Get your patient on Tramadol Hydrochloride - Tramadol Hydrochloride tablet, Extended Release (Tramadol Hydrochloride)
Tramadol Hydrochloride - Tramadol Hydrochloride tablet, Extended Release prescribing information
WARNING: SERIOUS AND LIFE-THREATENING RISKS FROM USE OF TRAMADOL HYDROCHLORIDE EXTENDED-RELEASE TABLETS
Addiction, Abuse, and Misuse
Because the use of tramadol hydrochloride extended-release tablets exposes patients and other users to the risks of opioid addiction, abuse, and misuse, which can lead to overdose and death, assess each patient’s risk prior to prescribing and reassess all patients regularly for the development of these behaviors and conditions [see Warnings] .
Life-Threatening Respiratory Depression
Serious, life-threatening, or fatal respiratory depression may occur with use of tramadol hydrochloride extended-release tablets, especially during initiation or following a dose increase. To reduce the risk of respiratory depression, proper dosing and titration of tramadol hydrochloride extended-release tablets are essential [see Warnings] . Instruct patients to swallow tramadol hydrochloride extended-release tablets whole to avoid exposure to a potentially fatal dose of tramadol.
Accidental Ingestion
Accidental ingestion of even one dose of tramadol hydrochloride extended-release tablets, especially by children, can result in a fatal overdose of tramadol [see Warnings] .
Risks From Concomitant Use With Benzodiazepines Or Other CNS Depressants
Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Reserve concomitant prescribing of tramadol hydrochloride extended-release tablets and benzodiazepines or other CNS depressants for use in patients for whom alternative treatment options are inadequate [see Warnings, Precautions; Drug Interactions ] .
Neonatal Opioid Withdrawal Syndrome (NOWS)
Advise pregnant women using opioids for an extended period of time of the risk of Neonatal Opioid Withdrawal Syndrome, which may be life-threatening if not recognized and treated. Ensure that management by neonatology experts will be available at delivery [see Warnings ].
Opioid Analgesic Risk Evaluation and Mitigation Strategy (REMS):
Healthcare providers are strongly encouraged to complete a REMS-compliant education program and to counsel patients and caregivers on serious risks, safe use, and the importance of reading the Medication Guide with each prescription [see Warnings] .
Ultra-Rapid Metabolism of Tramadol and Other Risk Factors for Life-Threatening Respiratory Depression in Children
Life-threatening respiratory depression and death have occurred in children who received tramadol. Some of the reported cases followed tonsillectomy and/or adenoidectomy; in at least one case, the child had evidence of being an ultra-rapid metabolizer of tramadol due to a CYP2D6 polymorphism [see WARNINGS]. Tramadol hydrochloride extended-release tablets are contraindicated in children younger than 12 years of age and in children younger than 18 years of age following tonsillectomy and/or adenoidectomy [see CONTRAINDICATIONS]. Avoid the use of tramadol hydrochloride extended-release tablets in adolescents 12 to 18 years of age who have other risk factors that may increase their sensitivity to the respiratory depressant effects of tramadol [see WARNINGS].
Interactions with Drugs Affecting Cytochrome P450 Isoenzymes
The effects of concomitant use or discontinuation of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors with tramadol hydrochloride are complex. Use of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors with Tramadol Extended-Release Tablets requires careful consideration of the effects on the parent drug, tramadol, and the active metabolite, M1 [see WARNINGS, PRECAUTIONS; Drug Interactions].
INDICATIONS AND USAGE
Tramadol hydrochloride extended-release tablets are indicated for the management of severe and persistent pain that requires an opioid analgesic and that cannot be adequately treated with alternative options, including immediate-release opioids.
Limitations of Use
• Because of the risks of addiction, abuse, misuse, overdose, and death, which can occur at any dosage or duration and persist over the course of therapy [see Warnings] , reserve opioid analgesics, including tramadol hydrochloride extended-release tablets, for use in patients for whom alternative treatment options are ineffective, not tolerated, or would be otherwise inadequate to provide sufficient management of pain.
• Tramadol hydrochloride extended-release tablets are not indicated as an as-needed (prn) analgesic.
DOSAGE AND ADMINISTRATION
Important Dosage and Administration Instructions
- Tramadol hydrochloride extended-release tablets should be prescribed only by healthcare professionals who are knowledgeable about the use of extended-release/long-acting opioids and how to mitigate the associated risks.
- Do not use tramadol hydrochloride extended-release tablets concomitantly with other tramadol products [ see WARNINGS ].
- Do not administer tramadol hydrochloride extended-release tablets at a dose exceeding 300 mg per day.
- Use the lowest effective dosage for the shortest duration of time consistent with individual patient treatment goals [ see Warnings ] . Because the risk of overdose increases as opioid doses increase, reserve titration to higher doses of tramadol hydrochloride extended-release tablets for patients in whom lower doses are insufficiently effective and in whom the expected benefits of using a higher dose opioid clearly outweigh the substantial risks.
- Initiate the dosing regimen for each patient individually, taking into account the patient’s underlying cause and severity of pain, prior analgesic treatment and response, and risk factors for addiction, abuse, and misuse [ see Warnings ]
- Respiratory depression can occur at any time during opioid therapy, especially when initiating and following dosage increases with tramadol hydrochloride extended-release tablets. Consider this risk when selecting an initial dose and when making dose adjustments [see Warnings ].
- Tramadol hydrochloride extended-release tablets should be taken once daily, at approximately the same time every day.
- Instruct patients to swallow tramadol hydrochloride extended-release tablets whole [see PRECAUTIONS; Information for Patients ], and to take it with liquid. Crushing, chewing, splitting, or dissolving tramadol hydrochloride extended-release tablets will result in uncontrolled delivery of tramadol and can lead to overdose or death [ see WARNINGS ] .
- Tramadol hydrochloride extended-release tablets may be taken without regard to food, it is recommended that it be taken in a consistent manner [see CLINICAL PHARMACOLOGY ] .
Patient Access to an Opioid Overdose Reversal Agent for the Emergency Treatment of Opioid Overdose
Inform patients and caregivers about opioid overdose reversal agents (e.g., naloxone, nalmefene). Discuss the importance of having access to an opioid overdose reversal agent, especially if the patient has risk factors for overdose (e.g., concomitant use of CNS depressants, a history of opioid use disorder, or prior opioid overdose) or if there are household members (including children) or other close contacts at risk for accidental ingestion or opioid overdose. The presence of risk factors for overdose should not prevent the management of pain in any patient [see WARNINGS; Addiction, Abuse, and Misuse; Life-Threatening Respiratory Depression; Risks from Concomitant Use with Benzodiazepines or Other CNS Depressants ].
Discuss the options for obtaining an opioid overdose reversal agent (e.g., prescription, over-the-counter, or as part of a community-based program).
There are important differences among the opioid overdose reversal agents, such as route of administration, product strength, approved patient age range, and pharmacokinetics. Be familiar with these differences, as outlined in the approved labeling for those products, prior to recommending or prescribing such an agent.
