprolol also inhibits beta2-adrenoreceptors, chiefly located in the bronchial and vascular musculature. Metoprolol has no intrinsic sympathomimetic activity, and membrane-stabilizing activity is detectable only at plasma concentrations much greater than required for beta-blockade. Animal and human experiments indicate that metoprolol slows the sinus rate and decreases AV nodal conduction.
The mechanism of the antihypertensive effects of beta-blocking agents has not been elucidated. However, several possible mechanisms have been proposed: (1) competitive antagonism of catecholamines at peripheral (especially cardiac) adrenergic neuron sites, leading to decreased cardiac output; (2) a central effect leading to reduced sympathetic outflow to the periphery; and (3) suppression of renin activity.
The mechanism of antihypertensive effect of thiazide diuretics is unknown.
12.2 Pharmacodynamics
Metoprolol
Clinical pharmacology studies have confirmed the beta-blocking activity of metoprolol in man, as shown by (1) reduction in heart rate and cardiac output at rest and upon exercise, (2) reduction of systolic blood pressure upon exercise, (3) inhibition of isoproterenol-induced tachycardia, and (4) reduction of reflex orthostatic tachycardia.
Significant beta-blocking effect (as measured by reduction of exercise heart rate) occurs within 1 hour after oral administration, and its duration is dose-related. For example, a 50% reduction of the maximum registered effect after single oral doses of 20, 50, and 100 mg occurred at 3.3, 5.0, and 6.4 hours, respectively, in normal subjects. After repeated oral dosages of 100 mg twice daily, a significant reduction in exercise systolic blood pressure was evident at 12 hours.
There is a linear relationship between the log of plasma levels and reduction of exercise heart rate. However, antihypertensive activity does not appear to be related to plasma levels. Because of variable plasma levels attained with a given dose and lack of a consistent relationship of antihypertensive activity to dose, selection of proper dosage requires individual titration.
The onset of action of thiazides occurs in 2 hours and the peak effect at about 4 hours. The action persists for approximately 6 to 12 hours.
12.3 Pharmacokinetics
Absorption
In man, absorption of metoprolol HCT is rapid and complete. Plasma levels following oral administration, however, approximate 50% of levels following intravenous administration, indicating about 50% first-pass metabolism.
Hydrochlorothiazide is rapidly absorbed, as indicated by peak plasma concentrations 1 to 2.5 hours after oral administration. Plasma levels of the drug are proportional to dose; the concentration in whole blood is 1.6 to 1.8 times higher than in plasma.
Thiazides affect the renal tubular mechanism of electrolyte reabsorption. At maximal therapeutic dosage, all thiazides are approximately equal in their diuretic potency. Thiazides increase excretion of sodium and chloride in approximately equivalent amounts. Natriuresis causes a secondary loss of potassium.
The mechanism of the antihypertensive effect of thiazides is unknown. Thiazides do not affect normal blood pressure.
Effect of Food
Gastrointestinal absorption of hydrochlorothiazide is enhanced when administered with food. Absorption is decreased in patients with congestive heart failure, and the pharmacokinetics are considerably different in these patients.
Distribution
Plasma levels achieved are highly variable after oral administration. Only a small fraction of the drug (about 12%) is bound to human serum albumin. Metoprolol is a racemic mixture of R- and S-enantiomers. Less than 5% of an oral dose of metoprolol is recovered unchanged in the urine; the rest is excreted by the kidneys as metabolites that appear to have no clinical significance. The systemic availability and half-life of metoprolol in patients with renal failure do not differ to a clinically significant degree from those in normal subjects. Consequently, no reduction in dosage is usually needed in patients with chronic renal failure.
Elimination
Thiazides are eliminated rapidly by the kidney. After oral administration of 25 mg to 100 mg doses, 72% to 97% of the dose is excreted in the urine, indicating dose-independent absorption. Hydrochlorothiazide is eliminated from plasma in a biphasic fashion with a terminal half-life of 10 to 17 hours. Plasma protein binding is 67.9%. Plasma clearance is 15.9 to 30.0 L/hr; volume of distribution is 3.6 to 7.8 L/kg.
Specific Populations:
Geriatric Patients
In elderly subjects with clinically normal renal function, there are no significant differences in metoprolol pharmacokinetics compared to young subjects.
Racial or Ethnic Groups
Metoprolol is extensively metabolized by the cytochrome P450 enzyme system in the liver. The oxidative metabolism of metoprolol is under genetic control with a major contribution of the polymorphic cytochrome P450 isoform 2D6 (CYP2D6). There are marked ethnic differences in the prevalence of the poor metabolizers (PM) phenotype. Approximately 7% of Caucasians and less than 1% Asian are poor metabolizers.
12.5 Pharmacogenomics
CYP2D6 is absent in about 8% of Caucasians (poor metabolizers) and about 2% of most other populations. CYP2D6 can be inhibited by several drugs. Poor metabolizers of CYP2D6 will have increased (several-fold) metoprolol blood levels, decreasing metoprolol's cardioselectivity.
