Get your patient on Nityr - Nitisinone tablet (Nitisinone)
Nityr - Nitisinone tablet prescribing information
INDICATIONS AND USAGE
NITYR ® is indicated for the treatment of adult and pediatric patients with hereditary tyrosinemia type 1 (HT-1) in combination with dietary restriction of tyrosine and phenylalanine.
DOSAGE AND ADMINISTRATION
- The recommended starting dosage is 0.5 mg/kg (actual body weight) administered orally twice daily. (2.1 )
- Administer NITYR with or without food. (2.1 )
- Maintain dietary restriction of tyrosine and phenylalanine when administering NITYR. (2.1 )
- The recommended maintenance dosage of NITYR in patients 5 years of age and older who have undetectable serum and urine succinylacetone concentrations after a minimum of 4 weeks on a stable dosage of nitisinone, is 1 to 2 mg/kg once daily. (2.1 )
- See the full prescribing information for dosage titration and monitoring. (2.2 )
- See the full prescribing information for preparation and administration instructions. (2.2 )
Recommended Dosage
The recommended starting dosage of NITYR is 0.5 mg/kg (actual body weight) administered orally twice daily. Titrate the dose in each individual patient based on biochemical and/or clinical response.
Administer NITYR with or without food [see Clinical Pharmacology (12.3 )] .
Maintain dietary restriction of tyrosine and phenylalanine when administering NITYR.
Maintenance Dosage
The recommended maintenance dosage of NITYR in patients 5 years of age and older who have undetectable serum and urine succinylacetone concentrations after a minimum of 4 weeks on a stable dosage of nitisinone, is 1 to 2 mg/kg once daily [see Clinical Pharmacology (12.2 )] .
A maximum total daily dosage of 2 mg/kg may be needed based on the evaluation of all biochemical parameters.
Missed Dose
If a dose of NITYR is missed, do not administer two doses at once to make up for a missed dose. Take the next dose at the scheduled time.
2.2 Dosage Titration and Monitoring
Monitor plasma and/or urine succinylacetone concentrations, liver function parameters and alpha-fetoprotein levels.
Monitor all biochemical parameters more closely (i.e. plasma and/or urine succinylacetone, urine 5-aminolevulinate (ALA), and erythrocyte porphobilinogen (PBG)-synthase activity during initiation of therapy, when switching from twice daily to once daily dosing, or if there is a deterioration in the patient’s condition.
If succinylacetone is still detectable in blood or urine 4 weeks after the start of nitisinone treatment, increase the NITYR dosage to 0.75 mg/kg twice daily. If the biochemical response is satisfactory (undetectable blood and/or urine succinylacetone), the dosage should be adjusted only according to body weight gain and not according to plasma tyrosine levels.
Maintain plasma tyrosine levels below 500 micromol/L by dietary restriction of tyrosine and phenylalanine intake [see Warnings and Precautions (5.1 )] . In patients who develop plasma tyrosine levels above 500 micromol/L, assess dietary tyrosine and phenylalanine intake. Do not adjust the NITYR dosage in order to lower the plasma tyrosine concentration.
Preparation and Administration Instructions
For patients who have difficulty swallowing intact tablets, disintegrate NITYR in water and administer using an oral syringe. For patients who can swallow semi-solid foods, NITYR tablets can be crushed and mixed with applesauce.
Administration of NITYR with other liquids or foods has not been studied and is not recommended.
Preparation and Administration of NITYR with Water in an Oral Syringe: Do not prepare more than two tablets at once within the same oral syringe.
If patient’s dosage requires more than two tablets, follow the steps below using multiple oral syringes and prescribed number of tablets to achieve the required dose.
