Get your patient on Nitrofurantion - Nitrofurantion capsule (Nitrofurantion)
Nitrofurantion - Nitrofurantion capsule prescribing information
INDICATIONS AND USAGE:
Nitrofurantoin Capsules, USP (macrocrystals) is specifically indicated for the treatment of urinary tract infections when due to susceptible strains of Escherichia coli, enterococci,
Staphylococcus aureus, and certain susceptible strains of Klebsiella and Enterobacter species.
Nitrofurantoin is not indicated for the treatment of pyelonephritis or perinephric abscesses.
To reduce the development of drug-resistant bacteria and maintain the effectiveness of Nitrofurantoin Capsules, USP (macrocrystals) and other antibacterial drugs, Nitrofurantoin Capsules, USP (macrocrystals) should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria.
When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
Nitrofurantoins lack the broader tissue distribution of other therapeutic agents approved for urinary tract infections. Consequently, many patients who are treated with Nitrofurantoin Capsules, USP (macrocrystals) are predisposed to persistence or reappearance of bacteriuria. Urine specimens for culture and susceptibility testing should be obtained before and after completion of therapy. If persistence or reappearance of bacteriuria occurs after treatment with Nitrofurantoin Capsules, USP (macrocrystals), other therapeutic agents with broader tissue distribution should be selected. In considering the use of Nitrofurantoin Capsules, USP (macrocrystals), lower eradication rates should be balanced against the increased potential for systemic toxicity and for the development of antimicrobial resistance when agents with broader tissue distribution are utilized.
CONTRAINDICATIONS:
Anuria, oliguria, or significant impairment of renal function (creatinine clearance under 60 mL per minute or clinically significant elevated serum creatinine) are contraindications. Treatment of this type of patient carries an increased risk of toxicity because of impaired excretion of the drug.
Because of the possibility of hemolytic anemia due to immature erythrocyte enzyme systems (glutathione instability), the drug is contraindicated in pregnant patients at term (38-42 weeks’gestation), during labor and delivery, or when the onset of labor is imminent. For the same reason, the drug is contraindicated in neonates under one month of age.
Nitrofurantoin Capsules, USP (macrocrystals) is contraindicated in patients with a previous history of cholestatic jaundice/hepatic dysfunction associated with nitrofurantoin.
Nitrofurantoin Capsules, USP (macrocrystals) is also contraindicated in those patients with known hypersensitivity to nitrofurantoin.
ADVERSE REACTIONS
Respiratory:
CHRONIC, SUBACUTE, OR ACUTE PULMONARY HYPERSENSITIVITY REACTIONS MAY OCCUR.
CHRONIC PULMONARY REACTIONS OCCUR GENERALLY IN PATIENTS WHO HAVE RECEIVED CONTINUOUS TREATMENT FOR SIX MONTHS OR LONGER. MALAISE, DYSPNEA ON EXERTION, COUGH, AND ALTERED PULMONARY FUNCTION ARE COMMON MANIFESTATIONS WHICH CAN OCCUR INSIDIOUSLY. RADIOLOGIC AND HISTOLOGIC FINDINGS OF DIFFUSE INTERSTITIAL PNEUMONITIS OR FIBROSIS, OR BOTH, ARE ALSO COMMON MANIFESTATIONS OF THE CHRONIC PULMONARY REACTION. FEVER IS RARELY PROMINENT.
THE SEVERITY OF CHRONIC PULMONARY REACTIONS AND THEIR DEGREE OF RESOLUTION APPEAR TO BE RELATED TO THE DURATION OF THERAPY AFTER THE FIRST CLINICAL SIGNS APPEAR. PULMONARY FUNCTION MAY BE IMPAIRED PERMANENTLY, EVEN AFTER CESSATION OF THERAPY. THE RISK IS GREATER WHEN CHRONIC PULMONARY REACTIONS ARE NOT RECOGNIZED EARLY.
In subacute pulmonary reactions, fever and eosinophilia occur less often than in the acute form. Upon cessation of therapy, recovery may require several months. If the symptoms are not recognized as being drug-related and nitrofurantoin therapy is not stopped, the symptoms may become more severe.
