Get your patient on Zafirlukast - Zafirlukast tablet, Film Coated (Zafirlukast)
Zafirlukast - Zafirlukast tablet, Film Coated prescribing information
INDICATIONS AND USAGE
Zafirlukast tablets are indicated for the prophylaxis and chronic treatment of asthma in adults and children 5 years of age and older.
DOSAGE AND ADMINISTRATION
Because food can reduce the bioavailability of zafirlukast, zafirlukast tablets should be taken at least 1 hour before or 2 hours after meals.
Adults and Children 12 years of age and older
The recommended dose of zafirlukast tablets in adults and children 12 years and older is 20 mg twice daily.
Pediatric Patients 5 through 11 years of age
The recommended dose of zafirlukast tablets in children 5 through 11 years of age is 10 mg twice daily.
Elderly Patients
Based on cross-study comparisons, the clearance of zafirlukast is reduced in elderly patients (65 years of age and older), such that C max and AUC are approximately twice those of younger adults. In clinical trials, a dose of 20 mg twice daily was not associated with an increase in the overall incidence of adverse events or withdrawals because of adverse events in elderly patients.
Patients with Hepatic Impairment
Zafirlukast tablets are contraindicated in patients with hepatic impairment including hepatic cirrhosis (see Contraindications ). The clearance of zafirlukast is reduced in patients with stable alcoholic cirrhosis such that the C max and AUC are approximately 50 to 60% greater than those of normal adults. Zafirlukast tablets has not been evaluated in patients with hepatitis or in long-term studies of patients with cirrhosis.
Patients with Renal Impairment
Dosage adjustment is not required for patients with renal impairment.
CONTRAINDICATIONS
Zafirlukast tablets are contraindicated in patients who are hypersensitive to zafirlukast or any of its inactive ingredients.
Zafirlukast tablets are contraindicated in patients with hepatic impairment including hepatic cirrhosis.
ADVERSE REACTIONS
Adults and Children 12 years of age and older The safety database for zafirlukast consists of more than 4000 healthy volunteers and patients who received zafirlukast, of which 1723 were asthmatics enrolled in trials of 13 weeks duration or longer. A total of 671 patients received zafirlukast for 1 year or longer. The majority of the patients were 18 years of age or older; however, 222 patients between the age of 12 and 18 years received zafirlukast. A comparison of adverse events reported by ≥1% of zafirlukast-treated patients, and at rates numerically greater than in placebo-treated patients, is shown for all trials in the table below.
| ZAFIRLUKAST | PLACEBO | |
| Adverse Event | N=4058 | N=2032 |
| Headache | 12.9% | 11.7% |
| Infection | 3.5% | 3.4% |
| Nausea | 3.1% | 2.0% |
| Diarrhea | 2.8% | 2.1% |
| Pain (generalized) | 1.9% | 1.7% |
| Asthenia | 1.8% | 1.6% |
| Abdominal Pain | 1.8% | 1.1% |
| Accidental Injury | 1.6% | 1.5% |
| Dizziness | 1.6% | 1.5% |
| Myalgia | 1.6% | 1.5% |
| Fever | 1.6% | 1.1% |
| Back Pain | 1.5% | 1.2% |
| Vomiting | 1.5% | 1.1% |
| SGPT Elevation | 1.5% | 1.1% |
| Dyspepsia | 1.3% | 1.2% |
The frequency of less common adverse events was comparable between zafirlukast and placebo. Rarely, elevations of one or more liver enzymes have occurred in patients receiving zafirlukast in controlled clinical trials. In clinical trials, most of these have been observed at doses four times higher than the recommended dose. The following hepatic events (which have occurred predominantly in females) have been reported from postmarketing adverse event surveillance of patients who have received the recommended dose of zafirlukast (40 mg/day): cases of symptomatic hepatitis (with or without hyperbilirubinemia) without other attributable cause; and rarely, hyperbilirubinemia without other elevated liver function tests. In most, but not all postmarketing reports, the patient’s symptoms abated and the liver enzymes returned to normal or near normal after stopping zafirlukast. In rare cases, patients have presented with fulminant hepatitis or progressed to hepatic failure, liver transplantation and death (see WARNINGS , Hepatotoxicity and PRECAUTIONS , Information for Patients ). In