One Tablet
1. Remove the plunger from the 5-mL oral syringe and insert a single, intact tablet.
2. Replace the plunger and draw up 2.6 mL of room temperature water.
3. Cap the oral syringe and leave the oral syringe for at least the length of time below: • 15 minutes for a 2 mg tablet • 60 minutes for a 5 mg or 10 mg tablet
4. Turn the oral syringe up and down for at least 30 seconds to suspend the material.
5. Inspect the syringe to ensure the tablet has fully disintegrated. If the tablet is not fully disintegrated, leave the oral syringe for an additional 10 minutes. Do not administer unless the tablet has fully disintegrated. Before administration of the suspension, turn the oral syringe up and down for 30 seconds to ensure the particles are suspended.
6. Uncap the oral syringe and administer all the suspension into the patient's mouth. To facilitate full administration, avoid depressing the plunger to the end of the oral syringe and leave a gap between the plunger and the oral syringe.
7. Fill the oral syringe by drawing up 2 mL of water. Shake well and administer while this time fully depressing the plunger. If particles are still present in the syringe, repeat this step.
Two Tablets
1. Remove the plunger from the 5-mL oral syringe and insert two intact tablets.
2. Replace the plunger and draw up 5 mL of room temperature water.
3. Cap the oral syringe and leave it for at least the length of time below: • 15 minutes for 2 mg tablets • 60 minutes for 5 mg or 10 mg tablets
4. Turn the oral syringe up and down for at least 30 seconds to suspend the material.
5. Inspect the syringe to ensure the tablets have fully disintegrated. If the tablet is not fully disintegrated, leave the oral syringe for an additional 10 minutes. Do not administer unless the tablet has fully disintegrated. Before administration of the suspension, turn the oral syringe up and down for 30 seconds to ensure the particles are suspended.
6. Uncap the oral syringe and administer all the suspension into the patient's mouth. To facilitate full administration, avoid depressing the plunger to the end of the oral syringe and leave a gap between the plunger and the oral syringe.
7. Fill the oral syringe by drawing up 2 mL of water. Shake well and administer while this time fully depressing the plunger. If particles are still present in the syringe, repeat this step.
Storage Instructions for the NITYR with water in an Oral Syringe
The suspension can be stored at room temperature in the capped oral syringe, protected from direct sunlight for up to 24 hours after adding water to the tablets. Discard after 24 hours.
Preparation and Administration of NITYR Mixed in Applesauce For patients who can swallow semi-solid food, NITYR can be crushed and mixed with applesauce.
1. Measure approximately one teaspoon of applesauce and transfer it into a clean container (e.g., clean glass).
2. Crush only 1 tablet at a time between two teaspoons forming a fine powder. Repeat this step if more than 1 tablet is needed.
3. Transfer the powder to the applesauce container ensuring all the powder is transferred and no powder residue remains on the teaspoon.
4. Mix the powder into the applesauce until the powder is well dispersed.
5. Administer the entire NITYR-applesauce mixture to the patient immediately or within 2 hours of mixing.
6. To ensure that there is not any remaining NITYR-applesauce mixture, add approximately one teaspoon of applesauce to the same container and administer to the patient.
Storage Instructions for NITYR Mixed in Apple Sauce
The mixture can be stored at room temperature, out of direct sunlight, for up to 2 hours after adding the crushed tablets to the applesauce. Discard after 2 hours.
DOSAGE FORMS AND STRENGTHS
Tablets: 2 mg, 5 mg, and 10 mg white to beige, round, flat tablets, which may display light yellow to brown speckles, debossed with “L” on one side and the strength (“2” mg, “5” mg, or “10” mg), on the other side.
USE IN SPECIFIC POPULATIONS
Pregnancy
Risk Summary Limited available data with nitisinone use in pregnant women are not sufficient to determine a drug-associated risk of adverse developmental outcomes. Animal reproduction studies have been conducted for nitisinone. In these studies, nitisinone was administered to mice and rabbits during organogenesis with oral doses of nitisinone up to 20 and 8-times respectively, the recommended initial dose of 1 mg/kg/day. In mice, nitisinone caused incomplete skeletal ossification of fetal bones and decreased pup survival at doses 0.4 times the recommended initial dose, and increased gestational length at doses 4 times the recommended initial dose. In rabbits, nitisinone caused maternal toxicity and incomplete skeletal ossification of fetal bones at doses 1.6 times the recommended initial dose ( see Data ) .