Acute pulmonary reactions are commonly manifested by fever, chills, cough, chest pain, dyspnea, pulmonary infiltration with consolidation or pleural effusion on x-ray, and eosinophilia. Acute reactions usually occur within the first week of treatment and are reversible with cessation of therapy. Resolution often is dramatic (see WARNINGS ).
Changes in EKG (e.g., non-specific ST/T wave changes, bundle branch block) have been reported in association with pulmonary reactions.
Cyanosis has been reported rarely.
Hepatic: Hepatic reactions, including hepatitis, cholestatic jaundice, chronic active hepatitis, and hepatic necrosis, occur rarely (see WARNINGS ).
Neurologic : Peripheral neuropathy, which may become severe or irreversible, has occurred. Fatalities have been reported. Conditions such as renal impairment (creatinine clearance under 60 mL per minute or clinically significant elevated serum creatinine), anemia, diabetes mellitus, electrolyte imbalance, vitamin B deficiency, and debilitating diseases may increase the possibility of peripheral neuropathy (see WARNINGS ).
Asthenia, vertigo, nystagmus, dizziness, headache, and drowsiness also have been reported with the use of nitrofurantoin.
Benign intracranial hypertension (pseudotumor cerebri), confusion, depression, optic neuritis, and psychotic reactions have been reported rarely. Bulging fontanels, as a sign of benign intracranial hypertension in infants, have been reported rarely.
Dermatologic: Exfoliative dermatitis and erythema multiforme (including Stevens-Johnson syndrome) have been reported rarely. Transient alopecia also has been reported.
Allergic: A lupus-like syndrome associated with pulmonary reactions to nitrofurantoin has been reported. Also, angioedema; maculopapular, erythematous, or eczematous eruptions; pruritus; urticaria; anaphylaxis; arthralgia; myalgia; drug fever; chills; and vasculitis (sometimes associated with pulmonary reactions) have been reported. Hypersensitivity reactions represent the most frequent spontaneously-reported adverse events in worldwide post-marketing experience with nitrofurantoin formulations.
Gastrointestinal: Nausea, emesis, and anorexia occur most often. Abdominal pain and diarrhea are less common gastrointestinal reactions. These dose-related reactions can be minimized by reduction of dosage. Sialadenitis and pancreatitis have been reported. There have been sporadic reports of pseudomembranous colitis with the use of nitrofurantoin. The onset of pseudomembranous colitis symptoms may occur during or after antimicrobial treatment (see WARNINGS ).
Hematologic: Cyanosis secondary to methemoglobinemia has been reported rarely.
Miscellaneous: As with other antimicrobial agents, superinfections caused by resistant organisms, e.g., Pseudomonas species or Candida species, can occur.
Laboratory Adverse Events: The following laboratory adverse events have been reported with the use of nitrofurantoin: increased AST (SGOT), increased ALT (SGPT), decreased hemoglobin, increased serum phosphorus, eosinophilia, glucose-6-phosphate dehydrogenase deficiency anemia (see WARNINGS ), agranulocytosis, leukopenia, granulocytopenia, hemolytic anemia, thrombocytopenia, megaloblastic anemia. In most cases, these hematologic abnormalities resolved following cessation of therapy. Aplastic anemia has been reported rarely.
Drug Interactions:
Antacids containing magnesium trisilicate, when administered concomitantly with nitrofurantoin, reduce both the rate and extent of absorption. The mechanism for this interaction probably is absorption of nitrofurantoin onto the surface of magnesium trisilicate.
Uricosuric drugs, such as probenecid and sulfinpyrazone, can inhibit renal tubular secretion of nitrofurantoin. The resulting increase in nitrofurantoin serum levels may increase toxicity, and the decreased urinary levels could lessen its efficacy as a urinary tract antibacterial.
DESCRIPTION
Nitrofurantoin macrocrystals, USP is a synthetic chemical of controlled crystal size. It is a stable, yellow, crystalline compound. Nitrofurantoin macrocrystals, USP is an antibacterial agent for specific urinary tract infections. It is available in 25 mg, 50 mg, and 100 mg capsules for oral administration.