clinical trials, an increased proportion of zafirlukast patients over the age of 55 years reported infections as compared to placebo-treated patients. A similar finding was not observed in other age groups studied. These infections were mostly mild or moderate in intensity and predominantly affected the respiratory tract. Infections occurred equally in both sexes, were dose-proportional to total milligrams of zafirlukast exposure, and were associated with coadministration of inhaled corticosteroids. The clinical significance of this finding is unknown. In rare cases, patients with asthma on zafirlukast may present with systemic eosinophilia, eosinophilic pneumonia, or clinical features of vasculitis consistent with Churg-Strauss syndrome, a condition which is often treated with systemic steroid therapy. Physicians should be alert to eosinophilia, vasculitic rash, worsening pulmonary symptoms, cardiac complications, and/or neuropathy presenting in their patients. These events have usually, but not always, been associated with reductions and/or withdrawal of steroid therapy. The possibility that zafirlukast may be associated with emergence of Churg-Strauss syndrome can neither be excluded nor established (see PRECAUTIONS , Eosinophilic Conditions ). Neuropsychiatric adverse events, including insomnia and depression, have been reported in association with zafirlukast therapy (see PRECAUTIONS , Neuropsychiatric Events ). Hypersensitivity reactions, including urticaria, angioedema and rashes, with or without blistering, have also been reported in association with zafirlukast therapy. Additionally, there have been reports of patients experiencing agranulocytosis, bleeding, bruising, or edema, arthralgia, myalgia, malaise, and pruritus in association with zafirlukast therapy. Rare cases of patients experiencing increased theophylline levels with or without clinical signs or symptoms of theophylline toxicity after the addition of zafirlukast to an existing theophylline regimen have been reported. The mechanism of the interaction between zafirlukast and theophylline in these patients is unknown and not predicted by available in vitro metabolism data and the results of two clinical drug interaction studies (see CLINICAL PHARMACOLOGY and PRECAUTIONS , Drug Interactions ). Pediatric Patients 5 through 11 years of age Zafirlukast has been evaluated for safety in 788 pediatric patients 5 through 11 years of age. Cumulatively, 313 pediatric patients were treated with zafirlukast 10 mg twice daily or higher for at least 6 months, and 113 of them were treated for one year or longer in clinical trials. The safety profile of zafirlukast 10 mg twice daily-versus placebo in the 4- and 6-week double-blind trials was generally similar to that observed in the adult clinical trials with zafirlukast 20 mg twice daily. In pediatric patients receiving zafirlukast in multi-dose clinical trials, the following events occurred with a frequency of ≥ 2% and more frequently than in pediatric patients who received placebo, regardless of causality assessment: headache (4.5 vs. 4.2%) and abdominal pain (2.8 vs. 2.3%). The post-marketing experience in this age group is similar to that seen in adults, including hepatic dysfunction, which may lead to liver failure.
Drug Interactions:
In a drug interaction study in 16 healthy male volunteers, coadministration of multiple doses of zafirlukast (160 mg/day) to steady-state with a single 25 mg dose of warfarin resulted in a significant increase in the mean AUC (+ 63%) and half-life (+36%) of S-warfarin. The mean prothrombin time (PT) increased by approximately 35%. This interaction is probably due to an inhibition by zafirlukast of the cytochrome P450 2C9 isoenzyme system. Patients on oral warfarin anticoagulant therapy and zafirlukast should have their prothrombin times monitored closely and anticoagulant dose adjusted accordingly (see WARNINGS , Concomitant Warfarin Administration ). No formal drug-drug interaction studies with zafirlukast and other drugs known to be metabolized by the cytochrome P450 2C9 isoenzyme (e.g., tolbutamide, phenytoin, carbamazepine) have been conducted; however, care should be exercised when zafirlukast is coadministered with these drugs.
