Get your patient on Theophylline anhydrous - Theophylline tablet, Extended Release (Theophylline)
Theophylline anhydrous - Theophylline tablet, Extended Release prescribing information
INDICATIONS AND USAGE
Theophylline is indicated for the treatment of the symptoms and reversible airflow obstruction associated with chronic asthma and other chronic lung diseases, e.g., emphysema and chronic bronchitis.
DOSAGE AND ADMINISTRATION
Theophylline (anhydrous) extended-release tablets 400 mg can be taken once a day in the morning or evening. It is recommended that theophylline (anhydrous) extended-release tablets be taken with meals. Patients should be advised that if they choose to take theophylline (anhydrous) extended-release tablets with food it should be taken consistently with food and if they take it in a fasted condition it should routinely be taken fasted. It is important that the product whenever dosed be dosed consistently with or without food.
Theophylline (anhydrous) extended-release tablets are not to be chewed or crushed because it may lead to a rapid release of theophylline with the potential for toxicity. The scored tablet may be split. Infrequently, patients receiving theophylline (anhydrous) extended-release tablets 400 mg may pass an intact matrix tablet in the stool or via colostomy. These matrix tablets usually contain little or no residual theophylline.
Stabilized patients, 12 years of age or older, who are taking an immediate-release or controlled-release theophylline product may be transferred to once-daily administration of 400 mg theophylline (anhydrous) extended-release tablets on a mg-for-mg basis.
It must be recognized that the peak and trough serum theophylline levels produced by the once-daily dosing may vary from those produced by the previous product and/or regimen.
General Considerations
The steady-state peak serum theophylline concentration is a function of the dose, the dosing interval, and the rate of theophylline absorption and clearance in the individual patient. Because of marked individual differences in the rate of theophylline clearance, the dose required to achieve a peak serum theophylline concentration in the 10 to 20 mcg/mL range varies fourfold among otherwise similar patients in the absence of factors known to alter theophylline clearance (e.g., 400 to 1600 mg/day in adults <60 years old and 10 to 36 mg/kg/day in children 1 to 9 years old). For a given population, there is no single theophylline dose that will provide both safe and effective serum concentrations for all patients. Administration of the median theophylline dose required to achieve a therapeutic serum theophylline concentration in a given population may result in either sub-therapeutic or potentially toxic serum theophylline concentrations in individual patients. For example, at a dose of 900 mg/d in adults <60 years or 22 mg/kg/d in children 1 to 9 years, the steady-state peak serum theophylline concentration will be <10 mcg/mL in about 30% of patients, 10 to 20 mcg/mL in about 50% and 20 to 30 mcg/mL in about 20% of patients. The dose of theophylline must be individualized on the basis of peak serum theophylline concentration measurements in order to achieve a dose that will provide maximum potential benefit with minimal risk of adverse effects.
Transient caffeine-like adverse effects and excessive serum concentrations in slow metabolizers can be avoided in most patients by starting with a sufficiently low dose and slowly increasing the dose, if judged to be clinically indicated, in small increments (see Table V ) . Dose increases should only be made if the previous dosage is well tolerated and at intervals of no less than 3 days to allow serum theophylline concentrations to reach the new steady-state. Dosage adjustment should be guided by serum theophylline concentration measurement (see PRECAUTIONS, Laboratory Tests and DOSAGE AND ADMINISTRATION, Table VI ) . Healthcare providers should instruct patients and caregivers to discontinue any dosage that causes adverse effects, to withhold the medication until these symptoms are gone, and to then resume therapy at a lower, previously tolerated dosage (see WARNINGS ) .
If the patient's symptoms are well controlled, there are no apparent adverse effects, and no intervening factors that might alter dosage requirements (see WARNINGS and PRECAUTIONS ) , serum theophylline concentrations should be monitored at 6 month intervals for rapidly growing children and at yearly intervals for all others. In acutely ill patients, serum theophylline concentrations should be monitored at frequent intervals, e.g., every 24 hours.
Theophylline distributes poorly into body fat; therefore, mg/kg dose should be calculated on the basis of ideal body weight.
Table V contains theophylline dosing titration schema recommended for patients in various age groups and clinical circumstances. Table VI contains recommendations for theophylline dosage adjustment based upon serum theophylline concentrations. Application of these general dosing recommendations to individual patients must take into account the unique clinical characteristics of each patient. In general, these recommendations should serve as the upper limit for dosage adjustments in order to decrease the risk of potentially serious adverse events associated with unexpected large increases in serum theophylline concentration.
| A. Children (12 to 15 years) and adults (16 to 60 years) without risk factors for impaired clearance . | ||
|---|---|---|
| Titration Step | Children <45 kg | Children >45 kg and adults |
| 12 to 14 mg/kg/day up to a maximum of 300 mg/day admin. QD | 300 to 400 mg/day If caffeine-like adverse effects occur, then consideration should be given to a lower dose and titrating the dose more slowly (see ADVERSE REACTIONS ). admin. QD |
| 16 mg/kg/day up to a maximum of 400 mg/day admin. QD | 400 to 600 mg/dayadmin. QD |
| 20 mg/kg/day up to a maximum of 600 mg/day admin. QD | As with all theophylline products, doses greater than 600 mg should be titrated according to blood level (see Table VI ). |
- B. Patients with risk factors for impaired clearance, the elderly (>60 years), and those in whom it is not feasible to monitor serum theophylline concentrations:
In children 12 to 15 years of age, the theophylline dose should not exceed 16 mg/kg/day up to a maximum of 400 mg/day in the presence of risk factors for reduced theophylline clearance (see WARNINGS ) or if it is not feasible to monitor serum theophylline concentrations.