Initial Dosage
It is safer to underestimate a patient’s 24-hour tramadol requirements and provide rescue medication (e.g., immediate-release opioid) than to overestimate the 24-hour tramadol dosage and manage an adverse reaction due to an overdose. While useful tables of opioid equivalents are readily available, there is inter-patient variability in the potency of opioid drugs and opioid formulations. Frequently reevaluate patients for signs and symptoms of opioid withdrawal and for signs of oversedation/toxicity after converting patients to Tramadol Hydrochloride Extended-Release Tablets.
Use of Tramadol Hydrochloride Extended-Release Tablets The initial dose of tramadol hydrochloride extended-release tablets is 100 mg once daily.
Patients Currently on Tramadol Immediate-Release (IR) Products
Calculate the 24-hour tramadol IR dose and initiate a total daily dose of tramadol hydrochloride extended-release tablets rounded down to the next lower 100 mg increment. The dose should be taken once daily. The dose may subsequently be individualized according to patient need.
Due to limitations in flexibility of dose selection with tramadol hydrochloride extended-release tablets, some patients maintained on tramadol IR products may not be able to convert to tramadol hydrochloride extended-release tablets.
Conversion from Other Opioid Analgesics to Tramadol Hydrochloride Extended-Release Tablets
When tramadol hydrochloride extended-release tablets therapy is initiated, discontinue all opioid analgesics other than those used on an as needed basis for breakthrough pain when appropriate. There are no established conversion ratios for conversion from other opioids to tramadol hydrochloride extended-release tablets defined by clinical trials. It is safer to underestimate a patient’s 24-hour tramadol requirements and provide rescue medication (e.g., immediate-release opioid) than to overestimate the 24-hour tramadol dosage and manage an adverse reaction due to an overdose. While useful tables of opioid equivalents are readily available, there is inter-patient variability in the potency of opioid drugs and opioid formulations. Frequently reevaluate patients for signs and symptoms of opioid withdrawal and for signs of oversedation/toxicity after converting patients to Tramadol Hydrochloride Extended-Release Tablets.
Use of Tramadol Hydrochloride Extended-Release Tablets The initial dose of tramadol hydrochloride extended-release tablets is 100 mg once daily.
Titration and Maintenance of Therapy
Individually titrate tramadol hydrochloride extended-release tablets by 100 mg every five days to a dose that provides adequate analgesia and minimizes adverse reactions. The maximum daily dose of tramadol hydrochloride extended-release tablets is 300 mg per day.
Continually reevaluate patients receiving tramadol hydrochloride extended-release tablets to assess the maintenance of pain control and, signs and symptoms of opioid withdrawal, and other adverse reactions as well as to reassess for the development of addiction, abuse, or misuse [see Warnings and Withdrawal ] . Frequent communication is important among the prescriber, other members of the healthcare team, the patient, and the caregiver/family during periods of changing analgesic requirements, including initial titration. During use of opioid therapy for an extended period of time, periodically reassess the continued need for the use of opioid analgesics.
Patients who experience breakthrough pain may require a dosage adjustment of tramadol hydrochloride extended-release tablets, or may need rescue medication with an appropriate dose of an immediate-release analgesic.
If the level of pain increases after dosage stabilization, attempt to identify the source of increased pain before increasing the tramadol hydrochloride extended-release tablets dosage.
If after increasing the dosage, unacceptable opioid-related adverse reactions are observed (including an increase in pain after dosage increase), consider reducing the dosage [see Warnings ] . Adjust the dosage to obtain an appropriate balance between management of pain and opioid-related adverse reactions.
Safe Reduction or Discontinuation of Tramadol Hydrochloride Extended-Release Tablets
Do not rapidly reduce or abruptly discontinue tramadol hydrochloride extended-release tablets in patients who may be physically dependent on opioids. Rapid reduction or abrupt discontinuation of opioid analgesics in patients who are physically dependent on opioids has resulted in serious withdrawal symptoms, uncontrolled pain, and suicide. Rapid reduction or abrupt discontinuation has also been associated with attempts to find other sources of opioid analgesics, which may be confused with drug-seeking for abuse. Patients may also attempt to treat their pain or withdrawal symptoms with illicit opioids, such as heroin, and other substances.
When a decision has been made to decrease the dose or discontinue therapy in an opioid-dependent patient taking tramadol hydrochloride extended-release tablets, there are a variety of factors that should be considered, including the total daily dose of opioid (including tramadol hydrochloride extended-release tablets) the patient has been taking, the duration of treatment, the type of pain being treated, and the physical and psychological attributes of the patient. It is important to ensure ongoing care of the patient and to agree on an appropriate tapering schedule and follow-up plan so that patient and provider goals and expectations are clear and realistic. When opioid analgesics are being discontinued due to a suspected substance use disorder, evaluate and treat the patient, or refer for evaluation and treatment of the substance use disorder. Treatment should include evidence-based approaches, such as medication assisted treatment of opioid use disorder. Complex patients with co-morbid pain and substance use disorders may benefit from referral to a specialist.
There are no standard opioid tapering schedules that are suitable for all patients. Good clinical practice dictates a patient-specific plan to taper the dose of the opioid gradually. For patients on tramadol hydrochloride extended-release tablets who are physically opioid-dependent, initiate the taper by a small enough increment (e.g., no greater than 10% to 25% of the total daily dose) to avoid withdrawal symptoms, and proceed with dose lowering at an interval of every 2 to 4 weeks. Patients who have been taking opioids for briefer periods of time may tolerate a more rapid taper.
It may be necessary to provide the patient with lower dosage strengths to accomplish a successful taper. Reassess the patient frequently to manage pain and withdrawal symptoms, should they emerge. Common withdrawal symptoms include restlessness, lacrimation, rhinorrhea, yawning, perspiration, chills, myalgia, and mydriasis. Other signs and symptoms also may develop, including irritability, anxiety, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhea, or increased blood pressure, respiratory rate, or heart rate. If withdrawal symptoms arise, it may be necessary to pause the taper for a period of time or raise the dose of the opioid analgesic to the previous dose, and then proceed with a slower taper. In addition, evaluate patients for any changes in mood, emergence of suicidal thoughts, or use of other substances.
When managing patients taking opioid analgesics, particularly those who have been treated for an extended period of time, and/or with high doses for chronic pain, ensure that a multimodal approach to pain management, including mental health support (if needed), is in place prior to initiating an opioid analgesic taper. A multimodal approach to pain management may optimize the treatment of chronic pain, as well as assist with the successful tapering of the opioid analgesic [see WARNINGS/ Withdrawal, DRUG ABUSE and DEPENDENCE ].
CONTRAINDICATIONS
Tramadol hydrochloride extended-release tablets are contraindicated for:
- all children younger than 12 years of age [see WARNINGS ].
- postoperative management in children younger than 18 years of age following tonsillectomy and/or adenoidectomy [ see WARNINGS ].