In a drug interaction study in 11 asthmatic patients, coadministration of a single dose of zafirlukast (40 mg) with erythromycin (500 mg three times daily for 5 days) to steady-state resulted in decreased mean plasma levels of zafirlukast by approximately 40% due to a decrease in zafirlukast bioavailability.
Coadministration of zafirlukast (20 mg/day) or placebo at steady-state with a single dose of sustained release theophylline preparation (16 mg/kg) in 16 healthy boys and girls (6 through 11 years of age) resulted in no significant differences in the pharmacokinetic parameters of theophylline.
Coadministration of zafirlukast (80 mg/day) at steady-state with a single dose of a liquid theophylline preparation (6 mg/kg) in 13 asthmatic patients, 18 to 44 years of age, resulted in decreased mean plasma levels of zafirlukast by approximately 30%, but no effect on plasma theophylline levels was observed.
Rare cases of patients experiencing increased theophylline levels with or without clinical signs or symptoms of theophylline toxicity after the addition of zafirlukast to an existing theophylline regimen have been reported. The mechanism of the interaction between zafirlukast and theophylline in these patients is unknown (see ADVERSE REACTIONS ).
Coadministration of zafirlukast (40 mg/day) with aspirin (650 mg four times daily) resulted in mean increased plasma levels of zafirlukast by approximately 45%.
In a single-blind, parallel-group, 3-week study in 39 healthy female subjects taking oral contraceptives, 40 mg twice daily of zafirlukast had no significant effect on ethinyl estradiol plasma concentrations or contraceptive efficacy.
Coadministration of zafirlukast with fluconazole, a moderate CYP2C9 inhibitor, resulted in increased plasma levels of zafirlukast, by approximately 58% (90% CI:28, 95). The clinical significance of this interaction is unknown. Zafirlukast exposure is likely to be increased by other moderate and strong CYP2C9 inhibitors. Coadministration of zafirlukast with itraconazole, a strong CYP3A4 inhibitor, caused no change in plasma levels of zafirlukast.
No other formal drug-drug interaction studies between zafirlukast and marketed drugs known to be metabolized by the P450 3A4 (CYP3A4) isoenzyme (e.g., dihydropyridine calcium-channel blockers, cyclosporin, cisapride) have been conducted. As zafirlukast is known to be an inhibitor of CYP3A4 in vitro , it is reasonable to employ appropriate clinical monitoring when these drugs are coadministered with zafirlukast.
DESCRIPTION
Zafirlukast is a synthetic, selective peptide leukotriene receptor antagonist (LTRA), with the chemical name 4-(5-cyclopentyloxy-carbonylamino-1-methyl-indol-3-ylmethyl)-3-methoxy-N-o-tolylsulfonylbenzamide. The molecular weight of zafirlukast is 575.7 and the structural formula is:
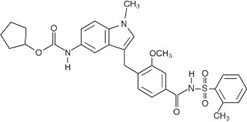
The molecular formula is: C 31 H 33 N 3 O 6 S
Zafirlukast, off-white to light pink color powder, is practically insoluble in water, freely soluble in tetrahydrofuran, dimethylsulfoxide and acetone.
Zafirlukast is supplied as 10 and 20 mg tablets for oral administration.
Inactive Ingredients : Film-coated tablets containing croscarmellose sodium, hypromellose, lactose monohydrate, magnesium stearate, microcrystalline cellulose, povidone and titanium dioxide.