In adolescents ≥16 years and adults, including the elderly, the theophylline dose should not exceed 400 mg/day in the presence of risk factors for reduced theophylline clearance (see WARNINGS ) or if it is not feasible to monitor serum theophylline concentrations.
| Peak Serum | |
|---|---|
| Concentration | Dosage Adjustment |
| ¶Dose reduction and/or serum theophylline concentration measurement is indicated whenever adverse effects are present, physiologic abnormalities that can reduce theophylline clearance occur (e.g. sustained fever), or a drug that interacts with theophylline is added or discontinued (see WARNINGS ). | |
| <9.9 mcg/mL | If symptoms are not controlled and current dosage is tolerated, increase dose about 25%. Recheck serum concentration after three days for further dosage adjustment. |
| 10 to 14.9 mcg/mL | If symptoms are controlled and current dosage is tolerated, maintain dose and recheck serum concentration at 6 to12 month intervals. If symptoms are not controlled and current dosage is tolerated, consider adding additional medication(s) to treatment regimen. |
| 15 to 19.9 mcg/mL | Consider 10% decrease in dose to provide greater margin of safety even if current dosage is tolerated. |
| 20 to 24.9 mcg/mL | Decrease dose by 25% even if no adverse effects are present. Recheck serum concentration after 3 days to guide further dosage adjustment. |
| 25 to 30 mcg/mL | Skip next dose and decrease subsequent doses at least 25% even if no adverse effects are present. Recheck serum concentration after 3 days to guide further dosage adjustment. If symptomatic, consider whether overdose treatment is indicated (see recommendations for chronic overdosage ). |
| >30 mcg/mL | Treat overdose as indicated (see recommendations for chronic overdosage ). If theophylline is subsequently resumed, decrease dose by at least 50% and recheck serum concentration after 3 days to guide further dosage adjustment. |
CONTRAINDICATIONS
Theophylline (anhydrous) extended-release tablets are contraindicated in patients with a history of hypersensitivity to theophylline or other components in the product.
ADVERSE REACTIONS
Adverse reactions associated with theophylline are generally mild when peak serum theophylline concentrations are <20 mcg/mL and mainly consist of transient caffeine-like adverse effects such as nausea, vomiting, headache, and insomnia. When peak serum theophylline concentrations exceed 20 mcg/mL, however, theophylline produces a wide range of adverse reactions including persistent vomiting, cardiac arrhythmias, and intractable seizures which can be lethal (see OVERDOSAGE ) . The transient caffeine-like adverse reactions occur in about 50% of patients when theophylline therapy is initiated at doses higher than recommended initial doses (e.g., >300 mg/day in adults and >12 mg/kg/day in children beyond >1 year of age). During the initiation of theophylline therapy, caffeine-like adverse effects may transiently alter patient behavior, especially in school age children, but this response rarely persists. Initiation of theophylline therapy at a low dose with subsequent slow titration to a predetermined age-related maximum dose will significantly reduce the frequency of these transient adverse effects (see DOSAGE AND ADMINISTRATION, Table V ) . In a small percentage of patients (<3% of children and <10% of adults) the caffeine-like adverse effects persist during maintenance therapy, even at peak serum theophylline concentrations within the therapeutic range (i.e., 10 to 20 mcg/mL). Dosage reduction may alleviate the caffeine-like adverse effects in these patients; however, persistent adverse effects should result in a reevaluation of the need for continued theophylline therapy and the potential therapeutic benefit of alternative treatment.
Other adverse reactions that have been reported at serum theophylline concentrations <20 mcg/mL include abdominal pain, agitation, anaphylactic reaction, anaphylactoid reaction, anxiety, cardiac arrhythmias, diarrhea, dizziness, fine skeletal muscle tremors, gastric irritation, gastroesophageal reflux, hyperuricemia, irritability, palpitations, pruritus, rash, sinus tachycardia, restlessness, transient dieresis, urinary retention, and urticaria. In patients with hypoxia secondary to COPD, multifocal atrial tachycardia and flutter have been reported at serum theophylline concentrations ≥15 mcg/mL. There have been a few isolated reports of seizures at serum theophylline concentrations <20 mcg/mL in patients with an underlying neurological disease or in elderly patients. The occurrence of seizures in elderly patients with serum theophylline concentrations <20 mcg/mL may be secondary to decreased protein binding resulting in a larger proportion of the total serum theophylline concentration in the pharmacologically active unbound form. The clinical characteristics of the seizures reported in patients with serum theophylline concentrations <20 mcg/mL have generally been milder than seizures associated with excessive serum theophylline concentrations resulting from an overdose (i.e., they have generally been transient, often stopped without anticonvulsant therapy, and did not result in neurological residua).
| Percentage of patients reported with sign or symptom | ||||
|---|---|---|---|---|
| Acute Overdose | Chronic Overdosage | |||
| (Large Single Ingestion) | (Multiple Excessive Doses) | |||
| Sign/Symptom | Study 1 | Study 2 | Study 1 | Study 2 |
| (n=157) | (n=14) | (n=92) | (n=102) | |
| Asymptomatic | NR NR=Not reported in a comparable manner. | 0 | NR | 6 |
| Gastrointestinal | ||||
| Vomiting | 73 | 93 | 30 | 61 |
| Abdominal Pain | NR | 21 | NR | 12 |
| Diarrhea | NR | 0 | NR | 14 |
| Hematemesis | NR | 0 | NR | 2 |
| Metabolic/Other | ||||
| Hypokalemia | 85 | 79 | 44 | 43 |
| Hyperglycemia | 98 | NR | 18 | NR |
| Acid/base disturbance | 34 | 21 | 9 | 5 |
| Rhabdomyolysis | NR | 7 | NR | 0 |
| Cardiovascular | ||||
| Sinus tachycardia | 100 | 86 | 100 | 62 |
| Other supraventricular tachycardias | 2 | 21 | 12 | 14 |
| Ventricular premature beats | 3 | 21 | 10 | 19 |
| Atrial fibrillation or flutter | 1 | NR | 12 | NR |
| Multifocal atrial tachycardia | 0 | NR | 2 | NR |
| Ventricular arrhythmias with hemodynamic instability | 7 | 14 | 40 | 0 |
| Hypotension/shock | NR | 21 | NR | 8 |
| Neurologic | ||||
| Nervousness | NR | 64 | NR | 21 |
| Tremors | 38 | 29 | 16 | 14 |
| Disorientation | NR | 7 | NR | 11 |
| Seizures | 5 | 14 | 14 | 5 |
| Death | 3 | 21 | 10 | 4 |
Drug Interactions
Theophylline interacts with a wide variety of drugs. The interaction may be pharmacodynamic, i.e., alterations in the therapeutic response to theophylline or another drug or occurrence of adverse effects without a change in serum theophylline concentration. More frequently, however, the interaction is pharmacokinetic, i.e., the rate of theophylline clearance is altered by another drug resulting in increased or decreased serum theophylline concentrations. Theophylline only rarely alters the pharmacokinetics of other drugs.