Tramadol hydrochloride extended-release tablets are also contraindicated in patients with:
- Significant respiratory depression [see WARNINGS ]
- Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment [see WARNINGS ]
- Known or suspected gastrointestinal obstruction, including paralytic ileus [see WARNINGS ]
- Hypersensitivity to tramadol (e.g., anaphylaxis) [see ADVERSE REACTIONS ]
- Concurrent use of monoamine oxidase inhibitors (MAOIs) or use within the last 14 days [see PRECAUTIONS; Drug Interactions ]
ADVERSE REACTIONS
The following serious adverse reactions are described, or described in greater detail, in other sections:
- Addiction, Abuse, and Misuse (see WARNINGS )
- Life-Threatening Respiratory Depression (see WARNINGS )
- Ultra-Rapid Metabolism of Tramadol and Other Risk Factors for Life-Threatening Respiratory Depression in Children (see WARNINGS )
- Neonatal Opioid Withdrawal Syndrome (see WARNINGS )
- Interactions with Benzodiazepines or Other CNS Depressants (see WARNINGS )
- Opioid-Induced Hyperalgesia and Allodynia (see WARNINGS )
- Serotonin Syndrome (see WARNINGS )
- Seizures (see WARNINGS )
- Suicide (see WARNINGS )
- Adrenal Insufficiency (see WARNINGS )
- Severe Hypotension (see WARNINGS )
- Gastrointestinal Adverse Reactions (see WARNINGS )
- Hypersensitivity Reactions (see WARNINGS )
- Withdrawal (see WARNINGS )
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Tramadol hydrochloride extended-release tablets were administered to a total of 2707 subjects (2406 patients and 301 healthy volunteers) during clinical studies, including four randomized double-blind studies (treatment ≥ 12 weeks) and two open-label long-term studies (treatment up to 12 months) in patients with moderate to severe pain due to osteoarthritis of the knee. A total of 844 patients were exposed to tramadol hydrochloride extended-release tablets for 12 weeks, 493 patients for 6 months and 243 patients for 12 months. Treatment emergent adverse events increased with dose from 100 mg to 300 mg in the three twelve-week, randomized, double-blind, placebo-controlled studies (Table 2).
| ADVERSE EVENTS (MEDRA Preferred Terms) | Tramadol Hydrochloride Extended-Release Tablets | Placebo | |||
| 100 mg | 200 mg | 300 mg | Total • | ||
| N=216 | N=311 | N=530 | N=1095 | N=668 | |
| Nausea | 28 (13%) | 42 (14%) | 76 (14%) | 179 (16%) | 37 (6%) |
| Constipation | 21 (10%) | 36 (12%) | 52 (10%) | 140 (13%) | 26 (4%) |
| Dizziness | 16 (7%) | 28 (9%) | 52 (10%) | 106 (10%) | 18 (3%) |
| Somnolence | 11 (5%) | 22 (7%) | 23 (4%) | 77 (7%) | 12 (2%) |
| Vomiting | 7 (3%) | 16 (5%) | 31 (6%) | 58 (5%) | 4 (1%) |
| Pruritus | 9 (4%) | 15 (5%) | 18 (3%) | 51 (5%) | 7 (1%) |
| Headache | 10 (5%) | 9 (3%) | 15 (3%) | 41 (4%) | 21 (3%) |
| Sweating increased | 1 (0%) | 9 (3%) | 14 (3%) | 35 (3%) | 5 (1%) |
| Dry mouth | 7 (3%) | 13 (4%) | 6 (1%) | 32 (3%) | 8 (1%) |
| Fatigue | 6 (3%) | 7 (2%) | 9 (2%) | 26 (2%) | 6 (1%) |
| Anorexia | 4 (2%) | 4 (1%) | 10 (2%) | 25 (2%) | 2 (0%) |
| Vertigo | 2 (1%) | 3 (1%) | 6 (1%) | 21 (2%) | 3 (0%) |
| Insomnia | 2 (1%) | 6 (2%) | 9 (2%) | 18 (2%) | 8 (1%) |
The majority of patients who experienced the most common adverse events (≥5%) reported mild to moderate symptoms. Less than 3% of adverse events were rated as severe. Overall, onset of these adverse events usually occurred within the first two weeks of treatment.
Adverse reactions with an incidence of 1.0% to <5.0%
Ear and labyrinth disorders: vertigo
Gastrointestinal disorders: abdominal pain, diarrhea, dry mouth, dyspepsia, upper abdominal pain
General disorders : fatigue, weakness
Investigations: weight decreased
Metabolism and nutrition disorders : anorexia
Musculoskeletal and connective tissue disorders: arthralgia
Nervous system disorders : headache, tremor
Psychiatric disorders : anxiety, insomnia
Skin and subcutaneous tissue disorders : pruritus, sweating increased
Vascular disorders: hot flushes
Adverse reactions with an incidence of <1.0%
Blood and lymphatic system disorders: anemia, thrombocytopenia
Cardiac disorders : bradycardia
Eye disorders: blurred vision, visual disturbance
Gastrointestinal disorders : abdominal discomfort, abdominal distension, abdominal tenderness, change in bowel habit, constipation aggravated, diverticulitis, diverticulum, dyspepsia aggravated, dysphagia, fecal impaction, gastric irritation, gastritis, gastrointestinal hemorrhage, gastrointestinal irritation, gastro-esophageal reflux disease, lower abdominal pain, pancreatitis aggravated, rectal hemorrhage, rectal prolapse, retching
General disorders : asthenia, malaise
Hepatobiliary disorders: biliary tract disorder, cholelithiasis
Immune system disorders: hypersensitivity
Investigations : alanine aminotransferase decreased, alanine aminotransferase increased, aspartate aminotransferase decreased, aspartate aminotransferase increased, blood amylase increased, blood creatinine increased, blood in stool, blood potassium abnormal, blood pressure increased gamma glutamyltransferase increased
Metabolism and nutrition disorders : appetite decreased, dehydration
Nervous system disorders : ataxia, disturbance in attention, dysarthria, gait abnormal, headache aggravated, mental impairment, sedation, seizure, sleep apnea syndrome, syncope, tremor
Psychiatric disorders : abnormal behavior, agitation, anxiety, confusion, depression, emotional disturbance, euphoric mood, indifference, irritability, libido decreased, nervousness, sleep disorder
Renal and urinary disorders : difficulty in micturition, urinary hesitation, urinary retention
Reproductive system and breast disorders : erectile dysfunction, sexual dysfunction
Respiratory, thoracic and mediastinal disorders : dyspnea
Skin and subcutaneous tissue disorders : allergic dermatitis, cold sweat, dermatitis, night sweats, pallor, generalized pruritus, urticaria
Vascular disorders : flushing, hypertension, hypotension, orthostatic hypotension
Postmarketing Experience
The following adverse reactions have been identified during post approval use of tramadol. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Serotonin syndrome: Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of opioids with serotonergic drugs.
- Adrenal insufficiency: Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use.
- Anaphylaxis: Anaphylaxis has been reported with ingredients contained in tramadol hydrochloride extended-release tablets.
- Androgen deficiency: Cases of androgen deficiency have occurred with use of opioids for an extended period of time .
- Hyperalgesia and Allodynia : Cases of hyperalgesia and allodynia have been reported with opioid therapy of any duration [see Warnings]
- Hyponatremia: Cases of severe hyponatremia and/or SIADH have been reported in patients taking tramadol, most often in females over the age of 65, and within the first week of therapy [see PRECAUTIONS ].
- Hypoglycemia: Cases of hypoglycemia have been reported in patients taking tramadol. Most reports were in patients with predisposing risk factors, including diabetes or renal insufficiency, or in elderly patients [see PRECAUTIONS ].
- Opioid-induced esophageal dysfunction (OIED): Cases of OIED have been reported in patients taking opioids, and may occur more frequently in patients taking higher doses of opioids, and/or in patients taking opioids longer term [see WARNINGS ].