13 NONCLINICAL TOXICOLOGY
Lopressor HCT:
Carcinogenicity and mutagenicity studies have not been conducted with Lopressor HCT. Lopressor HCT produced no evidence of impaired fertility in male or female rats administered gavaged doses up to 200/50 mg/kg (about 10 and 20 times the maximum recommended human dose (MRHD) of metoprolol and hydrochlorothiazide, respectively, on a mg/m 2 basis) prior to mating and throughout gestation and rearing of young.
Lopressor:
Long-term studies in animals have been conducted to evaluate carcinogenic potential. In a 2-year study in rats at three oral dosage levels of up to 800 mg/kg per day (41 times, on a mg/m 2 basis, the daily dose of 200 mg for a 60-kg patient), there was no increase in the development of spontaneously occurring benign or malignant neoplasms of any type. The only histologic changes that appeared to be drug related were an increased incidence of generally mild focal accumulation of foamy macrophages in pulmonary alveoli and a slight increase in biliary hyperplasia. In a 21-month study in Swiss albino mice at three oral dosage levels of up to 750 mg/kg per day (about 18 times, on a mg/m 2 basis, the daily dose of 200 mg for a 60-kg patient), benign lung tumors (small adenomas) occurred more frequently in female mice receiving the highest dose than in untreated control animals. There was no increase in malignant or total (benign plus malignant) lung tumors, or in the overall incidence of tumors or malignant tumors. This 21-month study was repeated in CD-1 mice, and no statistically or biologically significant differences were observed between treated and control mice of either sex for any type of tumor.
All mutagenicity tests performed (a dominant lethal study in mice, chromosome studies in somatic cells, a Salmonella /mammalian-microsome mutagenicity test, and a nucleus anomaly test in somatic interphase nuclei) were negative.
No evidence of impaired fertility due to Lopressor was observed in a study performed in rats at doses up to 22 times, on a mg/m 2 basis, the daily dose of 200 mg in a 60 kg patient.
Hydrochlorothiazide:
Two-year feeding studies in mice and rats uncovered no evidence of a carcinogenic potential of hydrochlorothiazide in female mice at doses up to approximately 600 mg/kg/day (about 120 times the MRHD of 25 mg/day on a mg/m 2 basis) or in male and female rats at doses up to approximately 100 mg/kg/day (about 40 times the MRHD on a mg/m 2 basis). However, there was equivocal evidence for hepatocarcinogenicity in male mice.
Hydrochlorothiazide was not genotoxic in the Ames bacterial mutagenicity testor the Chinese Hamster Ovary (CHO) test for chromosomal aberrations. Nor was it genotoxic in vivo assays using mouse germinal cell chromosomes, Chinese hamster bone marrow chromosomes, and the Drosophila sex-linked recessive lethal trait gene. Positive test results were obtained in the in vitro CHO Sister Chromatid Exchange (clastogenicity) and in the Mouse Lymphoma Cell (mutagenicity) assays, and in the Aspergillus nidulans nondisjunction assay at an unspecified concentration.
Hydrochlorothiazide had no adverse effects on the fertility of mice and rats of either sex in studies wherein these species were exposed, via their diet, to doses of up to 100 and 4 mg/kg/day (about 20 and 1.6 times the MRHD, on a mg/m 2 basis), respectively, prior to mating and throughout gestation.
16 HOW SUPPLIED/STORAGE AND HANDLING
Tablets 50/25 - capsule-shaped, white and mottled-blue, scored (imprinted LOPHCT on one side and 463 twice on the scored side), 50 mg of metoprolol tartrate and 25 mg of hydrochlorothiazide
Bottles of 100……………………………………NDC 30698-463- 01
Tablets 100/25 - capsule-shaped, white and mottled-pink, scored (imprinted LOPHCT on one side and 461 twice on the scored side), 100 mg of metoprolol tartrate and 25 mg of hydrochlorothiazide
Bottles of 100……………………………………NDC 30698-461-01
Tablets 100/50 - capsule- shaped, white and mottled-yellow, scored (imprinted LOPHCT on one side and 462 twice on the scored side), 100 mg of metoprolol tartrate and 50 mg of hydrochlorothiazide
Bottles of 100……………………………………NDC 30698-462-01
Store at 77ºF (25ºC); excursions permitted to 59º to 86ºF (15º to 30ºC) [See USP Controlled Room Temperature]. Protect from moisture.
Dispense in a tight, light-resistant container (USP).
12.1 Mechanism of Action
Metoprolol is a beta 1 -selective (cardioselective) adrenergic receptor blocker. This preferential effect is not absolute however, and at higher plasma concentrations, metoprolol also inhibits beta2-adrenoreceptors, chiefly located in the bronchial and vascular musculature. Metoprolol has no intrinsic sympathomimetic activity, and membrane-stabilizing activity is detectable only at plasma concentrations much greater than required for beta-blockade. Animal and human experiments indicate that metoprolol slows the sinus rate and decreases AV nodal conduction.
The mechanism of the antihypertensive effects of beta-blocking agents has not been elucidated. However, several possible mechanisms have been proposed: (1) competitive antagonism of catecholamines at peripheral (especially cardiac) adrenergic neuron sites, leading to decreased cardiac output; (2) a central effect leading to reduced sympathetic outflow to the periphery; and (3) suppression of renin activity.
The mechanism of antihypertensive effect of thiazide diuretics is unknown.