The drugs listed in Table II have the potential to produce clinically significant pharmacodynamic or pharmacokinetic interactions with theophylline. The information in the "Effect" column of Table II assumes that the interacting drug is being added to a steady-state theophylline regimen. If theophylline is being initiated in a patient who is already taking a drug that inhibits theophylline clearance (e.g., cimetidine, erythromycin), the dose of theophylline required to achieve a therapeutic serum theophylline concentration will be smaller. Conversely, if theophylline is being initiated in a patient who is already taking a drug that enhances theophylline clearance (e.g., rifampin), the dose of theophylline required to achieve a therapeutic serum theophylline concentration will be larger. Discontinuation of a concomitant drug that increases theophylline clearance will result in accumulation of theophylline to potentially toxic levels, unless the theophylline dose is appropriately reduced. Discontinuation of a concomitant drug that inhibits theophylline clearance will result in decreased serum theophylline concentrations, unless the theophylline dose is appropriately increased.
The drugs listed in Table III have either been documented not to interact with theophylline or do not produce a clinically significant interaction (i.e., <15% change in theophylline clearance).
The listing of drugs in Tables II and III are current as of February 9, 1995. New interactions are continuously being reported for theophylline, especially with new chemical entities. The healthcare professional should not assume that a drug does not interact with theophylline if it is not listed in Table II.Before addition of a newly available drug in a patient receiving theophylline, the package insert of the new drug and/or the medical literature should be consulted to determine if an interaction between the new drug and theophylline has been reported.
| Drug | Type of Interaction | Effect Average effect on steady-state theophylline concentration or other clinical effect for pharmacologic interactions. Individual patients may experience larger changes in serum theophylline concentration than the value listed. |
|---|---|---|
| Adenosine | Theophylline blocks adenosine receptors. | Higher doses of adenosine may be required to achieve desired effect. |
| Alcohol | A single large dose of alcohol (3 mL/kg of whiskey) decreases theophylline clearance for up to 24 hours. | 30% increase |
| Allopurinol | Decreases theophylline clearance at allopurinol doses ≥600 mg/day. | 25% increase |
| Aminoglutethimide | Increases theophylline clearance by induction of microsomal enzyme activity. | 25% decrease |
| Carbamazepine | Similar to aminoglutethimide. | 30% decrease |
| Cimetidine | Decreases theophylline clearance by inhibiting cytochrome P450 1A2. | 70% increase |
| Ciprofloxacin | Similar to cimetidine. | 40% increase |
| Clarithromycin | Similar to erythromycin. | 25% increase |
| Diazepam | Benzodiazepines increase CNS concentrations of adenosine, a potent CNS depressant, while theophylline blocks adenosine receptors. | Larger diazepam doses may be required to produce desired level of sedation. Discontinuation of theophylline without reduction of diazepam dose may result in respiratory depression. |
| Disulfiram | Decreases theophylline clearance by inhibiting hydroxylation and demethylation. | 50% increase |
| Enoxacin | Similar to cimetidine. | 300% increase |
| Ephedrine | Synergistic CNS effects. | Increased frequency of nausea, nervousness, and insomnia. |
| Erythromycin | Erythromycin metabolite decreases theophylline clearance by inhibiting cytochrome P450 3A3. | 35% increase. Erythromycin steady-state serum concentrations decrease by a similar amount. |
| Estrogen | Estrogen containing oral contraceptives decrease theophylline clearance in a dose-dependent fashion. The effect of progesterone on theophylline clearance is unknown. | 30% increase |
| Flurazepam | Similar to diazepam. | Similar to diazepam. |
| Fluvoxamine | Similar to cimetidine. | Similar to cimetidine. |
| Halothane | Halothane sensitizes the myocardium to catecholamines, theophylline increases release of endogenous catecholamines. | Increased risk of ventricular arrhythmias. |
| Interferon, human recombinant alpha-A | Decreases theophylline clearance. | 100% increase |
| Isoproterenol (IV) | Increases theophylline clearance. | 20% decrease |
| Ketamine | Pharmacologic | May lower theophylline seizure threshold. |
| Lithium | Theophylline increases renal lithium clearance. | Lithium dose required to achieve a therapeutic serum concentration increased an average of 60%. |
| Lorazepam | Similar to diazepam. | Similar to diazepam. |
| Methotrexate (MTX) | Decreases theophylline clearance. | 20% increase after low dose MTX, higher dose MTX may have a greater effect. |
| Mexiletine | Similar to disulfiram. | 80% increase |
| Midazolam | Similar to diazepam. | Similar to diazepam. |
| Moricizine | Increases theophylline clearance. | 25% decrease |
| Pancuronium | Theophylline may antagonize non-depolarizing neuromuscular blocking effects; possibly due to phosphodiesterase inhibition. | Larger dose of pancuronium may be required to achieve neuromuscular blockade. |
| Pentoxifylline | Decreases theophylline clearance. | 30% increase |
| Phenobarbital (PB) | Similar to aminoglutethimide. | 25% decrease after two weeks of concurrent PB. |
| Phenytoin | Phenytoin increases theophylline clearance by increasing microsomal enzyme activity. Theophylline decreases phenytoin absorption. | Serum theophylline and phenytoin concentrations decrease about 40%. |