Adverse Reactions from Observational Studies
A prospective, observational cohort study estimated the risks of addiction, abuse, and misuse in patients initiating long-term use of Schedule II opioid analgesics between 2017 and 2021. Study participants included in one or more analyses had been enrolled in selected insurance plans or health systems for at least one year, were free of at least one outcome at baseline, completed a minimum number of follow-up assessments, and either: 1) filled multiple extended-release/long-acting opioid analgesic prescriptions during a 90 day period (n=978); or 2) filled any Schedule II opioid analgesic prescriptions covering at least 70 of 90 days (n=1,244). Those included also had no dispensing of the qualifying opioids in the previous 6 months.
Over 12 months: • approximately 1% to 6% of participants across the two cohorts newly met criteria for addiction, as assessed with two validated interview-based measures of moderate-to-severe opioid use disorder based on Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) criteria, and • approximately 9% and 22% of participants across the two cohorts newly met criteria for prescription opioid abuse and misuse [defined in DRUG ABUSE AND DEPENDENCE], respectively, as measured with a validated self-reported instrument.
A retrospective, observational cohort study estimated the risk of opioid-involved overdose or opioid overdose-related death in patients with new long-term use of Schedule II opioid analgesics from 2006 through 2016 (n=220,249). Included patients had been enrolled in either one of two commercial insurance programs, one managed care program, or one Medicaid program for at least 9 months. New long-term use was defined as having Schedule II opioid analgesic prescriptions covering at least 70 days’ supply over the 3 months prior to study entry and none during the preceding 6 months. Patients were excluded if they had an opioid-involved overdose in the 9 months prior to study entry. Overdose was measured using a validated medical code-based algorithm with linkage to the National Death Index database. The 5-year cumulative incidence estimates for opioid-involved overdose or opioid overdose-related death ranged from approximately 1.5% to 4% across study sites, counting only the first event during follow-up. Approximately 17% of first opioid overdoses observed over the entire study period (5-11 years, depending on the study site) were fatal. Higher baseline opioid dose was the strongest and most consistent predictor of opioid-involved overdose or opioid overdose-related death. Study exclusion criteria may have selected patients at lower risk of overdose, and substantial loss to follow-up (approximately 80%) also may have biased estimates.
The risk estimates from the studies described above may not be generalizable to all patients receiving opioid analgesics, such as those with exposures shorter or longer than the duration evaluated in the studies.
DRUG ABUSE AND DEPENDENCE
Controlled Substance
Tramadol hydrochloride extended-release tablets contain tramadol, a Schedule IV controlled substance.
Abuse
Tramadol hydrochloride extended-release tablets contain tramadol, a substance with high potential for misuse and abuse, which can lead to the development of substance use disorder, including addiction [see Warnings ] .
Misuse is the intentional use, for therapeutic purposes, of a drug by an individual in a way other than prescribed by a healthcare provider or for whom it was not prescribed.
Abuse is the intentional, non-therapeutic use of a drug, even once, for its desirable psychological or physiological effects.
Drug addiction is a cluster of behavioral, cognitive, and physiological phenomena that may include a strong desire to take the drug, difficulties in controlling drug use (e.g., continuing drug use despite harmful consequences, giving a higher priority to drug use than other activities and obligations), and possible tolerance or physical dependence.
Misuse and abuse of tramadol hydrochloride extended-release tablets increases risk of overdose, which may lead to central nervous system and respiratory depression, hypotension, seizures, and death. The risk is increased with concurrent use of tramadol hydrochloride extended-release tablets with alcohol and/or other CNS depressants. Abuse of and addiction to opioids in some individuals may not be accompanied by concurrent tolerance and symptoms of physical dependence. In addition, abuse of opioids can occur in the absence of addiction.
All patients treated with opioids require careful and frequent re-evaluation for signs of misuse, abuse, and addiction, because use of opioid analgesic products carries the risk of addiction even under appropriate medical use. Patients at high risk of tramadol hydrochloride extended-release tablets abuse include those with a history of prolonged use of any opioids, including products containing tramadol, those with a history of drug or alcohol abuse, or those who use tramadol hydrochloride extended-release tablets in combination with other abused drugs.
“Drug-seeking” behavior is very common in persons with substance use disorders. Drug-seeking tactics include emergency calls or visits near the end of office hours, refusal to undergo appropriate examination, testing, or referral, repeated “loss” of prescriptions, tampering with prescriptions, and reluctance to provide prior medical records or contact information for other treating healthcare provider(s). “Doctor shopping” (visiting multiple prescribers to obtain additional prescriptions) is common among people who abuse drugs and people with substance use disorder. Preoccupation with achieving adequate pain relief can be appropriate behavior in a patient with inadequate pain control.
Tramadol hydrochloride extended-release tablets, like other opioids, can be diverted for nonmedical use into illicit channels of distribution. Careful record-keeping of prescribing information, including quantity, frequency, and renewal requests, as required by state and federal law, is strongly advised.
Proper assessment of the patient, proper prescribing practices, periodic reevaluation of therapy, and proper dispensing and storage are appropriate measures that help to limit abuse of opioid drugs.
Risks Specific to Abuse of Tramadol Hydrochloride Extended-Release Tablets
Abuse of tramadol hydrochloride extended-release tablets poses a risk of overdose and death.
Tramadol hydrochloride extended-release tablets are approved for oral use only. Inappropriate intravenous, intramuscular, or subcutaneous use of tramadol hydrochloride extended-release tablets can result in local tissue necrosis, infection, pulmonary granulomas, increased risk of endocarditis and valvular heart injury, embolism, and death.
Parenteral drug abuse is commonly associated with transmission of infectious diseases such as hepatitis and HIV.
Dependence
Both tolerance and physical dependence can develop during use of opioid therapy.
Tolerance is a physiological state characterized by a reduced response to a drug after repeated administration (i.e., a higher dose of a drug is required to produce the same effect that was once obtained at a lower dose).
Physical dependence is a state that develops as a result of a physiological adaptation in response to repeated drug use, manifested by withdrawal signs and symptoms after abrupt discontinuation or a significant dose reduction of a drug.
Withdrawal may be precipitated through the administration of drugs with opioid antagonist activity (e.g., naloxone, nalmefene), mixed agonist/antagonist analgesics (e.g., pentazocine, butorphanol, nalbuphine), or partial agonists (e.g., buprenorphine). Physical dependence may not occur to a clinically significant degree until after several days to weeks of continued use.
Do not rapidly reduce or abruptly discontinue tramadol hydrochloride extended-release tablets in a patient physically dependent on opioids. Rapid reduction or abrupt discontinuation of tramadol hydrochloride extended-release tablets in a patient physically dependent on opioids may lead to serious withdrawal symptoms, uncontrolled pain, and suicide. Rapid reduction or abrupt discontinuation has also been associated with attempts to find other sources of opioid analgesics, which may be confused with drug-seeking for abuse.
When discontinuing tramadol hydrochloride extended-release tablets, gradually taper the dosage using a patient-specific plan that considers the following: the dose of tramadol hydrochloride extended-release tablets the patient has been taking, the duration of treatment, and the physical and psychological attributes of the patient. To improve the likelihood of a successful taper and minimize withdrawal symptoms, it is important that the opioid tapering schedule is agreed upon by the patient. In patients taking opioids for an extended period of time at high doses, ensure that a multimodal approach to pain management, including mental health support (if needed), is in place prior to initiating an opioid analgesic taper [see Dosage and Administration , and Warnings ] .