The background risk of major birth defects and miscarriage for the indicated population are unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
Data Animal Data
Reproduction studies have been performed in mice at oral doses of about 0.4, 4 and 20 times the recommended initial dose (1 mg/kg/day) and in rabbits at oral doses of about 1.6, 4 and 8 times the recommended initial dose based on the body surface area. In mice, nitisinone has been shown to cause incomplete skeletal ossification of fetal bones at 0.4, 4 and 20 times the recommended initial dose, increased gestational length at 4 and 20 times the recommended initial dose, and decreased pup survival at 0.4 times the recommended initial dose based on the body surface area. In rabbits, nitisinone caused incomplete skeletal ossification of fetal bones at 1.6, 4 and 8 times the recommended initial dose based on the body surface area.
Lactation
Risk Summary There are no data on the presence of nitisinone in human milk, the effects on the breastfed infant, or the effects on milk production. Data suggest that nitisinone is present in rat milk due to findings of ocular toxicity and lower body weight seen in drug naive nursing rat pups. The development and health benefits of breastfeeding should be considered along with the mother’s clinical need for NITYR and any potential adverse effects on the breastfed infant from NITYR or from the underlying maternal condition.
Pediatric Use
The safety and effectiveness of nitisinone have been established for the treatment of HT-1 in combination with dietary restriction of tyrosine and phenylalanine in pediatric patients. Use of NITYR for this indication is supported by evidence from one open-label, uncontrolled clinical study conducted with another oral formulation of nitisinone in 207 patients with HT-1 ages 0 to 22 years (median age 9 months) [see Clinical Studies (14 )] .
Geriatric Use
Clinical studies of nitisinone did not include any subjects aged 65 and over to determine whether they respond differently from younger subjects. No pharmacokinetic studies of nitisinone have been performed in geriatric patients. In general, dose selection for an elderly patient should be cautious reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy in this patient population.
CONTRAINDICATIONS
None.
WARNINGS AND PRECAUTIONS
Ocular Symptoms, Developmental Delay and Hyperkeratotic Plaques Due To Elevated Plasma Tyrosine Levels: Inadequate restriction of tyrosine and phenylalanine intake can lead to elevations in plasma tyrosine and levels above 500 micromol/L may lead to ocular signs and symptoms, intellectual disability and developmental delay, or painful hyperkeratotic plaques on the soles and palms. (5.1 )
- Do not adjust NITYR dosage in order to lower the plasma tyrosine concentration. (5.1 )
- Obtain slit-lamp examination prior to treatment and regularly thereafter. Reexamine patients if symptoms develop or tyrosine levels are > 500 micromol/L. Assess plasma tyrosine levels in patients with an abrupt change in neurologic status. (5.1 )
Leukopenia and Severe Thrombocytopenia: Monitor platelet and white blood cell counts. (5.2 )
5.1 Ocular Symptoms, Developmental Delay and Hyperkeratotic Plaques Due To Elevated Plasma Tyrosine Levels
Treatment with NITYR may cause elevated plasma tyrosine levels in patients with HT-1. Inadequate restriction of tyrosine and phenylalanine intake can lead to elevations in plasma tyrosine levels and levels greater than 500 micromol/L may lead to the following:
- Ocular signs and symptoms including corneal ulcers, corneal opacities, keratitis, conjunctivitis, eye pain, and photophobia. All of which have been reported in patients treated with nitisinone [see Adverse Reactions (6.1 )] . In a clinical study in a non HT-1 population without dietary restriction and reported tyrosine levels > 500 micromol/L both symptomatic and asymptomatic keratopathies have been observed. Therefore, perform a baseline ophthalmologic examination including slit-lamp examination prior to initiating NITYR treatment and regularly thereafter. Patients who develop photophobia, eye pain, or signs of inflammation such as redness, swelling, or burning of the eyes or tyrosine levels are > 500 micromol/L during treatment with NITYR should undergo slit-lamp reexamination and immediate measurement of the plasma tyrosine concentration.