| Propafenone | Decreases theophylline clearance and pharmacologic interaction. | 40% increase. Beta-2 blocking effect may decrease efficacy of theophylline. |
| Propranolol | Similar to cimetidine and pharmacologic interaction. | 100% increase. Beta-2 blocking effect may decrease efficacy of theophylline. |
| Rifampin | Increases theophylline clearance by increasing cytochrome P450 1A2 and 3A3 activity. | 20 to 40% decrease |
| St. John's Wort (Hypericum Perforatum) | Decrease in theophylline plasma concentrations. | Higher doses of theophylline may be required to achieve desired effect. Stopping St. John's Wort may result in theophylline toxicity. |
| Sulfinpyrazone | Increases theophylline clearance by increasing demethylation and hydroxylation. Decreases renal clearance of theophylline. | 20% decrease |
| Tacrine | Similar to cimetidine, also increases renal clearance of theophylline. | 90% increase |
| Thiabendazole | Decreases theophylline clearance. | 190% increase |
| Ticlopidine | Decreases theophylline clearance. | 60% increase |
| Troleandomycin | Similar to erythromycin. | 33 to 100% increase depending on troleandomycin dose. |
| Verapamil | Similar to disulfiram. | 20% increase |
| albuterol, systemic and inhaled | mebendazole |
| amoxicillin | medroxyprogesterone |
| ampicillin, with or without sulbactam | methylprednisolone metronidazole |
| atenolol | metoprolol |
| azithromycin | nadolol |
| caffeine, dietary ingestion | nifedipine |
| cefaclor | nizatidine |
| co-trimoxazole (trimethoprim and sulfamethoxazole) | norfloxacin ofloxacin |
| diltiazem | omeprazole |
| dirithromycin | prednisone, prednisolone |
| enflurane | ranitidine |
| famotidine | rifabutin |
| felodipine | roxithromycin |
| finasteride | sorbitol (purgative doses do not inhibit theophylline absorption) |
| hydrocortisone | |
| isoflurane | sucralfate |
| isoniazid | terbutaline, systemic |
| isradipine | terfenadine |
| influenza vaccine | tetracycline |
| ketoconazole | tocainide |
| lomefloxacin |
DESCRIPTION
Theophylline (Anhydrous) Extended-Release Tablets, in a controlled-release system, allow a 24-hour dosing interval for appropriate patients.
Theophylline is structurally classified as a methylxanthine. It occurs as a white, odorless, crystalline powder with a bitter taste. Anhydrous theophylline has the chemical name 1H-Purine-2,6-dione, 3,7-dihydro-1,3-dimethyl-, and is represented by the following structural formula:
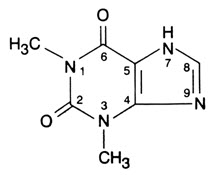
The molecular formula of anhydrous theophylline is C 7 H 8 N 4 O 2 with a molecular weight of 180.17.
Each extended-release tablet for oral administration contains 400 of anhydrous theophylline.
Inactive Ingredients: cetostearyl alcohol, hydroxyethyl cellulose, magnesium stearate, povidone, and talc.
CLINICAL PHARMACOLOGY
Mechanism of Action
Theophylline has two distinct actions in the airways of patients with reversible obstruction; smooth muscle relaxation (i.e., bronchodilation) and suppression of the response of the airways to stimuli (i.e., non-bronchodilator prophylactic effects). While the mechanisms of action of theophylline are not known with certainty, studies in animals suggest that bronchodilatation is mediated by the inhibition of two isozymes of phosphodiesterase (PDE III and, to a lesser extent, PDE IV) while non-bronchodilator prophylactic actions are probably mediated through one or more different molecular mechanisms, that do not involve inhibition of PDE III or antagonism of adenosine receptors. Some of the adverse effects associated with theophylline appear to be mediated by inhibition of PDE III (e.g., hypotension, tachycardia, headache, and emesis) and adenosine receptor antagonism (e.g., alterations in cerebral blood flow).
Theophylline increases the force of contraction of diaphragmatic muscles. This action appears to be due to enhancement of calcium uptake through an adenosine-mediated channel.
Serum Concentration-Effect Relationship
Bronchodilation occurs over the serum theophylline concentration range of 5 to 20 mcg/mL. Clinically important improvement in symptom control has been found in most studies to require peak serum theophylline concentrations >10 mcg/mL, but patients with mild disease may benefit from lower concentrations. At serum theophylline concentrations >20 mcg/mL, both the frequency and severity of adverse reactions increase. In general, maintaining peak serum theophylline concentrations between 10 and 15 mcg/mL will achieve most of the drug's potential therapeutic benefit while minimizing the risk of serious adverse events.
Pharmacokinetics
Overview
Theophylline is rapidly and completely absorbed after oral administration in solution or immediate-release solid oral dosage form. Theophylline does not undergo any appreciable pre-systemic elimination, distributes freely into fat-free tissues, and is extensively metabolized in the liver.
The pharmacokinetics of theophylline vary widely among similar patients and cannot be predicted by age, sex, body weight or other demographic characteristics. In addition, certain concurrent illnesses and alterations in normal physiology (see Table I ) and co-administration of other drugs (see Table II ) can significantly alter the pharmacokinetic characteristics of theophylline. Within-subject variability in metabolism has also been reported in some studies, especially in acutely ill patients. It is, therefore, recommended that serum theophylline concentrations be measured frequently in acutely ill patients (e.g., at 24-hr intervals) and periodically in patients receiving long-term therapy, e.g., at 6 to 12 month intervals. More frequent measurements should be made in the presence of any condition that may significantly alter theophylline clearance (see PRECAUTIONS, Laboratory Tests ).