It is chemically designated as 1-[[(5-nitro-2-furanyl)methylene] amino]-2,4-imidazolidinedione and has the following structural formula:
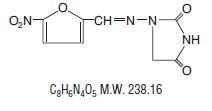
Each Nitrofurantoin Capsules, USP (macrocrystals) contains nitrofurantoin (macrocrystals) USP equivalent to 25 mg, 50 mg or 100 mg and the following inactive ingredients: lactose monohydrate, corn starch, talc, titanium dioxide, gelatin, sodium lauryl sulfate, shellac, propylene glycol, potassium hydroxide and black iron oxide. In addition 50 mg capsules contain FD&C Blue #1, red iron oxide and yellow iron oxide.
CLINICAL PHARMACOLOGY:
Nitrofurantoin macrocrystals are a larger crystal form of nitrofurantoin. The absorption of Nitrofurantoin macrocrystals is slower and its excretion somewhat less when compared to nitrofurantoin. Blood concentrations at therapeutic dosage are usually low. It is highly soluble in urine, to which it may impart a brown color.
Following a dose regimen of 100 mg q.i.d. for 7 days, average urinary drug recoveries (0-24 hours) on day 1 and day 7 were 37.9% and 35.0%.
Unlike many drugs, the presence of food or agents delaying gastric emptying can increase the bioavailability of Nitrofurantoin macrocrystals, presumably by allowing better dissolution in gastric juices.
MICROBIOLOGY
Nitrofurantoin is a nitrofuran antimicrobial agent with activity against certain Gram-positive and Gram-negative bacteria.
Mechanism of Action
The mechanism of the antimicrobial action of nitrofurantoin is unusual among antibacterials.
Nitrofurantoin is reduced by bacterial flavoproteins to reactive intermediates which inactivate or alter bacterial ribosomal proteins and other acromolecules. As a result of such inactivations, the vital biochemical processes of protein synthesis, aerobic energy metabolism, DNA synthesis, RNA synthesis, and cell wall synthesis are inhibited. Nitrofurantoin is bactericidal in urine at therapeutic doses. The broad-based nature of this mode of action may explain the lack of acquired bacterial resistance to nitrofurantoin, as the necessary multiple and simultaneous mutations of the target macromolecules would likely be lethal to the bacteria.
Interactions with Other Antibiotics
Antagonism has been demonstrated in vitro between nitrofurantoin and quinolone antimicrobials. The clinical significance of this finding is unknown.
Development of Resistance
Development of resistance to nitrofurantoin has not been a significant problem since its introduction in 1953. Cross-resistance with antibiotics and sulfonamides has not been observed, and transferable resistance is, at most, a very rare phenomenon.
Nitrofurantoin has been shown to be active against most strains of the following bacteria both in vitro and in clinical infections [see Indications and Usage ]:
Aerobic and facultative Gram-positive microorganisms:
Staphylococcus aureus
Enterococci (e.g. Enterococcus faecalis)
Aerobic and facultative Gram-negative microorganisms:
Escherichia coli
NOTE: While nitrofurantoin has excellent activity against Enterococcus faecalis, the majority of Enterococcus faecium isolates are not susceptible to nitorfurantoin.
At least 90 percent of the following microorganisms exhibit an in vitro minimum inhibitory concentration (MIC) less than or equal to the susceptible breakpoint for nitrofurantoin. However, the efficacy of nitrofurantoin in treating clinical infections due to these microorganisms has not been established in adequate and well-controlled trials.
Aerobic and facultative Gram-positive microorganisms:
Coagulase-negative staphylococci (including Staphylococcus epidermidis and Staphylococcus saprophyticus )
Streptococcus agalactiae
Group D streptococci
Viridans group streptococci
Aerobic and facultative Gram-negative microorganisms:
Citrobacter amalonaticus
Citrobacter diversus
Citrobacter freundii
Klebsiella oxytoca
Klebsiella ozaenae
NOTE: Some strains of Enterobacter species and Klebsiella species are resistant to nitrofurantoin.