CLINICAL PHARMACOLOGY
Mechanism of Action: Zafirlukast is a selective and competitive receptor antagonist of leukotriene D 4 and E 4 (LTD 4 and LTE 4 ), components of slow-reacting substance of anaphylaxis (SRSA). Cysteinyl leukotriene production and receptor occupation have been correlated with the pathophysiology of asthma, including airway edema, smooth muscle constriction, and altered cellular activity associated with the inflammatory process, which contribute to the signs and symptoms of asthma. Patients with asthma were found in one study to be 25 to 100 times more sensitive to the bronchoconstricting activity of inhaled LTD 4 than nonasthmatic subjects. In vitro studies demonstrated that zafirlukast antagonized the contractile activity of three leukotrienes (LTC 4 , LTD 4 and LTE 4 ) in conducting airway smooth muscle from laboratory animals and humans. Zafirlukast prevented intradermal LTD 4 -induced increases in cutaneous vascular permeability and inhibited inhaled LTD 4 -induced influx of eosinophils into animal lungs. Inhalational challenge studies in sensitized sheep showed that zafirlukast suppressed the airway responses to antigen; this included both the early- and late-phase response and the nonspecific hyperresponsiveness. In humans, zafirlukast inhibited bronchoconstriction caused by several kinds of inhalational challenges. Pretreatment with single oral doses of zafirlukast inhibited the bronchoconstriction caused by sulfur dioxide and cold air in patients with asthma. Pretreatment with single doses of zafirlukast attenuated the early- and late-phase reaction caused by inhalation of various antigens such as grass, cat dander, ragweed, and mixed antigens in patients with asthma. Zafirlukast also attenuated the increase in bronchial hyperresponsiveness to inhaled histamine that followed inhaled allergen challenge. Clinical Pharmacokinetics and Bioavailability: Absorption Zafirlukast is rapidly absorbed following oral administration. Peak plasma concentrations are generally achieved 3 hours after oral administration. The absolute bioavailability of zafirlukast is unknown. In two separate studies, one using a high fat and the other a high protein meal, administration of zafirlukast with food reduced the mean bioavailability by approximately 40%. Distribution Zafirlukast is more than 99% bound to plasma proteins, predominantly albumin. The degree of binding was independent of concentration in the clinically relevant range. The apparent steady-state volume of distribution (Vss/F) is approximately 70 L, suggesting moderate distribution into tissues. Studies in rats using radiolabeled zafirlukast indicate minimal distribution across the blood-brain barrier. Metabolism Zafirlukast is extensively metabolized. The most common metabolic products are hydroxylated metabolites which are excreted in the feces. The metabolites of zafirlukast identified in plasma are at least 90 times less potent as LTD 4 receptor antagonists than zafirlukast in a standard in vitro test of activity. In vitro studies using human liver microsomes showed that the hydroxylated metabolites of zafirlukast excreted in the feces are formed through the cytochrome P450 2C9 (CYP2C9) pathway. Additional in vitro studies utilizing human liver microsomes show that zafirlukast inhibits the cytochrome P450 CYP3A4 and CYP2C9 isoenzymes at concentrations close to the clinically achieved total plasma concentrations (see Drug Interactions ). Excretion The apparent oral clearance (CL/f) of zafirlukast is approximately 20 L/h. Studies in the rat and dog suggest that biliary excretion is the primary route of excretion. Following oral administration of radiolabeled zafirlukast to volunteers, urinary excretion accounts for approximately 10% of the dose and the remainder is excreted in feces. Zafirlukast is not detected in urine. In the pivotal bioequivalence study, the mean terminal half-life of zafirlukast is approximately 10 hours in both normal adult subjects and patients with asthma. In other studies, the mean plasma half-life of zafirlukast ranged from approximately 8 to 16 hours in both normal subjects and patients with asthma. The pharmacokinetics of zafirlukast are approximately linear over the range from 5 mg to 80 mg. Steady-state plasma concentrations of zafirlukast are proportional to the dose and predictable from single-dose pharmacokinetic data. Accumulation of zafirlukast in the plasma following twice-daily dosing is approximately 45%. The pharmacokinetic parameters of zafirlukast 20 mg administered as a single dose to 36 male volunteers are shown with the table below.