Infants born to mothers physically dependent on opioids will also be physically dependent and may exhibit respiratory difficulties and withdrawal signs [see Precautions; Pregnancy ] .
Drug Interactions
Inhibitors of CYP2D6
The concomitant use of tramadol hydrochloride extended-release tablets and CYP2D6 inhibitors such as quinidine, fluoxetine, paroxetine and bupropion may result in an increase in the plasma concentration of tramadol and a decrease in the plasma concentration of M1, particularly when an inhibitor is added after a stable dose of tramadol hydrochloride extended-release tablets is achieved. Since M1 is a more potent μ-opioid agonist, decreased M1 exposure could result in decreased therapeutic effects, and may result in signs and symptoms of opioid withdrawal in patients who had developed physical dependence to tramadol. Increased tramadol exposure can result in increased or prolonged therapeutic effects and increased risk for serious adverse events including seizures and serotonin syndrome.
After stopping a CYP2D6 inhibitor, as the effects of the inhibitor decline, the tramadol plasma concentration will decrease and the M1 plasma concentration will increase which could increase or prolong therapeutic effects but also increase adverse reactions related to opioid toxicity, and may cause potentially fatal respiratory depression [see CLINICAL PHARMACOLOGY ] .
If concomitant use of a CYP2D6 inhibitor is necessary, follow patients closely for adverse reactions including opioid withdrawal, seizures and serotonin syndrome.
If a CYP2D6 inhibitor is discontinued, consider lowering tramadol hydrochloride extended-release tablets dosage until stable drug effects are achieved. Evaluate patients at frequent intervals for adverse events including respiratory depression and sedation.
Inhibitors of CYP3A4
The concomitant use of tramadol hydrochloride extended-release tablets and CYP3A4 inhibitors such as macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g. ketoconazole), protease inhibitors (e.g., ritonavir) can increase the plasma concentration of tramadol and may result in a greater amount of metabolism via CYP2D6 and greater levels of M1. Follow patients closely for increased risk of serious adverse events including seizures and serotonin syndrome, and adverse reactions related to opioid toxicity including potentially fatal respiratory depression, particularly when an inhibitor is added after a stable dose of tramadol hydrochloride extended-release tablets is achieved.
After stopping a CYP3A4 inhibitor, as the effects of the inhibitor decline, the tramadol plasma concentration will decrease [see CLINICAL PHARMACOLOGY ] , resulting in decreased opioid efficacy and possibly signs and symptoms of opioid withdrawal in patients who had developed physical dependence to tramadol.
If concomitant use is necessary, consider dosage reduction of tramadol hydrochloride extended-release tablets until stable drug effects are achieved. Inform patients and caregivers of this potential interaction, educate them on the signs and symptoms of seizures, serotonin syndrome, and signs of respiratory depression and sedation.
If a CYP3A4 inhibitor is discontinued, consider increasing the tramadol hydrochloride extended-release tablets dosage until stable drug effects are achieved and evaluate patients at frequent intervals for signs and symptoms of opioid withdrawal.
CYP3A4 Inducers
The concomitant use of tramadol hydrochloride extended-release tablets and CYP3A4 inducers such as rifampin, carbamazepine, phenytoin can decrease the plasma concentration of tramadol, [see CLINICAL PHARMACOLOGY ] , resulting in decreased efficacy or onset of a withdrawal syndrome in patients who have developed physical dependence to tramadol [see WARNINGS ] .
After stopping a CYP3A4 inducer, as the effects of the inducer decline, the tramadol plasma concentration will increase [see CLINICAL PHARMACOLOGY ] , which could increase or prolong both the therapeutic effects and adverse reactions, and may cause seizures and serotonin syndrome, and potentially fatal respiratory depression.
If concomitant use is necessary, consider increasing the tramadol hydrochloride extended-release tablets dosage until stable drug effects are achieved. Evaluate patients for signs of opioid withdrawal. If a CYP3A4 inducer is discontinued, consider tramadol hydrochloride extended-release tablets dose reduction and evaluate patients at frequent intervals for signs of respiratory depression and sedation.
Patients taking carbamazepine, a CYP3A4 inducer, may have a significantly reduced analgesic effect of tramadol. Because carbamazepine increases tramadol metabolism and because of the seizure risk associated with tramadol, concomitant administration of tramadol hydrochloride extended-release tablets and carbamazepine is not recommended.
Benzodiazepines and Other Central Nervous System (CNS) Depressants
Due to additive pharmacologic effect, the concomitant use of benzodiazepines or other CNS depressants such as alcohol, other sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, and other opioids, can increases the risk of respiratory depression, profound sedation, coma, and death.
Reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate. Limit dosages and durations to the minimum required. Inform patients and caregivers of this potential interaction, educate them on the signs and symptoms of respiratory depression (including sedation). If concomitant use is warranted, consider recommending or prescribing an opioid overdose reversal agent. [see WARNINGS, DOSAGE AND ADMINISTRATION].
Serotonergic Drugs
The concomitant use of opioids with other drugs that affect the serotonergic neurotransmitter system such as selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that affect the serotonin neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (i.e., cyclobenzaprine, metaxalone), monoamine oxidase (MAO) inhibitors (those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue) has resulted in serotonin syndrome.
If concomitant use is warranted, carefully observe the patient, particularly during treatment initiation and dose adjustment. Discontinue tramadol hydrochloride extended-release tablets if serotonin syndrome is suspected.
Monoamine Oxidase Inhibitors (MAOIs)
MAOI interactions with opioids may manifest as serotonin syndrome [see WARNINGS ] or opioid toxicity (e.g., respiratory depression, coma) [see WARNINGS ].
Do not use tramadol hydrochloride extended-release tablets in patients taking MAOIs or within 14 days of stopping such treatment.
Mixed Agonist/Antagonist and Partial Agonist Opioid Analgesics
Mixed agonist/antagonist and partial agonist opioid analgesics such as butorphanol, nalbuphine, pentazocine, buprenorphine, may reduce the analgesic effect of tramadol hydrochloride extended-release tablets and/or precipitate withdrawal symptoms. Advise patient to avoid concomitant use of these drugs.
Muscle Relaxants
Tramadol hydrochloride extended-release tablets may enhance the neuromuscular blocking action of skeletal muscle relaxants and produce an increased degree of respiratory depression.
Because respiratory depression may be greater than otherwise expected, decrease the dosage of tramadol hydrochloride extended-release tablets and/or the muscle relaxant as necessary. Due to the risk of respiratory depression with concomitant use of muscle relaxants and opioids, consider recommending or prescribing an opioid overdose reversal agent [see WARNINGS, DOSAGE AND ADMINISTRATION].
Diuretics
Opioids can reduce the efficacy of diuretics by inducing the release of antidiuretic hormone.
Evaluate patients for signs of diminished diuresis and/or effects on blood pressure and increase the dosage of the diuretic as needed.
Anticholinergic Drugs
The concomitant use of anticholinergic drugs may increase risk of urinary retention and/or severe constipation, which may lead to paralytic ileus.