- Variable degrees of intellectual disability and developmental delay. In patients treated with NITYR who exhibit an abrupt change in neurologic status, perform a clinical laboratory assessment including plasma tyrosine levels.
- Painful hyperkeratotic plaques on the soles and palms.
Maintain concomitant reduction in dietary tyrosine and phenylalanine while on NITYR treatment. In patients with HT-1 who are treated with NITYR and dietary restriction and develop elevated plasma tyrosine levels, assess dietary tyrosine and phenylalanine intake. Do not adjust NITYR dosage in order to lower the plasma tyrosine concentration. Maintain plasma tyrosine levels below 500 micromol/L.
5.2 Leukopenia and Severe Thrombocytopenia
In clinical trials, patients treated with another oral formulation of nitisinone and dietary restriction developed reversible leukopenia (3%), thrombocytopenia (3%), or both (1.5%) [see Adverse Reactions (6.1 )] . No patients developed infections or bleeding as a result of the episodes of leukopenia and thrombocytopenia. Monitor platelet and white blood cell counts during NITYR therapy.
ADVERSE REACTIONS
Most common adverse reactions (>1%) are elevated tyrosine levels, thrombocytopenia, leukopenia, conjunctivitis, corneal opacity, keratitis, photophobia, eye pain, blepharitis, cataracts, granulocytopenia, epistaxis, pruritus, exfoliative dermatitis, dry skin, maculopapular rash and alopecia. (6.1 )
To report SUSPECTED ADVERSE REACTIONS, contact Cycle Pharmaceuticals Ltd. at 1-855-831-5413 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Serious and or clinically significant adverse reactions described elsewhere in labeling include:
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The safety of NITYR has been established based on studies of another oral formulation of nitisinone in patients with HT-1 [see Clinical Studies (14 )] . Below is a display of the adverse reactions of nitisinone in these studies.
Nitisinone was studied in one open-label, uncontrolled study of 207 patients with HT-1, ages 0 to 22 years at enrollment (median age 9 months), who were diagnosed with HT-1 by the presence of succinylacetone in the urine or plasma. The starting dose of nitisinone was 0.3 to 0.5 mg/kg twice daily, and the dose was increased in some patients to 1 mg/kg twice daily based on weight, biochemical, and enzyme markers. The recommended starting dosage of NITYR is 0.5 mg/kg twice daily [see Dosage and Administration (2.1 ) ]. Median duration of treatment was 22 months (range 0.1 to 80 months).
The most serious adverse reactions reported during nitisinone treatment were thrombocytopenia, leukopenia, porphyria, and ocular/visual complaints associated with elevated tyrosine levels [see Warnings and Precautions (5.1 , 5.2 )] . Fourteen patients experienced ocular/visual events. The duration of the symptoms varied from 5 days to 2 years. Six patients had thrombocytopenia, three of which had platelet counts 30,000/microL or lower. In 4 patients with thrombocytopenia, platelet counts gradually returned to normal (duration up to 47 days) without change in the nitisinone dose. No patients developed infections or bleeding as a result of the episodes of leukopenia and thrombocytopenia.
Patients with HT-1 are at increased risk of developing porphyric crises, hepatic neoplasms, and liver failure requiring liver transplantation. These complications of HT-1 were observed in patients treated with nitisinone for a median of 22 months during the clinical trial (liver transplantation 13%, liver failure 7%, malignant hepatic neoplasms 5%, benign hepatic neoplasms 3%, porphyria 1%).