| 1. Median and range | ||||
| C max ng/ml | t max 1 h | AUC ng•h/mL | t 1/2 h | CL/f L/h |
| 326 (31.0) | 2 (0.5 to 5.0) | 1137 (34) | 13.3 (75.6) | 19.4 (32) |
Special Populations Gender: The pharmacokinetics of zafirlukast are similar in males and females. Weight-adjusted apparent oral clearance does not differ due to gender. Race: No differences in the pharmacokinetics of zafirlukast due to race have been observed. Elderly: The apparent oral clearance of zafirlukast decreases with age. In patients above 65 years of age, there is an approximately 2 to 3 fold greater C max and AUC compared to young adult patients. Children: Following administration of a single 20 mg dose of zafirlukast to 20 boys and girls between 7 and 11 years of age, and in a second study, to 29 boys and girls between 5 and 6 years of age, the following pharmacokinetic parameters were obtained:
| Parameter | Children age 5 to 6 years Mean (% Coefficient of Variation) | Children age 7 to 11 years Mean (% Coefficient of Variation) |
| C max (ng/mL) | 756 (39%) | 601 (45%) |
| AUC (ng•h/mL) | 2458 (34%) | 2027 (38%) |
| t max (h) | 2.1 (61%) | 2.5 (55%) |
| CL/f (L/h) | 9.2 (37%) | 11.4 (42%) |
Weight unadjusted apparent clearance was 11.4 L/h (42%) in the 7 to 11 year old children and 9.2 L/h (37%) in the 5 to 6 year old children, which resulted in greater systemic drug exposures than that obtained in adults for an identical dose. To maintain similar exposure levels in children compared to adults, a dose of 10 mg twice daily is recommended in children 5 to 11 years of age (see DOSAGE AND ADMINISTRATION ). Zafirlukast disposition was unchanged after multiple dosing (20 mg twice daily) in children and the degree of accumulation in plasma was similar to that observed in adults. Hepatic Insufficiency: In a study of patients with hepatic impairment (biopsy-proven cirrhosis), there was a reduced clearance of zafirlukast resulting in a 50 to 60% greater C max and AUC compared to normal subjects. Renal Insufficiency: Based on a cross-study comparison, there are no apparent differences in the pharmacokinetics of zafirlukast between renally-impaired patients and normal subjects. Drug-Drug Interactions: The following drug interaction studies have been conducted with zafirlukast (see PRECAUTIONS , Drug Interactions ).
- Coadministration of multiple doses of zafirlukast (160 mg/day) to steady-state with a single 25 mg dose of warfarin (a substrate of CYP2C9) resulted in a significant increase in the mean AUC (+63%) and half-life (+36%) of S-warfarin. The mean prothrombin time increased by approximately 35%. The pharmacokinetics of zafirlukast were unaffected by coadministration with warfarin.
- Coadministration of zafirlukast (80 mg/day) at steady-state with a single dose of a liquid theophylline preparation (6 mg/kg) in 13 asthmatic patients, 18 to 44 years of age, resulted in decreased mean plasma concentrations of zafirlukast by approximately 30%, but no effect on plasma theophylline concentrations was observed.
- Coadministration of zafirlukast (20 mg/day) or placebo at steady-state with a single dose of sustained release theophylline preparation (16 mg/kg) in 16 healthy boys and girls (6 through 11 years of age) resulted in no significant differences in the pharmacokinetic parameters of theophylline.
- Coadministration of zafirlukast dosed at 40 mg twice daily in a single-blind, parallel-group, 3-week study in 39 healthy female subjects taking oral contraceptives, resulted in no significant effect on ethinyl estradiol plasma concentrations or contraceptive efficacy.
- Coadministration of zafirlukast (40 mg/day) with aspirin (650 mg four times daily) resulted in mean increased plasma concentrations of zafirlukast by approximately 45%.
- Coadministration of a single dose of zafirlukast (40 mg) with erythromycin (500 mg three times daily for 5 days) to steady-state in 11 asthmatic patients resulted in decreased mean plasma concentrations of zafirlukast by approximately 40% due to a decrease in zafirlukast bioavailability.
- Coadministration of zafirlukast with fluconazole, a moderate CYP2C9 inhibitor, resulted in increased plasma levels of zafirlukast, by approximately 58% (90% CI:28, 95). The clinical significance of this interaction is unknown. Zafirlukast exposure is likely to be increased by other moderate and strong CYP2C9 inhibitors. Coadministration of zafirlukast with itraconazole, a strong CYP3A4 inhibitor, caused no change in plasma levels of zafirlukast.