Evaluate patients for signs of urinary retention or reduced gastric motility when tramadol hydrochloride extended-release tablets are used concomitantly with anticholinergic drugs.
Digoxin
Postmarketing surveillance has revealed rare reports of digoxin toxicity. Follow patients for signs of digoxin toxicity and adjust dosage of digoxin as needed.
Warfarin
Postmarketing surveillance of tramadol has revealed rare reports of alteration of warfarin effect, including elevation of prothrombin times. Monitor the prothrombin time of patients on warfarin for signs of an interaction and adjust the dosage of warfarin as needed.
DESCRIPTION
Tramadol hydrochloride extended-release tablets, USP are an opioid agonist composed of a matrix delivery system with extended-release characteristics. The chemical name for tramadol hydrochloride, USP is (±) cis -2-[(dimethylamino) methyl]-1-(3 methoxyphenyl) cyclohexanol hydrochloride. Its structural formula is: 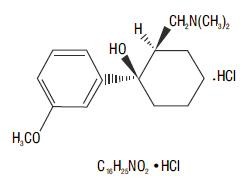
The molecular weight of tramadol hydrochloride, USP is 299.8. Tramadol hydrochloride, USP is a white crystalline powder that is freely soluble in water and ethanol. Tramadol hydrochloride extended-release tablets, USP are for oral administration and contain 100 mg, 200 mg or 300 mg of tramadol hydrochloride, USP. The tablets are white in color. The inactive ingredients in the tablet are pregelatinized maize starch, hypromellose, mannitol, magnesium stearate, cellulose acetate and polyethylene glycol.
Imprinting ink contains shellac glaze, iron oxide black, N-butyl alcohol, propylene glycol and ammonium hydroxide.
Meets USP dissolution test 4.
CLINICAL PHARMACOLOGY
Mechanism of Action
Tramadol hydrochloride extended-release tablets, contain tramadol, an opioid agonist inhibitor of norepinenphrine and serotonin re-uptake. Although the mode of action of tramadol is not completely understood, the analgesic effect of tramadol is believed to be due to binding to μ-opioid receptors and weak inhibition of reuptake of norepinephrine and serotonin.
Opioid activity of tramadol is due to both low affinity binding of the parent compound and higher affinity binding of the O -demethylated metabolite (M1) to mu-opioid receptors. In animal models, M1 is up to 6 times more potent than tramadol in producing analgesia and 200 times more potent in mu-opioid binding. Tramadol-induced analgesia is only partially antagonized by the opiate antagonist naloxone in several animal tests. The relative contribution of both tramadol and M1 to human analgesia is dependent upon the plasma concentrations of each compound.
Tramadol has been shown to inhibit reuptake of norepinephrine and serotonin in vitro , as have some other opioid analgesics. These mechanisms may contribute independently to the overall analgesic profile of tramadol.
Apart from analgesia, tramadol hydrochloride administration may produce various symptoms (including dizziness, somnolence, nausea, constipation, sweating and pruritus) similar to that of other opioids. In contrast to morphine, tramadol has not been shown to cause histamine release. At therapeutic doses, tramadol has no effect on heart rate, left-ventricular function or cardiac index. Orthostatic hypotension has been observed.
Pharmacodynamics
Effects on the Central Nervous System
Tramadol produces respiratory depression by direct action on brain stem respiratory centers. The respiratory depression involves a reduction in the responsiveness of the brain stem respiratory centers to both increases in carbon dioxide tension and electrical stimulation.
Tramadol causes miosis, even in total darkness. Pinpoint pupils are a sign of opioid overdose but are not pathognomonic (e.g., pontine lesions of hemorrhagic or ischemic origins may produce similar findings). Marked mydriasis rather than miosis may be seen due to hypoxia in overdose situations.
Effects on the Gastrointestinal Tract and Other Smooth Muscle
Tramadol causes a reduction in motility associated with an increase in smooth muscle tone in the antrum of the stomach and duodenum. Digestion of food in the small intestine is delayed and propulsive contractions are decreased. Propulsive peristaltic waves in the colon are decreased, while tone may be increased to the point of spasm, resulting in constipation. Other opioid-induced effects may include a reduction in biliary and pancreatic secretions, spasm of sphincter of Oddi, transient elevations in serum amylase, and opioid-induced esophageal dysfunction (OIED).
Effects on the Cardiovascular System
Tramadol produces peripheral vasodilation, which may result in orthostatic hypotension or syncope. Manifestations of histamine release and/or peripheral vasodilation may include pruritus, flushing, red eyes, sweating, and/or orthostatic hypotension.
Effects on the Endocrine System
Opioids inhibit the secretion of adrenocorticotropic hormone (ACTH), cortisol, and luteinizing hormone (LH) in humans [see ADVERSE REACTIONS ]. They also stimulate prolactin, growth hormone (GH) secretion, and pancreatic secretion of insulin and glucagon.
Use of opioids for an extended period of time may influence the hypothalamic-pituitary-gonadal axis, leading to androgen deficiency that may manifest as low libido, impotence, erectile dysfunction, amenorrhea, or infertility. The causal role of opioids in the clinical syndrome of hypogonadism is unknown because the various medical, physical, lifestyle, and psychological stressors that may influence gonadal hormone levels have not been adequately controlled for in studies conducted to date [see ADVERSE REACTIONS ].
Effects on the Immune System
Opioids have been shown to have a variety of effects on components of the immune system. The clinical significance of these findings is unknown. Overall, the effects of opioids appear to be modestly immunosuppressive.
Concentration–Efficacy Relationships
The minimum effective analgesic concentration will vary widely among patients, especially among patients who have been previously treated with extended-release agonist opioids. The minimum effective analgesic concentration of tramadol for any individual patient may increase over time due to an increase in pain, the development of a new pain syndrome, and/or the development of analgesic tolerance [see DOSAGE and ADMINISTRATION ].
Concentration–Adverse Reaction Relationships
There is a relationship between increasing tramadol plasma concentration and increasing frequency of dose-related opioid adverse reactions such as nausea, vomiting, CNS effects, and respiratory depression. In opioid-tolerant patients, the situation may be altered by the development of tolerance to opioid-related adverse reactions [see DOSAGE and ADMINISTRATION ].
Pharmacokinetics
Tramadol hydrochloride extended-release tablets are formulated as a racemate and both tramadol and M1 are detected in the circulation.
The pharmacokinetics of tramadol and M1 are dose-proportional over a 100 to 300 mg dose range in healthy subjects.
Absorption
The median time to peak plasma concentrations of tramadol and M1 after multiple-dose administration of a tramadol hydrochloride extended-release tablet 200 mg to healthy subjects are attained at about 4 h and 5 h, respectively (Table 1 and Figure 1).