The most common adverse reactions reported in the clinical trial are summarized in TABLE 1.
| •reported in at least 1% of patients; •• another oral formulation of nitisinone | |
| TABLE 1 Most Common Adverse Reactions • in Patients with HT-1 Treated with Nitisinone •• | |
| Elevated tyrosine levels | >10% |
| Leukopenia | 3% |
| Thrombocytopenia | 3% |
| Conjunctivitis | 2% |
| Corneal Opacity | 2% |
| Keratitis | 2% |
| Photophobia | 2% |
| Eye Pain | 1% |
| Blepharitis | 1% |
| Cataracts | 1% |
| Granulocytopenia | 1% |
| Epistaxis | 1% |
| Pruritus | 1% |
| Exfoliative Dermatitis | 1% |
| Dry Skin | 1% |
| Maculopapular Rash | 1% |
| Alopecia | 1% |
Adverse reactions reported in less than 1% of the patients, included death, seizure, brain tumor, encephalopathy, hyperkinesia, cyanosis, abdominal pain, diarrhea, enanthema, gastrointestinal hemorrhage, melena, elevated hepatic enzymes, liver enlargement, hypoglycemia, septicemia, and bronchitis.
DRUG INTERACTIONS
CYP2C9 Substrates : Increased systemic exposure of these co-administered drugs; reduce the dosage. Additional dosage adjustments may be needed to maintain therapeutic drug concentrations for narrow therapeutic index drugs. (7 ) OAT1/OAT3 Substrates : Increased systemic exposure of these co-administered drugs; monitor for potential adverse reactions. (7 )
Nitisinone is a moderate CYP2C9 inhibitor, a weak CYP2E1 inducer and an inhibitor of OAT1/OAT3. TABLE 2 includes drugs with clinically significant drug interactions when administered concomitantly with NITYR and instructions for preventing or managing them.
TABLE 2. Clinically Significant Interactions Affecting Co-Administered Drugs
Sensitive CYP2C9 Substrates (e.g., celecoxib, tolbutamide) or CYP2C9 Substrates with a Narrow Therapeutic Index (e.g., phenytoin, warfarin) | |
Clinical Impact | Increased exposure of the co-administered drugs metabolized by CYP2C9. [see Clinical Pharmacology (12.3 )] |
Prevention or Management | Reduce the dosage of the co-administered drugs metabolized by CYP2C9 drug by half. Additional dosage adjustments may be needed to maintain therapeutic drug concentrations for narrow therapeutic index drugs. See prescribing information for those drugs. |
OAT1/OAT3 Substrates (e.g., adefovir, ganciclovir, methotrexate) | |
Clinical Impact | Increased exposure of the interacting drug. [see Clinical Pharmacology (12.3 )] |
Prevention or Management | Monitor for potential adverse reactions related to the co-administered drug. |
DESCRIPTION
NITYR (nitisinone) is a hydroxyphenyl-pyruvate dioxygenase inhibitor.
Nitisinone occurs as a white to yellowish-white, crystalline powder. It is practically insoluble in water, soluble in 2M sodium hydroxide and in methanol, and sparingly soluble in alcohol.
The chemical name of nitisinone is 2-(2-nitro-4-trifluoromethylbenzoyl) cyclohexane-1,3-dione. The empirical formula is C 14 H 10 F 3 NO 5 and the molecular weight is 329.23. The structural formula is:
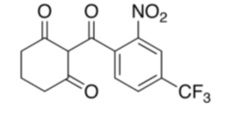
Each NITYR (nitisinone) tablet contains 2, 5 or 10 mg of nitisinone. Inactive ingredients are: glyceryl dibehenate, and lactose monohydrate. NITYR tablets are intended for oral administration.