Clinical Studies: Three U.S. double-blind, randomized, placebo-controlled, 13-week clinical trials in 1380 adults and children 12 years of age and older with mild-to-moderate asthma demonstrated that zafirlukast improved daytime asthma symptoms, nighttime awakenings, mornings with asthma symptoms, rescue beta 2 -agonist use, FEV 1 , and morning peak expiratory flow rate. In these studies, the patients had a mean baseline FEV 1 of approximately 75% of predicted normal and a mean baseline beta 2 -agonist requirement of approximately 4 to 5 puffs of albuterol per day. The results of the largest of the trials are shown in the table below.
| 1. p<0.05, compared to placebo | ||
| Zafirlukast 20 mg twice daily N=514 | Placebo N=248 | |
| Daytime Asthma symptom score (0 to 3 scale) | -0.44 1 | -0.25 |
| Nightime Awakenings (number per week) | -1.27 1 | -0.43 |
| Mornings with Asthma Symptoms (days per week) | -1.32 1 | -0.75 |
| Rescue β 2 -agonist use (puffs per day) | -1.15 1 | -0.24 |
| FEV 1 (L) | +0.15 1 | +0.05 |
| Morning PEFR (L/min) | +22.06 1 | +7.63 |
| Evening PEFR (L/min) | +13.12 | +10.14 |
In a second and smaller study, the effect of zafirlukast on most efficacy parameters was comparable to the active control (inhaled cromolyn sodium 1600 mcg four times per day) and superior to placebo at end point for decreasing rescue beta 2 -agonist use (figure below). 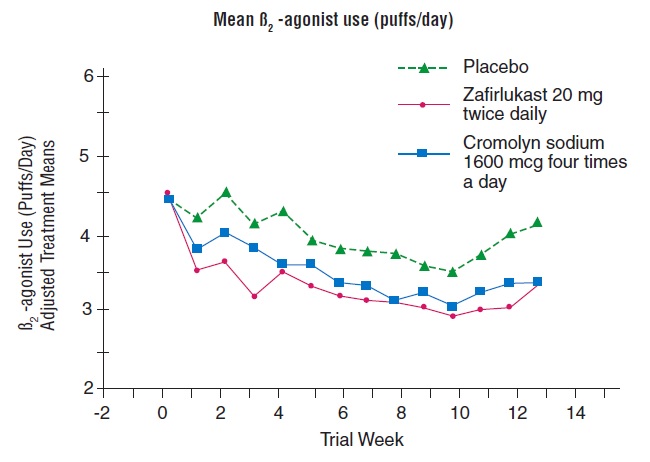 In these trials, improvement in asthma symptoms occurred within one week of initiating treatment with zafirlukast. The role of zafirlukast in the management of patients with more severe asthma, patients receiving antiasthma therapy other than as-needed, inhaled beta 2 -agonists, or as an oral or inhaled corticosteroid-sparing agent remains to be fully characterized.
In these trials, improvement in asthma symptoms occurred within one week of initiating treatment with zafirlukast. The role of zafirlukast in the management of patients with more severe asthma, patients receiving antiasthma therapy other than as-needed, inhaled beta 2 -agonists, or as an oral or inhaled corticosteroid-sparing agent remains to be fully characterized.
HOW SUPPLIED
Zafirlukast Tablets 10 mg , are white, round, biconvex, film-coated tablets debossed with “1” on one side and “B” on other side. Bottles of 60 NDC 59651-291-60 Zafirlukast Tablets 20 mg , are white, round, biconvex, film-coated tablets debossed with “2” on one side and “B” on other side. Bottles of 60 NDC 59651-292-60
Store at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature]. Protect from light and moisture. Dispense in the original air-tight container.
Distributed by: Aurobindo Pharma USA, Inc. 279 Princeton-Hightstown Road East Windsor, NJ 08520 Manufactured by: Aurobindo Pharma Limited Hyderabad-500 032, India Issued: June 2023