The pharmacokinetic parameter values of a tramadol hydrochloride extended-release tablet 200 mg administered once daily and tramadol immediate-release 50 mg administered every six hours are provided in Table 1. The relative bioavailability of a 200 mg tramadol hydrochloride extended-release tablet compared to a 50 mg immediate-release tablet dosed every six hours was approximately 95% in healthy subjects.
| Pharmacokinetic Parameter | Tramadol | M1 Metabolite | ||
| Tramadol Hydrochloride Extended-Release 200 mg Tablet Once-Daily | Immediate- Release Tramadol 50 mg Tablet Every 6 Hours | Tramadol Hydrochloride Extended-Release 200 mg Tablet Once-Daily | Immediate- Release Tramadol 50 mg Tablet Every 6 Hours | |
| AUC 0-24 (ng·h/mL) | 5991 (22) | 6399 (28) | 1361 (27) | 1438 (23) |
| C max (ng/mL) | 345 (21) | 423 (23) | 71 (27) | 79 (22) |
| C min (ng/mL) | 157 (31) | 190 (34) | 41 (30) | 50 (29) |
| T max (hr) Tmax is presented as Median (Range) | 4.0 (3.0 to 9.0) | 1.0 (1.0 to 3.0) | 5.0 (3.0 to 20) | 1.5 (1.0 to 3.0) |
| Fluctuation (%) | 77 (26) | 91 (22) | 53 (29) | 49 (26) |
Steady-state plasma concentrations are reached within approximately 48 hours. Figure 1. Mean Tramadol Plasma Concentrations at Steady State Following Five Days of Oral Administration of A Tramadol Hydrochloride Extended-Release Tablet 200 mg Once Daily and Immediate-Release Tramadol 50 mg Every 6 Hours. 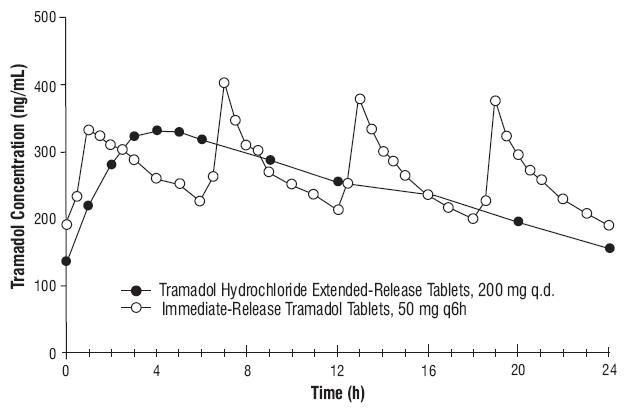 Figure 2. Mean M1 Plasma Concentrations at Steady State Following Five Days of Oral Administration of A Tramadol Hydrochloride Extended-Release Tablet 200 mg Once Daily and Immediate-Release Tramadol 50 mg Every 6 Hours
Figure 2. Mean M1 Plasma Concentrations at Steady State Following Five Days of Oral Administration of A Tramadol Hydrochloride Extended-Release Tablet 200 mg Once Daily and Immediate-Release Tramadol 50 mg Every 6 Hours 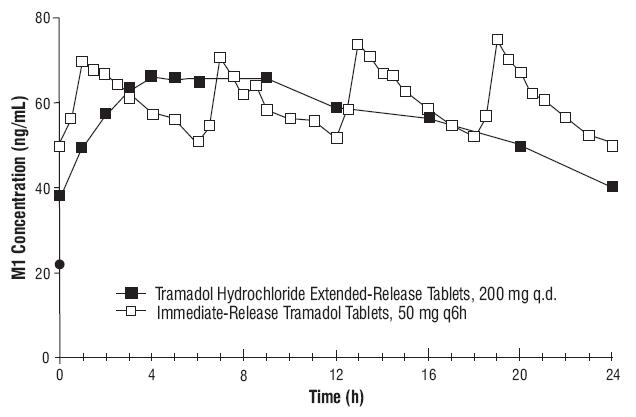 Food Effect
Food Effect
Coadministration with a high fat meal did not significantly affect AUC (overall exposure to tramadol); however, C max (peak plasma concentration) increased 67% following a single 300 mg tablet administration and 54% following a single 200 mg tablet administration. Tramadol hydrochloride extended-release tablets were administered without regard to food in all clinical trials.
Distribution
The volume of distribution of tramadol is 2.6 and 2.9 L/kg in males and females, respectively, following a 100 mg intravenous dose. The binding of tramadol to human plasma proteins is approximately 20%. Protein binding also appears to be independent of concentration up to 10 mcg/mL. Saturation of plasma protein binding occurs only at concentrations outside the clinically relevant range.
Elimination
After single administration of tramadol hydrochloride extended-release tablets, the mean terminal plasma elimination half-lives of racemic tramadol and racemic M1 are 6.5 ± 1.5 and 7.5 ± 1.4 hours, respectively.
Metabolism
Tramadol is extensively metabolized after oral administration. The major metabolic pathways appear to be N- and O- demethylation and glucuronidation or sulfation in the liver. N -demethylation is mediated by CYP3A4 and CYP2B6. One metabolite ( O -desmethyltramadol, denoted M1) is pharmacologically active in animal models. Formation of M1 is dependent on CYP2D6 and as such is subject to inhibition and polymorphism, which may affect the therapeutic response [see PRECAUTIONS - Drug Interactions ] .
Excretion
Approximately 30% of the dose is excreted in the urine as unchanged drug, whereas 60% of the dose is excreted as metabolites. The remainder is excreted either as unidentified or as unextractable metabolites.
Special Populations
Hepatic Impairment
The metabolism of tramadol and M1 is reduced in patients with advanced cirrhosis of the liver, resulting in both a larger area under the concentration time curve (AUC) for tramadol and longer mean tramadol and M1 elimination half-lives (13 hours for tramadol and 19 hours for M1) after the administration of tramadol immediate-release tablets. Tramadol hydrochloride extended-release tablets have not been studied in patients with hepatic impairment. The limited availability of dose strengths and once daily dosing of tramadol hydrochloride extended-release tablets do not permit the dosing flexibility required for safe use in patients with hepatic impairment. Therefore, tramadol hydrochloride extended-release tablets should not be used in patients with hepatic impairment [s ee WARNINGS, Use in Renal and Hepatic Disease and DOSAGE and ADMINISTRATION ].
Renal Impairment
Impaired renal function results in a decreased rate and extent of excretion of tramadol and its active metabolite, M1 in patients taking an immediate-release formulation of tramadol. Tramadol hydrochloride extended-release tablets have not been studied in patients with renal impairment. The limited availability of dose strengths and once daily dosing of tramadol hydrochloride extended-release tablets do not permit the dosing flexibility required for safe use in patients with severe renal impairment. Therefore, tramadol hydrochloride extended-release tablets should not be used in patients with severe renal impairment (creatinine clearance less than 30 mL/min) [see WARNINGS, Use in Renal and Hepatic Disease and DOSAGE and ADMINISTRATION ] . The total amount of tramadol and M1 removed during a 4-hour dialysis period is less than 7% of the administered dose.
Geriatric Patients
Healthy elderly subjects aged 65 to 75 years administered an immediate-release formulation of tramadol, have plasma concentrations and elimination half-lives comparable to those observed in healthy subjects less than 65 years of age. In subjects over 75 years, mean maximum plasma concentrations are elevated (208 vs. 162 ng/mL) and the mean elimination half-life is prolonged (7 vs. 6 hours) compared to subjects 65 to 75 years of age. Adjustment of the daily dose is recommended for patients older than 75 years [s ee DOSAGE and ADMINISTRATION] .