CLINICAL PHARMACOLOGY
Mechanism of Action
Nitisinone is a competitive inhibitor of 4-hydroxyphenyl-pyruvate dioxygenase, an enzyme upstream of fumarylacetoacetate hydrolase (FAH) in the tyrosine catabolic pathway. By inhibiting the normal catabolism of tyrosine in patients with HT-1, nitisinone prevents the accumulation of the catabolic intermediates maleylacetoacetate and fumarylacetoacetate. In patients with HT-1, these catabolic intermediates are converted to the toxic metabolites succinylacetone and succinylacetoacetate, which are responsible for the observed liver and kidney toxicity. Succinylacetone can also inhibit the porphyrin synthesis pathway leading to the accumulation of 5-aminolevulinate, a neurotoxin responsible for the porphyric crises characteristic of HT-1.
12.2 Pharmacodynamics
In a clinical study, patients with HT-1 were diagnosed by the presence of succinylacetone in urine or plasma and treated with another oral formulation of nitisinone [see Clinical Studies (14 )]. In all 186 patients whose urine succinylacetone was measured, the urinary succinylacetone concentration decreased to less than 1 mmol/mol creatinine, the lower limit of quantitation. The median time to normalization of urine succinylacetone was 0.3 months. The probability of recurrence of abnormal values of urine succinylacetone was 1% at a nitisinone concentration of 37 micromol/L (95% confidence interval: 23, 51 micromol/L). In 87% (150/172) of patients whose plasma succinylacetone was measured, the plasma succinylacetone concentration decreased to less than 0.1 micromol/L, the lower limit of quantitation. The median time to normalization of plasma succinylacetone was 3.9 months.
In another study, comparing two dosing regimens of another oral formulation of nitisinone, succinylacetone was measured in urine and/or blood in 16 patients with HT-1 aged 5 years to 24 years. All study patients were on a stable nitisinone daily dosage (0.4 mg/kg/day to 1 mg/kg/day) during both study dosing regimens. After at least 4 weeks of twice daily dosing with nitisinone, both the urine and/or blood succinylacetone concentrations were below the limit of quantitation for the assay. Patients were then switched to once daily dosing with the same total daily dosage of nitisinone and blood and/or urine succinylacetone concentrations remained undetectable when measured following at least 4 weeks of treatment with once daily dosing.
Nitisinone inhibits catabolism of the amino acid tyrosine and can result in elevated plasma levels of tyrosine. Therefore, treatment with nitisinone requires restriction of the dietary intake of tyrosine and phenylalanine to prevent the toxicity associated with elevated plasma levels of tyrosine [see Warnings and Precautions (5.1 )] .
Pharmacokinetics
The single-dose pharmacokinetics of nitisinone have been studied for NITYR tablets in healthy adult subjects.
Absorption The pharmacokinetic characteristics following single oral administration of 10 mg NITYR under fasting conditions are shown in TABLE 3.
TABLE 3. Geometric Mean Pharmacokinetic Parameters in Healthy Subjects Following a Single Oral 10 mg Dose of NITYR Under Fasting Conditions
| Treatment | C max (ng/mL) [range] | T max • (h) [range] | AUC 0-120h (ng•h/mL) [range] |
|---|---|---|---|
• presented as median [range] | |||
| Single 10 mg NITYR Tablet fasted (n=23) | 1278 [780 to 1649] | 3.5 [1.0 to 4.0] | 77874 [42335 to 104211] |
Effect of Food: In a food effect study, a high-fat and high-calorie breakfast (973.6 cal distributed in carbohydrate 250.1 cal, proteins 157 cal, fat 566.5 cal) did not significantly affect the total exposure (AUC 0-120h ) and C max of nitisinone following single oral administration of 10 mg NITYR. The median T max was delayed to 6 hours under fed conditions [see Dosage and Administration (2.2 )].
Distribution In vitro binding of nitisinone to human plasma proteins is greater than 95% at 50 micromolar concentration. For NITYR, the arithmetic mean (SD) apparent volume of distribution of nitisinone is 8.2 (1.6) L in healthy subjects (n=23).