| Population Characteristics | Total body clearance Clearance represents the volume of blood completely cleared of theophylline by the liver in one minute. Values listed were generally determined at serum theophylline concentrations <20 mcg/mL; clearance may decrease and half-life may increase at higher serum concentrations due to non-linear pharmacokinetics. mean (range) Reported range or estimated range (mean ±2 SD) where actual range not reported. (mL/kg/min) | Half-life mean (range) (hr) |
|---|---|---|
| Age | ||
| Premature neonates | ||
| postnatal age 3 to 15 days | 0.29 (0.09 to 0.49) | 30 (17 to 43) |
| postnatal age 25 to 57 days | 0.64 (0.04 to 1.2) | 20 (9.4 to 30.6) |
| Term infants | ||
| postnatal age 1 to 2 days | NR NR=not reported or not reported in a comparable format. | 25.7 (25 to 26.5) |
| postnatal age 3 to 30 weeks | NR | 11 (6 to 29) |
| Children | ||
| 1 to 4 years | 1.7 (0.5 to 2.9) | 3.4 (1.2 to 5.6) |
| 4 to 12 years | 1.6 (0.8 to 2.4) | NR |
| 13 to 15 years | 0.9 (0.48 to 1.3) | NR |
| 6 to 17 years | 1.4 (0.2 to 2.6) | 3.7 (1.5 to 5.9) |
| Adults (16 to 60 years) | ||
| otherwise healthy | ||
| non-smoking asthmatics | 0.65 (0.27 to 1.03) | 8.7 (6.1 to 12.8) |
| Elderly (>60 years) | ||
| non-smokers with normal cardiac, liver, and renal function | 0.41 (0.21 to 0.61) | 9.8 (1.6 to 18) |
| Concurrent illness or altered physiological state | ||
| Acute pulmonary edema | 0.33 Median (0.07 to 2.45) | 19(3.1 to 82) |
| COPD->60 years, stable | ||
| non-smoker >1 year | 0.54 (0.44 to 0.64) | 11 (9.4 to 12.6) |
| COPD with cor pulmonale | 0.48 (0.08 to 0.88) | NR |
| Cystic fibrosis (14 to 28 years) | 1.25 (0.31 to 2.2) | 6.0 (1.8 to 10.2) |
| Fever associated with acute viral | ||
| respiratory illness | ||
| (children 9 to 15 years) | NR | 7.0 (1.0 to 13) |
| Liver disease | ||
| cirrhosis | 0.31(0.1 to 0.7) | 32(10 to 56) |
| acute hepatitis | 0.35 (0.25 to 0.45) | 19.2 (16.6 to 21.8) |
| cholestasis | 0.65 (0.25 to 1.45) | 14.4 (5.7 to 31.8) |
| Pregnancy | ||
| 1st trimester | NR | 8.5 (3.1 to 13.9) |
| 2nd trimester | NR | 8.8 (3.8 to 13.8) |
| 3rd trimester | NR | 13.0 (8.4 to 17.6) |
| Sepsis with multi-organ failure | 0.47 (0.19 to 1.9) | 18.8 (6.3 to 24.1) |
| Thyroid disease | ||
| hypothyroid | 0.38 (0.13 to 0.57) | 11.6 (8.2 to 25) |
| hyperthyroid | 0.8 (0.68 to 0.97) | 4.5 (3.7 to 5.6) |
Note: In addition to the factors listed above, theophylline clearance is increased and half-life decreased by low carbohydrate/high protein diets, parenteral nutrition, and daily consumption of charcoal-broiled beef. A high carbohydrate/low protein diet can decrease the clearance and prolong the half-life of theophylline.
Absorption
Theophylline (anhydrous) extended-release tablets administered in the fed state is completely absorbed after oral administration.
In a single-dose crossover study, two 400 mg theophylline (anhydrous) extended-release tablets were administered to 19 normal volunteers in the morning or evening immediately following the same standardized meal (769 calories consisting of 97 grams carbohydrates, 33 grams protein and 27 grams fat). There was no evidence of dose dumping nor were there any significant differences in pharmacokinetic parameters attributable to time of drug administration. On the morning arm, the pharmacokinetic parameters were AUC=241.9±83.0 mcg hr/mL, C max =9.3±2.0 mcg/mL, T max =12.8±4.2 hours. On the evening arm, the pharmacokinetic parameters were AUC=219.7±83.0 mcg hr/mL, C max =9.2±2.0 mcg/mL, T max =12.5±4.2 hours.
A study in which theophylline (anhydrous) extended-release 400 mg tablets were administered to 17 fed adult asthmatics produced similar theophylline level-time curves when administered in the morning or evening. Serum levels were generally higher in the evening regimen but there were no statistically significant differences between the two regimens.
| MORNING | EVENING | |
|---|---|---|
| AUC (0 to 24 hrs) (mcg hr/mL) | 236.0±76.7 | 256.0±80.4 |
| C max (mcg/mL) | 14.5±4.1 | 16.3±4.5 |
| C min (mcg/mL) | 5.5±2.9 | 5.0±2.5 |
| T max (hours) | 8.1±3.7 | 10.1±4.1 |
A single-dose study in 15 normal fasting male volunteers whose theophylline inherent mean elimination half-life was verified by a liquid theophylline product to be 6.9±2.5 (SD) hours were administered two or three 400 mg theophylline (anhydrous) extended-release tablets. The relative bioavailability of theophylline (anhydrous) extended-release tablets given in the fasting state in comparison to an immediate-release product was 59%. Peak serum theophylline levels occurred at 6.9±5.2 (SD) hours, with a normalized (to 800 mg) peak level being 6.2±2.1 (SD). The apparent elimination half-life for the 400 mg theophylline (anhydrous) extended-release tablets was 17.2±5.8 (SD) hours.
Steady-state pharmacokinetics were determined in a study in 12 fasted patients with chronic reversible obstructive pulmonary disease. All were dosed with two 400 mg theophylline (anhydrous) extended-release tablets given once daily in the morning and a reference controlled-release BID product administered as two 200 mg tablets given 12 hours apart. The pharmacokinetic parameters obtained for theophylline (anhydrous) extended-release tablets given at doses of 800 mg once daily in the morning were virtually identical to the corresponding parameters for the reference drug when given as 400 mg BID. In particular, the AUC, C max and C min values obtained in this study were as follows:
| Theophylline (Anhydrous) Extended-Release Tablets | Reference Drug | ||
|---|---|---|---|
| 800 mg | 400 mg | ||
| Q24h±SD | Q12h±SD | ||
| AUC, (0 to 24 hours), mcg hr/mL | 288.9±21.5 | 283.5±38.4 | |
| C max , mcg/mL | 15.7±2.8 | 15.2±2.1 | |
| C min , mcg/mL | 7.9±1.6 | 7.8±1.7 | |
| C max -C min diff. | 7.7±1.5 | 7.4±1.5 | |
Single-dose studies in which subjects were fasted for twelve (12) hours prior to and an additional four (4) hours following dosing, demonstrated reduced bioavailability as compared to dosing with food. One single-dose study in 20 normal volunteers dosed with two (2) 400 mg tablets in the morning, compared dosing under these fasting conditions with dosing immediately prior to a standardized breakfast (769 calories, consisting of 97 grams carbohydrates, 33 grams protein and 27 grams fat). Under fed conditions, the pharmacokinetic parameters were: AUC=231.7±92.4 mcg hr/mL, C max =8.4±2.6 mcg/mL, T max =17.3±6.7 hours. Under fasting conditions, these parameters were AUC=141.2±6.53 mcg hr/mL, C max =5.5±1.5 mcg/mL, T max =6.5±2.1 hours.