Sex
Following a 100 mg IV dose of tramadol, plasma clearance was 6.4 mL/min/kg in males and 5.7 mL/min/kg in females. Following a single oral dose of immediate-release tramadol, and after adjusting for body weight, females had a 12% higher peak tramadol concentration and a 35% higher area under the concentration-time curve compared to males. The clinical significance of this difference is unknown.
Drug Interaction Studies
Potential for Tramadol to Affect Other Drugs
In vitro studies indicate that tramadol is unlikely to inhibit the CYP3A4-mediated metabolism of other drugs when tramadol is administered concomitantly at therapeutic doses. Tramadol does not appear to induce its own metabolism in humans, since observed maximal plasma concentrations after multiple oral doses are higher than expected based on single-dose data.
Poor/Extensive Metabolizers, CYP2D6
The formation of the active metabolite of tramadol, M1, is mediated by CYP2D6, a polymorphic enzyme. Approximately 7% of the population has reduced activity of CYP2D6. These individuals are "poor metabolizers" of debrisoquine, dextromethorphan and tricyclic antidepressants, among other drugs. In studies in healthy subjects administered immediate-release tramadol products, concentrations of tramadol were approximately 20% higher in "poor metabolizers" versus “extensive metabolizers”, while M1 concentrations were 40% lower.
CYP2D6 Inhibitors
In vitro drug interaction studies in human liver microsomes indicate that concomitant administration with inhibitors of CYP2D6 such as (fluoxetine paroxetine, and amitriptyline could result in some inhibition of the metabolism of tramadol.
Quinidine
Quinidine is a selective inhibitor of CYP2D6, so that concomitant administration of quinidine and tramadol hydrochloride extended-release tablets may result in increased concentrations of tramadol and reduced concentrations of M1. The clinical consequences of these findings are unknown [see PRECAUTIONS ] . In vitro drug interaction studies in human liver microsomes indicate that tramadol has no effect on quinidine metabolism.
CYP3A4 Inhibitors and Inducers
Tramadol is also metabolized by CYP3A4. Administration of CYP3A4 inhibitors such as ketoconazole and erythromycin, or inducers, such as rifampin and St. John’s Wort, with tramadol hydrochloride extended-release tablets may affect the metabolism of tramadol leading to altered tramadol exposure [see PRECAUTIONS ] .
Cimetidine
Concomitant administration of tramadol immediate-release tablets with cimetidine, a weak CYP3A4 inhibitor, does not result in clinically significant changes in tramadol pharmacokinetics. No alteration of the tramadol hydrochloride extended-release tablets dosage regimen with cimetidine is recommended.
Carbamazepine Carbamazepine, a CYP3A4 inducer, increases tramadol metabolism. Patients taking carbamazepine may have a significantly reduced analgesic effect of tramadol. Concomitant administration of tramadol hydrochloride extended-release tablets and carbamazepine is not recommended [see PRECAUTIONS ] .
CLINICAL STUDIES
Tramadol hydrochloride extended-release tablets were studied in four 12-week, randomized, double-blind, controlled studies in patients with moderate to severe pain due to osteoarthritis. Efficacy was demonstrated in one double-blind, placebo-controlled, randomized withdrawal design study. In this study, patients who experienced a reduction of pain and were able to tolerate tramadol hydrochloride extended-release tablets during an open-label titration period, were then randomized to tramadol hydrochloride extended-release tablets or to placebo for 12 weeks. Sixty-five percent of patients were able to successfully titrate onto tramadol hydrochloride extended-release tablets. After a washout, patients randomized to tramadol hydrochloride extended-release tablets were titrated to 200 mg or 300 mg of tramadol hydrochloride extended-release tablets based on tolerability and remained on that dose for the following 12-week period. Approximately 24% of patients discontinued during the randomized period of the study, with more patients discontinuing from the tramadol hydrochloride extended-release tablets arm than the placebo arm due to adverse events (10% vs. 5%, respectively) and more patients discontinuing from the placebo arm than the tramadol hydrochloride extended-release tablets arm due to lack of efficacy (10% vs. 8%, respectively). Patients treated with tramadol hydrochloride extended-release tablets demonstrated a greater improvement in pain intensity, measured on an 11-point numerical rating scale, at the end of treatment compared to patients randomized to placebo. Figure 3 shows the fraction of patients achieving various degree of improvement in pain from baseline to the end of treatment (week 12). The figure is cumulative, so that patients whose change from baseline is, for example, 50%, are also included at every level of improvement below 50%. Patients who did not complete the study were assigned 0% improvement.
Figure 3. Proportion of Patients Achieving Various Levels of Pain Relief as Measured by 12-Week Pain Intensity. 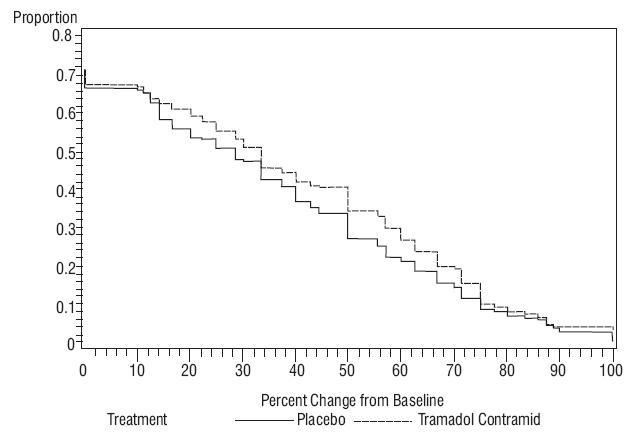
HOW SUPPLIED
Tramadol hydrochloride extended-release tablets, USP are available as follows:
100 mg: White, round shape, biconvex, beveled edge, coated tablet with release portal on the center of the tablet on any one side, imprinted “531” with black ink on one side and plain on other side.
Bottles of 30’s with Child Resistant Cap…………..….NDC 47335-531-83
Bottles of 100’s with Child Resistant Cap………….....NDC 47335-531-88
Bottles of 100’s with Non Child Resistant Cap…….....NDC 47335-531-08
Bottles of 1000’s with Non Child Resistant Cap……...NDC 47335-531-18
200 mg: White, round shape, biconvex, beveled edge, coated tablet with release portal on the center of the tablet on any one side, imprinted “533” with black ink on one side and plain on other side.
Bottles of 30’s with Child Resistant Cap………………NDC 47335-533-83
Bottles of 100’s with Child Resistant Cap……………..NDC 47335-533-88
Bottles of 100’s with Non Child Resistant Cap………..NDC 47335-533-08
Bottles of 1000’s with Non Child Resistant Cap……....NDC 47335-533-18
300 mg: White, round shape, biconvex, beveled edge, coated tablet with release portal on the center of the tablet on any one side, imprinted “537” with black ink on one side and plain on other side.
Bottles of 30’s with Child Resistant Cap…...................NDC 47335-537-83
Bottles of 100’s with Child Resistant Cap….................NDC 47335-537-88
Bottles of 100’s with Non Child Resistant Cap….........NDC 47335-537-08
Bottles of 1000’s with Non Child Resistant Cap….......NDC 47335-537-18
Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° and 30°C (59° and 86°F) [see USP Controlled Room Temperature].
Dispense in a tight, light resistant container.
Warning: keep out of reach of children.
Store tramadol hydrochloride extended-release tablets securely and dispose of properly [see PRECAUTIONS/ Information for Patients ].