Elimination For NITYR, the arithmetic mean (SD) terminal half-life of nitisinone is 59.3 (8.9) hours in healthy subjects (n=23).
Metabolism: In vitro studies have shown that nitisinone is relatively stable in human liver microsomes with minor metabolism possibly mediated by CYP3A4 enzyme.
Excretion: Renal elimination of nitisinone is of minor importance, since the mean of the fraction of dose excreted as unchanged nitisinone in the urine (fe(%)) was 3.0% (n=3) following multiple oral doses of 80 mg daily in healthy subjects. The estimated mean (CV%) renal clearance of nitisinone was 0.003 L/h (25%).
Drug Interaction Studies Nitisinone does not inhibit CYP2D6. Nitisinone is a moderate inhibitor of CYP2C9, and a weak inducer of CYP2E1 (TABLE 4). Nitisinone is an inhibitor of OAT1/3 (TABLE 4).
TABLE 4. Percent Change in AUC0-∞ and Cmax for Co-administered Drugs in the Presence of Nitisinone in 18 Healthy Subjects
Co-administered Drug a | Dose of Co-administered Drug (Route of Administration) | Effect of Nitisinone on the Pharmacokinetics of Co-administered Drug b | |
AUC 0-∞ | C max | ||
CYP2C9 Substrate Tolbutamide c | 500 mg (oral) | 131%↑ | 16%↑ |
CYP2E1 Substrate Chlorzoxazone | 250 mg (oral) | 27%↓ | 18%↓ |
OAT1/3 Substrate Furosemide | 20 mg (intravenous) | 72%↑ | 12%↑ |
↑= Increased; ↓= Decreased
a The interacting drug was administered alone on Day 1 and together with nitisinone on Day 17. b Multiple doses of 80 mg nitisinone were administered daily alone from Day 3 to Day 16. c 16 subjects in Period 2 received nitisinone and tolbutamide while 18 subjects in Period 1 received nitisinone alone.
In Vitro Studies Where Drug Interaction Potential Was Not Further Evaluated Clinically
In vitro studies showed that nitisinone does not inhibit CYP1A2, 2C19, or 3A4. Nitisinone does not induce CYP1A2, 2B6 or 3A4/5. Nitisinone does not inhibit P-gp, BCRP, OATP1B1, OATP1B3 and OCT2-mediated transports at therapeutically relevant concentrations.
NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, Impairment of Fertility
The carcinogenic potential of nitisinone was assessed in a 26-week oral (gavage) carcinogenicity study in Tg.rasH2 mice. There were no drug-related neoplastic findings in male or female Tg.rasH2 mice at doses up to 100 mg/kg/ day nitisinone (approximately 8.1 times the recommended initial dose of 1 mg/kg/day on a body surface area basis).
Nitisinone was not genotoxic in the Ames test and the in vivo mouse liver unscheduled DNA synthesis (UDS) test. Nitisinone was mutagenic in the mouse lymphoma cell (L5178Y/TK+/-) forward mutation test and in an in vivo mouse bone marrow micronucleus test.
In a single dose-group study in rats given 100 mg/kg (16.2 times the recommended initial dose of 1 mg/kg/day on a body surface area basis), reduced litter size, decreased pup weight at birth, and decreased survival of pups after birth was demonstrated.
CLINICAL STUDIES
The safety and efficacy of NITYR have been established based on studies of another oral formulation of nitisinone in patients with HT-1. Below is a display of the results of these studies.
The efficacy and safety of nitisinone in patients with HT-1 was evaluated in one open-label, uncontrolled study of 207 patients with HT-1, ages 0 to 22 years at enrollment (median age 9 months). Patients were diagnosed with HT-1 by the presence of succinylacetone in the urine or plasma. All patients were treated with nitisinone at a starting dose of 0.3 to 0.5 mg/kg orally twice daily, and the dose was increased in some patients to 1 mg/kg twice daily based on weight, liver and kidney function tests, platelet count, serum amino acids, urinary phenolic acid, plasma and urine succinylacetone, erythrocyte PBG- synthase, and urine 5-ALA. The median duration of treatment was 22 months (range less than 1 month to 80 months). Efficacy was assessed by comparison of survival and incidence of liver transplant to historical controls.