Another single-dose study in 21 normal male volunteers, dosed in the evening, compared fasting to a standardized high calorie, high fat meal (870 to 1,020 calories, consisting of 33 grams protein, 55 to 75 grams fat, 58 grams carbohydrates). In the fasting arm, subjects received one theophylline (anhydrous) extended-release 400mg tablet at 8 p.m. after an eight hour fast followed by a further four hour fast. In the fed arm, subjects were again dosed with one 400 mg theophylline (anhydrous) extended-release tablet, but at 8 p.m. immediately after the high fat content standardized meal cited above. The pharmacokinetic parameters (normalized to 800 mg) fed were AUC=221.8±40.9 mcg hr/mL, C max =10.9±1.7 mcg/mL, T max =11.8±2.2 hours. In the fasting arm, the pharmacokinetic parameters (normalized to 800 mg) were AUC=146.4±40.9 mcg hr/mL, C max =6.7±1.7 mcg/mL, T max =7.3±2.2 hours.
Thus, administration of single theophylline (anhydrous) extended-release doses to healthy normal volunteers, under prolonged fasted conditions (at least 10 hour overnight fast before dosing followed by an additional four (4) hour fast after dosing) results in decreased bioavailability. However, there was no failure of this delivery system leading to a sudden and unexpected release of a large quantity of theophylline with theophylline (anhydrous) extended-release tablets even when they are administered with a high fat, high calorie meal.
Similar studies were conducted with the 600 mg theophylline (anhydrous) extended-release tablet. A single-dose study in 24 subjects with an established theophylline clearance of ≤4 L/hr, compared the pharmacokinetic evaluation of one 600 mg theophylline (anhydrous) extended-release tablet and one and one-half 400 mg theophylline (anhydrous) extended-release tablets under fed (using a standard high fat diet) and fasted conditions. The results of this 4-way randomized crossover study demonstrate the bioequivalence of the 400 mg and 600 mg theophylline (anhydrous) extended-release tablets. Under fed conditions, the pharmacokinetic results for the one and one-half 400 mg tablets were AUC=214.64±55.88 mcg hr/mL, C max =10.58±2.21 mcg/mL, and T max =9.00±2.64 hours, and for the 600 mg tablet were AUC=207.85±48.9 mcg hr/mL, C max =10.39±1.91 mcg/mL, and T max =9.58±1.86 hours. Under fasted conditions, the pharmacokinetic results for the one and one-half 400 mg tablets were AUC=191.85 ±51.1 mcg hr/mL, C max = 7.37±1.83 mcg/mL, and T max =8.08±4.39 hours; and for the 600 mg tablet were AUC=199.39±70.27 mcg hr/mL, C max =7.66±2.09 mcg/mL, and T max =9.67±4.89 hours.
In this study, the mean fed/fasted ratios for the one and one-half 400 mg tablets and the 600 mg tablet were about 112% and 104%, respectively.
In another study, the bioavailability of the 600 mg theophylline (anhydrous) extended-release tablet was examined with morning and evening administration. This single-dose crossover study in 22 healthy males was conducted under fed (standard high fat diet) conditions. The results demonstrated no clinically significant difference in the bioavailability of the 600 mg theophylline (anhydrous) extended-release tablet administered in the morning or in the evening. The results were: AUC=233.6±45.1 mcg hr/mL, C max =10.6±1.3 mcg/mL, and T max =12.5±3.2 hours with morning dosing; AUC=209.8±46.2 mcg hr/mL, C max =9.7±1.4 mcg/mL, and T max =13.7±3.3 hours with evening dosing. The PM/AM ratio was 89.3%.
The absorption characteristics of theophylline (anhydrous) extended-release tablets (theophylline anhydrous) have been extensively studied. A steady-state crossover bioavailability study in 22 normal males compared two theophylline (anhydrous) extended-release 400 mg tablets administered q24h at 8 a.m. immediately after breakfast with a reference controlled-release theophylline product administered BID in fed subjects at 8 a.m. immediately after breakfast and 8 p.m. immediately after dinner (769 calories, consisting of 97 grams carbohydrates, 33 grams protein, and 27 grams fat).
The pharmacokinetic parameters for theophylline (anhydrous) extended-release 400 mg tablets under these steady-state conditions were AUC=203.3±87.1 mcg hr/mL, C max =12.1±3.8 mcg/mL, C min =4.50±3.6, T max =8.8±4.6 hours. For the reference BID product, the pharmacokinetic parameters were AUC=219.2±88.4 mcg hr/mL, C max =11.0±4.1 mcg/mL, C min =7.28±3.5, T max =6.9±3.4 hours. The mean percent fluctuation [(C max -C min /C min )×100]=169% for the once-daily regimen and 51% for the reference product BID regimen.
The bioavailability of the 600 mg theophylline (anhydrous) extended-release tablet was further evaluated in a multiple dose, steady-state study in 26 healthy males comparing the 600 mg tablet to one and one-half 400 mg theophylline (anhydrous) extended-release tablets. All subjects had previously established theophylline clearances of ≤4 L/hr and were dosed once-daily for 6 days under fed conditions. The results showed no clinically significant difference between the 600 mg and one and one-half 400 mg theophylline (anhydrous) extended-release tablet regimens. Steady-state results were:
| 600 MG | ||
|---|---|---|
| (ONE+ONE-HALF | ||
| 600 MG TABLET FED | 400 MG TABLETS) | |
| FED | ||
| AUC 0 to 24hrs (mcg hr/mL) | 209.77±51.04 | 212.32±56.29 |
| C max (mcg/mL) | 12.91±2.46 | 13.17±3.11 |
| C min (mcg/mL) | 5.52±1.79 | 5.39±1.95 |
| T max (hours) | 8.62±3.21 | 7.23±2.35 |
| Percent Fluctuation | 183.73±54.02 | 179.72±28.86 |
The bioavailability ratio for the 600/400 mg tablets was 98.8%. Thus, under all study conditions, the 600 mg tablet is bioequivalent to one and one-half 400 mg tablets.