Susceptibility Test Methods:
For specific information regarding susceptibility test interpretive criteria and associated test methods and quality control standards recognized by FDA for this drug, please see: https://www.fda.gov/STIC.
HOW SUPPLIED
Nitrofurantoin Capsules, USP (Macrocrystals), 25 mg are size “4” white opaque hard gelatin capsule, axially printed “231” in black ink on both cap and body containing cream to yellow colored powder available as follows:
- Bottles of 100 NDC 68001-384-00
Nitrofurantoin Capsules, USP (Macrocrystals), 50 mg are size “3” light brown hard gelatin capsule, axially printed “232” in black ink on both cap and body containing cream to yellow colored powder available as follows:
- Bottles of 100 NDC 68001-385-00
Nitrofurantoin Capsules, USP (Macrocrystals), 100 mg are size “2” grey opaque hard gelatin capsule, axially printed “233” in black ink on both cap and body containing cream to yellow colored powder available as follows:
- Bottles of 100 NDC 68001-386-00
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature].
Protect from light and moisture.
Dispense in a tight, light-resistant container as defined in the USP.
To report SUSPECTED ADVERSE REACTIONS, contact Sun Pharmaceutical Industries, Inc. at 1-800-406-7984 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Manufactured by:
Sidmak Laboratories (India) Pvt. Ltd.
Plot No. 20, Pharmacity, Selaqui Industrial Area,
Dehradun - 248 197
Uttarakhand, India
For BluePoint Laboratories
Iss.03/2019
M. L. No. 38/UA/2007
Mechanism of Action
The mechanism of the antimicrobial action of nitrofurantoin is unusual among antibacterials.
Nitrofurantoin is reduced by bacterial flavoproteins to reactive intermediates which inactivate or alter bacterial ribosomal proteins and other acromolecules. As a result of such inactivations, the vital biochemical processes of protein synthesis, aerobic energy metabolism, DNA synthesis, RNA synthesis, and cell wall synthesis are inhibited. Nitrofurantoin is bactericidal in urine at therapeutic doses. The broad-based nature of this mode of action may explain the lack of acquired bacterial resistance to nitrofurantoin, as the necessary multiple and simultaneous mutations of the target macromolecules would likely be lethal to the bacteria.
Interactions with Other Antibiotics
Antagonism has been demonstrated in vitro between nitrofurantoin and quinolone antimicrobials. The clinical significance of this finding is unknown.
Development of Resistance
Development of resistance to nitrofurantoin has not been a significant problem since its introduction in 1953. Cross-resistance with antibiotics and sulfonamides has not been observed, and transferable resistance is, at most, a very rare phenomenon.
Nitrofurantoin has been shown to be active against most strains of the following bacteria both in vitro and in clinical infections [see Indications and Usage ]:
Aerobic and facultative Gram-positive microorganisms:
Staphylococcus aureus
Enterococci (e.g. Enterococcus faecalis)
Aerobic and facultative Gram-negative microorganisms:
Escherichia coli
NOTE: While nitrofurantoin has excellent activity against Enterococcus faecalis, the majority of Enterococcus faecium isolates are not susceptible to nitorfurantoin.
At least 90 percent of the following microorganisms exhibit an in vitro minimum inhibitory concentration (MIC) less than or equal to the susceptible breakpoint for nitrofurantoin. However, the efficacy of nitrofurantoin in treating clinical infections due to these microorganisms has not been established in adequate and well-controlled trials.
Aerobic and facultative Gram-positive microorganisms:
Coagulase-negative staphylococci (including Staphylococcus epidermidis and Staphylococcus saprophyticus )
Streptococcus agalactiae
Group D streptococci
Viridans group streptococci
Aerobic and facultative Gram-negative microorganisms:
Citrobacter amalonaticus
Citrobacter diversus
Citrobacter freundii
Klebsiella oxytoca
Klebsiella ozaenae
NOTE: Some strains of Enterobacter species and Klebsiella species are resistant to nitrofurantoin.