For patients presenting with HT-1 younger than 2 months of age who were treated with dietary restriction and nitisinone, 2- and 4-year survival probabilities were 88% and 88%, respectively. Data from historical controls showed that patients presenting with HT-1 younger than 2 months of age treated with dietary restriction alone had 2- and 4-year survival probabilities of 29% and 29%, respectively. For patients presenting between 2 months and 6 months of age who were treated with dietary restrictions and nitisinone, 2-and 4-year survival probabilities were 94% and 94%, respectively. Data for historical controls showed that patients presenting with HT-1 between 2 months and 6 months of age treated with dietary restriction alone had 2-and 4-year survival probabilities of 74% and 60%, respectively.
The effects of nitisinone on urine and plasma succinylacetone, porphyrin metabolism, and urinary alpha-1-microglobulin were also assessed in this clinical study.
Porphyria-like crisis were reported in 3 patients (0.3% of cases per year) during the clinical study. This compares to an incidence of 5 to 20% of cases per year expected as part of the natural history of the disorder. An assessment of porphyria-like crises was performed because these events are commonly reported in patients with HT-1 who are not treated with nitisinone.
Urinary alpha-1-microglobulin, a proposed marker of proximal tubular dysfunction, was measured in 100 patients at baseline. The overall median pretreatment level was 4.3 grams/mol creatinine. After one year of treatment in a subgroup of patients (N=100), overall median alpha-1-microglobulin decreased by 1.5 grams/mol creatinine. In patients 24 months of age and younger in whom multiple values were available (N=65), median alpha-1-microglobulin levels decreased from 5 to 3 grams/mol creatinine (reference value for age less than or equal to 12 grams/mol creatinine). In patients older than 24 months in whom multiple values were available (N=35), median alpha-1-microglobulin levels decreased from 2.8 to 2 grams/mol creatinine (reference for age less than or equal to 6 grams/mol creatinine).
HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
NITYR (nitisinone) tablet is white to beige, round, flat which may display light yellow to brown speckles, debossed with the “strength” in mg on one side and “L” on the other side. Each tablet contains 2, 5 or 10 mg nitisinone.
NITYR is supplied in a high-density polyethylene (HDPE) square bottle with a child-resistant tamper-evident polypropylene (PP) screw cap. Each bottle contains 60 tablets.
2 mg tablets: NDC 70709-002-60
5 mg tablets: NDC 70709-005-60
10 mg tablets: NDC 70709-000-60
Storage and Handling
Store NITYR tablets at room temperature between 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C and 30°C (59°F and 86°F) [see USP Controlled Room Temperature].
Pharmacist: Dispense in tight and light resistant container as defined in USP. Dispense 5-mL oral syringe with a cap to use for preparation.
Mechanism of Action
Nitisinone is a competitive inhibitor of 4-hydroxyphenyl-pyruvate dioxygenase, an enzyme upstream of fumarylacetoacetate hydrolase (FAH) in the tyrosine catabolic pathway. By inhibiting the normal catabolism of tyrosine in patients with HT-1, nitisinone prevents the accumulation of the catabolic intermediates maleylacetoacetate and fumarylacetoacetate. In patients with HT-1, these catabolic intermediates are converted to the toxic metabolites succinylacetone and succinylacetoacetate, which are responsible for the observed liver and kidney toxicity. Succinylacetone can also inhibit the porphyrin synthesis pathway leading to the accumulation of 5-aminolevulinate, a neurotoxin responsible for the porphyric crises characteristic of HT-1.