Studies demonstrate that as long as subjects were either consistently fed or consistently fasted, there is similar bioavailability with once-daily administration of theophylline (anhydrous) extended-release tablets whether dosed in the morning or evening.
Distribution
Once theophylline enters the systemic circulation, about 40% is bound to plasma protein, primarily albumin. Unbound theophylline distributes throughout body water, but distributes poorly into body fat. The apparent volume of distribution of theophylline is approximately 0.45 L/kg (range 0.3 to 0.7 L/kg) based on ideal body weight. Theophylline passes freely across the placenta, into breast milk and into the cerebrospinal fluid (CSF). Saliva theophylline concentrations approximate unbound serum concentrations, but are not reliable for routine or therapeutic monitoring unless special techniques are used. An increase in the volume of distribution of theophylline, primarily due to reduction in plasma protein binding, occurs in premature neonates, patients with hepatic cirrhosis, uncorrected acidemia, the elderly and in women during the third trimester of pregnancy. In such cases, the patient may show signs of toxicity at total (bound+unbound) serum concentrations of theophylline in the therapeutic range (10 to 20 mcg/mL) due to elevated concentrations of the pharmacologically active unbound drug. Similarly, a patient with decreased theophylline binding may have a sub-therapeutic total drug concentration while the pharmacologically active unbound concentration is in the therapeutic range. If only total serum theophylline concentration is measured, this may lead to an unnecessary and potentially dangerous dose increase. In patients with reduced protein binding, measurement of unbound serum theophylline concentration provides a more reliable means of dosage adjustment than measurement of total serum theophylline concentration. Generally, concentrations of unbound theophylline should be maintained in the range of 6 to 12 mcg/mL.
Metabolism
Following oral dosing, theophylline does not undergo any measurable first-pass elimination. In adults and children beyond one year of age, approximately 90% of the dose is metabolized in the liver. Biotransformation takes place through demethylation to 1-methylxanthine and 3-methylxanthine and hydroxylation to 1,3-dimethyluric acid. 1-methylxanthine is further hydroxylated, by xanthine oxidase, to 1-methyluric acid. About 6% of a theophylline dose is N-methylated to caffeine. Theophylline demethylation to 3-methylxanthine is catalyzed by cytochrome P-450 1A2, while cytochromes P-450 2E1 and P-450 3A3 catalyze the hydroxylation to 1,3-dimethyluric acid. Demethylation to 1-methylxanthine appears to be catalyzed either by cytochrome P-450 1A2 or a closely related cytochrome. In neonates, the N-demethylation pathway is absent while the function of the hydroxylation pathway is markedly deficient. The activity of these pathways slowly increases to maximal levels by one year of age.
Caffeine and 3-methylxanthine are the only theophylline metabolites with pharmacologic activity. 3-methylxanthine has approximately one tenth the pharmacologic activity of theophylline and serum concentrations in adults with normal renal function are <1 mcg/mL. In patients with end-stage renal disease, 3-methylxanthine may accumulate to concentrations that approximate the unmetabolized theophylline concentration. Caffeine concentrations are usually undetectable in adults regardless of renal function. In neonates, caffeine may accumulate to concentrations that approximate the unmetabolized theophylline concentration and thus, exert a pharmacologic effect.
Both the N-demethylation and hydroxylation pathways of theophylline biotransformation are capacity-limited. Due to the wide intersubject variability of the rate of theophylline metabolism, non-linearity of elimination may begin in some patients at serum theophylline concentrations <10 mcg/mL. Since this non-linearity results in more than proportional changes in serum theophylline concentrations with changes in dose, it is advisable to make increases or decreases in dose in small increments in order to achieve desired changes in serum theophylline concentrations (see DOSAGE AND ADMINISTRATION, Table VI ). Accurate prediction of dose-dependency of theophylline metabolism in patients a priori is not possible, but patients with very high initial clearance rates (i.e., low steady-state serum theophylline concentrations at above average doses) have the greatest likelihood of experiencing large changes in serum theophylline concentration in response to dosage changes.
Excretion
In neonates, approximately 50% of the theophylline dose is excreted unchanged in the urine. Beyond the first three months of life, approximately 10% of the theophylline dose is excreted unchanged in the urine. The remainder is excreted in the urine mainly as 1,3-dimethyluric acid (35 to 40%), 1-methyluric acid (20 to 25%) and 3-methylxanthine (15 to 20%). Since little theophylline is excreted unchanged in the urine and since active metabolites of theophylline (i.e., caffeine, 3-methylxanthine) do not accumulate to clinically significant levels even in the face of end-stage renal disease, no dosage adjustment for renal insufficiency is necessary in adults and children >3 months of age. In contrast, the large fraction of the theophylline dose excreted in the urine as unchanged theophylline and caffeine in neonates requires careful attention to dose reduction and frequent monitoring of serum theophylline concentrations in neonates with reduced renal function (see WARNINGS ).
Serum Concentrations at Steady State
After multiple doses of theophylline, steady-state is reached in 30 to 65 hours (average 40 hours) in adults. At steady-state, on a dosage regimen with 24-hour intervals, the expected mean trough concentration is approximately 50% of the mean peak concentration, assuming a mean theophylline half-life of 8 hours. The difference between peak and trough concentrations is larger in patients with more rapid theophylline clearance. In these patients, administration of theophylline may be required more frequently (every 12 hours).
Special Populations
(see Table I for mean clearance and half-life values)
Geriatric
The clearance of theophylline is decreased by an average of 30% in healthy elderly adults (>60 yrs) compared to healthy young adults. Careful attention to dose reduction and frequent monitoring of serum theophylline concentrations are required in elderly patients (see WARNINGS ).
Pediatrics
The clearance of theophylline is very low in neonates (see WARNINGS ) . Theophylline clearance reaches maximal values by one year of age, remains relatively constant until about 9 years of age and then slowly decreases by approximately 50% to adult values at about age 16. Renal excretion of unchanged theophylline in neonates amounts to about 50% of the dose, compared to about 10% in children older than three months and in adults. Careful attention to dosage selection and monitoring of serum theophylline concentrations are required in pediatric patients (see WARNINGS and DOSAGE AND ADMINISTRATION ).
Gender
Gender differences in theophylline clearance are relatively small and unlikely to be of clinical significance. Significant reduction in theophylline clearance, however, has been reported in women on the 20th day of the menstrual cycle and during the third trimester of pregnancy.
Race
Pharmacokinetic differences in theophylline clearance due to race have not been studied.
Renal Insufficiency
Only a small fraction, e.g., about 10%, of the administered theophylline dose is excreted unchanged in the urine of children greater than three months of age and adults. Since little theophylline is excreted unchanged in the urine and since active metabolites of theophylline (i.e., caffeine, 3-methylxanthine) do not accumulate to clinically significant levels even in the face of end-stage renal disease, no dosage adjustment for renal insufficiency is necessary in adults and children >3 months of age. In contrast, approximately 50% of the administered theophylline dose is excreted unchanged in the urine in neonates. Careful attention to dose reduction and frequent monitoring of serum theophylline concentrations are required in neonates with decreased renal function (see WARNINGS ) .
Hepatic Insufficiency
Theophylline clearance is decreased by 50% or more in patients with hepatic insufficiency (e.g., cirrhosis, acute hepatitis, cholestasis). Careful attention to dose reduction and frequent monitoring of serum theophylline concentrations are required in patients with reduced hepatic function (see WARNINGS ) .
Congestive Heart Failure (CHF)
Theophylline clearance is decreased by 50% or more in patients with CHF. The extent of reduction in theophylline clearance in patients with CHF appears to be directly correlated to the severity of the cardiac disease. Since theophylline clearance is independent of liver blood flow, the reduction in clearance appears to be due to impaired hepatocyte function rather than reduced perfusion. Careful attention to dose reduction and frequent monitoring of serum theophylline concentrations are required in patients with CHF (see WARNINGS ) .
Smokers
Tobacco and marijuana smoking appears to increase the clearance of theophylline by induction of metabolic pathways. Theophylline clearance has been shown to increase by approximately 50% in young adult tobacco smokers and by approximately 80% in elderly tobacco smokers compared to non-smoking subjects. Passive smoke exposure has also been shown to increase theophylline clearance by up to 50%. Abstinence from tobacco smoking for one week causes a reduction of approximately 40% in theophylline clearance. Careful attention to dose reduction and frequent monitoring of serum theophylline concentrations are required in patients who stop smoking (see WARNINGS ) . Use of nicotine gum has been shown to have no effect on theophylline clearance.
Fever
Fever, regardless of its underlying cause, can decrease the clearance of theophylline. The magnitude and duration of the fever appear to be directly correlated to the degree of decrease of theophylline clearance. Precise data are lacking, but a temperature of 39°C (102°F) for at least 24 hours is probably required to produce a clinically significant increase in serum theophylline concentrations. Children with rapid rates of theophylline clearance (i.e., those who require a dose that is substantially larger than average [e.g., >22 mg/kg/day] to achieve a therapeutic peak serum theophylline concentration when afebrile) may be at greater risk of toxic effects from decreased clearance during sustained fever. Careful attention to dose reduction and frequent monitoring of serum theophylline concentrations are required in patients with sustained fever (see WARNINGS ) .
Miscellaneous
Other factors associated with decreased theophylline clearance include the third trimester of pregnancy, sepsis with multiple organ failure, and hypothyroidism. Careful attention to dose reduction and frequent monitoring of serum theophylline concentrations are required in patients with any of these conditions (see WARNINGS ) . Other factors associated with increased theophylline clearance include hyperthyroidism and cystic fibrosis.
CLINICAL STUDIES
In patients with chronic asthma, including patients with severe asthma requiring inhaled corticosteroids or alternate-day oral corticosteroids, many clinical studies have shown that theophylline decreases the frequency and severity of symptoms, including nocturnal exacerbations, and decreases the "as needed" use of inhaled beta-2 agonists. Theophylline has also been shown to reduce the need for short courses of daily oral prednisone to relieve exacerbations of airway obstruction that are unresponsive to bronchodilators in asthmatics.
In patients with chronic obstructive pulmonary disease (COPD), clinical studies have shown that theophylline decreases dyspnea, air trapping, the work of breathing, and improves contractility of diaphragmatic muscles with little or no improvement in pulmonary function measurements.
HOW SUPPLIED
Theophylline (Anhydrous) Extended-Release Tablets are supplied as follows:
| 400 mg - | round flat faced radius edged embossed (i.e. imprinted) with "P" bisect "F" on the upper side and "U" over "400" on lower side. | |
| Bottles of 100 tablets | NDC 42858-701-01 | |
Store at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature].
Dispense in a tight, light-resistant container.
Mechanism of Action
Theophylline has two distinct actions in the airways of patients with reversible obstruction; smooth muscle relaxation (i.e., bronchodilation) and suppression of the response of the airways to stimuli (i.e., non-bronchodilator prophylactic effects). While the mechanisms of action of theophylline are not known with certainty, studies in animals suggest that bronchodilatation is mediated by the inhibition of two isozymes of phosphodiesterase (PDE III and, to a lesser extent, PDE IV) while non-bronchodilator prophylactic actions are probably mediated through one or more different molecular mechanisms, that do not involve inhibition of PDE III or antagonism of adenosine receptors. Some of the adverse effects associated with theophylline appear to be mediated by inhibition of PDE III (e.g., hypotension, tachycardia, headache, and emesis) and adenosine receptor antagonism (e.g., alterations in cerebral blood flow).
Theophylline increases the force of contraction of diaphragmatic muscles. This action appears to be due to enhancement of calcium uptake through an adenosine-mediated channel.